Abstracts
Introduction
Medical disorders complicating pregnancy have recently emerged as the most common cause for maternal morbidity and mortality and it is important to predict mortality risk when they present in moribund state to emergency obstetric care so as to take and timely effective measures to prevent mortality.
Methods
This prospective observational study was conducted over 6 months among pregnant and post-partum women with medical disorders who sought emergency obstetric care at a tertiary care hospital. Severity of morbidity was assessed using SOFA and APACHE II scores at admission.
Results
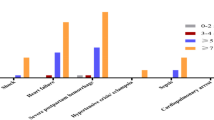
Of the 128 women, 87.5% were pregnant, and 12.5% were post-partum. Hypertensive disorders, cardiac disorders, neurological disorders and infective disorders were 24.2%, 22.6%, 14% and 9.4%, respectively. The optimal cut-off SOFA score was 2 (AUC = 0.739) with 66% sensitivity and 71% specificity and APACHE II score cut-off was 6 (AUC = 0.732) with a sensitivity of 60% and specificity of 78% in predicting severe maternal morbidity. The median scores of APACHE II and SOFA are 14 and 4, respectively, for non-survivors and for survivors it was 4 and 1.
Conclusion
Hypertensive disorder was the most common medical disorder, but severity was high in cardiac disorder. SOFA and APACHE II scores are good predictors of morbidity and mortality risk.


Similar content being viewed by others
References
Narayan B, Nelson-Piercy C. Medical problems in pregnancy. Clin Med. 2017;17(3):251.
Mantel GD, Buchmann E, Rees H, et al. Severe acute maternal morbidity: a pilot study of a definition for a near-miss. BJOG Int J Obstet Gynaecol. 1998;105(9):985–90.
Ferreira FL, Bota DP, Bross A, et al. Serial evaluation of the SOFA score to predict outcome in critically ill patients. JAMA. 2001;286(14):1754–8.
Knaus WA, Draper EA, Wagner DP, et al. APACHE II: a severity of disease classification system. Crit Care Med. 1985;13(10):818–29.
Demirkiran O, Dikmen Y, Utku T, et al. Critically ill obstetric patients in the intensive care unit. Int J Obstet Anesth. 2003;12(4):266–70.
Keizer JL, Zwart JJ, Meerman RH, et al. Obstetric intensive care admissions: a 12-year review in a tertiary care centre. Europ J Obstet Gynecol Reprod Biol. 2006;128(1–2):152–6.
Vargas M, Marra A, Buonanno P, et al. Obstetric admissions in ICU in a tertiary care center: a 5-years retrospective study. Indian J Crit Care Med Peer-Rev. 2019;23(5):213.
Pattinson RC, Buchmann E, Mantel G, et al. Can enquiries into severe acute maternal morbidity act as a surrogate for maternal death enquiries? BJOG Int J Obstet Gynaecol. 2003;110(10):889–93.
Parmar NT, Parmar AG, Mazumdar VS. Incidence of maternal “near-miss” events in a tertiary care hospital of central Gujarat, India. J Obstet Gynecol India. 2016;66(1):315–20.
Kumar R, Gupta A, Suri T, et al. Determinants of maternal mortality in a critical care unit: a prospective analysis. Lung India. 2022;39(1):44–50.
Sodhi K, Bansal V, Shrivastava A, et al. Predictors of mortality in critically ill obstetric patients in a tertiary care intensive care unit: a prospective 18 months study. J Obstet Anaesth Crit Care. 2018;8(2):73.
Fadiloglu E, Yuksel ND, Unal C, et al. Characteristics of obstetric admissions to intensive care unit: APACHE II, SOFA and the Glasgow coma scale. J Perinat Med. 2019;47(9):947–57.
Khergade M, Suri J, Bharti R, et al. Obstetric early warning score for prognostication of critically ill obstetric patient. Indian J Crit Care Med Peer-Rev. 2020;24(6):398.
Escobar MF, Nasner D, Hurtado CF, et al. Characterization of obstetric patients with sepsis identified by two diagnostic scales at a fourth-level clinic in Colombia. Int J Gynecol Obstet. 2018;143(1):71–6.
Oliveira-Neto AF, Parpinelli MA, Costa ML, et al. Prediction of severe maternal outcome among pregnant and puerperal women in obstetric ICU. Crit Care Med. 2019;47(2):e136-43.
Oliveira-Neto A, Parpinelli MA, Cecatti JG, et al. Sequential organ failure assessment score for evaluating organ failure and outcome of severe maternal morbidity in obstetric intensive care. Sci World J. 2012;1:2012.
Roopa P, Verma S, Rai L, et al. “Nearmiss” obstetric events and maternal deaths in a tertiary care hospital: an audit. J Pregnancy. 2013;2013:393758
Norhayati MN, Hazlina NH, Sulaiman Z, et al. Severe maternal morbidity and near misses in tertiary hospitals, Kelantan, Malaysia: a cross-sectional study. BMC Public Health. 2016;16(1):1–3.
Binda J, Solanki G. Clinical and etiological study of maternal near-miss at a tertiary referral hospital of central India. Indian J Obstet Gynaecol Res. 2016;3(1):28–31.
Siddiqui SA, Soomro N, Hasnain FS. Severe obstetric morbidity and its outcome in patients presenting in a tertiary care hospital of Karachi. JPMA J Pak Med Assoc. 2012;62(3):226.
Bhadade R, de Souza R, More A, et al. Maternal outcomes in critically ill obstetrics patients: a unique challenge. Indian J Crit Care Med Peer-Reviewed Off Publ Indian Soc Crit Care Med. 2012;16(1):8.
Jain S, Guleria K, Vaid NB, et al. Predictors and outcome of obstetric admissions to intensive care unit: a comparative study. Indian J Public Health. 2016;60(2):15914.
