Abstract
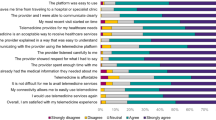
The COVID-19 pandemic has led to a change in healthcare models. The aim of this study was to evaluate patient acceptance of telehealth as an alternative to physical consultations, and to identify factors predicting higher satisfaction. This was an observational, cross-sectional, multi-center, international study. All consecutive patients for whom telehealth was used in consultations between April and July 2020 were considered for inclusion. The validated Telehealth Usability Questionnaire (TUQ) was used as a model to measure patient acceptance. Overall, 747 patients were observed, of whom 721 agreed to participate (96·5%). The TUQ showed that 86·9% of patients agreed that telehealth was useful; 85·2% supported the interface quality and 81·4% endorsed the interaction quality. Patients aged > 60 y were less likely to agree with the use of telehealth (p < 0·05). A web-based prediction tool was generated to calculate global satisfaction and to identify patients more likely to feel comfortable with telehealth. Telehealth is feasible and allows consultations that are satisfactory for patients. Technological advancements could ease safe implementation of telehealth into everyday practice. Adequate patient selection can be useful to ensure that the ideal strategy is used for each individual during and after the pandemic.





Similar content being viewed by others
Data availability
The authors confirm that the data supporting the findings of this study are available within the article and its Supplementary material. Raw data that support the findings of this study are available from the corresponding author, upon reasonable request.
References
Guan WJ, Ni Z-Y, Hu Y et al (2020) Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med 382:1708–1720. https://doi.org/10.1016/j.jemermed.2020.04.004
Singh AP, Berman AT, Marmarelis ME et al (2020) Management of lung cancer during the COVID-19 pandemic. JCO Oncol Pract 16(9):579–586. https://doi.org/10.1200/OP.20.00286
Smith AC, Thomas E, Snoswell CL et al (2020) Telehealth for global emergencies: implications for coronavirus disease 2019 (COVID-19). J Telemed Telecare 26(5):309–313. https://doi.org/10.1177/1357633X20916567
Chopra V, Toner E, Waldhorn R, Washer L (2020) How should U.S. hospitals prepare for Coronavirus disease 2019 (COVID-19)? Ann Intern Med 172(9):621–622. https://doi.org/10.7326/M20-0907
Buvik A, Bugge E, Knutsen G, Småbrekke A, Wilsgaard T (2019) Patient reported outcomes with remote orthopaedic consultations by telemedicine: a randomised controlled trial. J Telemed Telecare 25(8):451–459. https://doi.org/10.1177/1357633X18783921
Bator EX, Gleason JM, Lorenzo AJ et al (2015) The burden of attending a pediatric surgical clinic and family preferences toward telemedicine. J Pediatr Surg 50(10):1776–1782. https://doi.org/10.1016/j.jpedsurg.2015.06.005
Cremades M, Ferret G, Parés D et al (2020) Telemedicine to follow patients in a general surgery department. A randomized controlled trial. Am J Surg 219(6):882–887. https://doi.org/10.1016/j.amjsurg.2020.03.023
von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP (2014) The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. Int J Surg 12(12):1495–1499. https://doi.org/10.1016/j.ijsu.2014.07.013
Parmanto B, Lewis AN, Graham KM, Bertolet MH (2016) Development of the telehealth usability questionnaire (TUQ). Int J Telerehabil 8(1):3–10. https://doi.org/10.5195/ijt.2016.6196
Torre AC, Bibiloni N, Sommer J et al (2020) Spanish translation and transcultural adaptation of a questionnaire on telemedicine usability. Medicina (B. Aires). 80(2):134–137
Harrell FE (2018) Regression Modeling Strategies. 14:330 (Bios, 2018)
Jogoo P, Golamgous IS, Chuttur Y (2019) From desktop to mobile view: a simplified approach to mobile website development. In: 2019 Conference on Next Generation Computing Applications (NextComp). IEEE
Mora CG. TelemedicineRiskCalculator. https://github.com/cgmora12/TelemedicineRiskCalculator
Park B, Bashshur R (1975) Some implications of telemedicine. J Commun 25(3):161–166. https://doi.org/10.1111/j.1460-2466.1975.tb00619.x
Ekeland AG, Bowes A, Flottorp S (2010) Effectiveness of telemedicine: a systematic review of reviews. Int J Med Inform 79(11):736–771. https://doi.org/10.1016/j.ijmedinf.2010.08.006
World Health Organization. https://iris.wpro.who.int. Accessed 6 2021
Serper M, Nunes F, Ahmad N, Roberts D, Metz DC, Mehta SJ (2020) Positive early patient and clinician experience with telemedicine in an academic gastroenterology practice during the COVID-19 pandemic. Gastroenterology 159(4):1589-1591.e4. https://doi.org/10.1053/j.gastro.2020.06.034
Park H-Y, Kwon Y-M, Jun H-R, Jung S-E, Kwon S-Y (2021) Satisfaction survey of patients and medical staff for telephone-based telemedicine during hospital closing due to COVID-19 transmission. Telemed J E Health 27(7):724–732. https://doi.org/10.1089/tmj.2020.0369
Abelson JS, Symer M, Peters A, Charlson M, Yeo H (2017) Mobile health apps and recovery after surgery: what are patients willing to do? Am J Surg 214(4):616–622. https://doi.org/10.1016/j.amjsurg.2017.06.009
