Abstract
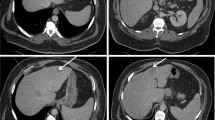
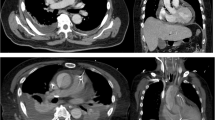
A mycotic aneurysm caused by a Clostridium septicum is a rare infection and has a strong association with colorectal cancer. If left untreated, the mortality rate of the first 24 h is high. This case report discusses the optimal treatment of emergency surgery combined with antibiotic treatment to improve survival. We present a fatal case of a 71-year-old male with abscedation of a caecal carcinoma who shortly after developed a mycotic aneurysm of the infrarenal aorta as a result of a C. septicum infection.


Similar content being viewed by others
References
Bodey GP, Rodriguez S, Fainstein V, Elting LS. Clostridial bacteremia in cancer patients. A 12-year experience. Cancer. 1991;67:1928–42.
Smith-Slatas CL, Bourque M, Salazar JC. Clostridium septicum infections in children: a case report and review of the literature. Pediatrics. 2006;117:796–805.
Kopliku FA, Schubert AM, Mogle J, Schloss PD, Young VB, Aronoff DM. Low prevalence of Clostridium septicum fecal carriage in an adult population. Anaerobe. 2015;32:34–6.
Kennedy CL, Krejany EO, Young LF, O’Connor JR, Awad MM, Boyd RL, et al. The alpha-toxin of Clostridium septicum is essential for virulence. Mol Microbiol. 2005;57:1357–66.
Kennedy CL, Lyras D, Cordner LM, Melton-Witt J, Emmins JJ, Tweten RK, et al. Pore-forming activity of alpha-toxin is essential for Clostridium septicum-mediated myonecrosis. Infect Immun. 2009;77:943–51.
Schaaf RE, Jacobs N, Kelvin FM, Gallis HA, Akwari O, Thompson WM. Clostridium septicum infection associated with colonic carcinoma and hematologic abnormality. Radiology. 1980;137:625–27.
Seder CW, Kramer M, Long G, Uzieblo MR, Shanley CJ, Bove P. Clostridium septicum aortitis: report of two cases and review of the literature. J Vasc Surg. 2009;49:1304–09.
Jendrzejewski JW, Jones SR, Newcombe RL, Gilbert DN. Nontraumatic clostridial myonecrosis. Am J Med. 1978;65:542–6.
Ito F, Inokuchi R, Matsumoto A, Kumada Y, Yokoyama H, Ishida T, et al. Presence of periaortic gas in Clostridium septicum-infected aortic aneurysm aids in early diagnosis: a case report and systematic review of the literature. J Med Case Rep. 2017. https://doi.org/10.1186/s13256-017-1422-0.
Kornbluth AA, Danzig JB, Bernstein LH. Clostridium septicum infection and associated malignancy. Report of 2 cases and review of the literature. Medicine (Baltim). 1989;68:30–7.
Alimi Y, Sosin M, Borsinger TM, et al. Implications of Clostridium septicum in vascular surgery: a case report and outcomes literature review. Ann Vasc Surg. 2017 Aug;43:314.e5–314.e11.
Müller BT, Wegener OR, Grabitz K, Pillny M, Thomas L, Sandmann W, et al. Mycotic aneurysms of the thoracic and abdominal aorta and iliac arteries: experience with anatomic and extraanatomic repair in 33 cases. J Vasc Surg. 2001;33:106–13.
Ting AC, Cheng SW, Ho P, Poon JT, Tsu JH. Surgical treatment of infected aneurysms and pseudoaneurysms of the thoracic and abdominal aorta. Am J Surg. 2005;189:150–4.
Hernandez-Richter T, Schardey HM, Wittmann F, Mayr S, Schmitt-Sody M, Blasenbreu S, et al. Rifampin and Triclosan but not silver is effective in preventing bacterial infection of vascular dacron graft material. Eur J Vasc Endovasc Surg. 2003;26:550–7.
Young RM, Cherry KJ Jr, Davis PM, Gloviczki P, Bower TC, Panneton JM, et al. The results of in situ prosthetic replacement for infected aortic grafts. Am J Surg. 1999;178:136–40.
Weis-Muller BT, Rascanu C, Sagban A, Grabitz K, Godehardt E, Sandmann W. Single-center experience with open surgical treatment of 36 infected aneurysms of the thoracic, thoracoabdominal, and abdominal aorta. Ann Vasc Surg. 2011;25:1020–5.
Stevens DL, Aldape MJ, Bryant AE. Life-threatening clostridial infections. Anaerobe. 2012;18(2):254–9.
Stevens DL, Laine BM, Mitten JE. Comparison of single and combination antimicrobial agents for prevention of experimental gas gangrene caused by Clostridium perfringens. Antimicrob Agents Chemother. 1987;31:312–6.
Stevens DL, Maier KA, Mitten JE. Effect of antibiotics on toxin production and viability of Clostridium perfringens. Antimicrob Agents Chemother. 1987;31:213–8.
Stevens DL, Bryant AE, Hackett SP. Antibiotic effects on bacterial viability, toxin production, and host response. Clin Infect Dis. 1995;20:154–7.
Hollier LH, Money SR, Creely B, Bower TC, Kazmier FJ. Direct replacement of mycotic thoracoabdominal aneurysms. J Vasc Surg. 1993;18:477–84.
Chan FY, Crawford ES, Coselli JS, Safi HJ, Williams TW Jr. In situ prosthetic graft replacement for mycotic aneurysm of the aorta. Ann Thorac Surg. 1989;47:193–203.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Rights and permissions
About this article
Cite this article
Ramphal, W., Raaijmakers, N.J., van der Klift, M. et al. Mycotic aneurysm caused by Clostridium septicum in a patient with colorectal cancer. Infection 46, 711–716 (2018). https://doi.org/10.1007/s15010-018-1155-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-018-1155-z