Abstract
Introduction
We report a comprehensive summary of the safety outcomes in adult patients with moderate-to-severe psoriasis with up to 5 years of exposure to ixekizumab.
Methods
Long-term safety of the IL-17A antagonist ixekizumab was assessed from 17 randomized trials. Treatment-emergent adverse events (TEAEs)-adjusted incidence rates (IRs) per 100 patient-years (PY) within 1-year time periods through 19 March 2021 were calculated for all patients treated with at least one dose of ixekizumab. Reported cases of major adverse cerebro-cardiovascular events (MACE) and inflammatory bowel disease (IBD) were adjudicated.
Results
A total of 6892 adult patients with a cumulative exposure of 18,025.7 PY were included. The IRs per 100 PY for any TEAE and serious adverse events (AEs) were 32.5 and 5.4. IR of discontinuation because of AE was 2.9. A total of 36 deaths were reported. IR of serious infections was low (1.3). There were no confirmed cases of reactivation of tuberculosis (TB). IR of Candida infections (IR 1.9) was low; most cases of Candida were localized, and no systemic cases were reported. IRs of injection site reactions and allergic/hypersensitivity were 5.9 and 5.6, respectively. No confirmed cases of anaphylaxis were observed. IRs were low for malignancies, depression, cytopenia, and MACE (all ≤ 1.2). IBD events were uncommon, although a total of 31 patients (IR 0.2) had confirmed IBD (ulcerative colitis, n = 18; Crohn disease, n = 13). Across safety topics, IRs decreased or remained constant over time.
Conclusions
The long-term safety profile for ixekizumab is consistent with that previously reported in patients with psoriasis. No new or unexpected safety events were detected.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
The safety profile in 6892 (18,025.7 PY) patients with moderate-to-severe psoriasis with up to 5 years of ixekizumab exposure is reported |
The overall benefit–risk profile of ixekizumab remained favorable through 5 years |
Yearly IRs decreasing or remaining constant across safety topics from the first year of exposure |
In patients with active moderate-to-severe psoriasis, long-term safety data did not show any new or unexpected safety events |
Introduction
Owing to the chronic and recalcitrant nature of psoriasis, a common chronic inflammatory disease, long-term pharmaceutical management is required to maintain adequate disease control. For patients with moderate-to-severe disease, biologic therapies such as monotherapy or combined therapy with other topical or systemic medications are recommended because of a high benefit–risk ratio [1]. Thus, there is a need to monitor long-term safety of biologic therapies.
Ixekizumab, a high-affinity monoclonal antibody that selectively targets interleukin (IL)-17A, is a biologic approved for the treatment of moderate-to-severe plaque psoriasis, psoriatic arthritis, ankylosing spondylitis, nonradiographic axial spondyloarthritis, and pediatric psoriasis [2,3,4,5]. The safety profile of ixekizumab in patients with moderate-to-severe plaque psoriasis has been published regularly since its introduction in 2016 [6,7,8,9]. The most recent integrated report from 13 clinical trials with 17,331.1 PY exposure in 5898 patients reported no new or unexpected safety issues with the long-term treatment of moderate-to-severe plaque psoriasis with ixekizumab [9]. Here, we establish the safety profile of up to 5 years of exposure to ixekizumab in a broader group of patients with moderate-to-severe plaque psoriasis. This was done by qualitatively evaluating incidence rates (IRs), outcomes, and medical history of patients who experienced selected adverse events (AEs).
Methods
Patients and Study Design
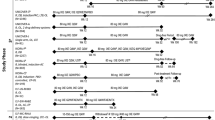
Patient data were integrated from 17 controlled clinical trials of ixekizumab in adult patients with moderate-to-severe psoriasis (Supplementary Table 1). The three largest trials, UNCOVER-1, UNCOVER-2, and UNCOVER-3, contributed the most patients for this analysis [10, 11]. Eligibility criteria have been previously described [10, 11]. Briefly, these studies enrolled adults (≥ 18 years old) with moderate-to-severe plaque psoriasis defined by ≥ 10% body surface area involvement, Static Physician’s Global Assessment of ≥ 3, and Psoriasis Area Severity Index (PASI) ≥ 12 at baseline. Detailed study designs have been published before [10, 11]. UNCOVER-1, UNCOVER-2, and UNCOVER-3 were multicenter, randomized, double-blinded, placebo-controlled phase 3 trials; an etanercept comparator group was included in the UNCOVER-2 and UNCOVER-3 trials.
The protocols for all the studies included in this analysis were approved by the institutional review board or ethics committee at each participating site. All studies were conducted in accordance with the ethical principles of the Declaration of Helsinki. All eligible patients provided written informed consent before undergoing study-related procedures.
