Abstract
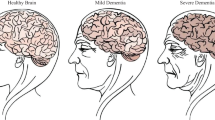
Deep learning algorithms have begun to be used in medical image processing studies, especially in the last decade. MRI is used in the diagnosis of Alzheimer’s disease, a type of dementia disease, which is the 7th among the diseases that cause death in the world. Alzheimer’s disease has no known cure in the literature, so it is important to attempt treatment before starting the irreversible path by diagnosing the pre-illness stages. In this study, the previous stages of Alzheimer’s disease were classified as normal, mild cognitive impairment, and Alzheimer’s disease through brain MRIs. Different models using CNN architecture were used to classify 2182 image objects obtained from the ADNI database. The study was presented in a very comprehensive comparison framework, and the performances of 29 different pre-trained models on images were evaluated. The accuracy values of each model and the precision, specificity, and sensitivity rates of each class were determined. In the study, the EfficientNetB0 model provided the highest accuracy at the test stage with an accuracy rate of 92.98%. In the comparative evaluation stage with the confusion matrix, the highest rates of precision, sensitivity, and specificity values of the Alzheimer’s disease class were achieved by EfficientNetB3 (89.78%), EfficientNetB2 (94.42%), and EfficientNetB3 (97.28%) models, respectively. The results of the study showed that among the pre-trained models, EfficientNet models achieved a high rate of classification performance as the models with the highest performance. This study will contribute to clinical studies in early prevention by detecting Alzheimer’s disease before it occurs.










Similar content being viewed by others
References
WHO. The top 10 causes of death (2020). https://www.who.int/news-room/fact-sheets/detail/the-top-10-causes-of-death.
WHO. Dementia (2020). https://www.who.int/news-room/fact-sheets/detail/dementia.
Soria Lopez, J.A.; González, H.M.; Léger, Gabriel C.: Chapter 13 - alzheimer’s disease. In Steven T. Dekosky and Sanjay Asthana, editors, Geriatric Neurology, volume 167 of Handbook of Clinical Neurology, pp. 231–255. Elsevier, (2019). https://doi.org/10.1016/B978-0-12-804766-8.00013-3. https://www.sciencedirect.com/science/article/pii/B9780128047668000133.
Penney, J.; Ralvenius, W.T.; Tsai, L.-H.: Modeling Alzheimer’s disease with ipsc-derived brain cells. Mol. Psych. 25(1), 148–167 (2020). https://doi.org/10.1038/s41380-019-0468-3.
Wan, Y.-W.; Al-Ouran, R.; Mangleburg, C.G.; Perumal, T.M.; Lee, T.V.; Allison, K.; Swarup, V.; Funk, C.C.; Gaiteri, C.; Allen, M.; Wang, M.; Neuner, S.M.; Kaczorowski, C.C.; Philip, V.M.; Howell, G.R.; Martini-Stoica, H.; Zheng, H.; Mei, H.; Zhong, X.; Kim, J.W.; Dawson, V.L.; Dawson, T.M.; Pao, P.-C.; Tsai, L.-H.; Haure-Mirande, J.-V.; Ehrlich, M.E.; Chakrabarty, P.; Levites, Y.; Wang, X.; Dammer, E.B.; Srivastava, G.; Mukherjee, S.; Sieberts, S.K.; Omberg, L.; Dang, K.D.; Eddy, J.A.; Snyder, P.; Chae, Y.; Amberkar, S.; Wei, W.; Hide, W.; Preuss, C.; Ergun, A.; Ebert, P.J.; Airey, D.C.; Mostafavi, S.; Yu, L.; Klein, H.-U.; Carter, G.W.; Collier, D.A.; Golde, T.E.; Levey, A.I.; Bennett, D.A.; Estrada, K.; Matthew Townsend, T.; Zhang, B.; Schadt, E.; De Jager, P.L.; Price, N.D.; Ertekin-Taner, N.; Liu, Z.; Shulman, J.M.; Mangravite, L.M.; Logsdon, B.A.: Meta-analysis of the alzheimer’s disease human brain transcriptome and functional dissection in mouse models. Cell Rep. 32(2):107908, (2020). ISSN 2211-1247. https://doi.org/10.1016/j.celrep.2020.107908. https://www.sciencedirect.com/science/article/pii/S2211124720308895.
