Abstract
Quality improvement (QI) in healthcare involves implementing small iterative changes by a team of people using a simple structured framework to resolve problems, improve systems, and to improve patient outcomes. These efforts are especially important in a resource-limited setting where infrastructure, staff and funds are meagre. The concept of QI often appears complex to a new careprovider who feels intimidated to participate in change activities. In this article, we describe our experience with QI activities to address various issues in the Neonatal intensive care unit. QI efforts resulted in improved patient outcomes, and motivated careproviders. QI is a continuous activity and can be done easily if the team is willing to learn from their experiences and use those lessons to adapt, adopt or abandon changes, and improve further. Our institute has also developed Point of Care Quality Improvement (POCQI), a free online resource for learning the science of QI, and also serves as a platform for sharing QI work.
Similar content being viewed by others
References
Batalden PB, Davidoff F. What is “quality improvement” and how can it transform healthcare? Qual Saf Health Care. 2007;16:2–3.
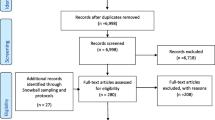
Zaka N, Alexander EC, Manikam L, Norman ICF, Akhbari M, Moxon S, et al. Quality improvement initiatives for hospitalised small and sick newborns in low- and middle-income countries: a systematic review. Implement Sci. 2018;13:20.
Singh M, Paul VK, Deorari AK, Ray D, Murali MV, Sundaram KR. Strategies which reduced sepsis-related neonatal mortality. Indian J Pediatr. 1988;55:955–60.
Mukherjee SB, Bandyopadhyay T. Perinatal mortalitywhat has changed? Indian Pediatr. 2016;53;242–3.
Darmstadt GL, Ahmed ASN, Saha SK, Azad Chowdhury MA, Alam MA, Khatun M, et al. Infection control practices reduce nosocomial infections and mortality in preterm infants in Bangladesh. J Perinatol. 2005;25: 331–5.
Varkey P, Kollengode A. A framework for healthcare quality improvement in India: the time is here and now! J Postgrad Med. 2011;57:237–41.
Pittet D. Improving compliance with hand hygiene in hospitals. Infect Control Hosp Epidemiol. 2000;21:381–6.
Gopalakrishnan S, Agarwal R, Paul VK, Deorari AK. Effect of stepwise interventions aimed at improving hand hygiene compliance among healthcare providers in a level III neonatal intensive care unit: Before and after study: Dissertation submitted to the faculty of Department of Pediatrics, AIIMS, New Delhi 2015.
Johnston M, Landers S, Noble L, Szucs KLV. Breastfeeding and the use of human milk. Pediatrics. 2012;129:e827–41.
Furman L, Minich N, Hack M. Correlates of lactation in mothers of very low birth weight infants. Pediatrics. 2002;109:e57.
Sethi A, Joshi M, Thukral A, Dalal JS, Deorari AK. A quality improvement initiative: improving exclusive breastfeeding rates of preterm neonates. Indian J Pediatr. 2017;84:322–5.
Sivanandan S, Jeeva Sankar M, Thukral A, Agarwal R, Paul VK, Deorari AK. Quality initiative on implementation of golden hour bundle to improve outcomes of preterm neonates <32 weeks gestation: focus on thermoregulation: Dissertation submitted to the faculty of Department of Pediatrics, AIIMS, New Delhi, 2016.
Perla RJ, Provost LP, Murray SK. The run chart: A simple analytical tool for learning from variation in healthcare processes. BMJ Qual Saf. 2011;20:46–51.
Benneyan JC, Lloyd RC, Plsek PE. Statistical process control as a tool for research and healthcare improvement. Qual Saf Health Care. 2003;12:458–64.
Datta V, Saili A, Goel S, Sooden A, Singh M, Vaid S, et al. Reducing hypothermia in newborns admitted to a neonatal care unit in a large academic hospital in New Delhi, India. BMJ Open Qual. 2017;6:e000183.
Colin WB, Scott JA. Breastfeeding: Reasons for starting, reasons for stopping and problems along the way. Breastfeed Rev. 2002;10:13–9.
Mangla MK, Jeeva Sankar M, Deorari AK, Thukral A, Agarwal R, Paul VK. Quality improvement study to reduce incidence of breastfeeding problems at discharge in postnatal mothers who delivered at term gestation: Dissertation submitted to the faculty of Department of Pediatrics, AIIMS, New Delhi; 2017.
Jensen D, Wallace S, Kelsay P. LATCH: A breastfeeding charting system and documentation tool. J Obstet Gynecol Neonatal Nurs. 1994;23:27–32.
Mainz J. Defining and classifying clinical indicators for quality improvement. Int J Qual Health Care. 2003;15:523–30.
Davidoff F, Batalden P, Stevens D, Ogrinc G, Mooney S, Group SD. Publication guidelines for quality improvement in health care: Evolution of the SQUIRE project. Qual Saf Health Care. 2008;17:i3–9.
Baker DP, Day R, Salas E. Teamwork as an essential component of high-reliability organizations. Health Serv Res. 2006;41:1576–98.
Bentley TG, Effros RM, Palar K, Keeler EB. Waste in the US health care system: A conceptual framework. Milbank Q. 2008;86:629–59.
Harolds J. Quality and safety in health care, part I: Five pioneers in quality. Clin Nucl Med. 2015;40:660–2.
Barker PM, Reid A, Schall MW. A framework for scaling up health interventions: Lessons from large-scale improvement initiatives in Africa. Implement Sci. 2016;11:12.
Nembhard IM. Learning and improving in quality improvement collaboratives: Which collaborative features do participants value most? Health Serv Res. 2009;44:359–78.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sivanandan, S., Sethi, A., Joshi, M. et al. Gains from Quality Improvement Initiatives — Experience from a Tertiary-care Institute in India. Indian Pediatr 55, 809–817 (2018). https://doi.org/10.1007/s13312-018-1386-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13312-018-1386-1