Abstract
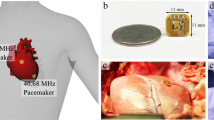
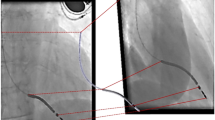
Implantation and maintenance of a permanent cardiac pacing system in children remains challenging due to small patient size, congenital heart defects and somatic growth. We are developing a novel epicardial micropacemaker for children that can be implanted on the epicardium within the pericardial space via a minimally-invasive technique. The key design configurations include a novel open-coiled lead in which living tissue replaces the usual polymeric support for the coiled conductor. To better understand and be able to predict the behavior of the implanted lead, we performed a radiographic image-based modeling study on a chronic animal test. We report a pilot study in which two mechanical dummy pacemakers with epicardial leads were implanted into an adult pig model via a minimally invasive approach. Fluoroscopy was obtained on the animal on Post-Operative Days #9, #35 and #56 (necropsy). We then constructed an analytic model to estimate the in vivo stress conditions on the open-coil lead based on the analysis of orthogonal biplane radiographic images. We obtained geometric deformation data of the implanted lead including elongation magnitudes and bending radii from sequenced films of cardiac motion cycles. The lead stress distribution was investigated on each film frame and the point of maximum stress (Mean Stress = 531.4 MPa; Alternating Stress = ± 216.4 MPa) was consistently where one of the leads exited the pericardial space, a deployment that we expected to be unfavorable. These results suggest the modeling approach can provide a basis for further design optimization. More animal tests and modeling will be needed to validate whether the novel lead design could meet the requirements to withstand ~200 million cardiac motion cycles over 5 years.








Similar content being viewed by others
References
Altman, P. A., J. M. Meagher, D. W. Walsh, and D. A. Hoffmann. Rotary bending fatigue of coils and wires used in cardiac lead design. J. Biomed. Mater. Res. 43(1):21–37, 1998.
Bhonsle, S., and C. Van Karsen. Mechanical and fatigue properties of stress relieved type 302 stainless steel wire. J. Mater. Eng. Perform. 1(3):363–369, 1992.
de Voogt, W. G. Pacemaker leads: performance and progress. Am. J. Cardiol. 83(5):187–191, 1999.
Durelli, A., V. Parks, and H. Hasseem. Helices under load. J. Manuf. Sci. Eng. 97(3):853–858, 1975.
Fortescue, E. B., C. I. Berul, F. Cecchin, E. P. Walsh, J. K. Triedman, and M. E. Alexander. Patient, procedural, and hardware factors associated with pacemaker lead failures in pediatrics and congenital heart disease. Heart Rhythm. 1(2):150–159, 2004.
Furman, S., D. L. Hayes, and D. R. Holmes. A Practice of Cardiac Pacing. Oxford: Wiley-Blackwell, 1989.
Juvinall, R. C., and K. M. Marshek. Fundamentals of Machine Component Design. New York: Wiley, 2006.
Kistler, P. M., G. Liew, and H. G. Mond. Long-term performance of active-fixation pacing leads: a prospective study. Pacing Clin. Electrophysiol. 29(3):226–230, 2006.
Loeb, G. E., L. Zhou, K. Zheng, A. Nicholson, R. A. Peck, A. Krishnan, et al. Design and testing of a percutaneously implantable fetal pacemaker. Ann. Biomed. Eng. 41(1):17–27, 2013.
Malvern, L. E. Introduction to the Mechanics of a Continuous Medium. Englewood Cliffs: Prentice-Hall, 1969.
Meagher, J. M., and P. Altman. Stresses from flexure in composite helical implantable leads. Med. Eng. Phys. 19(7):668–673, 1997.
Phillips, R., M. Frey, and R. O. Martin. Long-term performance of polyurethane pacing leads: mechanisms of design-related failures. Pacing Clin. Electrophysiol. 9(6):1166–1172, 1986.
Podnos, E., E. Becker, J. Klawitter, and P. Strzepa. FEA analysis of silicone MCP implant. J. Biomech. 39(7):1217–1226, 2006.
Silka, M. J., and Y. Bar-Cohen. Pacemakers and implantable cardioverter-defibrillators in pediatric patients. Heart Rhythm. 3(11):1360–1366, 2006.
Silver, F., Y. Kato, M. Ohno, and A. Wasserman. Analysis of mammalian connective tissue: relationship between hierarchical structures and mechanical properties. J Long Term Effects Med. Implants 2(2–3):165–198, 1991.
Wahl, A. M. Mechanical Springs. Cleveland: Penton Publishing Company, 1944.
Acknowledgement
This research was funded by a NIH R01 Grant (1R01HD075135). Some aspects of the mechanical design and fabrication are the subjects of patents as well as pending patent applications assigned to Children’s Hospital Los Angeles and University of Southern California. No commercial partnerships have yet been arranged.
Conflict of interest
Author Li Zhou, Yaniv Bar-Cohen, Raymond A. Peck, Giorgio V. Chirikian, Brett Harwin, Ramen H. Chmait, Jay D. Pruetz, Michael J. Silka, Gerald E. Loeb declare that they have no conflict of interest.
Human and Animal Ethics
No human studies were carried out by the authors for this article. All institutional and national guidelines for the care and use of laboratory animals were followed and approved by the appropriate institutional committees.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editors Timothy Kelley and Ajit P. Yoganathan oversaw the review of this article.
Rights and permissions
About this article
Cite this article
Zhou, L., Bar-Cohen, Y., Peck, R.A. et al. Analytical Modeling for Computing Lead Stress in a Novel Epicardial Micropacemaker. Cardiovasc Eng Tech 8, 96–105 (2017). https://doi.org/10.1007/s13239-017-0292-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13239-017-0292-3