Leandrou, S.; Petroudi, S.; Kyriacou, P.A.; Reyes-Aldasoro, C.C.; Pattichis, C.S.: Quantitative MRI brain studies in mild cognitive impairment and Alzheimer’s disease: a methodological review. IEEE Rev. Biomed. Eng. 11, 97–111 (2018). https://doi.org/10.1109/rbme.2018.2796598.
Alzheimer’s Association.: 2015 Alzheimer’s disease facts and figures. Alzheimer’s and Dementia 11(3):332–384, (2015). https://doi.org/10.1016/j.jalz.2015.02.003.
Wang, Z.; Zhu, X.; Adeli, E.; Zhu, Y.; Nie, F.; Munsell, B.; Guorong, W.: Multi-modal classification of neurodegenerative disease by progressive graph-based transductive learning. Med. Image Anal. 39, 218–230 (2017). https://doi.org/10.1016/j.media.2017.05.003.
Hadjichrysanthou, C.; McRae-McKee, K.; Evans, S.; de Wolf, F.; Anderson, R.M.: Initiative for the Alzheimer’s Disease Neuroimaging: Potential factors associated with cognitive improvement of individuals diagnosed with mild cognitive impairment or dementia in longitudinal studies. J. Alzheimer’s Dis. 66, 587–600 (2018). https://doi.org/10.3233/JAD-180101.
Sullivan, M.D.; Anderson, J.A.E.; Turner, G.R.; Nathan Spreng, R.: Intrinsic neurocognitive network connectivity differences between normal aging and mild cognitive impairment are associated with cognitive status and age. Neurobiol. Aging 73:219–228 (2019). https://doi.org/10.1016/j.neurobiolaging.2018.10.001.
Molinuevo, J.L.; Ayton, S.; Batrla, R.; Bednar, M.M.; Bittner, T.; Cummings, J.; Fagan, A.M.; Hampel, H.; Mielke, M.M.; Mikulskis, A.; O’Bryant, S.; Scheltens, P.; Sevigny, J.; Shaw, L.M.; Soares, H.D.; Tong, G.; Trojanowski, J.Q.; Zetterberg, H.; Blennow, K.: Current state of Alzheimer’s fluid biomarkers. Acta Neuropathol. 136(6), 821–853 (2018). https://doi.org/10.1007/s00401-018-1932-x.
Villa, C.; Lavitrano, M.; Salvatore, E.; Combi, R.: Molecular and imaging biomarkers in Alzheimer’s disease: A focus on recent insights. J. Pers. Med. 10(3), 1 (2020). https://doi.org/10.3390/jpm10030061.
Cooper, Yonatan A.; Nachun, Daniel; Dokuru, Deepika; Yang, Zhongan; Karydas, Anna M.; Serrero, Ginette; Yue, Binbin; Initiative, Alzheimer’s Disease Neuroimaging.; Boxer, Adam L.; Miller, Bruce L.; Coppola, Giovanni: Progranulin levels in blood in alzheimer’s disease and mild cognitive impairment. Annals of Clinical and Translational Neurology 5(5), 616–629 (2018) ISSN 2328-9503. https://doi.org/10.1002/acn3.560. https://onlinelibrary.wiley.com/doi/abs/10.1002/acn3.560.
Goldstein, F.C.; Milloy, A.; Loring, D.W.: Incremental validity of montreal cognitive assessment index scores in mild cognitive impairment and alzheimer disease. Dement. Geriatr. Cogn. Disord. 45(1), 49–55 (2018). https://doi.org/10.1159/000487131.
Salvatore, C.; Cerasa, A.; Castiglioni, I.: Mri characterizes the progressive course of ad and predicts conversion to Alzheimer’s dementia 24 months before probable diagnosis. Front. Aging Neurosci. 10(135), 1 (2018). https://doi.org/10.3389/fnagi.2018.00135.
Turing, A.M.: I. Computing machinery and intelligence. Mind 59(236), 433–460 (1950). https://doi.org/10.1093/mind/LIX.236.433.
