Abstract
Background
Novel topical esmolol is shown to significantly improve wound healing than standard of care. Certain patient-related factors especially anemia and poor glycemic control may impede wound healing.
Objective
To study whether novel topical esmolol may circumvent patient-related factors to improve wound healing in diabetic foot ulcer (DFU).
Methods
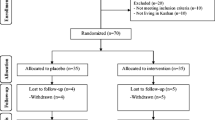
The present study is a double-blind, vehicle (placebo)-controlled, randomized clinical trial in subjects with non-infected DFU of University of Texas grade 1A and 1C. Participants were randomized to receive either topical esmolol gel (Galnobax) with standard of care (SoC), SoC only, and vehicle (Placebo) with SoC in 3:3:1 proportion. The hematologic and biochemistry parameters were evaluated at the screening visit and at every 4 weeks after randomization during treatment phase and at the end of the study (EOS). Outcome was the proportion of complete ulcer closure with reference to baseline hemoglobin, albumin, and HbA1c during the 12-week treatment phase.
Results
A total of 176 subjects were included. Ninety-four out of 140 participants (67.1%) had anemia at baseline. Among anemic participants, 57.4% ulcers closed in the Galnobax group whereas 42.6% closed in the SoC only group during the 12-week treatment phase (p = 0.148, OR = 1.823, 95% CI = 0.80–4.13). One-third participants reported albumin < 4.0 g/dL. Among participants having albumin < 4.0 g/dL (one-third of participants), the proportion of ulcer closure was 60.9% in the Galnobax group compared to 42.1% in the SoC only group (p = 0.225, OR = 2.139, 95% CI = 0.62–7.37). The proportion of ulcer closure in Galnobax with the SoC group was higher (72.5%) compared to the SoC only group (43.5%) (p = 0.0067, OR = 3.427, 95% CI = 1.38–8.48) in participants with poor glycemic control (HbA1c > 8%).
Conclusions
Novel topical esmolol with SoC treatment exhibited significant DFU healing independent of patient-related factors including anemia, hypoalbuminemia, and poor glycemic control.
Similar content being viewed by others
Data Availability
Data pertaining to the manuscript is available on reasonable request from corresponding author.
References
Pradeepa R, Shreya L, Anjana RM, et al. Frequency of iron deficiency anemia in type 2 diabetes - insights from tertiary diabetes care centres across India. Diabetes Metab Syndr. 2022;16(11):102632. https://doi.org/10.1016/j.dsx.2022.102632.
Taderegew MM, Gebremariam T, Tareke AA, Woldeamanuel GG. Anemia and its associated factors among type 2 diabetes mellitus patients attending Debre Berhan Referral Hospital, North-East Ethiopia: a cross-sectional study. J Blood Med. 2020;11:47–58. https://doi.org/10.2147/JBM.S243234.
Guo S, Dipietro LA. Factors affecting wound healing. J Dent Res. 2010;89(3):219–29. https://doi.org/10.1177/0022034509359125.
Chuan F, Zhang M, Yao Y, Tian W, He X, Zhou B. Anemia in patients with diabetic foot ulcer: prevalence, clinical characteristics, and outcome. Int J Low Extrem Wounds. 2016;15(3):220–6. https://doi.org/10.1177/1534734616660224.
Costa RHR, Cardoso NA, Procópio RJ, Navarro TP, Dardik A, de Loiola CL. Diabetic foot ulcer carries high amputation and mortality rates, particularly in the presence of advanced age, peripheral artery disease and anemia. Diabetes Metab Syndr. 2017;11(Suppl 2):S583–7. https://doi.org/10.1016/j.dsx.2017.04.008.
Xie Y, Zhang H, Ye T, Ge S, Zhuo R, Zhu H. The geriatric nutritional risk index independently predicts mortality in diabetic foot ulcers patients undergoing amputations. J Diabetes Res. 2017;2017:5797194. https://doi.org/10.1155/2017/5797194.
Busher JT. Serum albumin and globulin. In: Walker HK, Hall WD, Hurst JW, editors. Clinical Methods: The History, Physical, and Laboratory Examinations. 3rd edition. Boston: Butterworths; 1990. Chapter 101. Available from: https://www.ncbi.nlm.nih.gov/books/NBK204/.
Cheng P, Dong Y, Hu Z, et al. Biomarker prediction of postoperative healing of diabetic foot ulcers: a retrospective observational study of serum albumin. J Wound Ostomy Continence Nurs. 2021;48(4):339–44. https://doi.org/10.1097/WON.0000000000000780.
Soedjana H, Lukman K, Harianti S. Relationship between serum albumin levels and the outcome of split-thickness skin graft in burn injury patients. Ann Burns Fire Disasters. 2021;34(2):157–62.
Margolis DJ, Kantor J, Santanna J, Strom BL, Berlin JA. Risk factors for delayed healing of neuropathic diabetic foot ulcers: a pooled analysis. Arch Dermatol. 2000;136(12):1531–5. https://doi.org/10.1001/archderm.136.12.1531.