Outcomes
AEs were classified according to the Medical Dictionary for Regulatory Activities (MedDRA) version 23.1. A treatment-emergent adverse event (TEAE) was one that first occurred or worsened in severity after baseline or on or before the last day of the treatment period. Selected AEs of interest included infections, serious infections, opportunistic infections (OIs), latent tuberculosis (TB), candidiasis infections, respiratory viral infections, injection site reactions (ISRs), allergic reactions/hypersensitivities, malignancies including nonmelanoma skin cancer (NMSC), malignancies excluding NMSC, inflammatory bowel disease (IBD) including Crohn’s disease, ulcerative colitis, IBD unclassified, depression, suicidal behavior/self-injury, cytopenia, major adverse cerebro-cardiovascular event (MACE), and asthma. All potential and suspected cases of IBD identified by MedDRA terms were adjudicated in a blinded manner by an external committee that comprised three independent experts in IBD. Suspected IBD cases were assessed as to whether the cases represented one of the following Registre Epidemiologique des Maladies de l’Appareil Digestif (EPIMAD) criteria [12]: “definite,” “probable,” or “possible.” EPIMAD criteria used for adjudication are shown in Supplementary Material, Methods. Additionally, the adjudicators could classify events as “not consistent with IBD,” or “lack of sufficient documentation for confirmation of an event.” Only cases classified as “probable” and “definite” per external adjudication were considered as confirmed. MACE events were adjudicated by external adjudication. Depression was measured using Quick Inventory of Depressive Symptomatology-Self Report 16 items (QIDS-SR16) and/or Colombia Suicide Scale Rating Scale (C-SSRS). Opportunistic infections were reported according to the consensus recommendations for OIs and biologic therapies report published by Winthrop and colleagues [13]. Latent TB infection was identified by either latent TB preferred term (PTs) or a positive result on either the tuberculin test or Mycobacterium tuberculosis complex test. Patients who tested positive for latent TB at screening could be rescreened and enrolled after receiving at least 4 weeks of appropriate latent TB infection therapy and having no evidence of hepatotoxicity (alanine transaminase/aspartate transaminase remained at least two times the upper limit of normal). ISRs (broad term) included the following PTs: ISR, injection site (IS) erythema, pain, swelling, pruritus, hypersensitivity, bruising, rash, hematoma, induration, papule, urticaria, mass, warmth, discoloration, inflammation, and edema.
Statistical Analysis
Safety analyses were based on all randomized patients who received at least one dose of study drug. Total exposure was calculated by summarizing the duration of ixekizumab exposure (in days) for all patients, divided by 365.25 and expressed in total PY. All safety events were reported by the number and percentage of patients with AE and exposure-adjusted IRs (95% CI). Incidence rates were calculated by dividing total number of patients who experienced the TEAE for each PT by the sum of all patients’ time (in 100 years) of exposure during the treatment period. The incidence rate confidence intervals were determined from likelihood ratio test of treatment effect from the Poisson regression. The entire treatment period was included in the analysis. The current analysis includes data from initiation of the studies to 19 March 2021 cutoff. Statistical analyses were performed using SAS software version 9.3 or higher (SAS Institute).
Results
Demographic and Baseline Characteristics
Patients’ demographic and baseline characteristics are provided in Table 1. The mean (SD) age was 45.7 (± 13.2) years. Patients were predominantly males (68.1%), and 81.5% of participants were white. The body mass index (BMI) mean (SD) was 30.4 (± 7.3) kg/m2, and 12.7% of patients were smokers at baseline. The duration (SD) of psoriasis was 18.7 (± 12.2) years. The proportion of patients who were naïve to systemic therapy was 35.9%; most patients experienced previous systemic therapy (64.1%), which includes nonbiologics only (35.1% of patients), biologics only (12.0% of patients), and both biologics and nonbiologics (17.0% of patients).
Exposure
A total of 6892 adult patients with psoriasis with up to 5 years’ cumulative exposure to ixekizumab of 18,025.7 PY were included in this safety analysis pooled from 17 clinical trials (Table 2). The minimum exposure was 1 day, and the maximum was 2236 days. The mean exposure of this pooled population was 955.3 days with a median exposure of 478.5 days.
General Safety
Over the entire safety period, the proportion of patients with at least one TEAE was 85.0% (IR of 32.5 per 100 PY) (Table 2). Most cases were mild (26.1%, IR of 10.0 per 100 PY) to moderate (43.9%, IR of 16.8 per 100PY); severe TEAEs were reported by 15.0% of patients (IR of 5.7 per 100 PY). The most common TEAEs (defined as at least 5.0%) were nasopharyngitis, upper respiratory tract infection, IS reaction, arthralgia, headache, back pain, hypertension, bronchitis, diarrhea, sinusitis, and urinary tract infection. A total of 969 patients presented SAEs (14.1%, IR of 5.4 per 100 PY). A total of 862 patients required hospitalizations (12.5%, IR of 4.8 per 100 PY), 49 patients had a life-threatening event (0.7%, IR of 0.3 per 100 PY), 36 patients had a fatal outcome (0.5%, IR of 0.2 per 100 PY), 10 patients had events that led to disability (0.1%, IR of 0.1 per 100 PY), 9 patients had events requiring intervention (0.1%, IR of 0.0 per 10 PY), and 140 patients reported SAEs due to other reasons (2.0%, IR of 0.8 per 100 PY) (Table 2). A total of 36 deaths were reported; causes of death were cardiovascular (n = 20), unknown (n = 4, including 1 unconfirmed death due to lung cancer, 1 lost to follow-up, 2 fatality unknown cause of death), neoplasm (n = 5), respiratory (n = 1), and other cause of deaths (n = 6, including, 1 IBD, 1 end-stage senile dementia, 1 cholelithiasis, 1 accidental death, 1 trauma, and 1 homicide). Overall, discontinuations from the study due to AEs were reported by 7.5% of patients (IR of 2.9 per 100 PY). The main causes of discontinuation were latent TB (IR of 0.4 per 100 PY), maternal exposure during pregnancy and pregnancy (IR of 0.4 per 100 PY; calculation adjusted to women only), prostate cancer (IR of 0.1 per 100 PY; calculation adjusted to men only), IS reaction (IR of 0.1 per 100 PY), psoriatic arthropathy (IR of 0.1 per 100 PY), and ulcerative colitis (IR of 0.1 per 100 PY).
