Abstract
Aim
Hyperinsulinemia is considered the primary defect underlying the development of type 2 diabetes. The liver is essential for the regular glucose homeostasis. In this study, we examined the effect of physical training on the insulin signaling, oxidative stress enzymes and Glucose-6-phosphatase(G6Pase) activity in the liver of Wistar rats.
Methods
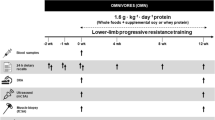
Adult male Wistar rats were divided into Control diet group(C), High carbohydrate diet(HCD), High fat diet(HFD), HCD and HFD with training(HCD Ex & HFD Ex). HFD Ex and HCD Ex were trained on a small animal treadmill running at 20 m/min for 30 min, 5 days/wk. The present work investigated the effect of training on hepatic insulin receptor(InsR) signaling events, oxidative stress marker expressions and G6Pase activity in hyperinsulinemic rats.
Results
High carbohydrate and fat feeding led to hyperinsulinemic status with increased hepatic G6Pase activity and impaired phosphorylation of insulin receptor substrate 1(IRS1) and reduced expression of antioxidant enzymes.Training significantly reduced hepatic G6Pase activity, upregulated phosphoinositide 3 kinase(PI3K) docking site phosphorylation and downregulated the negative IRS1 phosphorylations thereby increasing the glucose transporter(GLUT) expressions (aa(P < 0.001) when compared to HFD, b(P < 0.01),bb (P < 0.001 when compared to HCD). Anti oxidant enzymes like CAT, SOD, eNOS expression were increased with reduction in the expression of inflammatory enzymes like TNF-α and COX-2 (*(P < 0.05),**(P < 0.01),***(P < 0.001) when compared to control, †(P < 0.05),††(P < 0.01),†††(P < 0.001) when compared to HFD and HCD).
Conclusion
Thus, our study shows that four weeks training enhanced the hepatic insulin sensitivity in high fat and high carbohydrate-diet fed hyperinsulinemic rats.






Similar content being viewed by others
References
Pan XR, Li GW, Hu YH, Wang JX, Yang WY, An ZX, Hu ZX, Lin J, Xiao JZ, Cao HB, Liu PA, Jiang XG, Jiang YY, Wang JP, Zheng H, Zhang H, Bennett PH, Howard BV. Effects of diet and exercise in preventing NIDDM in people with impaired glucose tolerance. The Da Qing IGT and Diabetes Study. Diabetes Care. 1997;20(4):537–44.
Sigal RJ, Kenny GP, Wasserman DH, Castaneda-Sceppa C, White RD. Physical activity/exercise and type 2 diabetes: a consensus statement from the American Diabetes Association. Diabetes Care. 2006;29(6):1433–8.
Venkatasamy VV, Pericherla S, Manthuruthil S, Mishra S, Hanno R. Effect of physical activity on insulin resistance, inflammation and oxidative stress in diabetes mellitus. J Clin Diagn Res. 2013;7(8):1764–6.
Rutter GA. Diabetes: the importance of the liver. Curr Biol. 2000;10(20):R736-8.
Petersen MC, Vatner DF, Shulman GI. Regulation of hepatic glucose metabolism in health and disease. Nat Rev Endocrinol. 2017;13(10):572–87.
Gregory JM, Muldowney JA, Engelhardt BG, et al. Aerobic exercise training improves hepatic and muscle insulin sensitivity, but reduces splanchnic glucose uptake in obese humans with type 2 diabetes. Nutr Diabetes. 2019;9(1):25.
Suk M, Shin YJ. Effect of high-intensity exercise and high-fat diet on lipid metabolism in the liver of rats. Exerc Nutrition Biochem. 2015;19(4):289–95.
Valverde AM, González-Rodríguez A. IRS2 and PTP1B: Two opposite modulators of hepatic insulin signalling. Arch Physiol Biochem. 2011;117(3):105–15.
Samuel VT, Shulman GI. The pathogenesis of insulin resistance: integrating signaling pathways and substrate flux. J Clin Invest. 2016;126(1):12–22.
Hurrle S, Hsu WH. The etiology of oxidative stress in insulin resistance. Biomed J. 2017;40(5):257–62.
O’Brien RM, Granner DK. Regulation of gene expression by insulin. Physiol Rev. 1996;76(4):1109–61.
Michael MD, Kulkarni RN, Postic C, Previs SF, Shulman GI, Magnuson MA, Kahn CR. Loss of insulin signaling in hepatocytes leads to severe insulin resistance and progressive hepatic dysfunction. Mol Cell. 2000;6(1):87–97.
Choukem SP, Gautier JF. How to measure hepatic insulin resistance? Diabetes Metab. 2008;34:664–73.