McCarthy, J.; Minsky, M.L.; Rochester, N.; Shannon, C.E.: A proposal for the Dartmouth summer conference on artificial intelligence. Rep. Dartmouth Coll. 31(08), 1955 (1955)
Jha, D.; Alam, S.; Pyun, J.-Y.; Lee, K.; Ho, K., Goo-Rak.: Alzheimer’s disease detection using extreme learning machine, complex dual tree wavelet principal coefficients and linear discriminant analysis. J. Med. Imag. Health Inf. 8(5), 881–890 (2018). https://doi.org/10.1166/jmihi.2018.2381.
Jie, B.; Liu, M.; Shen, D.: Integration of temporal and spatial properties of dynamic connectivity networks for automatic diagnosis of brain disease. Med. Image Anal. 47, 81–94 (2018). https://doi.org/10.1016/j.media.2018.03.013.
Niu, Yan; Wang, Bin; Zhou, Mengni; Xue, Jiayue; Shapour, Habib; Cao, Rui; Cui, Xiaohong; Jinglong, Wu.; Xiang, Jie: Dynamic complexity of spontaneous bold activity in alzheimer’s disease and mild cognitive impairment using multiscale entropy analysis. Front. Neurosci. 12(677), 1 (2018). https://doi.org/10.3389/fnins.2018.00677.
Sampath, R.; Indumathi, J.: Earlier detection of Alzheimer disease using n-fold cross validation approach. J. Med. Syst. 42(11), 217 (2018). https://doi.org/10.1007/s10916-018-1068-5.
Li, D.; Iddi, S.; Thompson, W.K.; Rafii, M.S.; Aisen, P.S.; Donohue, M.C.; Initiative, Alzheimer’s Disease Neuroimaging.: Bayesian latent time joint mixed-effects model of progression in the Alzheimer’s disease neuroimaging initiative. Alzheimer’s and Dement. Diagnos., Assessm. Dis. Monit. 10(1), 657–668 (2018). https://doi.org/10.1016/j.dadm.2018.07.008.
Buyrukoğlu, S.: Early detection of alzheimer’s disease using data mining: comparision of ensemble feature selection approaches. Konya Mühendislik Bilimleri Dergisi 9(1), 50–61 (2021). https://doi.org/10.36306/konjes.731624.
Rajendra Acharya, U.; Fernandes, S.L.; WeiKoh, J.E.; Ciaccio, E.J.; Mohd, F.; Mohd, K.; John, T.U.; Rajinikanth, V.; Yeong, C.H.: Automated detection of alzheimer’s disease using brain mri images-a study with various feature extraction techniques. J. Med. Syst. 43(9), 302 (2019). https://doi.org/10.1007/s10916-019-1428-9.
Lu, S.; Xia, Y.; Cai, W.; Fulham, M.; Feng, D.D.: Early identification of mild cognitive impairment using incomplete random forest-robust support vector machine and fdg-pet imaging. Comput. Med. Imag. Gr. 60, 35–41 (2017). https://doi.org/10.1016/j.compmedimag.2017.01.001.
Savaş, S.; Topaloğlu, N.; Kazcı, Ö.; Koşar, P.N.: Performance comparison of carotid artery intima media thickness classification by deep learning methods. In SETSCI Conference Proceedings, volume 4(5), pp. 125–131. International Congress on Human–Computer Interaction, Optimization, and Robotic Applications (2019). https://doi.org/10.36287/setsci.4.5.025.
Luo, S.; Li, X.L.J.: Automatic Alzheimer’s disease recognition from mri data using deep learning method. J. Appl. Math. Phys. 5(9), 1892–1898 (2017)
Lin, W.; Tong, T.; Gao, Q.; Guo, D.; Du, X.; Yang, Y.; Guo, G.; Xiao, M.; Du, M.; Qu, X.: The Alzheimer’s Disease Neuroimaging Initiative. Convolutional neural networks-based MRI image analysis for the Alzheimer’s disease prediction from mild cognitive impairment. Front. Neurosci. 12(777), 1 (2018). https://doi.org/10.3389/fnins.2018.00777.
