Abstract
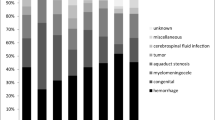
The aim of this study is to evaluate the clinical history and prognosis of children with early-onset hydrocephalus. The retrospective study’s inclusion criteria were hydrocephalus diagnosis before the age of 5 years, independent of aetiology, and birth details, January 1, 2000 to December 31, 2014. Overall, 142 children were entered into the study, divided into 11 aetiological groups: premature-birth post-intraventricular haemorrhage (16%), brain tumours (16%), spina bifida (15%), aqueductal stenosis (8%), post-meningitis (8%), post-haemorrhage (8%), Dandy–Walker malformation (6%), unknown origin (6%), arachnoid cyst (5%), miscellaneous obstruction (4%), and various causes (8%). In total, 23 patients died, primarily from the tumour group. Ventriculostomy, performed 42 times, was successful in 20 patients. Overall, 226 internal shunts were placed in 99 children. Infectious complications affected 19% of children after shunt placement and 51% after mechanical complications. Mean follow-up was 4 years 10 months, with 61% of children progressing fairly well, especially those with aqueductal stenosis, cysts, and unknown or diverse obstructive causes. Post-meningitis hydrocephalus displayed the poorest outcome. Isolated obstructive hydrocephalus exhibited better prognosis, with most obstructive aetiologies effectively treated via ventriculostomy. Children treated by shunt placement were more at risk of complications. Aetiologies with associated abnormalities and neurological sequelae had poorer outcomes.


Similar content being viewed by others
Notes
(Minimum−maximum) in years (yrs) months (mo) and days (d).
(Minimum−maximum) in years (yrs) months (mo) and days (d).
(Minimum−maximum) in years (yrs) months (mo) and days (d).
(Minimum−maximum) in years (yrs) months (mo) and days (d).
(Minimum−maximum) in years (yrs) months (mo) and days (d).
Abbreviations
- CNS:
-
Central nervous system
- CSF:
-
Cerebrospinal fluid
- ETV:
-
Endoscopic third ventriculostomy
- PHH:
-
Post-haemorrhage hydrocephalus
- PIVHH:
-
Post-intraventricular haemorrhage hydrocephalus
- PMH:
-
Post-meningitis hydrocephalus
- VPS:
-
Ventriculoperitoneal shunt
- QOL:
-
Quality of life
References
Volpe JJ (2008) Neurology of the newborn, 5th edn. Elsevier Saunders, Philadelphia
Lyon G, Evrard P (2000) Hydrocéphalies, collections liquidiennes péricérébrales chroniques. Neuropédiatrie, 2nd edn. Elsevier Masson, Paris, pp 83–96
Johnston MV, Kinsman S (2004) Congenital anomalies of the central nervous system. In: Behrman RE, Kliegman RM, Jenson HB (eds) Nelson textbook of pediatrics, 17th edn. Elsevier Saunders, Philadelphia, pp 1983–1993
Pinton F, Ponsot G (2010) Hydrocéphalies. In: Chabrol B, Dulac O, Mancini J, Ponsot G (eds) Neurologie pédiatrique, 3rd edn. Médecine Sciences Flammarion, Paris, pp 162–172
Lindquist B, Fernell E, Persson EK, Uvebrant P (2014) Quality of life in adults treated in infancy for hydrocephalus. Childs Nerv Syst 30(8):1413–1418. https://doi.org/10.1007/s00381-014-2425-4
Limbrick DD, Baird LC, Klimo P, Riva-Cambrin J, Flannery AM (2014) Pediatric hydrocephalus: systematic literature review and evidence-based guidelines. Part 4: cerebrospinal fluid shunt or endoscopic third ventriculostomy for the treatment of hydrocephalus in children. J Neurosurg Pediatr 14(Suppl 1):30–34. https://doi.org/10.3171/2014.7.peds14324
Kulkarni AV, Sgouros S, Constantin S (2016) International infant hydrocephalus study: initial results of a prospective, multicenter comparison of endoscopic third ventriculostomy (ETV) and shunt for infant hydrocephalus. Childs Nerv Syst 32(6):1039–1048. https://doi.org/10.1007/s00381-016-3095-1
Lam S, Harris D, Rocque BG, Ham SA (2014) Pediatric endoscopic third ventriculostomy: a population-based study. J Neurosurg Pediatr 14(5):455–464. https://doi.org/10.3171/2014.8.PEDS13680
Kadrian D, van Gelder J, Florida D, Jones R, Vonau M, Teo C, Stening W, Kwok B (2008) Long-term reliability of endoscopic third ventriculostomy. Neurosurgery 62(Suppl 2):614–621. https://doi.org/10.1227/01.neu.0000316265.59596.8c
Kamalo P (2013) Exit ventriculoperitoneal shunt; enter endoscopic third ventriculostomy (ETV): contemporary views on hydrocephalus and their implications on management. Malawi Medl J 25(3):78–82
Kulkarni AV, Riva-Cambrin J, Browd SR, Drake JM, Holubkov R, Kestle JRW, Limbrick DD, Rozzelle CJ, Simon TD, Tamber MS, Wellons JC, Whitehead WE (2014) Endoscopic third ventriculostomy and choroid plexus cauterization in infants with hydrocephalus: a retrospective hydrocephalus clinical research network study. J Neurosurg Pediatr 14(3):224–229. https://doi.org/10.3171/2014.6.PEDS13492