TEAEs were more common during the first year of ixekizumab exposure (IR of 88.9 per 100 PY) and decreased over time (63.2 per 100 PY over the fifth year of exposure) (Fig. 1a). On the basis of yearly exposure periods analysis, IRs for SAEs and discontinuations were stable for each of the 1-year periods (Fig. 1b,c).
Exposure-adjusted incidence rate of TEAEs, SAEs, and discontinuation because of AE (Exposure Safety Populations). The data points on the graph are the IR (95% CI)/100 PY at successive year intervals from year 0 to year 5. The CIs for the IRs are from likelihood ratio tests of treatment effect from the Poisson regression model. AEs adverse events, CI confidence interval, IR exposure-adjusted incidence rate, PY patient-years, SAEs serious adverse events, TEAEs treatment-emergent adverse events
Summary of Selected Adverse Events
Infections
Over the entire safety period, infections were reported by 62.5% of patients (IR of 23.9 per 100 PY) (Table 3). Most cases of infection were mild (IR of 10.0 per 100 PY) or moderate (12.5 per 100 PY) in severity; the IR of severe infections was 1.4 per 100 PY. The most common types of infections (defined by IR ≥ 2.0 per 100 PY) were nasopharyngitis, upper respiratory tract infections, bronchitis, sinusitis, and urinary tract infection.
Overall, frequency of serious infections was low (3.4%; IR of 1.3 per 100 PY) (Table 3). A total of 231 patients presented with serious infections (total of 327 events), of which most resolved (n = 291; 89.0%), 12 patients recovered with sequelae, 4 patients were recovering, 17 patients did not recover, 1 patient had a fatal event (case of septic shock; later adjudicated as cardiovascular death), and the outcome was unknown for 2 patients at the time of the data lock. Over the 5-year period observed, the IRs of serious infections remained constant over time (Fig. 2a).
Exposure-adjusted incidence rate of selected adverse events (Exposure Safety Populations). The data points on the graph are the IR (95% CI)/100 PY at successive year intervals from year 0 to year 5. Overall serious infections, ISR, IBD, MACE, malignancies, and depression. The CIs for the IRs are from likelihood ratio test of treatment effect from the Poisson regression model. aThe data represent confirmed cases per external adjudication. bThe data represent events confirmed by adjudication. CI confidence interval, IBD inflammatory bowel disease, IR incidence rate, ISR injection site reaction, IXE ixekizumab, MACE major adverse cerebro-cardiovascular event, PsO psoriasis, PY patient-year
Overall, OIs were reported by 4.6% of patients (IR of 1.8 per 100 PY) (Table 3). OIs were mostly oral candidiasis (2.1%; IR of 0.8 per 100 PY), localized herpes zoster (1.7%; IR of 0.7 per 100 PY), unspecified Candida infections (0.5%; IR of 0.2 per 100 PY), and esophageal candidiasis (0.2%; IR of 0.1 per 100 PY). Herpes zoster infections were mostly nonserious (119/120), with no disseminated events reported.
A total of 106 cases of latent TB (IR of 0.6 per 100 PY) were reported by annual TB testing (Table 3). Positive TB test led to discontinuation of the study drug for 67 patients. Among these, one case was reported as TB by the investigator (occurred in a patient that was previously treated for latent TB, no symptoms were reported and patient was treated with isoniazid), and there was one case of pulmonary TB. There were no existing latent cases that presented any sign of active TB disease, and no fatal cases due to TB.
Candida infections were reported by 4.9% (IR of 1.9 per 100 PY) of patients (Table 3). All cases of Candida infections were localized; no systemic cases were observed. A total of 337 patients had events (total of 533 events) of Candida infection, which were mainly mild (n = 162, IR of 0.9 per 100 PY) to moderate (n = 170, IR of 0.9 per 100 PY) in severity. Severe Candida infections cases were reported by five patients (which included three cases of oral candidiasis, one case of otitis externa Candida, and one case of esophageal candidiasis). Serious Candida infections occurred in two patients (total of five events); patients recovered from all events.
Frequencies of viral infections were low (≤ 5%) (Table 3). Overall, influenza occurred in 315 patients (IR of 1.7 per 100 PY), viral upper respiratory tract infections occurred in 140 patients (IR of 0.8 per 100 PY), unspecified viral respiratory tract infections occurred in 14 patients (IR of 0.1 per 100 PY), and viral lower respiratory tract infections in 2 patients (IR of 0.0 per 100 PY). No cases of viral respiratory tract infection led to trial discontinuation.
Injection Site Reactions and Allergic Reactions/Hypersensitivities
TEAEs of ISRs (High Level Term according to MedDRA classification), were the most common TEAEs after infection in psoriasis patients exposed to ixekizumab (Table 4). Over the treatment period, ISRs were reported by 15.3% of patients (IR of 5.9 per 100 PY). The severity of ISRs events was mostly mild (n = 727, IR of 4.0 per 100 PY) or moderate (n = 294, IR of 1.6 per 100 PY). A total of 35 severe ISRs cases were reported (IR of 0.2 per 100 PY); no cases of serious ISRs were observed. ISRs were the cause of discontinuation of the study drug for 15 patients. The most commons PTs of ISRs were IS reaction (IR of 3.9 per 100 PY), IS erythema (IR of 1.1 per 100 PY), and IS pain (IR of 0.6 per 100 PY). Over the 5-year period observed, the incidence of ISRs decreased steadily from an IR of 16.5 per 100 PY the first year period to an IR of 1.7 per 100 PY at year 5 (Fig. 2b).
