Abstract
Background
Zotepine (ZTP), an antipsychotic drug is well tolerated and particularly effective for treating negative symptoms of psychosis. But is limited by low oral bioavailability caused by substantial first pass metabolism and thereby less amount of drug reaches the brain due to blood brain barrier (BBB).
Objectives
Since ZTP displays dose dependent side effects, purpose of the contemporary study is to develop zotepine loaded nanosuspension (ZTP-NS) for increased brain targeting in rats at lower doses.
Methods
ZTP-NS is prepared by two techniques viz., sonoprecipitation (SP) and combination technique (high pressure homogenization preceded by precipitation) by employing various stabilizers. Optimized ZTP-NS was characterized for particle size, solid state, morphology and solubility. In vitro drug release of ZTP and formulations was conducted using Franz diffusion cell. Stability study was performed at different temperature conditions. Pharmacokinetic study was performed in Wistar rats to determine the bioavailability and brain distribution of ZTP after intra-nasal (IN) and intravenous (IV) administration. Histopathology of brain was done after repeated administration of IN ZTP dispersion and NS up to 14 days.
Results
The optimized ZTP-NS formulated with Pluronic F-127 (0.3%w/v), Hydroxypropyl methyl cellulose E15 (0.3%w/v) and soya lecithin (0.4%w/v) showed particle size of 519.26 ± 10.44 nm & 330.2 ± 12.90 nm and zeta potential of −21.7 ± 1.39 mV and − 18.26 ± 1.64 mV with sonoprecipitation and combination technique respectively. In vitro drug release was high (81.79 ± 3.23%) for ZTP-NS prepared by combination technique. Intranasal NS resulted in high brain concentrations of 8.6 fold (sonoprecipitation) and 10.79-fold hike in AUC0–24h in contrast to intravenous ZTP solution. Histopathology results reveal no significant changes in brain microscopic images.
Conclusion
ZTP-NS was successfully developed, characterized and found that nanosuspension is a favorable approach for intranasal delivery of zotepine.

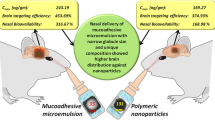
Graphical abstract representing zotepine drawbacks, nanosuspension preparation, characterization and pharmacokinetic study in rats










Similar content being viewed by others
References
Heckers S, Barch DM, Bustillo J, Gaebel W, Gur R, Malaspina D, et al. Structure of the psychotic disorders classification in DSM-5. Schizophr Res. 2013;150:11–4.
Seeman P. Atypical antipsychotics: mechanism of action. Can J Psychiatr. 2002;47:27–38.
Hwang TJ, Lin SK, Lin HN. Efficacy and safety of zotepine for the treatment of Taiwanese schizophrenic patients: a double-blind comparison with haloperidol. J Formos Med Assoc. 2001;100:811–6.
Needham PL, Atkinson J, Skill MJ, Heal DJ. Zotepine: preclinical tests predict antipsychotic efficacy and an atypical profile. Psychopharmacol Bull. 1996;32:123–8.
Shobo M, Kondo Y, Yamada H, Mihara T, Yamamoto N, Katsuoka M, et al. Norzotepine, a major metabolite of Zotepine, exerts atypical antipsychotic-like and antidepressant-like actions through its potent inhibition of norepinephrine reuptake. J Pharmacol Exp Ther. 2010;333:772–81.
Leucht S, Cipriani A, Spineli L, Mavridis D, Örey D, Richter F, et al. Comparative efficacy and tolerability of 15 antipsychotic drugs in schizophrenia: a multiple-treatments meta-analysis. Lancet. 2013;382:951–62.
Popescu C, Manda P. Preparation and characterization of Zotepine solid Didpersions by Cyclodextrin complexation. 2013.
Isabel Kalofonos, Dimitris Kalfonos, William Martin-Doyle, Janson A. Hanko EJH. US patent No. WO 2009/152347 A2.Crystalline forms of zotepine hydrochloride. 2009.
Green B. Zotepine: a clinical review. Expert Opin Drug Metab Toxicol. 2009;5:181–6.