Li, F.; Liu, M.: Alzheimer’s disease diagnosis based on multiple cluster dense convolutional networks. Comput. Med. Imag. Gr. 70, 101–110 (2018). https://doi.org/10.1016/j.compmedimag.2018.09.009.
Bi, X.; Jiang, Q.; Sun, Q.; Shu, Q.; Liu, Y.: Analysis of Alzheimer’s disease based on the random neural network cluster in FMRI. Front. Neuroinf. 12(60), 1 (2018). https://doi.org/10.3389/fninf.2018.00060.
Suk, H.-I.; Lee, S.-W.; Shen, D.: Deep ensemble learning of sparse regression models for brain disease diagnosis. Med. Image Anal. 37, 101–113 (2017). https://doi.org/10.1016/j.media.2017.01.008.
Liu, M.; Cheng, D.; Wang, K.; Wang, Y.: Initiative the Alzheimer’s Disease Neuroimaging: Multi-modality cascaded convolutional neural networks for Alzheimer’s disease diagnosis. Neuroinformatics 16(3):295–308. https://doi.org/10.1007/s12021-018-9370-4.
Yiming, D.; Jae, H.S.; Kawczynski, M.G.; Trivedi, H.; Harnish, R.; Jenkins, N.W.; Lituiev, D.; Copeland, T.P.; Aboian, M.S.; Aparici, C.M.; Behr, S.C.; Flavell, R.R.; Huang, S.-Y.; Zalocusky, K.A.; Nardo, L.; Seo, Y.; Hawkins, R.A.; Pampaloni, M.H.; Hadley, D.; Franc, B.L.: A deep learning model to predict a diagnosis of Alzheimer disease by using 18f-fdg pet of the brain. Radiology 290(2), 456–464 (2019). https://doi.org/10.1148/radiol.2018180958.
Yapıcı, M.M.; Tekerek, A.; Topaloğlu, N.: Literature review of deep learning research areas. Gazi Mühendislik Bilimleri Dergisi (GMBD) 5(3), 188–215 (2019)
Savaş, S.; Topaloğlu, N.; Kazcı, Ö.; Koşar, P.N.: Classification of carotid artery intima media thickness ultrasound images with deep learning. J. Med. Syst. 43(8), 273 (2019). https://doi.org/10.1007/s10916-019-1406-2.
Krizhevsky, A.; Sutskever, I.; Hinton, G.E.: Imagenet classification with deep convolutional neural networks. Adv. Neural. Inf. Process. Syst. 25, 1097–1105 (2012)
Zeiler, M.D.; Fergus, R.: Visualizing and understanding convolutional networks. In: European conference on computer vision, pp. 818–833. Springer (2014).
He, K.; Zhang, X.; Ren, S.; Sun, J.: Deep residual learning for image recognition. In: Proceedings of the IEEE conference on computer vision and pattern recognition, pp. 770–778 (2016).
Simonyan, K.; Zisserman, A.: Very deep convolutional networks for large-scale image recognition. arXiv preprint arXiv:1409.1556 (2014).
LeCun, Y.; Bottou, L.; Bengio, Y.; Haffner, P.: Gradient-based learning applied to document recognition. Proc. IEEE 86(11), 2278–2324 (1998)
Keras. Keras applications (2021). https://keras.io/api/applications/.
ADNI. Alzheimer’s disease neuroimaging initiative (2021). http://adni.loni.usc.edu/.
Daldal, N.; Cömert, Z.; Polat, K.: Automatic determination of digital modulation types with different noises using convolutional neural network based on time-frequency information. Appl. Soft Comput. 86, 105834 (2020). https://doi.org/10.1016/j.asoc.2019.105834
LeCun, Y.; Bengio, Y.; Hinton, G.: Deep learning. Nature 521(7553), 436–444 (2015)
Weisstein, E.W.: Convolution (2021). https://mathworld.wolfram.com/Convolution.html.
Gao, B.; Pavel, L.: On the properties of the softmax function with application in game theory and reinforcement learning. arXiv preprint arXiv:1704.00805 (2017).
