Abstract
Purpose of Review
Untreated obstructive sleep apnea is associated with increased all-cause mortality, cardiovascular, cerebrovascular, and metabolic diseases. Obtructive sleep apnea disproportionately affects the African American community with reports of younger age of onset, increased severity of disease, and higher prevalence compared to Caucasians. The purpose of this review is to explore the degree to which heredity and social determinants of health affect obstructive sleep apnea prevalence, presentation, and outcomes.
Recent Findings
Recent studies have found obstructive sleep apnea characteristics in African Americans that informs putative mechanisms that drive the observed differences. These factors include reduced role of obesity, a tendency towards a lower respiratory arousal threshold, and the higher burden of inflammatory environmental exposures.
Summary
The difference in disease burden and adverse outcomes of obstructive sleep apnea experienced by African Americans is multifactorial and involves an intricate relationship between social determinants of health with genetic, anatomic, and physiologic factors. These influences have implications on the reliability of obstructive sleep apnea screening tools, disease presentation, and treatment success.

Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: •• Of major importance
Yeghiazarians Y, Jneid H, Tietjens JR, Redline S, Brown DL, El-Sherif N, et al. Obstructive sleep apnea and cardiovascular disease: a scientific statement from the American Heart Association. Circulation. 2021;144(3):e56–67.
Sutherland K, Keenan BT, Bittencourt L, Chen NH, Gislason T, Leinwand S, et al. A global comparison of anatomic risk factors and their relationship to obstructive sleep apnea severity in clinical samples. J Clin Sleep Med. 2019;15(4):629–39.
Billings ME, Gold D, Szpiro A, Aaron CP, Jorgensen N, Gassett A, et al. The association of ambient air pollution with sleep apnea: the multi-ethnic study of atherosclerosis. Ann Am Thorac Soc. 2019;16(3):363–70.
Johnson DA, Sofer T, Guo N, Wilson J, Redline S. A sleep apnea prediction model developed for African Americans: the Jackson Heart Sleep Study. J Clin Sleep Med. 2020;16(7):1171–8.
Dong L, Dubowitz T, Haas A, Ghosh-Dastidar M, Holliday SB, Buysse DJ, et al. Prevalence and correlates of obstructive sleep apnea in urban-dwelling, low-income, predominantly African-American women. Sleep Med. 2020;73:187–95.
Edwards BA, Redline S, Sands SA, Owens RL. More than the sum of the respiratory events: personalized medicine approaches for obstructive sleep apnea. Am J Respir Crit Care Med. 2019;200(6):691–703.
•• Wang H, Cade BE, Sofer T, Sands SA, Chen H, Browning SR, et al. Admixture mapping identifies novel loci for obstructive sleep apnea in Hispanic/Latino Americans. Hum Mol Genet. 2019;28(4):675–87. This recent publication identifies specific genetic markers that may influence the presentation of sleep-disordered breathing among racial and ethnic groups.
•• Borker PV, Reid M, Sofer T, Butler MP, Azarbarzin A, Wang H, et al. Non-REM apnea and hypopnea duration varies across population groups and physiologic traits. Am J Respir Crit Care Med. 2021;203(9):1173–82. This publication compares physiologic differences in sleep-disordered breathing presentation among racial and ethnic groups.
Lam B, Ip MS, Tench E, Ryan CF. Craniofacial profile in Asian and white subjects with obstructive sleep apnoea. Thorax. 2005;60(6):504–10.
Schwab RJ, Pasirstein M, Pierson R, Mackley A, Hachadoorian R, Arens R, et al. Identification of upper airway anatomic risk factors for obstructive sleep apnea with volumetric magnetic resonance imaging. Am J Respir Crit Care Med. 2003;168(5):522–30.
Cakirer B, Hans MG, Graham G, Aylor J, Tishler PV, Redline S. The relationship between craniofacial morphology and obstructive sleep apnea in whites and in African-Americans. Am J Respir Crit Care Med. 2001;163(4):947–50.
Rizzatti FG, Mazzotti DR, Mindel J, Maislin G, Keenan BT, Bittencourt L, et al. Defining extreme phenotypes of OSA across international sleep centers. Chest. 2020;158(3):1187–97.
Moghalu O, Whitesell P, Kwagyan J. Low respiratory arousal threshold (LRAT) in African Americans with obstructive sleep apnea (OSA). Neurology. 2020;94(15).
Healthy People 2030, U.S. Department of Health and Human Services, Office of Disease Prevention and Health Promotion. 2022. [Available from: https://health.gov/health.gov/healthypeople/objectives-and-data/social-determinants-health.
Quintos A, Naranjo M, Kelly C, Quan SF, Sharma S. Recognition and treatment of sleep-disordered breathing in obese African American hospitalized patients may improve outcome. J Natl Med Assoc. 2019;111(2):176–84.
Lavie CJ, Kuruvanka T, Milani RV, Prasad A, Ventura HO. Exercise capacity in adult African-Americans referred for exercise stress testing: is fitness affected by race? Chest. 2004;126(6):1962–8.
