Abstract
The objective of the present study was to develop a W/O/W nanoemulsion (NE) drug delivery system loaded with punicalagin (PGN) for oral delivery and evaluate its potential in antibacterial therapy. The W/O/W PGN-NE was prepared using a two-step process by combining ultrasonic with high-energy emulsification and subsequently characterized by its droplet size, zeta potential, and morphology. The PGN-NE was further evaluated for its pH, in vitro antibacterial activity, drug release property, and cytotoxicity. The results indicated the formation of spherical, nano-sized globules of PGN-NE had a mean particle size of 45.53 ± 2.2 nm, with a PDI value of 0.22 ± 0.028, zeta potential was −4.67 ± 0.88 mV, and pH value was 5.8. In vitro antibacterial activity studies showed a significantly higher antibacterial activity of PGN-NE in comparison to free PGN, suggesting that NE can effectively improve the antibacterial effect of natural pharmaceuticals. The drug release assay demonstrated that PGN was slowly released from the NE preparation and absorbed, helping to prolong the potency and improve the bioavailability of PGN. Cytotoxicity testing showed that PGN had reduced toxicity when encapsulated in NE. Thus, the developed NE formulation of PNG exhibited a greater potential for the slow-release effect delivery and in the treatment of microbial infections with favorable safety profile.
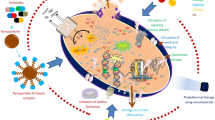
Graphical abstract
Micromorphology of W/O/W PGN nanoemulsion

The W/O/W PGN-NE are uniform in size and non-adhesive, with a size distribution of 28.214 to 141.772 nm and a mean size of 45.53 ± 2.2 nm, respectively, with a PDI value of 0.22 ± 0.028.








Similar content being viewed by others
References
P. Ilana et al., Making the hospital a safer place by sonochemical coating of all its textiles with antibacterial nanoparticles. Ultrason. Sonochem. 25, 82–88 (2015). https://doi.org/10.1016/j.ultsonch.2014.12.012
A. Anna et al., A sonochemical technology for coating of textiles with antibacterial nanoparticles and equipment for its implementation. Mater. Lett. 96, 121–124 (2013). https://doi.org/10.1016/j.matlet.2013.01.041
A. Mariscal et al., Antimicrobial effect of medical textiles containing bioactive fibres. Eur. J. Clin. Microbiol. Infect. Dis. 30, 227–232 (2011). https://doi.org/10.1007/s10096-010-1073-1
A. Haji, A. Shoushtari, Natural antibacterial finishing of wool fiber using plasma technology. Industria Textila 62(5), 244–247 (2011). https://doi.org/10.3993/tbis2011358
R. Zhang et al., Antibiotic resistance as a global threat: evidence from China, Kuwait and the United States. Globalization Health 2, 6–20 (2006). https://doi.org/10.1186/1744-8603-2-6
A.I. Dan, H. Diarmaid, Antibiotic resistance and its cost: is it possible to reverse resistance? Nat. Rev. Microbiol. 8, 260–271 (2010). https://doi.org/10.1038/nrmicro2319
C. Liu et al., Antibacterial and antibiotic synergistic activities of the extract from Pithecellobium clypearia against clinically important multidrug-resistant gram-negative bacteria. Eur. J. Integr. Med. 32, 100999 (2019). https://doi.org/10.1016/j.eujim.2019.100999
M.I. Ahmad et al., Pharkphoom Panichayupakaranant, Synergistic effect of α-mangostin on antibacterial activity of tetracycline, erythromycin, and clindamycin against acne involved bacteria. Chin. Herbal Med. 11(4), 412–416 (2019). https://doi.org/10.1016/j.chmed.2019.03.013
S.A. Zacchino et al., SortinoPlant phenolics and terpenoids as adjuvants of antibacterial and antifungal drugs. Phytomedicine 37, 27–48 (2017). https://doi.org/10.1016/j.phymed.2017.10.018
W. Qian et al., Antibacterial and antibiofilm activity of ursolic acid against carbapenem-resistant enterobacter cloacae. J. Biosci. Bioeng. 129(5), 528–534 (2020)