Ioannidis A, Blanco-Colino R, Chand M, Pellino G, Nepogodiev D, Wexner SD, Mayol J (2020) How to make an impact in surgical research: a consensus summary from the #SoMe4Surgery community. Updates Surg 72(4):1229–1235. https://doi.org/10.1007/s13304-020-00780-z
Data. GSMA Intelligence. https://www.gsmaintelligence.com/data/
Hales W (2012) Html5 and JavaScript web apps: Bridging the gap between the web and the mobile web. O’Reilly Media
Kong SS, Otalora Rojas LA, Ashour A, Robinson M, Hosterman T, Bhanusali N (2021) Ability and willingness to utilize telemedicine among rheumatology patients-a cross-sectional survey. Clin Rheumatol 40(12):5087–5093. https://doi.org/10.1007/s10067-021-05759-8
Gallegos-Rejas VM, Thomas EE, Kelly JT, Smith AC (2022) A multi-stakeholder approach is needed to reduce the digital divide and encourage equitable access to telehealth. J Telemed Telecare 29(1):73–78. https://doi.org/10.1177/1357633X221107995
Taylor ML, Thomas EE, Vitangcol K et al (2022) Digital health experiences reported in chronic disease management: an umbrella review of qualitative studies. J Telemed Telecare 28(10):705–717. https://doi.org/10.1177/1357633X221119620
Acknowledgements
iHealthStudy Collaborators (all listed in Pubmed): Ana Belén Gallardo-Herrera, Hospital Universitario de Torrejón (Madrid), Laura Colao-García, Hospital Universitario de Torrejón (Madrid), Carlota García-Fernández, Hospital San Pedro (Logroño), Sara Subirats-Bort, Hospital San Pedro (Logroño), Aitor Landaluce-Olavarria, Hospital Urduliz (Bizcaia), Begoña Estraviz-Mateos, Hospital Urduliz (Bizcaia), Jorge Martínez-Iñiguez Blasco, Hospital San Pedro (Logroño), Cristina Tejedor-Carreño, Hospital San Pedro (Logroño), Teresa Calderón-Duque, Hospital Nuestra Señora del Prado (Toledo), Lourdes Gómez-Ruiz, Hospital Nuestra Señora del Prado (Toledo), Juan José Segura-Sampedro, Hospital Universitario Son Espases (Palma de Mallorca), Andrea Craus-Migue, l Hospital Universitario Son Espases (Palma de Mallorca), Ana María García-Cabrera, Hospital Universitario Virgen del Rocío (Sevilla), María Luisa Reyes-Díaz, Hospital Universitario Virgen del Rocío (Sevilla), Irene Ramallo, Hospital Universitario Virgen del Rocío (Sevilla), Patricia Tejedor, Hospital Universitario Central de la Defensa Gómez Ulla (Madrid), Luis de Nicolas Navas, Hospital Universitario Central de la Defensa Gómez Ulla (Madrid), Elena Viejo-Martínez, Hospital Universitario Infanta Leonor (Madrid), Alicia Ruiz de la Hermosa García Pardo, Hospital Universitario Infanta Leonor (Madrid), Rebeca Saeta Campo, Hospital de la Marina Baixa (Alicante), Ana Apio-Cepeda, Hospital de la Marina Baixa (Alicante), Carlos Cerdán-Santacruz, Hospital Universitario de la Princesa (Madrid), Lara Blanco-Terés, Hospital Universitario de la Princesa (Madrid), David Moro-Valdezate, Hospital Clínico Universitario de Valencia (Valencia), Ernesto Muñoz-Sornosa, Hospital Clínico Universitario de Valencia (Valencia), Sara Roldán-Baños, Hospital de Zafra (Badajoz), Ernesto Jesús Barzola-Navarro, Hospital de Zafra (Badajoz), Ismael Antón-Fernández, Hospital Insular Las Palmas de Gran Canaria (Las Palmas), Antonio Navarro-Sánchez, Hospital Insular Las Palmas de Gran Canaria (Las Palmas), Rega Daniela, IRCSS—Fondazione G. Pascale (Italy), Delrio Paolo, IRCSS—Fondazione G. Pascale (Italy), Hosam Hamed, Truelife Digestive and Bariatric Center (Egypt), Mohamed Said, Truelife Digestive and Bariatric Center (Egypt), Andrea Belli, INT Pascale IRCCS Napoli (Italy), Renato Patrone, INT Pascale IRCCS Napoli (Italy), Arcangelo Picciariello, Policlinico of Bari (Italy), Donato F. Altomare, Policlinico of Bari (Italy), Sohail Bakkar, The Hashemite University (Jordan), Luca Pio, Hospital Robert-Debré (France), Liza Ali, Hospital Robert-Debré (France), Pierfrancesco Lapolla, Policlinico Umberto I—Sapienza University of Rome, Andrea Mingoli, Policlinico Umberto I—Sapienza University of Rome, Ljiljana Milic, University Clinacal Center “Zvezdara” (Serbia), Dragana Arbutina, University Clinacal Center “Zvezdara” (Serbia), Víctor Turrado-Rodríguez, Hospital Clínic de Barcelona
Author information
Authors and Affiliations
Consortia
Contributions
Conceptualization, LS-G and CL-G; formal analysis, LS-G, CL-G, and XB; investigation, LS-G and CL-G; methodology, LS-G, CL-G, and XB; writing—original draft preparation, LS-G and CL-G; writing—review and editing, LS-G, CL-G, CG-M, MA-G, AI, SC, AF, RS, JM, and GP; all authors have read and agreed to the published version of the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
This study does not have external funding. All the researchers participating in the study do it altruistically without receiving financial retribution. The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sánchez-Guillén, L., Lillo-García, C., Barber, X. et al. Patients’ perception of using telehealth for consultation: insights after pandemic and development of an online calculator platform to predict acceptance of remote consultation: the TELEMED international study. Updates Surg (2024). https://doi.org/10.1007/s13304-024-01780-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s13304-024-01780-z