Overall, 14.5% of patients reported allergic reactions or hypersensitivity (IR of 5.6 per 100 PY) (Table 4). The most common type of allergic reactions or hypersensitivity were contact dermatitis (IR of 1.1 per 100 PY), eczema (IR of 1.1 per 100 PY), urticaria (IR of 0.9 per 100 PY), dermatitis (IR of 0.6 per 100 PY), rash (IR of 0.5 per 100 PY), and allergic rhinitis (IR of 0.5 per 100 PY). TEAEs of allergic reactions or hypersensitivities were mainly mild (8.8%, IR of 3.4 per 100 PY) to moderate (5.3%, IR of 2.0 per 100 PY) in severity. IR of severe cases was low (0.5%, IR of 0.2 per 100 PY). A total of 28 cases of serious allergic reactions or hypersensitivity were observed (IR of 0.2 per 100 PY). After medical review, no confirmed cases of anaphylaxis were reported in the safety population.
Inflammatory Bowel Disease (IBD)
Per external adjudication, a total of 26 patients (IR of 0.1 per 100 PY, 0.4%) had TEAE of IBD confirmed as either Crohn’s disease [n = 10, IR of 0.1 per 100PY, 0.1%; which included 9 patients with de novo cases (IR of 0.05 per 100 PY) and 1 patient with IBD history of ulcerative colitis], or ulcerative colitis [n = 16, IR of 0.1 per 100 PY, 0.2%; which included 14 patients with de novo cases (IR of 0.08 per 100 PY) and 2 patients with history of ulcerative colitis] (Table 4). Half of the patients (n = 13) had discontinued the study drug because of confirmed TEAE IBD event. Among the 13 patients with confirmed IBD who did not discontinue the study drug owing to IBD event, 4 patients had subsequent episodes of IBD during the study. As assessed on the basis of year of exposure, incidence of confirmed IBD ranged from 0.0 to 0.3 per 100 PY and was constant over time (Fig. 2c).
There were five additional cases of confirmed IBD (three cases of Crohn’s disease and two cases of ulcerative colitis) that occurred either on the safety follow-up period (n = 3) or on placebo maintenance period after ixekizumab treatment (n = 2). In these five additional cases, the time from the last ixekizumab injection to the IBD event (i.e., duration that patients were off ixekizumab treatment) ranged from 30 to 148 days. Therefore, in total, 31 patients had confirmed IBD (IR of 0.2 per 100 PY, 0.4%). Among the 31 patients with confirmed IBD events, 18 patients were male, and ages ranged from 22 to 67 years old. A total of 11 patients had more than one event of IBD. Most confirmed events of IBD were moderate to severe in severity, and 21 patients experienced a serious event (IR of 0.1 per 100 PY). Most cases were ongoing at the time of last study visit; nine were resolved, and one patient with ulcerative colitis had a fatal event.
Major Adverse Cerebro-Cardiovascular Event
Incidence of confirmed MACE events was low (0.5 per 100 PY) and occurred in 91 patients (Table 4). Most MACE cases were moderate (n = 19, 0.3%) to severe (n = 70, 1.1%). A total of 89 patients had serious event of MACE (IR of 0.5 per 100 PY). Among the 89 patients with serious MACE event, 20 cases were fatal (20.2%), 55 cases were recovered (55.6%), 17 cases were recovered with sequelae (17.2%), 4 cases were recovering (4.0%), and 3 were not recovered (3.0%) at data lock. The majority of patients with TEAE of MACE had medical history of preexisting vascular disorders (59.3%, n = 54), including hypertension (58.2%, n = 53), dyslipidemia (27.5%, n = 25), type 2 diabetes mellitus (19.8%, n = 18), hypercholesterolemia (13.2%, n = 12), obesity (12.1%, n = 11), and cardiac disorders (20.9%, n = 19), including coronary artery disease (13.2%, n = 12). The most common types of MACE were nonfatal myocardial infarction (0.7%; IR of 0.3 per 100 PY), followed by nonfatal stroke (0.3%; IR of 0.1 per 100 PY), and vascular death (0.3%; IR of 0.1 per 100 PY). As assessed on the basis of yearly exposure periods, the incidences of MACE were stable over time (Fig. 2d).
Malignancies
Malignancies occurred in 141 patients (IR of 0.8 per 100 PY), including 54 patients (IR of 0.3 per 100 PY) with NMSC and 94 patients (IR of 0.5 per 100 PY) with malignancies other than NMSC (Table 4). The most reported cases of NMSC were basal cell carcinoma (n = 44, IR of 0.2 per 100 PY), followed by squamous cell carcinoma of skin (n = 8, IR of 0.0 per 100 PY). The most reported type of malignancy other than NMSC was prostate cancer (n = 12, IR of 0.1 per 100 PY; denominator adjusted because of gender-specific event for males). TEAEs of NMSC were mainly mild (22/54 cases) to moderate (29/54) in severity, while malignancies other than NMSC were, in majority, moderate (24/94) to severe (58/94) events. The majority of patients reported nonserious NMSC. A total of five serious cases of NMSC were reported; all of them recovered, while 94.4% of nonserious cases reached the same outcome. Most cases of malignancies other than NMSC were serious (76/94 cases), 5 events were fatal, 18 cases were recovered, 47 cases were not recovered, 1 case was recovered with sequelae, 7 cases were recovering, and 4 cases had an unknown outcome at the time of data lock. The diagnosis of a malignancy led to discontinuation of the study drug for 73 patients (1.1%, IR of 0.4 per 100 PY). The mean time from start of the study drug to onset of malignancies event was 670 days (NMSC: 536.9 days, malignancies other than NMSC: 763.5 days). The incidence of malignancies was low and constant over the 5-year period (Fig. 2e).