Edgerton DS, Cardin S, Pan C, Neal D, Farmer B, Converse M, Cherrington AD. Effects of insulin deficiency or excess on hepatic gluconeogenic flux during glycogenolytic inhibition in the conscious dog. Diabetes. 2002;51(11):3151–62.
Draznin B. Molecular mechanisms of insulin resistance: serine phosphorylation of insulin receptor substrate-1 and increased expression of p85alpha: the two sides of a coin. Diabetes. 2006;55(8):2392–7.
Saeidi A, Hackney C, Tayebi A, Ahmadian SM, Zouhal M, Diabetes H. Insulin resistance, fetuin-B and exercise training. Ann Appl Sport Sci. 2019;7(2):1–2.
Haus JM, et al. Free fatty acid-induced hepatic insulin resistance is attenuated following lifestyle intervention in obese individuals with impaired glucose tolerance. J Clin Endocrinol Metab. 2010;95:323–7.
Joseph A, Parvathy S, Varma KK. Altered insulin signaling and lactate dehydrogenase activity in the heart of hyperinsulinemic rats: effect of exercise. Metabolism. 2020;104S:154091.
Wallert MA, Fosterb JD, Scholnick DA, Olmschenk SM, Kuehna BJ, Provost JJ. Kinetic analysis of glucose-6-phosphatase: an investigative approach to carbohydrate metabolism and kinetics. Biochem Mol Biol Educ. 2001;29:199–203.
Vijayan A, Varma KK, Malattiri R. Plasma insulin and insulin resistance in diabetes mellitus type 2. Gen Med (Los Angel). 2014;3:152.
Colberg SR, Sigal RJ, Fernhall B, et al. Exercise and type 2 diabetes: the American College of Sports Medicine and the American Diabetes Association: joint position statement. Diabetes Care. 2010;33(12):e147–67.
Saad MJ, Araki E, Miralpeix M, Rothenberg PL, White MF, Kahn CR. Regulation of insulin receptor substrate-1 in liver and muscle of animal models of insulin resistance. J Clin Invest. 1992;90(5):1839–49.
Lucchesi AN, Freitas NT, Cassettari LL, Marques SF, Spadella CT. Diabetes mellitus triggers oxidative stress in the liver of alloxan-treated rats: a mechanism for diabetic chronic liver disease. Acta Cir Bras. 2013;28(7):502–8.
Bedi O, Aggarwal S, Trehanpati N, Ramakrishna G, Krishan P. Molecular and pathological events involved in the pathogenesis of diabetes-associated nonalcoholic fatty liver disease. J Clin Exp Hepatol. 2019;9(5):607–18.
Rees MD, Kennett EC, Whitelock JM, Davies MJ. Oxidative damage to extracellular matrix and its role in human pathologies. Free Radic Med. 2008;44:1973–2001.
Botezelli JD, Cambri LT, Ghezzi AC, Dalia RA, Voltarelli FA, de Mello MA. Fructose-rich diet leads to reduced aerobic capacity and to liver injury in rats. Lipids Health Dis. 2012;11:78.
McNaughton L, Puttagunta L, Martinez-Cuesta MA, et al. Distribution of nitric oxide synthase in normal and cirrhotic human liver. Proc Natl Acad Sci U S A. 2002;99(26):17161–6.
Tateya S, Rizzo NO, Handa P, Cheng AM, Morgan-Stevenson V, Daum G, Clowes AW, Morton GJ, Schwartz MW, Kim F. Endothelial NO/cGMP/VASP signaling attenuates Kupffer cell activation and hepatic insulin resistance induced by high-fat feeding. Diabetes. 2011 ;60(11):2792–801.
Martín-Sanz P, Casado M, Boscá L. Cyclooxygenase 2 in liver dysfunction and carcinogenesis: Facts and perspectives. World J Gastroenterol. 2017;23(20):3572–80.
Pillon Barcelos R, Freire Royes LF, Gonzalez-Gallego J, Bresciani G. Oxidative stress and inflammation: liver responses and adaptations to acute and regular exercise. Free Radic Res. 2017;51(2):222–36.
Hoene M, Lehmann R, Hennige AM, Pohl AK, Häring HU, Schleicher ED, Weigert C. Acute regulation of metabolic genes and insulin receptor substrates in the liver of mice by one single bout of treadmill exercise. J Physiol. 2009;587:241–52.
Ropelle ER, Pauli JR, Prada PO, de Souza CT, Picardi PK, Faria MC, et al. Reversal of diet-induced insulin resistance with a single bout of exercise in the rat: the role of PTP1B and IRS-1 serine phosphorylation. J Physiol. 2006;577:997–1007.