E.M. Abdelfattah et al., Antibacterial, antifungal and antioxidant activity of total polyphenols of Withania frutescens.L. Bioorganic Chem.. 93, 103337–103346 (2019). https://doi.org/10.1016/j.bioorg.2019.103337
A.Z. Susana et al., Plant phenolics and terpenoids as adjuvants of antibacterial and antifungal drugs. Phytomedicine 37, 27–48 (2017). https://doi.org/10.1016/j.phymed.2017.10.018
L.T. Lin et al., Broad-spectrum antiviral activity of chebulagic acid and punicalagin against viruses that use glycosaminoglycans for entry. BMC Microbiol. 13, 187 (2013). https://doi.org/10.1186/1471-2180-13-187
T. Sachin et al., Rapid, enhanced and eco-friendly recovery of punicalagin from fresh waste pomegranate peels via aqueous ball milling. J. Clean. Prod. 228, 1238–1247 (2019). https://doi.org/10.1016/j.jclepro.2019.04.392
M. Akansha et al., Nanoparticles of punicalagin synthesized from pomegranate (Punica granatum L.) with enhanced efficacy against human hepatic carcinoma cells. J. Clust. Sci. 33, 349–359 (2022). https://doi.org/10.1007/s10876-021-01979-9
M. Labieniec, T.G. Gabryelak, Effects of tannins on Chinese hamster cell line B14. Mutat. Res. 539, 127–135 (2003). https://doi.org/10.1016/S1383-5718(03)00161-X
A. Debora, C., et al., Study of antimicrobial activity and atomic force microscopy imaging of the action mechanism of cashew tree gum. Carbohydr. Polym. 90(1), 270–274 (2012). https://doi.org/10.1016/j.carbpol.2012.05.034
A. Mariana et al., Pomegranate and grape by-products and their active compounds: are they a valuable source for food applications? Trends Food Sci. Technol. 86, 68–84 (2019). https://doi.org/10.1016/j.tifs.2019.02.010
A.A. Fouad et al., Punicalagin alleviates hepatotoxicity in rats challenged with cyclophosphamide. Environ. Toxicol. Pharmacol. 45, 158–162 (2016). https://doi.org/10.1016/j.etap.2016.05.031
F. Mo et al., Protective mechanism of punicalagin against endoplasmic reticulum stress in the liver of mice with type 2 diabetes mellitus. J. Funct. Foods. 56, 57–64 (2019). https://doi.org/10.1016/j.jff.2019.03.006
G. Beatriz et al., Assessment of polyphenolic profile and antibacterial activity of pomegranate peel (Punica granatum) flour obtained from co-product of juice extraction. Food Control 59, 94–98 (2016). https://doi.org/10.1016/j.foodcont.2015.05.025
S.H. Mun et al., Punicalagin suppresses methicillin resistance of Staphylococcus aureus to oxacillin. J. Pharmacol. Sci. 137, 317–323 (2018). https://doi.org/10.1016/j.jphs.2017.10.008
A.D. Smith et al., Pomegranate peel extract reduced colonic damage and bacterial translocation in a mouse model of infectious colitis induced by Citrobacter rodentium. Nutr. Res. 73, 27–37 (2020). https://doi.org/10.1016/j.nutres.2019.11.001
N. Badawi et al., Pomegranate extract-loaded solid lipid nanoparticles: design, optimization, and in vitro cytotoxicity study. Int. J. Nanomed. 13, 1313–1326 (2018). https://doi.org/10.2147/IJN.S154033
V. Sanna et al., Nanoformulation of natural products for prevention and therapy of prostate cancer. Cancer Lett. 334(1), 142–151 (2013). https://doi.org/10.1016/j.canlet.2012.11.037
A.B. Shirode et al., Nanoencapsulation of pomegranate bioactive compounds for breast cancer chemoprevention. Int. J. Nanomed. 10, 475–484 (2015). https://doi.org/10.2147/IJN.S65145
L. Yang et al., Bio-inspired dual-adhesive particles from microfluidic electrospray for bone regeneration. Nano Res. 16, 5292–5299 (2023). https://doi.org/10.1007/s12274-022-5202-9
L. Lanjie et al., Angiogenic microspheres for the treatment of a thin endometrium. ACS Biomater. Sci. Eng. 7, 4914–4920 (2021). https://doi.org/10.1021/acsbiomaterials.1c00615
Z. Lin et al., Antimicrobial curcumin nanoparticles downregulate joint inflammation and improve osteoarthritis. Macromol. Res. (2023). https://doi.org/10.1007/s13233-023-00196-9