Depression
Overall, depression events (including suicide and self-injury) were reported by 3.1% (IR of 1.2 per 100 PY) of patients exposed to ixekizumab (Table 4). Depression events were mainly mild (n = 89, 1.3%) to moderate cases (n = 100, 1.5%) in severity; 26 (0.4%) events of severe depression were reported. SAEs of depression occurred in 27 patients (0.4%, IR of 0.1 per 100 PY). Most common PTs of depression were depression (n = 132, IR of 0.7 per 100 PY; led to discontinuation of study drug by nine patients), depressed mood (n = 11, IR of 0.1 per 100 PY), suicide attempt (n = 11, IR of 0.1 per 100 PY; led to discontinuation of study drug by five patients), and adjustment disorder with depressed mood (n = 9, IR of 0.1 per 100 PY). Many patients with TEAE of depression had at baseline preexisting condition or medical history of psychiatric disorders (n = 78, 36.3%). Most common preexisting conditions included, but were not limited to, depression (n = 44, 20.5%), anxiety (n = 18, 8.4%), and insomnia (n = 14, 6.5%). Over the 5-year period observed, the incidence of TEAEs of depression was low (≤ 1.7 per 100 PY) and progressively decreased (Fig. 2f).
Other Selected Treatment-Emergent Adverse Events of Interest
Overall, cases of cytopenia were reported by 2.5% (IR of 0.9 per 100 PY) of patients exposed to ixekizumab (Table 4). A total of 27 cases of neutropenia grade 3 or worse were reported, including 3 cases of grade 4. Overall, asthma was reported by 0.7% of patients (IR of 0.3 per 100 PY). Two cases of asthma were serious; none led to discontinuation of the study drug.
Discussion
Owing to the chronic and recalcitrant nature of moderate-to-severe plaque psoriasis, most patients will require long-term treatment with biologics to manage their disease. Therefore, long-term monitoring of the safety of biologics is required. In this analysis, the IR of TEAEs with long-term exposure to ixekizumab in 6892 adult patients with moderate-to-severe psoriasis did not increase. Additionally, IRs of SAEs were low in ixekizumab-treated patients over 5 years of exposure. Rates of TEAEs tended to be stable or decreased from the first year of exposure.
There is evidence that IL-17 plays a key role in host defense against fungal infections. Thus, the use of IL-17 antagonist agents may increase susceptibility to infections, in particular mucocutaneous candidiasis [14]. Candida infections were commonly reported for ixekizumab (1.9 per 100 PY); all cases were localized (mainly oral candidiasis), and no systemic cases were observed. Of note, higher rates of oral candidiasis have recently been reported in patients treated with the anti-IL17A/F antibody (bimekizumab) compared with another IL-17A inhibitor (secukinumab) [15].
While infections in general were the most common TEAEs (IR of 23.9 per 100 PY), their severity tended to be mild or moderate. Serious infections were infrequent (3.4%) in patients exposed to ixekizumab. These serious infections were easily treated, most events resolved, and they generally did not interfere with maintenance of ixekizumab treatment.
IBD pathogenesis involves a complex network of cytokines associated with intestinal inflammation [16, 17]. In particular, interactions between IL-12, IL-23, and IL-17 play important roles in gut-defense mechanisms and in the regulation of tissue inflammation [18]. Previous animal studies have demonstrated conflicting findings on the role of IL-17 inhibitors for treatment of intestinal inflammation [19]. Furthermore, in a clinical trial utilizing secukinumab for the treatment of patients with Crohn’s disease, no benefit was found, with worsening of the IBD after treatment in a subset of patients [20].
Although the exact etiology of IBD is unknown, the mechanistic and pathologic role IL-17 plays in intestinal inflammation likely involves interactions with environmental, genetic, and microbial factors [21]. Patients with psoriasis experience a higher burden of IBD than the general population [22], and are at higher risk of developing Crohn’s disease and ulcerative colitis than matched reference populations [23, 24]. In the current safety analyses for ixekizumab, IBD events were uncommon (< 1% of the population). A total of 31 cases of confirmed IBD were detected, including 13 cases of Crohn’s disease and 18 cases of ulcerative colitis. Most of the IBD cases were de novo (27/31). In our studies, a total of 44 patients had a history of IBD, and 41 of them did not have an exacerbation during ixekizumab exposure. Although IBD is an adverse drug reaction for ixekizumab, the IRs reported in our studies are in line with the expected IR of IBD in patients with psoriasis [24, 25]. In patients with moderate-to-severe psoriasis, careful evaluation of confirmed diagnosis of Crohn’s disease or ulcerative colitis should be conducted by the physician when considering treatment with ixekizumab and other IL-17 inhibitors, and psoriasis patients should be monitored for IBD after initiation of ixekizumab. Further studies are needed to understand risk factors associated with IBD with IL-17 inhibition.
Cardiovascular risk factors are among the most common comorbidities in psoriasis [26]. The results of one observational study in patients with psoriasis suggest that a cumulative duration of exposure to low-grade chronic inflammation is associated with a high prevalence of vascular diseases and MACE events (1.0% per additional year of psoriasis duration) [27]. In the current report, the incidence of MACE events was low (0.5 per 100 PY). This finding is consistent with a study from three clinical trials that showed a neutral impact of ixekizumab on cardiovascular parameters in patients with moderate-to-severe psoriasis [28]. Interestingly, in two separate studies, Mehta and colleagues demonstrated 12% and 14.7% reductions in lipid-rich atherosclerotic plaques (via CT angiography) in patients with psoriasis treated for 1 year with an IL-17 inhibitor [29, 30]. Taken together, these results suggest that additional studies are needed to understand more fully the effects of IL-17 inhibitors on cardiovascular disease over time.