Banks WA. Characteristics of compounds that cross the blood-brain barrier. BMC Neurol BioMed Central. 2009;9 Suppl 1:S3.
Miller DS. Regulation of P-glycoprotein and other ABC drug transporters at the blood–brain barrier. Trends Pharmacol Sci. 2010;31:246–54.
Cooper SJ, Butler A, Tweed J, Welch C, Raniwalla J. Zotepine in the prevention of recurrence: a randomised, double-blind, placebo-controlled study for chronic schizophrenia. Psychopharmacology. 2000;150:237–43.
Gareri P, De Fazio P, De Fazio S, Marigliano N, Ferreri Ibbadu G, De Sarro G. Adverse effects of atypical antipsychotics in the elderly. Drugs Aging. 2006;23:937–56.
Dalvadi H, Patel N, Parmar K. Systematic development of design of experiments (DoE) optimised self-microemulsifying drug delivery system of Zotepine. J Microencapsul. 2017;34:308–18.
Dhuria SV, Hanson LR, Frey WH. Intranasal delivery to the central nervous system: mechanisms and experimental considerations. J Pharm Sci. 2010;99:1654–73.
Li X, Tsibouklis J, Weng T, Zhang B, Yin G, Feng G, et al. Nano carriers for drug transport across the blood–brain barrier. J Drug Target. 2017;25:17–28.
Miyake MM, Bleier BS. The blood-brain barrier and nasal drug delivery to the central nervous system. Am J Rhinol Allergy. 2015;29:124–7.
Saindane NS, Pagar KP, Vavia PR. Nanosuspension based in situ gelling nasal spray of carvedilol: development, in vitro and in vivo characterization. AAPS PharmSciTech. 2013;14:189–99.
Md S, Khan RA, Mustafa G, Chuttani K, Baboota S, Sahni JK, et al. Bromocriptine loaded chitosan nanoparticles intended for direct nose to brain delivery: Pharmacodynamic, pharmacokinetic and scintigraphy study in mice model. Eur J Pharm Sci. 2013;48:393–405.
Yasir M, Sara U, Som I. Haloperidol loaded solid lipid nanoparticles for nose to brain delivery: stability and in vivo studies. J Nanomed Nanotechnol OMICS International. 2015;01:1–9.
Gabal YM, Kamel AO, Sammour OA, Elshafeey AH. Effect of surface charge on the brain delivery of nanostructured lipid carriers in situ gels via the nasal route. Int J Pharm. 2014;473:442–57.
Shinde RL, Bharkad GP, Devarajan PV. Intranasal microemulsion for targeted nose to brain delivery in neurocysticercosis: role of docosahexaenoic acid. Eur J Pharm Biopharm. 2015;96:363–79.
Giuliani A, Balducci AG, Zironi E, Colombo G, Bortolotti F, Lorenzini L, et al. In vivo nose-to-brain delivery of the hydrophilic antiviral ribavirin by microparticle agglomerates. Drug Deliv Taylor & Francis. 2018;25:376–87.
Bhavna MS, Ali M, Ali R, Bhatnagar A, Baboota S, et al. Donepezil nanosuspension intended for nose to brain targeting: in vitro and in vivo safety evaluation. Int J Biol Macromol. 2014;67:418–25.
Mistry A, Stolnik S, Illum L. Nanoparticles for direct nose-to-brain delivery of drugs. Int J Pharm. 2009;379:146–57.
Keck C, Muller R. Drug nanocrystals of poorly soluble drugs produced by high pressure homogenisation. Eur J Pharm Biopharm. 2006;62:3–16.
Li X-S, Wang J-X, Shen Z-G, Zhang P-Y, Chen J-F, Yun J. Preparation of uniform prednisolone microcrystals by a controlled microprecipitation method. Int J Pharm. 2007;342:26–32.
Van Eerdenbrugh B, Van den Mooter G, Augustijns P. Top-down production of drug nanocrystals: Nanosuspension stabilization, miniaturization and transformation into solid products. Int J Pharm. 2008;364:64–75.