Mweshi MM, Amosun SL, Ngoma MS, Nkandu EM, Sichizya K, Chikoya L, Munthali J (2010) Endoscopic third ventriculostomy and choroid plexus cauterization in childhood hydrocephalus in Zambia. Med J Zambia 37(4):246–252
Stone SS, Warf BC (2014) Combined endoscopic third ventriculostomy and choroid plexus cauterization as primary treatment for infant hydrocephalus: a prospective North American series. J Neurosurg Pediatr 14:439–446. https://doi.org/10.3171/2014.7.PEDS14152
Warf BC (2005) Comparison of endoscopic third ventriculostomy alone and combined with choroid plexus cauterization in infants younger than 1 year of age: a prospective study in 550 African children. J Neurosurg Pediatr 103(6):475–481. https://doi.org/10.3171/ped.2005.103.6.0475
Zandian A, Haffner M, Johnson J, Rozzelle CJ, Tubbs RS, Loukas M (2014) Endoscopic third ventriculostomy with/without choroid plexus cauterization for hydrocephalus due to hemorrhage, infection, Dandy-Walker malformation, and neural tube defect: a meta-analysis. Childs Nerv Syst 30(4):571–578. https://doi.org/10.1007/s0038101323449
Platenkamp M, Hanlo PW, Fischer K, Gooskens RHJM (2007) Outcome in pediatric hydrocephalus: a comparison between previously used outcome measures and the hydrocephalus outcome questionnaire. J Neurosurg 107(1 Suppl):26–31. https://doi.org/10.3171/PED-07/07/026
Klepper J, Büsse M, Straßburg HM, Sörensen N (1998) Epilepsy in shunt-treated hydrocephalus. Dev Med Child Neurol 40(11):731–736
Tully HM, Ishak GE, Rue TC, Dempsey JC, Browd SR, Millen KJ, Doherty D, Dobyns WB (2016) Two hundred thirty-six children with developmental hydrocephalus: causes and clinical consequences. J Child Neurol 31(3):309–320. https://doi.org/10.1177/0883073815592222
Preuss M, Kutscher A, Wachowiak R, Merkenschlager A, Bernhard MK, Reiss-Zimmermann M, Meixensberger J, Nestler U (2015) Adult long-term outcome of patients after congenital hydrocephalus shunt therapy. Childs Nerv Syst 31(1):49–56. https://doi.org/10.1007/s00381-014-2571-8
Paulsen AH, Lundar T, Lindegaard KF (2015) Pediatric hydrocephalus: 40-year outcomes in 128 hydrocephalic patients treated with shunts during childhood. Assessment of surgical outcome, work participation, and health-related quality of life. J Neurosurg Pediatr 16(6):633–641. https://doi.org/10.3171/2015.5.peds14532
Bellin MH, Dicianno BE, Levey E, Dosa N, Roux G, Marben K, Zabel TA (2011) Interrelationships of sex, level of lesion, and transition outcomes among young adults with myelomeningocele. Dev Med Child Neurol 53(7):647–652. https://doi.org/10.1111/j.1469-8749.2011.03938.x
Verhoef M, Barf HA, Post MW, van Asbeck FW, Gooskens RH, Prevo AJ (2006) Functional independence among young adults with spina bifida, in relation to hydrocephalus and level of lesion. Dev Med Child Neurol 48(2):114–119. https://doi.org/10.1017/S0012162206000259
Bolduc ME, Limperopoulos C (2009) Neurodevelopmental outcomes in children with cerebellar malformations: a systematic review. Dev Med Child Neurol 51(4):256–267. https://doi.org/10.1111/j.1469-8749.2008.03224.x
Fletcher JM, Landry SH, Bohan TP, Davidson KC, Brookshire BL, Lachar D, Kramer LA, Francis DJ (1997) Effects of intraventricular hemorrhage and hydrocephalus on the long-term neurobehavioral development of preterm very-low-birthweight infants. Dev Med Child Neurol 39(9):596–606
Kulkarni AV, Shams I, Cochrane DD, McNeely PD (2010) Quality of life after endoscopic third ventriculostomy and cerebrospinal fluid shunting: an adjusted multivariable analysis in a large cohort. J Neurosurg Pediatr 6(1):11–16. https://doi.org/10.3171/2010.3.PEDS09358
Acknowledgement
No financial support of any institution, association or sponsor has been received to conduct this work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical standards
The trial protocol was approved by the ethical committee of the university and the study complied with its recommendations. Owing to its retrospective nature.
Informed consent
For this type of study, formal consent is not required.
Rights and permissions
About this article
Cite this article
Perdaens, O., Koerts, G. & Nassogne, MC. Hydrocephalus in children under the age of five from diagnosis to short-/medium-/long-term progression: a retrospective review of 142 children. Acta Neurol Belg 118, 97–103 (2018). https://doi.org/10.1007/s13760-018-0888-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13760-018-0888-x