Patients with psoriasis have an increased risk of malignancies owing to impaired immunosurveillance resulting from the effect of chronic inflammation [31]. A recent meta-analysis showed that the overall prevalence of cancer in patients with psoriasis was 4.78% with an incidence rate of 11.75 per 1000 PY [32]. In this study, malignancies were reported by 2.0% of patients receiving IXE (IR of 0.8 per 100 PY); no specific risk factors for malignancy in relation to treatment with ixekizumab have been identified.
Patients with psoriasis are more likely to have depression compared with those without psoriasis [33, 34]. In this integrated analysis of 18,025.7 PY of ixekizumab exposure, the IR of depression was 1.2 per 100 PY, which does not suggest any increased risk of depression associated with ixekizumab.
Although this analysis included a large sample size of 6892 individuals, the population was limited to adult patients. The shorter-term safety profile of ixekizumab in pediatric patients has previously been reported [4]. Generally, the safety profile of ixekizumab in children was consistent with that observed in adults with moderate-to-severe psoriasis.
Conclusion
In summary, the overall safety profile of ixekizumab remained favorable through 5 years with no increase in yearly TEAEs IRs from the first year of exposure. No new or unexpected safety events were identified, and the safety profile is consistent with the established safety profile in current labeling. These findings add value to physicians when assessing the benefit-to-risk balance in patients with moderate-to-severe psoriasis being treated with ixekizumab over time.
References
Menter A, Strober BE, Kaplan DH, Kivelevitch D, Prater EF, Stoff B, et al. Joint AAD-NPF guidelines of care for the management and treatment of psoriasis with biologics. J Am Acad Dermatol. 2019;80(4):1029–72. https://doi.org/10.1016/j.jaad.2018.11.057.
Liu L, Lu J, Allan BW, Tang Y, Tetreault J, Chow CK, et al. Generation and characterization of ixekizumab, a humanized monoclonal antibody that neutralizes interleukin-17A. J Inflamm Res. 2016;9:39–50. https://doi.org/10.2147/JIR.S100940.
Toussirot E. Ixekizumab: an anti- IL-17A monoclonal antibody for the treatment of psoriatic arthritis. Expert Opin Biol Ther. 2018;18(1):101–7. https://doi.org/10.1080/14712598.2018.1410133.
Paller AS, Seyger MM, Magariños G, Bagel J, Pinter A, Cather J, et al. Efficacy and safety of ixekizumab in a phase 3, randomized, double-blind, placebo-controlled study in paediatric patients with moderate-to-severe plaque psoriasis (IXORA-PEDS). Br J Dermatol. 2020;183:231–41.
Prescribing Information—Taltz. http://uspl.lilly.com/taltz/taltz.html#pi. Accessed 23 Apr 2020.
Strober B, Leonardi C, Papp KA, Mrowietz U, Ohtsuki M, Bissonnette R, et al. Short- and long-term safety outcomes with ixekizumab from 7 clinical trials in psoriasis: etanercept comparisons and integrated data. J Am Acad Dermatol. 2017;76(3):432-40 e17. https://doi.org/10.1016/j.jaad.2016.09.026.
Langley RG, Kimball AB, Nak H, Xu W, Pangallo B, Osuntokun OO, et al. Long-term safety profile of ixekizumab in patients with moderate-to-severe plaque psoriasis: an integrated analysis from 11 clinical trials. J Eur Acad Dermatol Venereol. 2019;33(2):333–9. https://doi.org/10.1111/jdv.15242.
Armstrong AW, Paul C, Puig L, Boehncke WH, Freeman M, Torii H, et al. Safety of ixekizumab treatment for up to 5 years in patients with moderate-to-severe psoriasis: results from greater than 17,000 patient-years of exposure. Dermatol Ther. 2019. https://doi.org/10.1007/s13555-019-00340-3.
Genovese MC, Mysler E, Tomita T, Papp KA, Salvarani C, Schwartzman S, et al. Safety of ixekizumab in adult patients with plaque psoriasis, psoriatic arthritis and axial spondyloarthritis: data from 21 clinical trials. Rheumatology (Oxford). 2020;59(12):3834–44. https://doi.org/10.1093/rheumatology/keaa189.
Gordon KB, Blauvelt A, Papp KA, Langley RG, Luger T, Ohtsuki M, et al. Phase 3 trials of ixekizumab in moderate-to-severe plaque psoriasis. N Engl J Med. 2016;375(4):345–56. https://doi.org/10.1056/NEJMoa1512711.
Griffiths CE, Reich K, Lebwohl M, van de Kerkhof P, Paul C, Menter A, et al. Comparison of ixekizumab with etanercept or placebo in moderate-to-severe psoriasis (UNCOVER-2 and UNCOVER-3): results from two phase 3 randomised trials. Lancet. 2015;386(9993):541–51. https://doi.org/10.1016/S0140-6736(15)60125-8.
Gower-Rousseau C, Salomez JL, Dupas JL, Marti R, Nuttens MC, Votte A, et al. Incidence of inflammatory bowel disease in northern France (1988–1990). Gut. 1994;35(10):1433–8. https://doi.org/10.1136/gut.35.10.1433.
