Abstract
Objectives
This study aimed to analyze the effect of audiovisual and group support foot exercises on the Ankle Brachial Pressure Index and foot sensation.
Methods
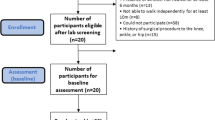
This study used a quasi-experimental design. The sample number of this study was 156 using a purposive sampling technique. The research group was divided into three groups. The variables measured in this study were ABPI, foot sensation, and foot exercise experience. The statistical analysis was conducted by a paired-sample t-test, an independent-sample t-test, and a two-way Manova.
Results
The results showed that each group had a difference in how ABPI and foot sensation were influenced (p = 0.000). Additionally, audiovisual and group support foot exercises have been shown to influence ABPI (p = 0.000) and foot sensation (p) = 0.000).
Conclusions
Audiovisual and group support foot exercises significantly influenced the Ankle Brachial Pressure Index value and foot sensation in diabetic mellitus patients. This intervention is encouraged for diabetic mellitus patients who would like to see the benefits of exercise and group support.
Similar content being viewed by others
References
Alqahtani KM, Bhangoo M, Vaida F, Denenberg JO, Allison MA, Criqui MH. Predictors of change in the ankle brachial index with Exercise. Eur J Vasc Endovasc Surg. Elsevier Ltd. 2018;55(3):399–404. https://doi.org/10.1016/j.ejvs.2017.12.004.
Alves-Cabratosa L, Comas-Cufí M, Ponjoan A, Garcia-Gil M, Martí-Lluch R, Blanch J, Elosua-Bayes M, Parramon D, Camós L, Guzmán L, Ramos R. Levels of ankle-brachial index and the risk of diabetes mellitus complications. BMJ Open Diabetes Res Care. 2020;8(1). https://doi.org/10.1136/bmjdrc-2019-0009772019-000977.
Betteridge DJ, Nicholls S. Managing cardiovascular complications in diabetes. 1st ed. Chichester: Wiley; 2014.
Colberg SR, et al. Exercise and type 2 Diabetes. Diabetes Care. 2010;33(12):e147–67. https://doi.org/10.2337/dc10-9990.
Cunningham JB, McCrum-Gardner E. Power, effect and sample size using GPower: practical issues for researchers and members of research ethics committees. Evid Based Midwifery. 2007;5(4):132–7.
Doughty D, McNichol L. Wound, Ostomy and continence nurses society. Philadelphia: Wolters Kluwer Health; 2014.
Fertman CI, Allensworth DD. Health promotion programs. 2nd ed. Hoboken: Wiley; 2016.
Forst T, Kaptiza C. Clinical advances in diabetes mellitus. London: Future Science Ltd.; 2015.
Francia P, Gulisano M, Anichini R, Seghieri G. Diabetic foot and exercise therapy: step by step the role of rigid posture and biomechanics treatment. Curr Diabetes Rev. 2014:86–99. https://doi.org/10.2174/1573399810666140507112536.
Glanz K, Rimer BK, Viswanath K. Health behavior: theory, research, and practice. 5th ed. New York: Wiley; 2015.
Hasneli Y, Amir Y. Identification and analysis of foot sensitivity and blood glucose levels post Apiyu massage. Enferm Clín. 2019:9–12. https://doi.org/10.1016/j.enfcli.2018.11.009.
Hess CT. Clinical guide to Skin & Wound Care. 7th ed. Philadelphia: Wolters Kluwer Health; 2012.
IDF. International Diabetes Federation: Diabetes Atlas. 9th ed. 2019. https://www.diabetesatlas.org/upload/resources/material/20200302_133351_IDFATLAS9e-final-web.pdf. Accessed 20 Dec 2020.
Ji L, Bai JJ, Sun J, Ming Y, Chen LR. Effect of combining music media therapy with lower extremity exercise on elderly patients with diabetes mellitus. Int J Nurs Sci. 2015;2(3):243–7. https://doi.org/10.1016/j.ijnss.2015.07.008.
Kemenkes. Riset Kesehatan Dasar RISKESDAS 2018. Jakarta: Balitbang Kemenkes RI; 2018.
Lindberg K, Møller BS, Kirketerp-Møller K, Kristensen MT. An exercise program for people with severe peripheral neuropathy and diabetic foot ulcers–a case series on feasibility and safety. Disabil Rehabil. Taylor & Francis. 2020;42(2):183–9. https://doi.org/10.1080/09638288.2018.1494212.
Lung CW, Wu FL, Liao F, Pu F, Fan Y, Jan YK. Emerging technologies for the prevention and management of diabetic foot ulcers. J Tissue Viability. 2020:0–1. https://doi.org/10.1016/j.jtv.2020.03.003.
Morowatisharifabad MA, et al. Study on social support for exercise and its impact on the level of physical activity of patients with type 2 Diabetes. J Med Sci. Public Health. 2019;1(7):143–7.
Schaper NC, et al. Prevention and management of foot problems in diabetes: a summary guidance for daily practice 2015, based on the IWGDF guidance Documents. Diabetes Metab Res Rev. Wiley Online Library. 2016;32:7–15.
Shaw KM, Cummings MH. Diabetes chronic complications. London: Wiley; 2012.
Sheehan JP, Ulchaker MM. Obesity and type 2 diabetes mellitus : obesity and type 2 diabetes mellitus. New York: Oxford University Press USA – OSO; 2011.
Taddei UT, Matias AB, Ribeiro FIA, Inoue RS, Bus SA, Sacco ICN. Effects of a therapeutic foot exercise program on injury incidence, foot functionality and biomechanics in long-distance runners: feasibility study for a randomized controlled trial. Phys Ther Sport Elsevier Ltd. 2018;34:216–26. https://doi.org/10.1016/j.ptsp.2018.10.015.
Tuomilehto J. Nonpharmacologic therapy and exercise in the prevention of type 2 Diabetes. Diabetes Care. 2009;32(suppl 2):S189–93. https://doi.org/10.2337/dc09-S308.
van Laake-Geelen CC, Smeets RJ, Quadflieg SP, Kleijnen J, Verbunt JA. The effect of exercise therapy combined with psychological therapy on physical activity and quality of life in patients with painful diabetic neuropathy. Scand J Pain. 2019;19(3):433–9. https://doi.org/10.1515/sjpain-2019-0001.
Wu FL, Wang WTJ, Liao F, Elliott J, Jain S, Jan YK. Effects of walking speeds and durations on plantar skin blood flow responses. Microvasc Res. 2020;128(October 2019):103936. https://doi.org/10.1016/j.mvr.2019.103936.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Faizah, R., Efendi, F. & Suprajitno, S. The effects of foot exercise with audiovisual and group support foot exercises to diabetes mellitus patients. J Diabetes Metab Disord 20, 377–382 (2021). https://doi.org/10.1007/s40200-021-00756-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40200-021-00756-9