Abstract
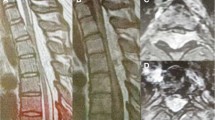
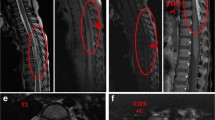
Spinal epidural angiolipomas are rare lesions composed of mature lipomatous and angiomatous elements. In this paper, the authors review a surgical series of ten patients with epidural angiolipomas. All patients had performed preoperative and postoperative magnetic resonance imaging. The diagnosis of angiolipoma was based on pathology. All the follow-up data were obtained during office visits. There were 5 males and 5 females with a mean age of 53.6 years. One tumor was located in the cervicothoracic, six in the thoracic, and three in the lumbar spine. The most common symptom was progressive motor deficit. Gross total resection of the tumor was achieved in nine cases, and subtotal resection was obtained in one case. No recurrence or regrowth of the residual tumor was observed during a follow-up period of 50.8 months. At the last follow-up, 90% of patients experienced improvement in the neurological function. Epidural angiolipomas are benign but clinically progressive lesions. Early surgery should be performed to prevent irreversible neurological deficits. Postoperative radiotherapy is not recommended. The risk of long-term recurrence/regrowth of the lesions is low, and a good clinical outcome after total or subtotal removal can be expected.




Similar content being viewed by others
References
Garg A, Gupta V, Gaikwad S, Deol P, Mishra NK, Sharma MC, Vaish S (2002) Spinal angiolipoma: report of three cases and review of MRI features. Australas Radiol 46:84–90
Nadi MM, Nadi AM, Zabara MY, Ahmad TM (2015) Management of infiltrating spinal epidural angiolipoma. Neurosciences (Riyadh) 20:159–163
Kitagawa Y, Miyamoto M, Konno S, Makino A, Maruyama G, Takai S, Higashi N (2014) Subcutaneous angiolipoma: magnetic resonance imaging features with histological correlation. J Nippon Med Sch 281:313–319
Gelabert-González M, García-Allut A (2009) Spinal extradural angiolipoma: report of two cases and review of the literature. Eur Spine J 18:324–335
Labram EK, el-Shunnar K, Hilton DA, Robertson NJ (1999) Revisited: spinal angiolipoma–three additional cases. Br J Neurosurg 13:25–29
Akhaddar A, Albouzidi A, Elmostarchid B, Gazzaz M, Boucetta M (2008) Sudden onset of paraplegia caused by hemorrhagic spinal epidural angiolipoma. A case report. Eur Spine J 17(Suppl 2):S296–S298
Andaluz N, Balko G, Bui H, Zuccarello M (2000) Angiolipomas of the central nervous system. J Neurooncol 49:219–230
Anson JA, Cybulski GR, Reyes M (1990) Spinal extradural angiolipoma: a report of two cases and review of the literature. Surg Neurol 34:173–178
Bardosi A, Schaake T, Friede RL, Roessmann U (1985) Extradural spinal angiolipoma with secretory activity. An ultrastructural, clinico-pathological study. Virchows Arch A Pathol Anat Histopathol 406:253–259
Bender JL, Van Landingham JH, Manno NJ (1974) Epidural lipoma producing spinal cord compression. Report of two cases. J Neurosurg 41:100–103
Bucy PC, Ritchey H (1947) Klippel-Feil’s syndrome associated with compression of the spinal cord by an extradural hemangiolipoma. J Neurosurg 4:476–481
Chotai S, Hur JS, Moon HJ, Kwon TH, Park YK, Kim JH (2011) Spinal angiolipoma–case report. Neurol Med Chir (Tokyo) 51:539–542
da Costa MD, Paz Dde A, Rodrigues TP, Gandolfi AC, Lamis FC, Stavale JN, Suriano IC, Cetl LD, Cavalheiro S (2014) Hemorrhagic onset of spinal angiolipoma. J Neurosurg Spine 21:913–915
Diyora B, Nayak N, Kukreja S, Kamble H, Sharma A (2011) Thoracic epidural angiolipoma with bilateral multilevel extraspinal extensions: a rare entity. Neurol India 59:134–136
Fujiwara H, Kaito T, Takenaka S, Makino T, Yonenobu K (2013) Thoracic spinal epidural angiolipoma: report of two cases and review of the literature. Turk Neurosurg 23:271–277
Griebel RW, Khan M, Rozdilsky B (1986) Spinal extradural angiolipoma. A case report and literature review. Spine (Phila Pa 1976) 11:47–48
Haddad FS, Abla A, Allam CK (1986) Extradural spinal angiolipoma. Surg Neurol 26:473–486
