Abstract
Purpose
Candidemia is a highly lethal infection; several scores have been developed to assist the diagnosis process and recently different models have been proposed. Aim of this work was to assess predictive performance of a Random Forest (RF) algorithm for early detection of candidemia in the internal medical wards (IMWs).
Methods
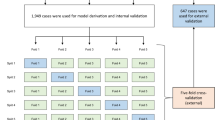
A set of 42 potential predictors was acquired in a sample of 295 patients (male: 142, age: 72 ± 15 years; candidemia: 157/295; bacteremia: 138/295). Using tenfold cross-validation, a RF algorithm was compared with a classic stepwise multivariable logistic regression model; discriminative performance was assessed by C-statistics, sensitivity and specificity, while calibration was evaluated by Hosmer–Lemeshow test.
Results
The best tuned RF algorithm demonstrated excellent discrimination (C-statistics = 0.874 ± 0.003, sensitivity = 84.24% ± 0.67%, specificity = 91% ± 2.63%) and calibration (Hosmer–Lemeshow statistics = 12.779 ± 1.369, p = 0.120), markedly greater than the ones guaranteed by the classic stepwise logistic regression (C-statistics = 0.829 ± 0.011, sensitivity = 80.21% ± 1.67%, specificity = 84.81% ± 2.68%; Hosmer–Lemeshow statistics = 38.182 ± 15.983, p < 0.001). In addition, RF suggests a major role of in-hospital antibiotic treatment with microbioma highly impacting antimicrobials (MHIA) that are found as a fundamental risk of candidemia, further enhanced by TPN. When in-hospital MHIA therapy is not performed, PICC is the dominant risk factor for candidemia, again enhanced by TPN. When PICC is not used and MHIA therapy is not performed, the risk of candidemia is minimum, slightly increased by in-hospital antibiotic therapy.
Conclusion
RF accurately estimates the risk of candidemia in patients admitted to IMWs. Machine learning technique might help to identify patients at high risk of candidemia, reduce the delay in empirical treatment and improve appropriateness in antifungal prescription.


Similar content being viewed by others
References
Wisplinghoff H, Bischoff T, Tallent SM, Seifert H, Wenzel RP, Edmond MB. Nosocomial bloodstream infections in US hospitals: analysis of 24,179 cases from a prospective nationwide surveillance study. Clin Infect Dis. 2004;39:309–17.
Marchetti O, Bille J, Fluckiger U, et al. Epidemiology of candidaemia in Swiss tertiary care hospitals: secular trends, 1991–2000. Clin Infect Dis. 2004;38:311–20.
Morrell M, Fraser VJ, Kollef MH. Delaying the empiric treatment of Candida bloodstream infection until positive blood culture results are obtained: a potential risk factor for hospital mortality. Antimicrob Agents Chemother. 2005;49:3640–5.
Zimlichman E, Henderson D, Tamir O, et al. Health care-associated infections: a meta-analysis of costs and financial impact on the US health care system. JAMA Intern Med. 2013;173:2039–46.
Cleveland AA, Farley MM, Harrison LH, et al. Changes in incidence and antifungal drug resistance in candidemia: results from population-based laboratory surveillance in Atlanta and Baltimore, 2008–2011. Clin Infect Dis. 2012;55:1352–61.
Zaoutis TE, Argon J, Chu J, Berlin JA, Walsh TJ, Feudtner C. The epidemiology and attributable outcomes of candidemia in adults and children hospitalized in the United States: a propensity analysis. Clin Infect Dis. 2005;41:1232–9.
Wey SB, Mori M, Pfaller MA, Woolson RF, Wenzel RP. Hospitalacquired candidemia. The attributable mortality and excess length of stay. Arch Intern Med. 1988;148:2642–5.
Pfaller MA, Diekema DJ. Epidemiology of invasive candidiasis: a persistent public health problem. Clin Microbiol Rev. 2007;20:133–63.
Puig-Asensio M, Padilla B, Garnacho-Montero J, et al. Epidemiology and predictive factors for early and late mortality in Candida bloodstream infections: a population-based surveillance in Spain. Clin Microbiol Infect. 2014;20:245–54.
Bassetti M, Merelli M, Righi E, et al. Epidemiology, species distribution, antifungal susceptibility, and outcome of Candidemia across five sites in Italy and Spain. J Clin Microbiol. 2013;51:4167–72.
Bassetti M, Taramasso L, Nicco E, Molinari MP, Mussap M, Viscoli C. Epidemiology. Species distribution, antifungal susceptibility and outcome of nosocomial Candidemia in a Tertiary Care Hospital in Italy. PLoS ONE. 2011;6:e24198.
Tascini C, Sozio E, Salini N, Sbrana F, Ripoli A, Viaggi B, Malacarne P. Risk factors for candidaemia in critically ill patients in intensive care units as compared to internal medicine wards. Infect Dis (Lond). 2017;49:153–4.