Merisko-Liversidge E, Liversidge GG, Cooper ER. Nanosizing: a formulation approach for poorly-water-soluble compounds. Eur J Pharm Sci Elsevier. 2003;18:113–20.
Kipp J, Wong J, Doty M, Rebbeck C. Microprecipitation method for preparing submicron suspensions. US pat. 6869617. 2001.
Liu D, Xu H, Tian B, Yuan K, Pan H, Ma S, et al. Fabrication of carvedilol nanosuspensions through the anti-solvent precipitation-ultrasonication method for the improvement of dissolution rate and oral bioavailability. AAPS PharmSciTech Springer. 2012;13:295–304.
Shelar DB, Pawar SK, Vavia PR. Fabrication of isradipine nanosuspension by anti-solvent microprecipitation–high-pressure homogenization method for enhancing dissolution rate and oral bioavailability. Drug Deliv Transl Res. 2013;3:384–91.
Gora S, Mustafa G, Sahni JK, Ali J, Baboota S. Nanosizing of valsartan by high pressure homogenization to produce dissolution enhanced nanosuspension: pharmacokinetics and pharmacodyanamic study. Drug Deliv. 2014;23:1–11.
Tang X-J, Fu Y-H, Meng Q-H, Li L-M, Ying X-Y, Han M, et al. Evaluation of pluronic nanosuspensions loading a novel insoluble anticancer drug both in vitro and in vivo. Int J Pharm. 2013;456:243–50.
Guo L, Kang L, Liu X, Lin X, Di D, Wu Y, et al. A novel nanosuspension of andrographolide: preparation, characterization and passive liver target evaluation in rats. Eur J Pharm Sci. 2017;104:13–22.
Aboud HM, Ali AA, El-Menshawe SF, Elbary AA. Nanotransfersomes of carvedilol for intranasal delivery: formulation, characterization and in vivo evaluation. Drug Deliv. 2016;23:2471–81.
K PS, S WK, Kamlesh M, T BD, K JD, Pharmacy C, et al. Development and evaluation of solid lipid nanoparticles containing anti-migraine drug. World J Pharm Sci. 2014;2:1014–21.
Vyas TK, Babbar AK, Sharma RK, Singh S, Misra A. Preliminary brain-targeting studies on intranasal mucoadhesive microemulsions of sumatriptan. AAPS PharmSciTech. 2006;7:E49–57.
Youssef NAHA, Kassem AA, Farid RM, Ismail FA, EL-Massik MAE, Boraie NA. A novel nasal almotriptan loaded solid lipid nanoparticles in mucoadhesive in situ gel formulation for brain targeting: preparation, characterization and in vivo evaluation. Int J Pharm. 2018;548:609–24.
Yasir M, Sara UVS. Solid lipid nanoparticles for nose to brain delivery of haloperidol: in vitro drug release and pharmacokinetics evaluation. Acta Pharm Sin B Elsevier. 2014;4:454–63.
Mahajan HS, Mahajan MS, Nerkar PP, Agrawal A. Nanoemulsion-based intranasal drug delivery system of saquinavir mesylate for brain targeting. Drug Deliv. 2014;21:148–54.
Vyas TK, Shahiwala A, Marathe S, Misra A. Intranasal drug delivery for brain targeting. Curr Drug Deliv. 2005;2:165–75.
Kozlovskaya L, Abou-Kaoud M, Stepensky D. Quantitative analysis of drug delivery to the brain via nasal route. J Control Release. 2014;189:133–40.
Li X, Wang X, Wang L, Xu Y, Cheng X, Wei P. Formulation and pharmacokinetic evaluation of a paclitaxel nanosuspension for intravenous delivery. Int J Nanomedicine. 2011;6:1497–507.
Hong C, Dang Y, Lin G, Yao Y, Li G, Ji G, et al. Effects of stabilizing agents on the development of myricetin nanosuspension and its characterization: an in vitro and in vivo evaluation. Int J Pharm. 2014;477:251–60.
Wang Y, Ma Y, Zheng Y, Song J, Yang X, Bi C, et al. In vitro and in vivo anticancer activity of a novel puerarin nanosuspension against colon cancer, with high efficacy and low toxicity. Int J Pharm. 2013;441:728–35.
