Abstract
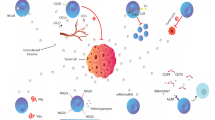
Cancers constitutively produce and secrete into the blood and other biofluids 30–150 nm-sized endosomal vehicles called exosomes. Cancer-derived exosomes exhibit powerful influence on a variety of biological mechanisms to the benefit of the tumors that produce them. We studied the immunosuppressive ability of epithelial ovarian cancer (EOC) exosomes on two cytotoxic pathways of importance for anticancer immunity—the NKG2D receptor-ligand pathway and the DNAM-1-PVR/nectin-2 pathway. Using exosomes, isolated from EOC tumor explant and EOC cell-line culture supernatants, and ascitic fluid from EOC patients, we studied the expression of NKG2D and DNAM-1 ligands on EOC exosomes and their ability to downregulate the cognate receptors. Our results show that EOC exosomes differentially and constitutively express NKG2D ligands from both MICA/B and ULBP families on their surface, while DNAM-1 ligands are more seldom expressed and not associated with the exosomal membrane surface. Consequently, the NKG2D ligand-bearing EOC exosomes significantly downregulated the NKG2D receptor expression on peripheral blood mononuclear cells (PBMC) while the DNAM-1 receptor was unaffected. The downregulation of NKG2D receptor expression was coupled to inhibition of NKG2D receptor-ligand-mediated degranulation and cytotoxicity measured in vitro with OVCAR-3 and K562 cells as targets. The EOC exosomes acted as a decoy impairing the NKG2D mediated cytotoxicity while the DNAM-1 receptor-ligand system remained unchanged. Taken together, our results support and explain the mechanism behind the recently reported finding that in EOC, NK-cell recognition and killing of tumor cells was mainly dependent on DNAM-1 signaling while the contribution of the NKG2D receptor-ligand pathway was complementary and uncertain.





Similar content being viewed by others
References
Campbell KS, Hasegawa J. Natural killer cell biology: an update and future direction. J Allergy Clin Immunol. 2013;132:536–44.
Lanier LL. NK cell recognition. Annu Rev Immunol. 2005;23:225–74.
Smyth MJ, Swann J, Cretney E, Zerafa N, Yokoyama WM, Hayakawa Y. NKG2D function protects the host from tumor initiation. J Exp Med. 2005;202:583–8.
Guerra N, Tan YX, Jincker NT, Choy A, Gallardo F, Xiong N, et al. NKG2D-deficient mice are defective in tumor surveillance in models of spontaneous malignancy. Immunity. 2008;28:571–80.
El-Sherbiny YM, Meade JL, Holmes TD, McConagle D, Mackie SL, Morgan AW, et al. The requirement for DNAM-1, NKG2D and NKp46 in the natural killer cell-mediated killing of myeloma cells. Cancer Res. 2007;67:8444–9.
Raulet DH. Roles of the NKG2D immunoreceptor and its ligands. Nat Rev Immunol. 2003;3:781–90.
Hildreth JE, Gotch FM, Hildreth PD, McMichael AJ. A human lymphocyte associated antigen involved in cell-mediated lympholysis. Eur J Immunol. 1983;13:202–8.
Gahmberg CG. Leukocyte adhesion: CD11/CD18 integrins and intercellular adhesion molecules. Curr Opin Cell Biol. 1997;9:643–50.
Fuchs A, Colonna M. The role of NK cell recognition of nectin and nectin-like proteins in tumor surveillance. Semin Cancer Biol. 2006;16:359–66.
Carlsten M, Björkström N, Norell H, Bryceson Y, van Hall T, Baumann B, et al. DNAX accessory molecule-1 mediated recognition of freshly isolated ovarian carcinoma by resting natural killer cells. Cancer Res. 2007;67:1317–25.
Gubbels JA, Claussen N, Kapur AK, Connor JP, Patankar MS. The detection, treatment, and biology of epithelial ovarian cancer. J Ovarian Res. 2010;3:8.
Yigit R, Massuger LF, Figdor CG, Torensma R. Ovarian cancer creates a suppressive microenvironment to escape immune elimination. Gynecol Oncol. 2010;117:366–72.
Holschneider CH, Berek JS. Ovarian cancer: epidemiology, biology, and prognostic factors. Semin Surg Oncol. 2000;19(1):3–10.
Mincheva-Nilsson L, Baranov V. Cancer exosomes and NKG2D receptor-ligand interactions: impairing NKG2D-mediated cytotoxicity and anti-tumor immune surveillance. Semin Cancer Biol. 2014;28:24–30.
Bustin SA, Benes V, Garson JA, Hellemans J, Huggett J, Kubista M, et al. The MIQE guidelines: minimum information for publication of quantitative real-time PCR experiments. Clin Chem. 2009;55:611–22.
Stenqvist AC, Nagaeva O, Baranov V, Mincheva-Nilsson L. Exosomes secreted by human placenta carry functional Fas ligand and TRAIL molecules and convey apoptosis in activated immune cells, suggesting exosome-mediated immune privilege of the fetus. J Immunol. 2013;191:5515–23.
