Abstract
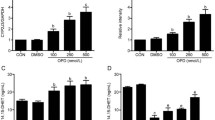
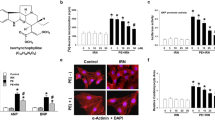
Salicylates, one of the oldest medicinal compounds known to humans, have been reported to show anti-inflammatory effects via cyclooxygenase (COX) inhibition. However, the pathophysiological role of COX-2 in the heart is conflicting, and the role of sodium salicylate in the regulation of cardiac inflammation has not yet been elucidated. We aimed to investigate the effect of salicylate on COX-2 expression and its associated prostaglandin production using cultured neonatal rat cardiomyocytes. The cells were incubated in the presence or absence of sodium salicylate (8 mM). Treatment with sodium salicylate significantly increased COX-2 expression at both mRNA and protein levels, induced prostaglandin D2 release, and increased TNF-α mRNA expression in cardiomyocytes. In addition, salicylate treatment induced cardiomyocyte hypertrophy. Taken together, we demonstrated that salicylate induced COX-2 expression, which in turn resulted in the regulation of expression of several inflammatory mediators in cardiomyocytes.
Similar content being viewed by others

References
Rumore, M. M. & Kim, K. S. Potential role of salicylates in type 2 diabetes. Ann Pharmacother 44: 1207–1221 (2010).
Yin, M. J., Yamamoto, Y. & Gaynor, R. B. The anti-inflammatory agents aspirin and salicylate inhibit the activity of I(kappa)B kinase-beta. Nature 396: 77–80 (1998).
Hennekens, C. H. & Dalen, J. E. Aspirin in the treatment and prevention of cardiovascular disease: past and current perspectives and future directions. Am J Med 126: 373–378 (2013).
Goldfine, A. B. et al. A randomised trial of salsalate for insulin resistance and cardiovascular risk factors in persons with abnormal glucose tolerance. Diabetologia 56: 714–723 (2013).
Pierce, G. L., Lesniewski, L. A., Lawson, B. R., Beske, S. D. & Seals, D. R. Nuclear factor-{kappa}B activation contributes to vascular endothelial dysfunction via oxidative stress in overweight/obese middle-aged and older humans. Circulation 119: 1284–1292 (2009).
Russo-Marie, F., Paing, M. & Duval, D. Mechanism of glucocorticoid-induced inhibition of prostaglandin synthesis. Agents Actions Suppl:49–62 (1979).
Steinberg, G. R., Dandapani, M. & Hardie, D. G. AMPK: mediating the metabolic effects of salicylate-based drugs? Trends Endocrinol Metab 24: 481–487 (2013).
Preston, S. J., Arnold, M. H., Beller, E. M., Brooks, P. M. & Buchanan, W. W. Comparative analgesic and anti-inflammatory properties of sodium salicylate and acetylsalicylic acid (aspirin) in rheumatoid arthritis. Br J Clin Pharmacol 27: 607–611 (1989).
Beynen, A. C., Buechler, K. F., van der Molen, A. J. & Geelen, M. J. Inhibition of hepatic lipogenesis by salicylate. Toxicology 24: 33–43 (1982).
Meex, R. C., Phielix, E., Moonen-Kornips, E., Schrauwen, P. & Hesselink, M. K. Stimulation of human whole-body energy expenditure by salsalate is fueled by higher lipid oxidation under fasting conditions and by higher oxidative glucose disposal under insulin-stimulated conditions. J Clin Endocrinol Metab 96: 1415–1423 (2011).
Tokudome, S. et al. Glucocorticoid protects rodent hearts from ischemia/reperfusion injury by activating lipocalin-type prostaglandin D synthase-derived PGD2 biosynthesis. J Clin Invest 119: 1477–1488 (2009).
Streicher, J. M., Kamei, K., Ishikawa, T. O., Herschman, H. & Wang, Y. Compensatory hypertrophy induced by ventricular cardiomyocyte-specific COX-2 expression in mice. J Mol Cell Cardiol 49: 88–94 (2010).
Chenevard, R. et al. Selective COX-2 inhibition improves endothelial function in coronary artery disease. Circulation 107: 405–409 (2003).
Mukherjee, D., Nissen, S. E. & Topol, E. J. Risk of cardiovascular events associated with selective COX-2 inhibitors. JAMA 286: 954–959 (2001).
Bolli, R. et al. Discovery of a new function of cyclooxygenase (COX)-2: COX-2 is a cardioprotective protein that alleviates ischemia/reperfusion injury and mediates the late phase of preconditioning. Cardiovasc Res 55: 506–519 (2002).
Inserte, J. et al. Constitutive COX-2 activity in cardiomyocytes confers permanent cardioprotection Constitutive COX-2 expression and cardioprotection. J Mol Cell Cardiol 46: 160–168 (2009).