Ladabaum U, Mannalithara A, Myer PA, Singh G. Obesity, abdominal obesity, physical activity, and caloric intake in US adults: 1988 to 2010. Am J Med. 2014;127(8):717–27 e12.
Netzer NC, Stoohs RA, Netzer CM, Clark K, Strohl KP. Using the Berlin Questionnaire to identify patients at risk for the sleep apnea syndrome. Ann Intern Med. 1999;131(7):485–91.
Nagappa M, Liao P, Wong J, Auckley D, Ramachandran SK, Memtsoudis S, et al. Validation of the STOP-Bang Questionnaire as a screening tool for obstructive sleep apnea among different populations: a systematic review and meta-analysis. PLoS ONE. 2015;10(12):e0143697.
Marti-Soler H, Hirotsu C, Marques-Vidal P, Vollenweider P, Waeber G, Preisig M, et al. The NoSAS score for screening of sleep-disordered breathing: a derivation and validation study. Lancet Respir Med. 2016;4(9):742–8.
Johns MW. Reliability and factor analysis of the Epworth Sleepiness Scale. Sleep. 1992;15(4):376–81.
Johns MW. A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep. 1991;14(6):540–5.
O’Connor GT, Lind BK, Lee ET, Nieto FJ, Redline S, Samet JM, et al. Variation in symptoms of sleep-disordered breathing with race and ethnicity: the Sleep Heart Health Study. Sleep. 2003;26(1):74–9.
Knutson KL, Rathouz PJ, Yan LL, Liu K, Lauderdale DS. Stability of the pittsburgh sleep quality index and the epworth sleepiness questionnaires over 1 year in early middle-aged adults: the CARDIA study. Sleep. 2006;29(11):1503–6.
Hayes AL, Spilsbury JC, Patel SR. The Epworth score in African American populations. J Clin Sleep Med. 2009;5(4):344–8.
Pandey A, Mereddy S, Combs D, Shetty S, Patel SI, Mashaq S, et al. Socioeconomic inequities in adherence to positive airway pressure therapy in population-level analysis. J Clin Med. 2020;9(2).
Mehrtash M, Bakker JP, Ayas N. Predictors of continuous positive airway pressure adherence in patients with obstructive sleep apnea. Lung. 2019;197(2):115–21.
Hsu N, Zeidler MR, Ryden AM, Fung CH. Racial disparities in positive airway pressure therapy adherence among veterans with obstructive sleep apnea. J Clin Sleep Med. 2020;16(8):1249–54.
Borker PV, Carmona E, Essien UR, Saeed GJ, Nouraie SM, Bakker JP, et al. Neighborhoods with greater prevalence of minority residents have lower continuous positive airway pressure adherence. Am J Respir Crit Care Med. 2021;204(3):339–46.
Andreozzi F, Van Overstraeten C, Ben Youssef S, Bold I, Carlier S, Gruwez A, et al. African ethnicity is associated with a higher prevalence of diabetes in obstructive sleep apnea patients: results of a retrospective analysis. Sleep Breath. 2020;24(3):857–64.
Holliday SB, Haas A, Dong L, Ghosh-Dastidar M, Hale L, Buysse DJ, et al. Examining the diagnostic validity of the Berlin Questionnaire in a low-income Black American sample. J Clin Sleep Med. 2021;17(10):1987–94.
Author information
Authors and Affiliations
Contributions
All authors met the four criteria for authorship established by the International Committee of Medical Journal Editors: Bianca Stewart, Pamela Barletta, Barbara Sorondo, Alexandre Abreu, and Alejandro Chediak were responsible for the conception, design, and drafting of the work; revision of the work, and review of the manuscript. All authors provided final approval of the version to be published and agreed to be accountable for all aspects of the work in ensuring the accuracy and/or integrity of the work.
Corresponding author
Ethics declarations
Conflict of Interest
None.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Sleeping and Breathing
Appendix
Appendix
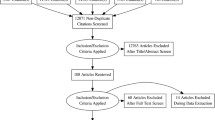
PubMed search strategy:
(("Blacks"[Mesh] OR "African American"[Title/Abstract] OR "African Americans"[Title/Abstract] OR black*[Title/Abstract]) AND ("Sleep Apnea Syndromes"[Mesh] OR "sleep apnea"[Title/Abstract] OR "sleep hypopnea"[Title/Abstract] OR "sleep-disordered breathing"[Title/Abstract] OR OSA[Title/Abstract] OR OSAS[Title/Abstract] OR SDB[Title/Abstract])) NOT ("Infant"[Mesh] OR "Child"[Mesh] OR "Adolescent"[Mesh] OR Child*[Title/Abstract] OR pediatric*[Title/Abstract] OR teen*[Title/Abstract] OR adolescen*[Title/Abstract] OR infan*[Title/Abstract] OR baby[Title/Abstract] OR babies[Title/Abstract] OR toddler*[Title/Abstract])
(All search strategies available upon request.)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Stewart, B., Barletta, P., Sorondo, B.M. et al. Obstructive Sleep Apnea in African Americans: A Literature Review. Curr Pulmonol Rep 12, 16–21 (2023). https://doi.org/10.1007/s13665-023-00300-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13665-023-00300-5