Abstract
Background
Streptococci involved in infective endocarditis (IE) primarily comprise alpha- or non-hemolytic streptococci (ANHS). Moreover, beta-hemolytic streptococci (BHS) can be involved, and guidelines recommend the addition of gentamicin for the first 2 weeks of treatment and the consideration of early surgery in such cases. This study compared the morbidity and mortality associated with IE depending on the microorganisms involved (BHS, ANHS, staphylococci, and enterococci).
Methods
We conducted a retrospective observational study between 2012 and 2017 in a single hospital in France. The endpoints were overall in-hospital mortality, 1-year mortality and the occurrence of complications.
Results
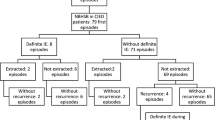
We analyzed 316 episodes of definite IE including 150 (38%), 96 (25%), 46 (12%), and 24 cases (6%) of staphylococcal, ANHS, enterococcal, and BHS IE, respectively. In-hospital mortality was significantly higher in the staphylococcal (n = 40; 26.7%) and BHS groups (n = 6; 25.0%) than in the ANHS (n = 9; 9.4%) and enterococcal groups (n = 5; 10.9%) (all p < 0.01). The rates of septic shock and cerebral emboli were also higher in the BHS group than in the ANHS group [n = 7 (29.2%) vs. n = 3 (3.1%), p < 0.001; n = 7 (29.2%) vs. n = 12 (12.5%); p = 0.05, respectively].
Conclusion
This study confirmed that BHS IE has a more severe prognosis than ANHS IE. The virulence of BHS may be similar to that of staphylococci, justifying increased monitoring of these patients and more ‘aggressive’ treatments such as early surgery.

Similar content being viewed by others
References
Slipczuk L, Codolosa JN, Davila CD, Romero-Corral A, Yun J, Pressman GS, et al. Infective endocarditis epidemiology over five decades: a systematic review. PLoS One. 2013;8:e82665.
Duval X, Delahaye F, Alla F, Tattevin P, Obadia J-F, Le Moing V, et al. Temporal trends in infective endocarditis in the context of prophylaxis guideline modifications: three successive population-based surveys. J Am Coll Cardiol. 2012;59:1968–76.
Sy RW, Kritharides L. Health care exposure and age in infective endocarditis: results of a contemporary population-based profile of 1536 patients in Australia. Eur Heart J. 2010;31:1890–7.
Murdoch DR, Corey GR, Hoen B, Miró JM, Fowler VG, Bayer AS, et al. Clinical presentation, etiology and outcome of infective endocarditis in the 21st century: the international collaboration on endocarditis-prospective cohort study. Arch Intern Med. 2009;169:463–73.
Habib G, Lancellotti P, Antunes MJ, Bongiorni MG, Casalta J-P, Del Zotti F, et al. ESC guidelines for the management of infective endocarditis: the Task Force for the Management of Infective Endocarditis of the European Society of Cardiology (ESC). Endorsed by: European Association for Cardio-Thoracic Surgery (EACTS), the European Association of Nuclear Medicine (EANM). Eur Heart J. 2015;36:3075–128.
Baddour LM, Wilson WR, Bayer AS, Fowler VG, Tleyjeh IM, Rybak MJ, et al. Infective endocarditis in adults: diagnosis, antimicrobial therapy, and management of complications: a scientific statement for healthcare professionals from the american heart association. Circulation. 2015;132:1435–86.
Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M, et al. The third international consensus definitions for sepsis and septic shock (sepsis-3). JAMA. 2016;315:801–10.
Baddour LM. Infective endocarditis caused by beta-hemolytic streptococci. The infectious diseases society of America’s emerging infections network. Clin Infect Dis. 1998;26:66–71.
Lefort A, Lortholary O, Casassus P, Selton-Suty C, Guillevin L, Mainardi J-L, et al. Comparison between adult endocarditis due to beta-hemolytic streptococci (serogroups A, B, C, and G) and Streptococcus milleri: a multicenter study in France. Arch Intern Med. 2002;162:2450–6.
Ekelund K, Skinhøj P, Madsen J, Konradsen HB. Invasive group A, B, C and G streptococcal infections in Denmark 1999–2002: epidemiological and clinical aspects. Clin Microbiol Infect. 2005;11:569–76.