AlGoblan A, Alrasheedi I, Basheir O, Haider K. Prediction of diabetic foot ulcer healing in type 2 diabetic subjects using routine clinical and laboratory parameters. Res Rep Endocrine Disord. 2016;6:11–6.
Fesseha BK, Abularrage CJ, Hines KF, et al. Association of hemoglobin A1c and wound healing in diabetic foot ulcers. Diabetes Care. 2018;41(7):1478–85. https://doi.org/10.2337/dc17-1683.
Lane KL, Abusamaan MS, Voss BF, et al. Glycemic control and diabetic foot ulcer outcomes: a systematic review and meta-analysis of observational studies. J Diabetes Complications. 2020;34(10):107638. https://doi.org/10.1016/j.jdiacomp.2020.107638.
Rastogi A, Kulkarni S, Deshpande S, Driver V, Berman H, Bal A, Deshmukh M, Nair H. Novel topical esmolol hydrochloride (Galnobax) for diabetic foot wound: phase 1 /2, multicentre, randomized, double-blind, vehicle-controlled, parallel-group study. Adv Wound Care (New Rochelle). 2022. https://doi.org/10.1089/wound.2022.0093.
Rastogi A, Kulkarni SA, Agarwal S, et al. Topical esmolol hydrochloride as a novel treatment modality for diabetic foot ulcers: a phase 3 randomized clinical trial. JAMA Netw Open. 2023;6(5):e2311509. https://doi.org/10.1001/jamanetworkopen.2023.11509.
Gezawa ID, Ugwu ET, Ezeani I, Adeleye O, Okpe I, Enamino M. Anemia in patients with diabetic foot ulcer and its impact on disease outcome among Nigerians: results from the MEDFUN study. PLoS One. 2019;14(12):e0226226. Published 2019 Dec 17. https://doi.org/10.1371/journal.pone.0226226.
Khanbhai M, Loukogeorgakis S, Wright J, Hurel S, Richards T. Anaemia, inflammation, renal function, and the diabetic foot: what are the relationships. Diabetic Foot J. 2012;15(4):150–8.
Haroon ZA, Amin K, Jiang X, Arcasoy MO. A novel role for erythropoietin during fibrin-induced wound-healing response. Am J Pathol. 2003;163:993–1000.
Kulkarni SA, Deshpande SK, Rastogi A. Novel topical esmolol hydrochloride improves wound healing in diabetes by inhibiting aldose reductase, generation of advanced glycation end products, and facilitating the migration of fibroblasts. Front Endocrinol (Lausanne). 2022;13:926129. https://doi.org/10.3389/fendo.2022.926129.
Utariani A, Rahardjo E, Perdanakusuma DS. Effects of albumin infusion on serum levels of albumin, proinflammatory cytokines (TNF-α, IL-1, and IL-6), CRP, and MMP-8; tissue expression of EGRF, ERK1, ERK2, TGF-β, collagen, and MMP-8; and wound healing in Sprague Dawley rats. Int J Inflam. 2020;20(2020):3254017. https://doi.org/10.1155/2020/3254017.
Nagachinta T, Stephens M, Reitz B, Polk BF. Risk factors for surgical-wound infection following cardiac surgery. J Infect Dis. 1987;156(6):967–73. https://doi.org/10.1093/infdis/156.6.967.
Foley EF, Borlase BC, Dzik WH, Bistrian BR, Benotti PN. Albumin supplementation in the critically ill: a prospective, randomized trial. Arch Surg. 1990;125(6):739–42. https://doi.org/10.1001/archsurg.1990.01410180063012.
Dutta A, Bhansali A, Rastogi A. Early and intensive glycemic control for diabetic foot ulcer healing: a prospective observational nested cohort study. Int J Low Extrem Wounds. 2021;19:15347346211033458. https://doi.org/10.1177/15347346211033458.
Rastogi A, Goyal G, Kesavan R, Bal A, Kumar H, Mangalanadanam P, Kamath P, Jude EB, Armstrong DG, Bhansali A. Long term outcomes after incident diabetic foot ulcer: multicenter large cohort prospective study (EDI-FOCUS investigators) epidemiology of diabetic foot complications study: epidemiology of diabetic foot complications study. Diabetes Res Clin Pract. 2020;162:108113. https://doi.org/10.1016/j.diabres.2020.108113.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Sudhir Kulkarni and Ashu Rastogi. The first draft of the manuscript was written by Sudhir Kulkarni and Ashu Rastogi, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Involved human participants. A written and informed consent was obtained from all participants.
Conflict of interest
Dr. Sudhir Kulkarni has the patent of the topical preparation of Esmolol (Galnobax). The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Rastogi, A., Singh, R., Adhikari, U. et al. Effect of patient and wound characteristics on diabetic foot ulcer healing in phase 3 study of novel topical esmolol hydrochloride. Int J Diabetes Dev Ctries (2024). https://doi.org/10.1007/s13410-024-01336-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s13410-024-01336-2