Hu S, Hu CH, Hu XY, Wang XM, Dai H, Fang XM, Cui L (2013) MRI features of spinal epidural angiolipomas. Korean J Radiol 14:810–817
Kujas M, Lopes M, Lalam TF, Fohanno D, Poirier J (1999) Infiltrating extradural spinal angiolipoma. Clin Neuropathol 18:93–98
Lacour M, Gilard V, Marguet F, Curey S, Perez A, Derrey S (2018) Sudden paraplegia due to spontaneous bleeding in a thoracic epidural angiolipoma and literature review. Neurochirurgie 64:73–75
Leu NH, Chen CY, Shy CG, Lu CY, Wu CS, Chen DC, Guo TH (2003) MR imaging of an infiltrating spinal epidural angiolipoma. Am J Neuroradiol 24:1008–1011
Pagni CA, Canavero S (1992) Spinal epidural angiolipoma: rare or unreported? Neurosurgery 31:758–764
Park JH, Jeon SR, Rhim SC, Roh SW (2008) Lumbar spinal extradural angiolipoma: case report and review of the literature. J Korean Neurosurg Soc 44:265–267
Preul MC, Leblanc R, Tampieri D, Robitaille Y, Pokrupa R (1993) Spinal angiolipomas. Report of three cases. J Neurosurg 78:280–286
Provenzale JM, McLendon RE (1996) Spinal angiolipomas: MR features. Am J Neuroradiol 17:713–719
Rabin D, Hon BA, Pelz DM, Ang LC, Lee DH, Duggal N (2004) Infiltrating spinal angiolipoma: a case report and review of the literature. J Spinal Disord Tech 17:456–461
Sandvik U, Svensdotter E, Gustavsson B (2015) Spinal cavernous extradural angiolipoma manifesting as a spontaneous spinal epidural hematoma in a child. Childs Nerv Syst 31:1223–1226
Sankaran V, Carey M, Shad A (2010) Traumatic bleeding of spinal angiolipoma presenting with subacute paraparesis–a case report and histopathological aspects. Br J Neurosurg 24:714–715
Si Y, Wang Z, Pan Y, Lin G, Yu T (2014) Spinal angiolipoma: etiology, imaging findings, classification, treatment, and prognosis. Eur Spine J 23:417–425
Tsutsumi S, Nonaka Y, Abe Y, Yasumoto Y, Ito M (2011) Spinal angiolipoma in a pregnant woman presenting with acute epidural hemorrhage. J Clin Neurosci 18:849–851
Turgut M (1999) Spinal angiolipomas: report of a case and review of the cases published since the discovery of the tumour in 1890. Br J Neurosurg 13:30–40
Wang B, Yang Z, Yang J, Wang G, Xu Y, Liu P (2014) Spinal angiolipoma: experience of twelve patients and literature. Neurol India 62:367–370
Aghakhani N, David P, Parker F, Lacroix C, Benoudiba F, Tadie M (2008) Intramedullary spinal ependymomas: analysis of a consecutive series of 82 adult cases with particular attention to patients with no preoperative neurological deficit. Neurosurgery 62:1279–1285
Lin JJ, Lin F (1974) Two entities in angiolipoma. A study of 459 cases of lipoma with review of literature on infiltrating angiolipoma. Cancer 34:720–727
Yamashita K, Fuji T, Nakai T, Hamada H, Kotoh K (1993) Extradural spinal angiolipoma: report of a case studied with MRI. Surg Neurol 39:49–52
Feng J, Xu YK, Li L, Yang RM, Ye XH, Zhang N, Yu T, Lin BQ (2009) MRI diagnosis and preoperative evaluation for pure epidural cavernous hemangiomas. Neuroradiology 51:741–747
Demachi H, Takashima T, Kadoya M, Suzuki M, Konishi H, Tomita K, Yonezawa K, Ubukata A (1990) MR imaging of spinal neurinomas with pathological correlation. J Comput Assist Tomogr 4:250–254
Boukobza M, Mazel C, Touboul E (1996) Primary vertebral and spinal epidural non-Hodgkin’s lymphoma with spinal cord compression. Neuroradiology 38:333–337
Acknowledgements
We would like to thank all the patients who trusted us and all the physicians and staff who helped this study.
Funding
The authors declare that no funding was involved.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflicts of interest.
Ethical approval
This study was approved by Institutional Review Board of The First Affiliated Hospital of USTC.
Informed consent
For this type of study, formal consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yang, T., Niu, C. Microsurgical treatment for spinal epidural angiolipomas. Acta Neurol Belg 121, 421–427 (2021). https://doi.org/10.1007/s13760-019-01192-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13760-019-01192-6