Wikipedia. Softmax function, (2021). https://en.wikipedia.org/wiki/Softmax_function.
Gholamalinezhad, H.; Khosravi, H.: Pooling methods in deep neural networks, a review. arXiv:2009.07485 (2020).
Srivastava, N.; Hinton, G.; Krizhevsky, A.; Sutskever, I.; Salakhutdinov, R.: Dropout: A simple way to prevent neural networks from overfitting. J. Mach. Learn. Res. 15, 1929–1958 (2014)
Amidi, A.; Amidi, S.: Convolutional neural networks cheatsheet (2018). https://stanford.edu/~shervine/teaching/cs-230/cheatsheet-convolutional-neural-networks.
Toprak, T.; Selver, M.A.; Secmen, M.; Zoral, E.Y.: Utilizing resonant scattering signal characteristics via deep learning for improved classification of complex targets. Turk. J. Electr. Eng. Comput. Sci. 29(1), 334–348 (2021). https://doi.org/10.3906/elk-2002-101.
Usmani, Z.: (2018). https://www.kaggle.com/getting-started/44916.
Colab.: (2021). https://research.google.com/colaboratory/faq.html.
Zhao, H.; Gallo, O.; Frosio, I.; Kautz, J.: Loss functions for image restoration with neural networks. IEEE Trans. Comput. Imaging 3(1), 47–57 (2017). https://doi.org/10.1109/TCI.2016.2644865.
Engle, R.F.: On the limitations of comparing mean square forecast errors: Comment. J. Forecast. 12(8), 642–644 (1993). https://doi.org/10.1002/for.3980120805.
Peltarion.: Categorical crossentropy math, (2021). https://peltarion.com/knowledge-center/documentation/modeling-view/build-an-ai-model/loss-functions/categorical-crossentropy.
Christoffersen, P.; Jacobs, K.: The importance of the loss function in option valuation. J. Financ. Econ. 72(2), 291–318 (2004). https://doi.org/10.1016/j.jfineco.2003.02.001.
Acknowledgements
Data collection and sharing for this project were funded by the Alzheimer’s Disease Neuroimaging Initiative (ADNI) (National Institutes of Health Grant U01 AG024904) and DOD ADNI (Department of Defense award number W81XWH-12-2-0012). ADNI is funded by the National Institute on Aging, the National Institute of Biomedical Imaging and Bioengineering, and through generous contributions from the following: AbbVie, Alzheimer’s Association; Alzheimer’s Drug Discovery Foundation; Araclon Biotech; BioClinica, Inc.; Biogen; Bristol-Myers Squibb Company; CereSpir, Inc.; Cogstate; Eisai Inc.; Elan Pharmaceuticals, Inc.; Eli Lilly and Company; EuroImmun; F. Hoffmann-La Roche Ltd and its affiliated company Genentech, Inc.; Fujirebio; GE Healthcare; IXICO Ltd.; Janssen Alzheimer Immunotherapy Research & Development, LLC.; Johnson & Johnson Pharmaceutical Research & Development LLC.; Lumosity; Lundbeck; Merck & Co., Inc.; Meso Scale Diagnostics, LLC.; NeuroRx Research; Neurotrack Technologies; Novartis Pharmaceuticals Corporation; Pfizer Inc.; Piramal Imaging; Servier; Takeda Pharmaceutical Company; and Transition Therapeutics. The Canadian Institutes of Health Research is providing funds to support ADNI clinical sites in Canada. Private sector contributions are facilitated by the Foundation for the National Institutes of Health (www.fnih.org). The grantee organization is the Northern California Institute for Research and Education, and the study is coordinated by the Alzheimer’s Therapeutic Research Institute at the University of Southern California. ADNI data are disseminated by the Laboratory for Neuro Imaging at the University of Southern California.
Funding
There is no funding for this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The author declares that there is no conflict of interest.
Rights and permissions
About this article
Cite this article
Savaş, S. Detecting the Stages of Alzheimer’s Disease with Pre-trained Deep Learning Architectures. Arab J Sci Eng 47, 2201–2218 (2022). https://doi.org/10.1007/s13369-021-06131-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13369-021-06131-3