Shinmura, K. et al. Cyclooxygenase-2 mediates the cardioprotective effects of the late phase of ischemic preconditioning in conscious rabbits. Proc Natl Acad Sci U S A 97: 10197–10202 (2000).
Tsatsanis, C., Androulidaki, A., Venihaki, M. & Margioris, A. N. Signalling networks regulating cyclooxygenase-2. Int J Biochem Cell Biol 38: 1654–1661 (2006).
Eguchi, Y. et al. Expression of lipocalin-type prostaglandin D synthase (beta-trace) in human heart and its accumulation in the coronary circulation of angina patients. Proc Natl Acad Sci U S A 94: 14689–14694 (1997).
Katsumata, Y. et al. Endogenous prostaglandin D2 and its metabolites protect the heart against ischemia-reperfusion injury by activating Nrf2. Hypertension 63: 80–87 (2014).
Xiao, C. Y. et al. Prostaglandin E2 protects the heart from ischemia-reperfusion injury via its receptor subtype EP4. Circulation 109: 2462–2468 (2004).
Mitchell, J. A., Saunders, M., Barnes, P. J., Newton, R. & Belvisi, M. G. Sodium salicylate inhibits cyclo-oxygenase-2 activity independently of transcription factor (nuclear factor kappaB) activation: role of arachidonic acid. Mol Pharmacol 51: 907–912 (1997).
Xu, X. M. et al. Suppression of inducible cyclooxygenase 2 gene transcription by aspirin and sodium salicylate. Proc Natl Acad Sci U S A 96: 5292–5297 (1999).
Chae, H. J., Chae, S. W., Reed, J. C. & Kim, H. R. Salicylate regulates COX-2 expression through ERK and subsequent NF-kappaB activation in osteoblasts. Immunopharmacol Immunotoxicol 26: 75–91 (2004).
Kwon, K. S. & Chae, H. J. Sodium salicylate inhibits expression of COX-2 through suppression of ERK and subsequent NF-kappaB activation in rat ventricular cardiomyocytes. Arch Pharm Res 26: 545–553 (2003).
Levine, B., Kalman, J., Mayer, L., Fillit, H. M. & Packer, M. Elevated circulating levels of tumor necrosis factor in severe chronic heart failure. N Engl J Med 323: 236–241 (1990).
Meldrum, D. R. Tumor necrosis factor in the heart. Am J Physiol 274:R577–595 (1998).
Yokoyama, T. et al. Tumor necrosis factor-alpha provokes a hypertrophic growth response in adult cardiac myocytes. Circulation 95: 1247–1252 (1997).
Mann, D. L. et al. Targeted anticytokine therapy in patients with chronic heart failure: results of the Randomized Etanercept Worldwide Evaluation (RENEWAL). Circulation 109: 1594–1602 (2004).
Lecour, S. et al. Identification of a novel role for sphingolipid signaling in TNF alpha and ischemic preconditioning mediated cardioprotection. J Mol Cell Cardiol 34: 509–518 (2002).
Tanno, M. et al. Tumor necrosis factor-induced protection of the murine heart is independent of p38-MAPK activation. J Mol Cell Cardiol 35: 1523–1527 (2003).
Kurrelmeyer, K. M. et al. Endogenous tumor necrosis factor protects the adult cardiac myocyte against ischemic-induced apoptosis in a murine model of acute myocardial infarction. Proc Natl Acad Sci U S A 97: 5456–5461 (2000).
Ichikawa, Y. et al. The role of ADAM protease in the tyrosine kinase-mediated trigger mechanism of ischemic preconditioning. Cardiovasc Res 62: 167–175 (2004).
Sack, M. Tumor necrosis factor-alpha in cardiovascular biology and the potential role for anti-tumor necrosis factor-alpha therapy in heart disease. Pharmacol Ther 94: 123–135 (2002).
Shimizu, I. & Minamino, T. Physiological and pathological cardiac hypertrophy. J Mol Cell Cardiol 97: 245–262 (2016).
Wang, D. et al. Cardiomyocyte cyclooxygenase-2 influences cardiac rhythm and function. Proc Natl Acad Sci U S A 106: 7548–7552 (2009).
Ock, S. et al. Receptor activator of nuclear factor-kappaB ligand is a novel inducer of myocardial inflammation. Cardiovasc Res 94: 105–114 (2012).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ock, S., Kim, H.M., Lee, W.S. et al. Effect of sodium salicylate on COX-2 expression in neonatal rat cardiomyocytes. Mol. Cell. Toxicol. 14, 87–92 (2018). https://doi.org/10.1007/s13273-018-0011-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13273-018-0011-7