Abstract
Objective
To describe clinical features and early neurological outcomes in neonatal Chikungunya.
Methods
Clinical, pathological and radiological details of neonates with acute encephalitic features and typical rash, later diagnosed as Chikungunya, are presented. Neurodevelopmental evaluation and imaging was done at discharge/three months.
Results
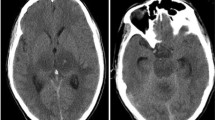
Abnormal neurological examination with fever was typical presentation in all 13 babies with/without seizures/peri-oral rashes; 12 had persistent neurological abnormalities at discharge. A follow-up at three months revealed continued neurodevelopmental deficits. Neuroimaging abnormalities were seen in eight out of ten cases.
Conclusions
Perinatal Chikungunya should be considered in neonates presenting within first week with fever, encephalopathy and perioral rashes with/without seizures with history of maternal Chikungunya within last week before delivery.
Similar content being viewed by others
References
Directorate General of Health Services, Ministry of Health and Family Welfare, Government of India. National Vector Borne Disease Control Programme. Available from: https://doi.org/nvbdcp.gov.in/chik-cd.html. Accessed January 28, 2018.
Da Cunha RV, Trinta KS. Chikungunya virus: Clinical aspects and treatment–A review. Mem Inst Oswaldo Cruz. 2017;112:523–31.
Chandak NH, Kashyap RS, Kabra D, Karandikar P, Saha SS, Morey SH, et al. Neurological complications of Chikungunya virus infection. Neurol India. 2009;57:177–80.
MacDonald MG, Seshia MMK. Avery’s Neonatology: Pathophysiology and Management of the Newborn. 7th ed; 2015. p. 967.
Valamparampil JJ, Chirakkarot S, Letha S, Jayakumar C, Gopinathan KM. Clinical profile of Chikungunya in infants. Indian J Pediatr. 2009;76:151–5.
Lenglet Y, Barau G, Robillard PY, Randrianaivo H, Michault A, Bouveret A, et al. Chikungunya infection in pregnancy: Evidence for intrauterine infection in pregnant women and vertical transmission in the parturient. Survey of the Reunion Island outbreak. J Gynecol Obstet Biol Reprod (Paris). 2006;35:578–83.
Torres JR, Falleiros–Arlant LH, Duenas L, Pleitez–Navarrete J, Salgado DM, Castillo JB. Congenital and perinatal complications of chikungunya fever: A Latin American experience. Int J Infect Dis. 2016 Oct;51:85–8.
Mohanty I, Dash M, Sahu S, Narasimham MV, Panda P, Padhi S. Seroprevalence of chikungunya in Southern Odisha. J Family Med Prim Care. 2013;2:33–6.
Couderc T, Chretien F, Schilte C, Disson O, Brigitte M, Guivel–Benhassine F, et al. A mouse model for Chikungunya: Young age and inefficient type–I interferon signaling are risk factors for severe disease. PLoS Pathog. 2008;4:e29.
Gerardin P, Samperiz S, Ramful D, Boumahni B, Bintner M, Alessandri JL, et al. Neurocognitive outcome of children exposed to perinatal mother–to–child Chikungunya virus infection: The CHIMERE cohort study on Reunion Island. PLoS Negl Trop Dis. 2014;8:e2996.
Seetharam KA, Sridevi K, Vidyasagar P. Cutaneous manifestations of chikungunya fever. Indian Pediatr. 2012;49:51–3.
Gopakumar H, Ramachandran S. Congenital chikungunya. J Clin Neonatol. 2012;1:155–6.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Maria, A., Vallamkonda, N., Shukla, A. et al. Encephalitic presentation of Neonatal Chikungunya: A Case Series. Indian Pediatr 55, 671–674 (2018). https://doi.org/10.1007/s13312-018-1356-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13312-018-1356-7