Schultz A, Mendonca LS, Aguila MB, Mandarim-de-Lacerda CA. Swimming training beneficial effects in a mice model of nonalcoholic fatty liver disease. Exp Toxicol Pathol. 2012;64(4):273–82.
Marques CMM, Motta VF, Torres TS, Aguila MB, Mandarim-de-Lacerda CA. Beneficial effects of exercise training (treadmill) on insulin resistance and nonalcoholic fatty liver disease in high-fat fed C57BL/6 mice. BJMBR. 2010;43(5):467–75.
Zheng F, Cai Y. Concurrent exercise improves insulin resistance and nonalcoholic fatty liver disease by upregulating PPAR-γ and genes involved in the beta-oxidation of fatty acids in ApoE-KO mice fed a high-fat diet. Lipids Health Dis. 2019;18(1):6.
Marcinko K, Sikkema SR, Samaan MC, Kemp BE, Fullerton MD. Steinberg GR High intensity interval training improves liver and adipose tissue insulin sensitivity. Mol Metab. 2015;4(12):903–15.
Eckstein SS, Weigert C, Lehmann R. Divergent roles of IRS (Insulin Receptor Substrate) 1 and 2 in liver and skeletal muscle. Curr Med Chem. 2017;24(17):1827–52.
Titchenell PM, Chu Q, Monks BR, Birnbaum MJ. Hepatic insulin signalling is dispensable for suppression of glucose output by insulin in vivo. Nat Commun. 2015;6:7078.
Argaud D, Zhang Q, Pan W, Maitra S, Pilkis SJ, Lange AJ. Regulation of rat liver glucose-6-phosphatase gene expression in different nutritional and hormonal states: gene structure and 5’-flanking sequence. Diabetes. 1996;45(11):1563–71.
Rui L. Energy metabolism in the liver. Compr Physiol. 2014;4(1):177–97.
Amy K, Rines K, Sharabi CDJ, Tavares, Puigserver P. Targeting hepatic glucose output in the treatment of type 2 diabetes. Nat Rev Drug Discov. 2016;15(11):786–804.
Ziv E, Kalman R, Hershkop K, Barash V, Shafrir E, Bar-On H. Insulin resistance in the NIDDM model Psammomys obesus in the normoglycaemic, normoinsulinemic state. Diabetologia. 1996;39(11):1269–75.
Knudsen JG, Bienso RS, Hassing HA, Jakobsen AH, Pilegaard H. Exercise-induced regulation of key factors in substrate choice and gluconeogenesis in mouse liver. Mol Cell Biochem. 2015;403:209–17.
Sheldon RD, Laughlin MH, Rector RS. Reduced hepatic eNOS phosphorylation is associated with NAFLD and type 2 diabetes progression and is prevented by daily exercise in hyperphagic OLETF rats. J Appl Physiol (1985). 2014;116(9):1156-64.
Kawanishi N, Yano H, Mizokami T, Takahashi M, Oyanagi E, Suzuki K. Exercise training attenuates hepatic inflammation, fibrosis and macrophage infiltration during diet induced-obesity in mice. Brain Behav Immun. 2012;26(6):931–41.
Farzanegi P, Dana A, Ebrahimpoor Z, Asadi M, Azarbayjani MA. Mechanisms of beneficial effects of exercise training on non-alcoholic fatty liver disease (NAFLD): Roles of oxidative stress and inflammation. Eur J Sport Sci. 2019;19(7):994–1003.
Acknowledgements
The authors thank Mr Sreerenj and faculties of Department of Health Sciences, University of Calicut for allowing the use of department facilities. We also thank the MIMSRF Lab manager Mr Varun and assistant Mrs Mahishiya for their timely help.
Funding
This work is supported by funding from DST SERB, Govt. of India (ECR/2015/000158) and MIMS Research Foundation, Calicut, Kerala.
Author information
Authors and Affiliations
Contributions
AJ: Conceptualization, Methodology, Writing- Reviewing and Editing, PS.: Methodology, Investigation, Validation Writing – Original Draft, KKV: Supervision, Writing – Review & Editing. AN- Standardisation All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
All animal care and procedures were in accordance with the recommendations in the Guide for the Care and Use of Laboratory Animals by the Committee for the Purpose of Control And Supervision of Experiments on Animals (CPCSEA), Govt. Of India and was approved by MIMS Research Foundation Ethics Committee.
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
ESM 1
(DOCX 27.7 KB)
Rights and permissions
About this article
Cite this article
Joseph, A., Parvathy, S., Varma, K.K. et al. Four weeks exercise training enhanced the hepatic insulin sensitivity in high fat- and high carbohydrate-diet fed hyperinsulinemic rats. J Diabetes Metab Disord 19, 1583–1592 (2020). https://doi.org/10.1007/s40200-020-00694-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40200-020-00694-y