Ganta S, Paxton JW, Baguley BC, Garg S. Formulation and pharmacokinetic evaluation of an asulacrine nanocrystalline suspension for intravenous delivery. Int J Pharm. 2009;367:179–86.
Ziller KH, Rupprecht H. Conteol of crystal growth in drug suspensions: 1) Design of a Conteol Unit and Application to acetaminophen suspensions. Drug Dev Ind Pharm Taylor & Francis; 1988;14:2341–70.
Warren DB, Benameur H, Porter CJH, Pouton CW. Using polymeric precipitation inhibitors to improve the absorption of poorly water-soluble drugs: a mechanistic basis for utility. J Drug Target. 2010;18:704–31.
Ali HSM, York P, Blagden N. Preparation of hydrocortisone nanosuspension through a bottom-up nanoprecipitation technique using microfluidic reactors. Int J Pharm. 2009;375:107–13.
Möschwitzer JP. Drug nanocrystals in the commercial pharmaceutical development process. Int J Pharm Elsevier. 2013;453:142–56.
Prakash A, Lamb HM. Zotepine: a review of its pharmacodynamic and pharmacokinetic properties and therapeutic efficacy in the management of schizophrenia. CNS Drugs. 1998;9:280–0.
Noda K, Suzuki A, Okui M, Noguchi H, Nishiura M, Nishiura N. Pharmacokinetics and metabolism of 2-chloro-11-(2-dimethylaminoethoxy)-dibenzo[b,f]thiepine (zotepine) in rat, mouse, dog and man. Arzneimittelforschung. 1979;29:1595–600.
Romeo VD, deMeireles JC, Gries WJ, Xia WJ, Sileno AP, Pimplaskar HK, et al. Optimization of systemic nasal drug delivery with pharmaceutical excipients. Adv Drug Deliv Rev. 1998;29:117–33.
Marttin E, Verhoef JC, Romeijn SG, Merkus FW. Effects of absorption enhancers on rat nasal epithelium in vivo: release of marker compounds in the nasal cavity. Pharm Res. 1995;12:1151–7.
Chaturvedi M, Kumar M, Pathak KA. Review on mucoadhesive polymer used in nasal drug delivery system. J Adv Pharm Technol Res Wolters Kluwer -- Medknow Publications. 2011;2:215–22.
Zhang Q, Jiang X, Jiang W, Lu W, Su L, Shi Z. Preparation of nimodipine-loaded microemulsion for intranasal delivery and evaluation on the targeting efficiency to the brain. Int J Pharm. 2004;275:85–96.
Mistry A, Glud SZ, Kjems J, Randel J, Howard KA, Stolnik S, et al. Effect of physicochemical properties on intranasal nanoparticle transit into murine olfactory epithelium. J Drug Target. 2009;17:543–52.
Acknowledgements
The authors are thankful to NIPER-HYD for providing the facilities and Department of Pharmaceuticals (DoP) for funding the research work.
Author information
Authors and Affiliations
Contributions
SR designed the study, conducted experiments and drafted the manuscript. ST: analytical and bioanalytical method development. NR: reviewed and revised the manuscript. RR: helped in preparation of nanosuspension. VS: supported in oral, intranasal and intravenous dosing and blood collection& brain extraction of all the animals. ND: helped in acute toxicity study. SS: supervision of all the experiments.
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all the authors, we report no conflict of interest.
Human participants and/or animals
Humans are not involved in the study. Wistar rats were used in pharmacokinetics and toxicity study. The animal protocol (NIP/8/2016/PE/203) was approved by Institutional Animal Ethical Committee (IAEC) for Care and Use of Laboratory animals and the Committee for the Purpose of Control and Supervision of Experiments on Animals (CPCSEA).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Pailla, S.R., Talluri, S., Rangaraj, N. et al. Intranasal Zotepine Nanosuspension: intended for improved brain distribution in rats. DARU J Pharm Sci 27, 541–556 (2019). https://doi.org/10.1007/s40199-019-00281-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40199-019-00281-4