Abstract
Purpose
In recent years antifungal stewardship (AFS) programmes have been increasingly recommended to provide optimal antifungal treatment. In a previous study (study I) in the department of haematology and oncology of a German tertiary care hospital we found areas for improvement concerning antifungal prescription. Subsequently, AFS measures were implemented and their impact on quality of antifungal use was assessed in this study.
Methods
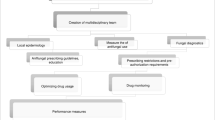
AFS measures included medical training (two sessions), a pocket card summarising main recommendations for antifungal use, and daily pharmaceutical counselling on the ward. In a 6-month observational study, antifungal prescriptions were analysed and compared to the previously collected data (study I) concerning indication, choice of drug, dosing, duration and drug–drug interactions. The study was approved by the university hospital ethical review board.
Results
Antifungal agents were prescribed for 103/1169 inpatients. Compared to study I, a significant increase in dosage accuracy (+ 19.3%; p < 0.05) and correct choice of drug (+ 15.9%; p < 0.05) was noted, as well as a decrease in potential clinically relevant drug–drug interactions with concomitant medication (− 13.9%; p < 0.05). However, no significant improvement in indication and duration of antifungal treatment was identified. 56 recommendations were given to the prescribing physicians (acceptance rate: 66.1%).
Conclusions
The implementation of AFS interventions based on pharmaceutical presence on the ward was associated with an improvement in antifungal use; however, indication and duration of therapy need to be communicated by infectious disease specialists. Considering the proportionally short observation period, the long-term effects of our AFS interventions need to be further investigated.


Similar content being viewed by others
References
Colombo AL, de Almeida Junior JN, Slavin MA, Chen SC, Sorrell TC. Candida and invasive mould diseases in non-neutropenic critically ill patients and patients with haematological cancer. Lancet Infect Dis. 2017;17:e344-e56.
Martino R, Subira M. Invasive fungal infections in hematology: new trends. Ann Hematol. 2002;81:233–43.
Pagano L, Caira M, Nosari A, Van Lint MT, Candoni A, Offidani M, et al. Fungal infections in recipients of hematopoietic stem cell transplants: results of the SEIFEM B-2004 study. Clin Infect Dis. 2007;45:1161–70.
Koehler P, Hamprecht A, Bader O, Bekeredjian-Ding I, Buchheidt D, Doelken G, et al. Epidemiology of invasive aspergillosis and azole resistance in patients with acute leukaemia: the SEPIA Study. Int J Antimicrob Agents. 2017;49:218–23.
Teng JC, Slavin MA, Teh BW, Lingaratnam SM, Ananda-Rajah MR, Worth LJ, et al. Epidemiology of invasive fungal disease in lymphoproliferative disorders. Haematologica. 2015;100:e462-6.
Pagano L, Caira M, Candoni A, Offidani M, Fianchi L, Martino B, et al. The epidemiology of fungal infections in patients with hematologic malignancies: the SEIFEM-2004 study. Haematologica. 2006;91:1068–75.
Rieger CT, Cornely OA, Hoppe-Tichy T, Kiehl M, Knoth H, Thalheimer M, et al. Treatment cost of invasive fungal disease (Ifd) in patients with acute myelogenous leukaemia (Aml) or myelodysplastic syndrome (Mds) in German hospitals. Mycoses. 2012;55:514–20.
Auberger J, Lass-Florl C, Aigner M, Clausen J, Gastl G, Nachbaur D. Invasive fungal breakthrough infections, fungal colonization and emergence of resistant strains in high-risk patients receiving antifungal prophylaxis with posaconazole: real-life data from a single-centre institutional retrospective observational study. J Antimicrob Chemother. 2012;67:2268–73.
Perlin DS, Rautemaa-Richardson R, Alastruey-Izquierdo A. The global problem of antifungal resistance: prevalence, mechanisms, and management. Lancet Infect Dis. 2017;17:e383–e92.
Padovani de Souza MC, Dos Santos AG, Moreira Reis AM. Adverse drug reactions in patients receiving systemic antifungal therapy at a high-complexity hospital. J Clin Pharmacol. 2016;56:1507–15.
Gedik H. The expenditures related to the use of antifungal drugs in patients with hematological cancers: a cost analysis. CEOR. 2015;7:537–43.
Lachenmayr SJ, Berking S, Horns H, Strobach D, Ostermann H, Berger K. Antifungal treatment in haematological and oncological patients: need for quality assessment in routine care. Mycoses. 2018;61:464–71.
de With K, Allerberger F, Amann S, Apfalter P, Brodt HR, Eckmanns T, et al. Strategies to enhance rational use of antibiotics in hospital: a guideline by the German Society for Infectious Diseases. Infection. 2016;44:395–439.
Ananda-Rajah MR, Slavin MA, Thursky KT. The case for antifungal stewardship. Curr Opin Infect Dis. 2012;25:107–15.
Munoz P, Bouza E. The current treatment landscape: the need for antifungal stewardship programmes. J Antimicrob Chemother. 2016;71:ii5–12.
Valerio M, Muñoz P, Rodríguez-González C, Sanjurjo M, Guinea J, Bouza E, et al. Training should be the first step toward an antifungal stewardship program. Enferm Infecc Microbiol Clin. 2015;33:221–7.
Mondain V, Lieutier F, Hasseine L, Gari-Toussaint M, Poiree M, Lions C, et al. A 6-year antifungal stewardship programme in a teaching hospital. Infection. 2013;41:621–8.
Ruhnke M. Antifungal stewardship in invasive Candida infections. Clin Microbiol Infect. 2014;20:11–8.
De Pauw B, Walsh TJ, Donnelly JP, Stevens DA, Edwards JE, Calandra T, et al. Revised definitions of invasive fungal disease from the European Organization for Research and Treatment of Cancer/Invasive Fungal Infections Cooperative Group and the National Institute of Allergy and Infectious Diseases Mycoses Study Group (EORTC/MSG) Consensus Group. Clin Infect Dis. 2008;46:1813–21.
Lopez-Medrano F, Juan RS, Lizasoain M, Catalan M, Ferrari JM, Chaves F, et al. A non-compulsory stewardship programme for the management of antifungals in a university-affiliated hospital. Clin Microbiol Infect. 2013;19:56–61.
Dodds-Ashley E. Management of drug and food interactions with azole antifungal agents in transplant recipients. Pharmacotherapy. 2010;30:842–54.
Bruggemann RJ, Alffenaar JW, Blijlevens NM, Billaud EM, Kosterink JG, Verweij PE, et al. Clinical relevance of the pharmacokinetic interactions of azole antifungal drugs with other coadministered agents. Clin Infect Dis. 2009;48:1441–58.
Haouala A, Widmer N, Duchosal MA, Montemurro M, Buclin T, Decosterd LA. Drug interactions with the tyrosine kinase inhibitors imatinib, dasatinib, and nilotinib. Blood. 2011;117:e75–87.
Acknowledgements
This work was supported by the interprofessional PhD-programme Clinical Pharmacy, LMU Munich.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Rights and permissions
About this article
Cite this article
Lachenmayr, S.J., Strobach, D., Berking, S. et al. Improving quality of antifungal use through antifungal stewardship interventions. Infection 47, 603–610 (2019). https://doi.org/10.1007/s15010-019-01288-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-019-01288-4