Luzzati R, Merelli M, Ansaldi F, et al. Nosocomial candidemia in patients admitted to medicine wards compared to other wards: a multicentre study. Infection. 2016;44:747–55.
Tascini C, Falcone M, Bassetti M, De Rosa FG, Sozio E, Russo A, Sbrana F, Ripoli A, Merelli M, Scarparo C, Carmassi F, Venditti M, Menichetti F. Candidemia in patients with body temperature below 37 °C and admitted to internal medicine wards: assessment of risk factors. Am J Med. 2016;129:e1–e6.
Hsu DI, Nguyen M, Nguyen LA. Multicentre study to evaluate the impact of timing of caspofungin administration on outcomes of invasive candidiasis in non-immunocompromised adult patients. J Antimicrob Chemother. 2010;65:1765–70.
Milazzo L, Peri AM, Mazzali C, et al. Candidaemia observed at university hospital in Milan (northern Italy) and review of published studies from 2010 to 2014. Mycopathologia. 2014;178:227–41.
Luzzati R, Cavinato S, Giangreco M, et al. Peripheral and total parenteral nutrition as the strongest risk factors for nosocomial candidemia in elderly patients: a matched case–control study. Mycoses. 2013;56:664–71.
Horn DL, Neofytos D, Anaissie EJ, Fishman JA, Steinbach WJ, Olyaei AJ, Marr KA, Pfaller MA, Chang CH, Webster KM. Epidemiology and outcomes of candidemia in 2019 patients: data from the prospective antifungal therapy alliance registry. Clin Infect Dis. 2009;48:1695–703.
Bassetti M, Molinari MP, Mussap M, Viscoli C, Righi E. Candidaemia in internal medicine departments: the burden of a rising problem. Clin Microbiol Infect. 2013;19:E281–E284284.
De Rosa FG, Trecarichi EM, Montrucchio C, Losito AR, Raviolo S, Posteraro B, Corcione S, Di Giambenedetto S, Fossati L, Sanguinetti M, Serra R, Cauda R, Di Perri G, Tumbarello M. Mortality in patients with early-or late-onset candidaemia. J Antimicrob Chemother. 2013;68:927–35.
León C, Ruiz-Santana S, Saavedra P, et al. A bedside scoring system (“Candida score”) for early antifungal treatment in nonneutropenic critically ill patients with Candida colonization. Crit Care Med. 2006;34:730–7.
Ostrosky-Zeichner L, Sabel C, Sobel J, et al. Multicenter retrospective development and validation of a clinical prediction rule for nosocomial invasive candidiasis in the intensive care setting. Eur J Clin Microbiol Infect Dis. 2007;26:271–6.
Paphitou NI, Ostrosky-Zeichner L, Rex JH. Rules for identifying patients at increased risk for candidal infections in the surgical intensive care unit: approach to developing practical criteria for systematic use in antifungal prophylaxis trials. Med Mycol. 2005;43:235–43.
Pittet D, Monod M, Suter PM, Frenk E, Auckenthaler R. Candida colonization and subsequent infections in critically ill surgical patients. Ann Surg. 1994;220:751–8.
Faiz S, Neale B, Rios E, et al. Risk-based fluconazole prophylaxis of Candida bloodstream infection in a medical intensive care unit. Eur J Clin Microbiol Infect Dis. 2009;28:689–92.
Sozio E, et al. A prediction rule for early recognition of patients with candidemia in Internal Medicine: results from an Italian, multicentric, case-control study. Infection. 2018;46:625–33.
Ruiz-Ruigómez M, Dueñas C, Hernandez C, Vinuesa D, Coronado-Álvarez NM, Portillo-Tuñón V, Cardozo C, Muñoz-Medina L, Cabo-Magadán R, Luna JD, Mensa J, Parra-Ruiz J. Clinical predictors of candidemia in medical non-neutropenic, non-ICU patients. The CaMed score. Int J Clin Pract. 2018;72:e13275.
Atamna A, Eliakim-Raz N, Mohana J, Ben-Zvi H, Sorek N, Shochat T, Bishara J. Predicting candidemia in the internal medicine wards: a comparison with gram-negative bacteremia-a retrospectives study. Diagn Microbiol Infect Dis. 2019;95:80–3.
Goldstein BA, Navar AM, Carter RE. Moving beyond regression techniques in cardiovascular risk prediction: applying machine learning to address analytic challenges. Eur Heart J. 2017;38:1805–14.
Deo RC. Machine learning in medicine. Circulation. 2015;132:1920–30.
Malley JD, Kruppa J, Dasgupta A, Malley KG, Ziegler A. Probability machines: consistent probability estimation using nonparametric learning machines. Methods Inf Med. 2012;51:74–81.
Dellinger RP, Levy MM, Rhodes A, et al. Surviving sepsis campaign: international guidelines for management of severe sepsis and septic shock. Intensive Care Med. 2013;39:165–228.
Efron B, Hastie T. Computer age statistical inference. Cambridge: Cambridge University Press; 2017.