W. Huan et al., Biomimetic enzyme cascade reaction system in microfluidic electrospray microcapsules. Sci. Adv. 4, 2816–2823 (2018). https://doi.org/10.1126/sciadv.aat2816
M.G.D. Silva et al., Nanoemulsion composed of 10-(4,5-dihydrothiazol-2-yl)thio)decan-1-ol), a synthetic analog of 3-alkylpiridine marine alkaloid: development, characterization, and antimalarial activity. Eur. J. Pharm. Sci. 151, 105382–105391 (2020). https://doi.org/10.1016/j.ejps.2020.105382
R.A. Schuenck-Rodrigues et al., Development, characterization and photobiological activity of nanoemulsion containing zinc phthalocyanine for oral infections treatment. J. Photochem. Photobiol. B. 211, 112010–112021 (2020). https://doi.org/10.1016/j.jphotobiol.2020.112010
B.M. Altaani et al., Oral delivery of teriparatide using a nanoemulsion system: design, in vitro and in vivo evaluation. Pharm. Res. 37, 80–95 (2020). https://doi.org/10.1016/j.jphotobiol.2020.112010
M. Handa et al., Therapeutic potential of nanoemulsions as feasible wagons for targeting Alzheimer’s disease. Drug Discov. Today 26, 2881–2888 (2021). https://doi.org/10.1016/j.drudis.2021.07.020
N. Vasdev et al., Rosemary oil low energy nanoemulsion: Optimization, µrheology, in silico, in vitro and Ex vivo characterization. J. Biomat. Sci. Polym. Edition. 33, 1901–1923 (2022). https://doi.org/10.1080/09205063.2022.2088527
T. Li et al., Preparation and properties of water-in-oil shiitake mushroom polysaccharide nanoemulsion. Int. J. Biol. Macromol. 140, 343–349 (2019). https://doi.org/10.1016/j.ijbiomac.2019.08.134
Y. Singh et al., Nanoemulsion: concepts, development and applications in drug delivery. J. Control. Release 252, 28–49 (2017). https://doi.org/10.1016/j.jconrel.2017.03.008
Badwan, A., et al., “Oral Delivery of Protein Drugs Using Microemulsion European”. Patent EP1797870, 2007.
Shin,S.H., et al.:Tracking perfluorocarbon nanoemulsion delivery by 19F MRI for precise high intensity focused ultrasound tumor ablation. Theranostics. 7, 562–572(2017). https://doi.org/10.7150/thno.16895
L. Guo et al., Preliminary evaluation of a novel oral delivery system for rhPTH1-34: in vitro and in vivo. Int. J. Pharm. 420(1), 172–179 (2011). https://doi.org/10.1016/j.ijpharm.2011.08.029
W. Li et al., A bufadienolide-loaded submicron emulsion for oral administration: stability, antitumor efficacy and toxicity. Int. J. Pharm. 479(1), 52–62 (2015). https://doi.org/10.1016/j.ijpharm.2014.12.054
G. Lida et al., Effective Inhibition and eradication of Pseudomonas aeruginosa bioflms by Satureja khuzistanica essential oil nanoemulsion. J. Drug Deliv. Sci Technol. 61, 102260–102268 (2021). https://doi.org/10.1016/j.jddst.2020.102260
L. HsuehYu et al., Preparation and evaluation of Cordyceps militaris polysaccharide- and sesame oil-loaded nanoemulsion for the treatment of candidal vaginitis in mice. Biomed. Pharmacother. 167, 115506–115517 (2023). https://doi.org/10.1016/j.biopha.2023.115506
A. Hairul et al., Preparation of nano-sized particles from bacterial cellulose using ultrasonication and their characterization. Carbohyd. Polym. 191, 161–167 (2018). https://doi.org/10.1016/j.carbpol.2018.03.026
K. Maheshika et al., Probe ultrasonication synthesis of Eu2O3-doped 2D WS2 nanosheets for highly selective and sensitive quantification of human catecholamines by fluorescent quenching and shifting. Mater. Res. Bull. 170, 112555–112564 (2024). https://doi.org/10.1016/j.materresbull.2023.112555
W. Jun et al., Formulation of water-in-oil-in-water (W/O/W) emulsions containing trans-resveratrol. RSC Adv. 7, 35917–35924 (2017). https://doi.org/10.1039/c7ra05945k
C. CLSI :Performance Standards for Antimicrobial Susceptibility Testing; Twenty-fourth Informational Supplement, M100-S24.2014.