Rantala S, Vuopio-Varkila J, Vuento R, Huhtala H, Syrjänen J. Clinical presentations and epidemiology of beta-haemolytic streptococcal bacteraemia: a population-based study. Clin Microbiol Infect. 2009;15:286–8.
Oppegaard O, Mylvaganam H, Kittang BR. Beta-haemolytic group A, C and G streptococcal infections in Western Norway: a 15-year retrospective survey. Clin Microbiol Infect. 2015;21:171–8.
El Rafei A, DeSimone DC, DeSimone CV, Lahr BD, Steckelberg JM, Sohail MR, et al. Beta-haemolytic streptococcal endocarditis: clinical presentation, management and outcomes. Infect Dis. 2016;48:373–8.
Sambola A, Miro JM, Tornos MP, Almirante B, Moreno-Torrico A, Gurgui M, et al. Streptococcus agalactiae infective endocarditis: analysis of 30 cases and review of the literature, 1962–1998. Clin Infect Dis. 2002;34:1576–84.
Rollán MJ, San Román JA, Vilacosta I, Sarriá C, López J, Acuña M, et al. Clinical profile of Streptococcus agalactiae native valve endocarditis. Am Heart J. 2003;146:1095–8.
Ivanova-Georgieva R, Ruiz-Morales J, García-Cabrera E, García-López MV, Gálvez-Acebal J, Plata-Ciezar A, et al. Left-sided infective endocarditis caused by Streptococcus agalactiae: rare and serious. Eur J Clin Microbiol Infect Dis. 2019;38:265–75.
Olmos C, Vilacosta I, Sarriá C, López J, Ferrera C, Sáez C, et al. Streptococcus bovis endocarditis: update from a multicenter registry. Am Heart J. 2016;171:7–13.
Bläckberg A, Nilson B, Özenci V, Olaison L, Rasmussen M. Infective endocarditis due to Streptococcus dysgalactiae: clinical presentation and microbiological features. Eur J Clin Microbiol Infect Dis. 2018;37:2261–72.
Wang A, Athan E, Pappas PA, Fowler VG, Olaison L, Paré C, et al. Contemporary clinical profile and outcome of prosthetic valve endocarditis. JAMA. 2007;297:1354–61.
Mahesh B, Angelini G, Caputo M, Jin XY, Bryan A. Prosthetic valve endocarditis. Ann Thorac Surg. 2005;80:1151–8.
Sendi P. Infective endocarditis caused by Streptococcus agalactiae: time for beta-hemolytic streptococci to follow treatment recommendations for S. aureus? Eur J Clin Microbiol Infect Dis. 2019;38:419–22.
Selton-Suty C, Célard M, Le Moing V, Doco-Lecompte T, Chirouze C, Iung B, et al. Preeminence of Staphylococcus aureus in infective endocarditis: a 1-year population-based survey. Clin Infect Dis. 2012;54:1230–9.
Day MD, Gauvreau K, Shulman S, Newburger JW. Characteristics of children hospitalized with infective endocarditis. Circulation. 2009;119:865–70.
Weidman DR, Al-Hashami H, Morris SK. Two cases and a review of Streptococcus pyogenes endocarditis in children. BMC Pediatr. 2014;14:227.
Chu VH, Park LP, Athan E, Delahaye F, Freiberger T, Lamas C, et al. Association between surgical indications, operative risk, and clinical outcome in infective endocarditis: a prospective study from the International Collaboration on Endocarditis. Circulation. 2015;131:131–40.
Acknowledgements
We thank François Lefebvre for his help in the statistical analysis. The authors would like to thank Enago (www.enago.com) for the English language review.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
YR, XA, and YH designed the study. YR, XA, YH, AM, NL, ND, and JPM collected the data. YR and XA analyzed the data. PR analyzed the microbiological data. YR performed the statistical analysis. YR and XA wrote the manuscript. All authors reviewed, revised, and approved the final report.
Corresponding author
Ethics declarations
Conflict of interest
There are no reported conflicts of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ruch, Y., Hansmann, Y., Riegel, P. et al. Virulence of beta-hemolytic streptococci in infective endocarditis. Infection 48, 91–97 (2020). https://doi.org/10.1007/s15010-019-01358-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-019-01358-7