Breiman L. Random forest. Mach Learn. 2001;45:5–32.
Kursa M, Rundnicki W. Feature selection with the Boruta package. J Stat Softw. 2010;36:1–13.
Hosmer D, Lemeshow S. Goodness of fit tests for the multiple logistic regression model. Commun Stat Theory Methods. 1980;9:1043–69.
R Core Team. R: a language and environment for statistical computing. R Foundation for Statistical Computing. Vienna, Austria; 2018; https://www.R-project.org/.
Falagas ME, Apostolou KE, Pappas VD. Attributable mortality of candidemia: a systematic review of matched cohort and case-control studies. Eur J Clin Microbiol Infect Dis. 2006;25:419–25.
Falcone M, Tiseo G, Tascini C, Russo A, Sozio E, Raponi G, Rosin C, Pignatelli P, Carfagna P, Farcomeni A, Luzzati R, Violi F, Menichetti F, Venditti M. Assessment of risk factors for candidemia in non-neutropenic patients hospitalized in internal medicine wards: a multicenter study. Eur J Intern Med. 2017;41:33–8.
Peres-Bota D, Rodriguez-Villalobos H, Dimopoulos G, Melot C, Vincent JL. Potential risk factors for infection with Candida spp. in critically ill patients. Clin Microbiol Infect. 2004;10:550–5.
Wenzel RP. Nosocomial candidemia: risk factors and attributable mortality. Clin Infect Dis. 1995;20:1531–4.
Tascini C, Sozio E, Tintori G, Ripoli A, Sbrana F, Rosselli Del Turco E, Bertolino G, Fortunato S, Carmassi F, Cardinali G, Menichetti F. Peripherally inserted central catheter as a predominant risk factor for candidemia in critically ill patients in Internal Medicine wards in Italy. Intensive Care Med. 2015;41:1498–9.
De Rosa FG, Corcione S, Pagani N, Di Perri G. From ESKAPE to ESCAPE, from KPC to CCC. Clin Infect Dis. 2015;60:1289–90.
McClave SA, Martindale RG, Rice TW, Heyland DK. Feeding the critically ill patient. Crit Care Med. 2014;42:2600–10.
Shin JH, Kee SJ, Shin MG, Kim SH, Shin DH, Lee SK, Suh SP, Ryang DW. Biofilm production by isolates of Candida species recovered from nonneutropenic patients: comparison of bloodstream isolates with isolates from other sources. J Clin Microbiol. 2002;40:1244–8.
Branchini ML, Pfaller MA, Rhine-Chalberg J, Frempong T, Isenberg HD. Genotypic variation and slime production among blood and catheter isolates of Candida parapsilosis. J Clin Microbiol. 1994;32:452–6.
Swindell K, Lattif AA, Chandra J, Mukherjee PK, Ghannoum MA. Parenteral lipid emulsion induces germination of Candida albicans and increases biofilm formation on medical catheter surfaces. J Infect Dis. 2009;200:473–80.
Pappo I, Polacheck I, Zmora O, Feigin E, Freund HR. Altered gut barrier function to Candida during parenteral nutrition. Nutrition. 1994;10:151–4.
Menichetti F, Bertolino G, Sozio E, Carmignani C, Rosselli Del Turco E, Tagliaferri E, Sbrana F, Ripoli A, Barnini S, Desideri I, Dal Canto L, Tascini C, GISA (Italian Group for Antimicrobial Stewardship) Candidemia Study Group. Impact of infectious diseases consultation as a part of an antifungal stewardship programme on candidemia outcome in an Italian tertiary-care University hospital. J Chemother. 2018;30:304–9.
Vellido A, Ribas V, Morales C, Ruiz Sanmartín A, Ruiz Rodríguez JC. Machine learning in critical care: state-of-the-art and a sepsis case study. Biomed Eng Online. 2018;17:135.
Peiffer-Smadja N, Rawson TM, Ahmad R, Buchard A, Pantelis G, Lescure FX, Birgand G, Holmes AH. Machine learning for clinical decision support in infectious diseases: a narrative review of current applications. Clin Microbiol Infect. 2019. https://doi.org/10.1016/j.cmi.2019.09.009.
Acknowledgements
None.
Funding
The project was partially funded with Digital Health Program 2017 funds—Gilead Sciences Srl.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by CT, AR, ES, GB, FS and GC. The first draft of the manuscript was written by AR and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
C.T. has received funds for speaking at symposia organized on behalf of Pfizer, Novartis, Merck, Angelini, Zambon, Thermofischer, Biotest, Gilead, Hikma, Biomerieux and Astellas. G.C. received a prize from GILEAD. No Conflict of Interest for the other authors.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ripoli, A., Sozio, E., Sbrana, F. et al. Personalized machine learning approach to predict candidemia in medical wards. Infection 48, 749–759 (2020). https://doi.org/10.1007/s15010-020-01488-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-020-01488-3