Winthrop KL, Novosad SA, Baddley JW, Calabrese L, Chiller T, Polgreen P, et al. Opportunistic infections and biologic therapies in immune-mediated inflammatory diseases: consensus recommendations for infection reporting during clinical trials and postmarketing surveillance. Ann Rheum Dis. 2015;74(12):2107–16. https://doi.org/10.1136/annrheumdis-2015-207841.
Blauvelt A, Chiricozzi A. The immunologic role of IL-17 in psoriasis and psoriatic arthritis pathogenesis. Clin Rev Allergy Immunol. 2018;55(3):379–90. https://doi.org/10.1007/s12016-018-8702-3.
Reich K, Warren RB, Lebwohl M, Gooderham M, Strober B, Langley RG, et al. Bimekizumab versus secukinumab in plaque psoriasis. N Engl J Med. 2021;385(2):142–52. https://doi.org/10.1056/NEJMoa2102383.
Friedrich M, Pohin M, Powrie F. Cytokine networks in the pathophysiology of inflammatory bowel disease. Immunity. 2019;50(4):992–1006. https://doi.org/10.1016/j.immuni.2019.03.017.
Leppkes M, Neurath MF. Cytokines in inflammatory bowel diseases—update 2020. Pharmacol Res. 2020;158: 104835. https://doi.org/10.1016/j.phrs.2020.104835.
Moschen AR, Tilg H, Raine T. IL-12, IL-23 and IL-17 in IBD: immunobiology and therapeutic targeting. Nat Rev Gastroenterol Hepatol. 2019;16(3):185–96. https://doi.org/10.1038/s41575-018-0084-8.
Li J, Casanova JL, Puel A. Mucocutaneous IL-17 immunity in mice and humans: host defense vs. excessive inflammation. Mucosal Immunol. 2018;11(3):581–9. https://doi.org/10.1038/mi.2017.97.
Hueber W, Sands BE, Lewitzky S, Vandemeulebroecke M, Reinisch W, Higgins PD, et al. Secukinumab, a human anti-IL-17A monoclonal antibody, for moderate to severe Crohn’s disease: unexpected results of a randomised, double-blind placebo-controlled trial. Gut. 2012;61(12):1693–700. https://doi.org/10.1136/gutjnl-2011-301668.
Scharl M, Rogler G. Inflammatory bowel disease pathogenesis: what is new? Curr Opin Gastroenterol. 2012;28(4):301–9. https://doi.org/10.1097/MOG.0b013e328353e61e.
Eppinga H, Poortinga S, Thio HB, Nijsten TEC, Nuij V, van der Woude CJ, et al. Prevalence and phenotype of concurrent psoriasis and inflammatory bowel disease. Inflamm Bowel Dis. 2017;23(10):1783–9. https://doi.org/10.1097/MIB.0000000000001169.
Egeberg A, Thyssen JP, Burisch J, Colombel JF. Incidence and risk of inflammatory bowel disease in patients with psoriasis-a nationwide 20-year cohort study. J Investig Dermatol. 2019;139(2):316–23. https://doi.org/10.1016/j.jid.2018.07.029.
Li WQ, Han JL, Chan AT, Qureshi AA. Psoriasis, psoriatic arthritis and increased risk of incident Crohn’s disease in US women. Ann Rheum Dis. 2013;72(7):1200–5. https://doi.org/10.1136/annrheumdis-2012-202143.
Lo CH, Khalili H, Lochhead P, Song M, Lopes EW, Burke KE, et al. Immune-mediated diseases and risk of Crohn’s disease or ulcerative colitis: a prospective cohort study. Aliment Pharmacol Ther. 2021;53(5):598–607. https://doi.org/10.1111/apt.16210.
Purzycka-Bohdan D, Kisielnicka A, Bohdan M, Szczerkowska-Dobosz A, Sobalska-Kwapis M, Nedoszytko B, et al. Analysis of the potential genetic links between psoriasis and cardiovascular risk factors. Int J Mol Sci. 2021. https://doi.org/10.3390/ijms22169063.
Egeberg A, Skov L, Joshi AA, Mallbris L, Gislason GH, Wu JJ, et al. The relationship between duration of psoriasis, vascular inflammation, and cardiovascular events. J Am Acad Dermatol. 2017;77(4):650-6 e3. https://doi.org/10.1016/j.jaad.2017.06.028.
Egeberg A, Wu JJ, Korman N, Solomon JA, Goldblum O, Zhao F, et al. Ixekizumab treatment shows a neutral impact on cardiovascular parameters in patients with moderate-to-severe plaque psoriasis: results from UNCOVER-1, UNCOVER-2, and UNCOVER-3. J Am Acad Dermatol. 2018;79(1):104-9 e8. https://doi.org/10.1016/j.jaad.2018.02.074.
Elnabawi YA, Dey AK, Goyal A, Groenendyk JW, Chung JH, Belur AD, et al. Coronary artery plaque characteristics and treatment with biologic therapy in severe psoriasis: results from a prospective observational study. Cardiovasc Res. 2019;115(4):721–8. https://doi.org/10.1093/cvr/cvz009.
Choi H, Uceda DE, Dey AK, Abdelrahman KM, Aksentijevich M, Rodante JA, et al. Treatment of psoriasis with biologic therapy is associated with improvement of coronary artery plaque lipid-rich necrotic core: results from a prospective, observational study. Circ Cardiovasc Imaging. 2020;13(9): e011199. https://doi.org/10.1161/CIRCIMAGING.120.011199.