T. Mosmann, Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. J. Immunol. Methods 65(1–2), 55–63 (1983). https://doi.org/10.1016/0022-1759(83)90303-4
I.V. Krishna et al., Cytotoxic studies of anti-neoplastic drugs on human lymphocytes in vitro studies. Cancer Biomark. 5, 261–272 (2009). https://doi.org/10.3233/CBM-2009-0111
H. Rachmawati et al., Curcumin nanoemulsion for transdermal application: formulation and evaluation. Drug Dev. Ind. Pharm. 41, 560–566 (2015). https://doi.org/10.3109/03639045.2014.884127
D.S. Santos et al., Oral delivery of fsh oil in oil-in-water nanoemulsion: development, colloidal stability and modulatory effect on in vivo inflammatory induction in mice. Biomed. Pharmacotherapy. 133, 110980–110997 (2021). https://doi.org/10.1016/j.biopha.2020.110980
S.K. Paudel et al., Antimicrobial activity of cinnamon oil nanoemulsion against Listeria monocytogenes and Salmonella spp. on melons. LWT Food Sci. Technol. 111, 682–687 (2019). https://doi.org/10.1016/j.lwt.2019.05.087
K.M.M. Leao et al., Physicochemical characterization and antimicrobial activity in novel systems containing buriti oil and structured lipids nanoemulsions. Biotechnology Reports. 24, e00365 (2019). https://doi.org/10.1016/j.btre.2019.e00365
W. Liping et al., Preparation of starch-based nanoemulsion for sustained release and enhanced bioaccessibility of quercetin. Colloids Surfaces A: Physicochemical Eng. 665, 131218–131230 (2023). https://doi.org/10.1016/j.colsurfa.2023.131218
Li. Meiting, Optimization of preparation conditions and in vitro sustained-release evaluation of a novel nanoemulsion encapsulating unsaturated guluronate oligosaccharide. Carbohyd. Polym. 264, 118047–118057 (2021). https://doi.org/10.1016/j.carbpol.2021.118047
R.B. Rigon et al., Solid lipid nanoparticles optimized by 2(2) factorial design for skin administration: Cytotoxicity in NIH3T3 fibroblasts. Colloids Surfaces B-Biointerfaces. 171, 501–505 (2018). https://doi.org/10.1016/j.colsurfb.2018.07.065
Acknowledgements
This research was based on the work supported by grants from the Natural Science Research of Jiangsu Higher Education Institutions of China (Grant No.19KJD230002), Scientific Research Foundation of Graduate School of Jiangsu Agri-animal Husbandry Vocational College, China (Grant No. NSFZP201902), and Animal medicine science and technology innovation team of Jiangsu Agri-Animal Husbandry Vocational College (Grant No. NSF2021TC02).
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shi, FF., Mao, YJ., Wang, Y. et al. Preparation of oral nanoemulsion drug delivery system loaded with punicalagin: in vitro antibacterial activity, drug release, and cell safety studies. Macromol. Res. 32, 243–252 (2024). https://doi.org/10.1007/s13233-023-00224-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13233-023-00224-8