Abstract
Objective
To compare the outcomes of preterm infants with respiratory distress initiated on either Heated Humidified High Flow Nasal Cannula or Nasal Continuous Positive Airway Pressure as a primary mode of respiratory support.
Study Design
Prospective observational cohort study
Setting
Tertiary care level III neonatal intensive care unit
Participants
88 preterm infants between 28 to 34 weeks of gestation with mild to moderate respiratory distress within 6 hours of birth.
Intervention
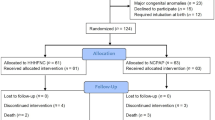
Eligible infants were treated either with Heated Humidified High Flow Nasal Cannula (n=46) or Nasal Continuous Positive Airway Pressure (n=42).
Primary outcome
Need for mechanical ventilation within 72 hrs of initiating support.
Results
Baseline demographic characteristics were comparable between the two groups. There was no difference in the requirement of mechanical ventilation between Heated Humidified High Flow Nasal Cannula (19.5%) and Nasal Continuous Positive Airway Pressure (26.2%) groups [RD–0.74 (95% CI 0.34–1.62; P =0.46)]. Moderate or severe nasal trauma occurred less frequently with Heated Humidified High Flow Nasal Cannula (10.9%) in comparison to Nasal Continuous Positive Airway Pressure (40.5%) (P= 0.004).
Conclusion
Heated Humidified High Flow Nasal Cannula was comparable to Nasal Continuous Positive Airway Pressure as a primary respiratory support for preterm infants with respiratory distress, with lesser incidence of nasal trauma.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Stevens TP, Harrington EW, Blennow M, Soll RF. Early surfactant administration with brief ventilation vs selective surfactant and continued mechanical ventilation for preterm infants with or at risk for respiratory distress syndrome. Cochrane Database Syst Rev. 2007;4:CD003063.
DiBlasi RM. Neonatal noninvasive ventilation techniques: do we really need to intubate? Respir Care. 2011;56: 1273–94.
Diblasi RM. Nasal continuous positive airway pressure (CPAP) for the respiratory care of the newborn infant. Respir Care. 2009;54:1209–35.
Bonner KM, Mainous RO. The nursing care of the infant receiving bubble CPAP therapy. Adv Neonatal Care. 2008;8:78–95.
McCoskey L. Nursing care guidelines for prevention of nasal breakdown in neonates receiving nasal CPAP. Adv Neonatal Care. 2008;8:116–24.
A. de Clerk. Humidified high-flow nasal cannula. Is it the new and improved CPAP? Adv Neonatal Care. 2008; 8: 98–106.
Nath P, Ponnusamy V, Willis K, Bissett L, Clarke P. Current practices of high and low flow oxygen therapy and humidification in UK neonatal units. Pediatr Int. 2010;52: 893–4.
Hough JL, Shearman AD, Jardine LA, Davies MW. Humidified high flow nasal cannulae: current practice in Australasian nurseries, a survey. J Paediatr Child Health. 2012;48:106–13.
Manley BJ, Owen LS, Doyle LW, Andersen CC, Cartwright DW, Pritchard MA et al. Highflow nasal cannulae in very preterm infants after extubation. N Engl J Med. 2013;369:1425–33.
Yoder BA, Stoddard RA, Li M, King J, Dirnberger DR, Abbasi S. Heated, humidified high-low nasal cannula versus nasal CPAP for respiratory support in neonates. Pediatrics. 2013;131:1482–90.
Ballard JL, Khoury JC, Wedig K, Wang L, Eilers-Walsman BL, Lipp R. New Ballard Score, expanded to include extremely premature infants. J Pediatr. 1991;119:417–23.
Battaglia FC, Lubchenco LO. A practical classification of newborn infants by weight and gestational age. J Pediatr. 1967;71:159–63.
Bancalari E, Jobe AH. Bronchopulmonary dysplasia. Am J Respir Crit Care Med. 2001;163:1723–9.
Papile LA, Burstein J, Burstein R, Koffler H. Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. J Pediatr. 1978;92:529–33.
Kliegman RM, Walsh MC. Necrotizing enterocolitis: pathogenesis, classification and spectrum of illness. Curr Probl Pediatr. 1987;17:213–88.
Committee for the Classification of Retinopathy of Prematurity. An international classification of retinopathy of prematurity. Arch Ophthalmol. 1984;102:1130–4.
Goel S, Mondkar J, Panchal H, Hegde D, Utture A, Manerkar S. Nasal mask versus nasal prongs for delivering nasal continuous positive airway pressure in preterm infants with respiratory distress: A randomized controlled trial. Indian Pediatr. 2015;52:1035–40.
Collins CL, Barfield C, Horne RS, Davis PG. A comparison of nasal trauma in preterm infants extubated to either heated humidified high-flow nasal cannulae or nasal continuous positive airway pressure. Eur J Pediatr. 2014;173:181–6.
Collins CL, Holberton JR, Barfield C, Davis PG. A randomized controlled trial to compare heated humidified high-flow nasal cannulae with nasal continuous positive airway pressure postextubation in premature infants. J Pediatr. 2013;162:949–54.
Graham III PL, Begg MD, Larson E, Della-Latta P, Allen A, Saiman L. Risk factors for late onset Gram-negative sepsis in low birth weight infants hospitalized in the neonatal intensive care unit. Pediatr Infect Dis J. 2006;25:113–7.
Shoemaker MT, Pierce MR, Yoder BA, DiGeronimo RJ. High flow nasal cannula versus nasal CPAP for neonatal respiratory disease: A retrospective study. J Perinatol. 2007;27:85–91.
Locke RG, Wolfson MR, Shaffer TH, Rubenstein SD, Greenspan JS. Inadvertent administration of positive enddistending pressure during nasal cannula flow. Pediatrics. 1993;91:135–8.
Sreenan C, Lemke RP, Hudson-Mason A, Osiovich H. High-flow nasal cannulae in management of apnea of prematurity: A comparison with conventional nasal continuous positive airway pressure. Pediatrics. 2001;107:1081–3.
Wilkinson DJ, Andersen CC, Smith K, Holberton J. Pharyngeal pressure with high-flow nasal cannulae in premature infants. J Perinatol. 2008;28:42–7.
Collins CL, Holberton JR, König K. Comparison of the pharyngeal pressure provided by two heated, humidified high flow nasal cannulae devices in premature infants. J Paediatr Child Health. 2013;49:554–6.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hegde, D., Mondkar, J., Panchal, H. et al. Heated humidified high flow nasal cannula versus nasal continuous positive airway pressure as primary mode of respiratory support for respiratory distress in preterm infants. Indian Pediatr 53, 129–133 (2016). https://doi.org/10.1007/s13312-016-0806-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13312-016-0806-3