Mincheva-Nilsson L, Nagaeva O, Chen T, Stendahl U, Antsiferova J, Mogren I, et al. Placenta-derived soluble MHC class I chain-related molecules down-regulate NKG2D receptor on peripheral blood mononuclear cells during human pregnancy: a possible novel immune escape mechanism for fetal survival. J Immunol. 2006;176:3585–92.
Hedlund M, Stenqvist AC, Nagaeva O, Kjellberg L, Wulff M, Baranov V, et al. Human placenta expresses and secretes NKG2D ligands via exosomes that down-modulate the cognate receptor expression: evidence for immunosuppressive function. J Immunol. 2009;183:340–51.
Greening DW, Xu R, Ji H, Tauro BJ, Simpson RJ. A protocol for exosome isolation and characterization: evaluation of ultracentrifugation, density-gradient separation and immunoaffinity capture methods. In Proteomic profiling: Methods and Protocols. Anton Posh (ed). Methods in molecular Biology, vol. 1295, DOI 10.1007/978-1-4939-2550-6_15, 2015.
Kiessling R, Klein E, Wigzell H. Natural killer cells in the mouse.I. Cytotoxic cells with specificity for mouse Moloney leukemia cells. Specificity and distribution according to genotype. Eur J Immunol. 1975;5:112–7.
Costello RT, Fauriat C, Sivori S, Marcenaro E, Olive D. NK cells: innate immunity against hematological malignancies. Trends Immunol. 2004;25:328–33.
Lanier LL. A renaissance for the tumor immunosurveillance hypothesis. Nat Med. 2001;7:1178–80.
Kaplan-Lefko PJ, Chen TM, Ittmann MM, Barrios RJ, Ayala GE, Huss WJ, et al. Pathobiology of autochthonous prostate cancer in a pre-clinical transgenic mouse model. Prostate. 2003;55:219–37.
Groh V, Reinhard R, Secrist H, Grabstein KH, Spies T. Broad tumor-associated expression and recognition by tumor-derived gamma-delta T cells of MICA and MICB. Proc Natl Acad Sci U S A. 1999;96:6879–84.
Clayton A, Mitchell JP, Court J, Linnane S, Mason MD, Tabi Z. Human tumor-derived exosomes downmodulate NKG2D expression. J Immunol. 2008;180:7249–58.
Lundholm L, Schroder M, Nagaeva O, Baranov V, Widmark A, Mincheva-Nilsson L, et al. Prostate tumor-derived exosomes down-regulate NKG2D expression on natural killer cells and CD8+ T cells: mechanism of immune evasion. PLoS ONE. 2014;9:e108925.
Clayton A, Mason MD. Exosomes in tumor immunity. Curr Oncol. 2009;16:46–9.
Hedlund M, Nagaeva O, Kargl D, Baranov V, Mincheva-Nilsson L. Thermal- and oxidative stress causes enhanced release of NKG2D ligand-bearing immunosuppressive exosomes in leukemia/lymphoma T and B cells. PLoS One. 2011;6:e16899.
Mizuki N, Ota M, Kimura M, Ohno S, Ando H, Katsuyama Y, et al. Triplet repeat polymorphism in the transmembrane region of MICA gene: a strong association of six CGT repetitions with Becet disease. Proc Natl Acad Sci U S A. 1997;94:1298–303.
Ashiru O, Boutet P, Fernandez-Messina L, Agüera-González S, Skepper J, Valés-Gómez M, et al. Natural killer cell cytotoxicity is suppressed by exposure to the human NKG2D ligand MICA*0008 that is shed by tumor cells in exosomes. Cancer Res. 2010;70:481–9.
Ghaderi M, Hjelmstrom, Hallmans G, Wiklund F, Lenner P, Dillner J, et al. MICA gene polymorphism and the risk to develop cervical epithelial neoplasia. Hum Immunol. 1999;60:970–3.
Filipazzi P, Bürdek M, Villa A, Rivoltini L, Huber V. Recent advances on the role of tumor exosomes in immunosuppression and disease progression. Semin Cancer Biol. 2012;22:342–9.
Acknowledgments
Patients and colleagues from the Dept. of Obstetrics and Gynecology at Norrland’s University Hospital are gratefully acknowledged. This work was supported by Swedish National Cancer Research Foundation (Cancerfonden, 2013/439), Swedish National Research Foundation (Vetenskapsrådet, K2013-54X-22341-01-05), Central ALF fund VLL, and Insamlingsstiftelsen, Umeå University.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Rights and permissions
About this article
Cite this article
Labani-Motlagh, A., Israelsson, P., Ottander, U. et al. Differential expression of ligands for NKG2D and DNAM-1 receptors by epithelial ovarian cancer-derived exosomes and its influence on NK cell cytotoxicity. Tumor Biol. 37, 5455–5466 (2016). https://doi.org/10.1007/s13277-015-4313-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-015-4313-2