Kamal S, Singh V, Singh S. A study of clinical characteristics and outcome of obstetric patients in intensive care and high dependency unit of a tertiary centre of Jharkhand, India. Int J Reprod Contracept Obstet Gynecol. 2020;9:394–9.
Acknowledgment
The authors thank Dr Simi, Resident in the Department of Preventive and Social Medicine, for her help in statistical analysis.
Funding
The author(s) received no financial support for the research, authorship and/or publication of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author(s) declared no potential conflict of interest with respect to the research, authorship and/or publication of this article.
Ethical Approval
All data collected after getting approval from institutional ethical committee (JIP/IEC/2021/059).
Human and Animal Rights
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation and with Helsinki Declaration 1975, as revised in 2008.
Informed Consent of Publications
Informed consent was obtained from all women for being included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Mecheril Balachandran Divya (MBBS, MS OBG, PDF Obstetric Medicine) is a Former Senior Resident; Papa Dasari (MD, DGO, FICOG, PDCR) is a Senior Professor.
Appendix 1
Appendix 1
Calculation of apache II score: value range from 0 to 71.
APACHE II Score = Acute physiology score (A) + Glasgow coma score (B) + Chronic health points (C).
A. Acute physiology score
Acute physiology score | Normal range | ||||||||
|---|---|---|---|---|---|---|---|---|---|
Score | 4 | 3 | 2 | 1 | 0 | 1 | 2 | 3 | 4 |
Rectal temperature (°C) | ≥ 41 | 39–40.9 | – | 38.5–38.9 | 36–38.4 | 34–35.9 | 32–33.9 | 30–31.9 | ≤ 29.9 |
Mean blood pressure (mmHg) | ≥ 160 | 130–159 | 110–129 | – | 70–109 | – | 50–69 | – | ≤ 49 |
Heart rate | ≥ 180 | 140–179 | 110–139 | – | 70–109 | – | 55–69 | 45–54 | ≤ 39 |
Respiratory rate | ≥ 50 | 35–49 | – | 25–34 | 12–24 | 10–11 | 6–9 | – | ≤ 5 |
Arterial pH | ≥ 7.7 | 7.6–7.69 | – | 7.5 –7.59 | 7.33–7.49 | – | 7.25–7.32 | 7.15–7.24 | ≤ 7.15 |
Oxygenation, PaO2 | ≥ 500 | 350–499 | 200–349 | – | < 200 > 70 | 61–70 | – | 55–60 | < 55 |
Serum sodium (mEq/L) | ≥ 180 | 160–179 | 155–159 | 150–154 | 130–149 | – | 120–129 | 111–119 | ≤ 110 |
Serum potassium (mEq/L) | ≥ 7 | 6–6.9 | – | 5.5–5.9 | 3.5–5.4 | 3–3.4 | 2.5–2.9 | – | < 2.5 |
Serum creatinine (mg/dL) | ≥ 3.5 | 2–3.4 | 1.5–1.9 | – | 0.6–1.4 | – | < 0.6 | – | – |
Haematocrit (%) | ≥ 60 | – | 50–59.9 | 46–49.9 | 30–45.9 | – | 20–29.9 | – | < 20 |
WBC count (103/ml) | ≥ 40 | – | 20–39.9 | 15–19.9 | 3–14.9 | – | 1–2.9 | – | < 1 |
B. Glasgow coma scale
Eye opening | Verbal non-intubated | Verbal intubated | Motor activity |
|---|---|---|---|
4 = spontaneous | 5—Oriented and talks | 5—Seems able to talk | 6—Verbal command |
3 = verbal stimuli | 4—Disoriented and talks | 3—Questionable ability to talk | 5—Localizes to pain |
2 = painful stimuli | 3—Inappropriate words | 1—Generally unresponsive | 4—Withdraws from pain |
1 = no response | 2—Incomprehensible sounds | 3—Decorticate | |
1—No response | 2—Decerebrate | ||
1—No response |
C. Chronic health points
History of chronic condition | Score |
|---|---|
None | 0 |
If elective post-operative patient with immunocompromise or severe organ insufficiency | 2 |
Non-operative patient or emergency post-operative patient with immunocompromise or severe organ insufficiency | 5 |
D. Calculation of SOFA score: value range from 0 to 24
System | Scores | ||||
|---|---|---|---|---|---|
0 | 1 | 2 | 3 | 4 | |
Respiratory system parameter, PaO2/FiO2 (mmHg) | ≥ 400 | < 400 | < 300 | < 200 | < 100 |
Coagulation system Platelets *103/µL | > 150 | < 150 | < 100 | < 50 | < 20 |
Hepatobiliary system parameter Bilirubin, mg/dL | < 1.2 | 1.2–1.9 | 2–5.9 | 6–11.9 | > 12 |
Cardiovascular parameter | MAP > 70 mmHg | MAP < 70 mmHg | Dopamine < 5 or dobutamine (any dose) | Dopamine 5.1–15 or epinephrine < 0.1 or norepinephrine < 0.1 | Dopamine > 15 or Epinephrine > 0.1 or norepinephrine > 0.1 |
Central nervous system Glasgow coma scale | 15 | 13–14 | 10–12 | 6–9 | < 6 |
Renal parameters creatinine, mg/dL | < 1.2 | 1.2–1.9 | 2–3.4 | 3.5–4.9 | > 5 |
Urine output, ml/day | < 500 | < 200 | |||
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Divya, M.B., Dasari, P. Prediction of Maternal Morbidity and Mortality Risk Among Women with Medical Disorders Presenting to Emergency Obstetric care (EMOC): A Prospective Observational Study. J Obstet Gynecol India 73, 522–530 (2023). https://doi.org/10.1007/s13224-023-01859-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13224-023-01859-4