Pouplard C, Brenaut E, Horreau C, Barnetche T, Misery L, Richard MA, et al. Risk of cancer in psoriasis: a systematic review and meta-analysis of epidemiological studies. J Eur Acad Dermatol Venereol. 2013;27(Suppl 3):36–46. https://doi.org/10.1111/jdv.12165.
Vaengebjerg S, Skov L, Egeberg A, Loft ND. Prevalence, incidence, and risk of cancer in patients with psoriasis and psoriatic arthritis: a systematic review and meta-analysis. JAMA Dermatol. 2020;156(4):421–9. https://doi.org/10.1001/jamadermatol.2020.0024.
Cohen BE, Martires KJ, Ho RS. Psoriasis and the risk of depression in the US population: national health and nutrition examination survey 2009–2012. JAMA Dermatol. 2016;152(1):73–9. https://doi.org/10.1001/jamadermatol.2015.3605.
Dowlatshahi EA, Wakkee M, Arends LR, Nijsten T. The prevalence and odds of depressive symptoms and clinical depression in psoriasis patients: a systematic review and meta-analysis. J Investig Dermatol. 2014;134(6):1542–51. https://doi.org/10.1038/jid.2013.508.
Acknowledgements
Funding
This study was funded by Eli Lilly and Company, which contributed to study design, data collection, data analysis, data interpretation, manuscript preparation, and publication decisions. Eli Lilly and Company funded the journal’s Rapid Service fees.
Medical Writing Assistance
Elsa Mevel, PhD provided writing, and editorial assistance. Funding for this assistance was provided by Eli Lilly and Company. The authors thank the study participants, caregivers, and investigators.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, had full access to all the data in this study, take responsibility for the integrity of data and accuracy of the data analysis, and have given their approval for this version to be published.
Author Contributions
All authors contributed to the analysis of the data, interpretation of data, and provided critical revisions of the manuscript for important intellectual content. All authors read and approved the final manuscript.
Disclosures
Christopher E. M Griffiths is supported in part by the National Institute for Health Research (NIHR) Manchester Biomedical Research Centre; has received honoraria and/or research grants from AbbVie, Almirall, Amgen, AnaptysBio, BMS, Celgene Corporation, Eli Lilly and Company, Galderma, GlaxoSmithKline, LEO Pharma, Janssen, MSD, Novartis, Pfizer, Sandoz, Sun Pharmaceuticals, and UCB Pharma; Melinda Gooderham reports personal fees from AbbVie, Actelion Pharmaceuticals, Akros Pharma Inc, Amgen, Arcutis Pharmaceuticals Inc, Boehringer Ingelheim, Bristol-Myers Squibb Company, Celgene Corporation, Dermavant, Dermira Inc, Eli Lilly and Company, Galderma, GlaxoSmithKline, Glenmark, Janssen Inc, LEO Pharma, MedImmune, Merck and Co, Novartis, Pfizer Inc, Regeneron Pharmaceuticals Inc, Roche Laboratories, Sanofi Genzyme, UCB and Valeant Pharmaceuticals Inc.; Jean-Frederic Colombel has received research grants from AbbVie, Janssen Pharmaceuticals, and Takeda; received payment for lectures from AbbVie, Amgen, Allergan, Inc, Ferring Pharmaceuticals, Shire, and Takeda; received consulting fees from AbbVie, Amgen, Arena Pharmaceuticals, Boehringer Ingelheim, Celgene Corporation, Celltrion, Eli Lilly and Company, Enterome, Ferring Pharmaceuticals, Genentech, Janssen Pharmaceuticals, Landos, Ipsen, MedImmune, Merck and Co, Novartis, Pfizer, Shire, Takeda, Tigenix, Viela Bio; and holds stock options in Intestinal Biotech Development and Genfit; Tadashi Terui has received research funds from Maruho, and honoraria for speaker, consultancy, and advisory board membership from: AbbVie, Boehringer Ingelheim, Celgene Corporation, Janssen, Kyowa Hakko Kirin, LEO Pharma, Eli Lilly and Company, Mitsubishi Tanabe Pharma Corporation, Novartis, Sanofi Genzyme, and Taiho Pharmaceutical; Ana P. Accioly, Gaia Gallo, and Danting Zhu are employees and stockholders of Eli Lilly and Company; Andrew Blauvelt has served as a scientific adviser and/or clinical study investigator for AbbVie, Abcentra, Aligos, Almirall, Amgen, Arcutis, Arena, Aslan, Athenex, Boehringer Ingelheim, Bristol-Myers Squibb, Dermavant, EcoR1, Eli Lilly and Company, Evommune, Forte, Galderma, Incyte, Janssen, Landos, LEO Pharma, Novartis, Pfizer, Rapt, Regeneron Pharmaceuticals Inc, Sanofi Genzyme, Sun Pharmaceuticals, UCB Pharma, and Vibliome.
Compliance with Ethics Guidelines
The protocols for all the studies included in this analysis were approved by the Institutional Review Board or Ethics Committee at each participating site. All studies were conducted in accordance with the ethical principles of the Declaration of Helsinki. All eligible patients provided written informed consent before undergoing study-related procedures.
Data Availability
The datasets generated and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Corresponding author
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Griffiths, C.E.M., Gooderham, M., Colombel, JF. et al. Safety of Ixekizumab in Adult Patients with Moderate-to-Severe Psoriasis: Data from 17 Clinical Trials with Over 18,000 Patient-Years of Exposure. Dermatol Ther (Heidelb) 12, 1431–1446 (2022). https://doi.org/10.1007/s13555-022-00743-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13555-022-00743-9