Abstract
Background
Given the underutilization of contraception in India, this study was undertaken to gauge cisgender female clients’ knowledge of, attitudes toward, and barriers to contraceptive usage in North India.
Methodology
The present study was done at a tertiary care Institute in North India, where 209 structured interviews were conducted with cisgender female patients attending the outpatient department. One-way chi-square tests for independence, Kruskal–Wallis test, and Wilcoxon test were applied to quantitative data. Themes from qualitative questions were coded and analyzed.
Results
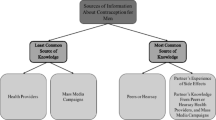
Differences in awareness among contraceptives were found to be highly statistically significant (H (9) = 1022.3, p < 2.2 e−16). Friends or colleagues comprised the predominant information source for most contraceptive methods. Participants’ contraceptive usage was low, with 27.27% stating no prior use and 47.47% indicating occasional use (X2 (3, N = 198) = 66.121, p < 2.89 e−14). Lack of perceived need, concern for side effects, fear and desire for children were top reasons for non-use of contraceptive methods. Majority of the participants (79.45%) expressed comfort speaking with their spouse about contraception, 47.18% with a medical provider, 32.82% with friends, 15.38% with family, 2.05% with a health educator, and 3.59% with no one. Participants indicated little prior contraceptive counseling experience.
Conclusion
Our study shows differential levels of awareness, usage, and barriers on contraceptive methods among participants. Results also suggest the importance of spouses and friends in clients’ contraceptive decision-making process and their limited counseling experience with health care providers.
Similar content being viewed by others
Notes
1While language around the study sample specifies their gender identity as cisgender females, in other places terms such as “women,” “men,” “female,” and “male” are used in accordance with the literature they refer to.
References
Bearak JM, Popinchalk A, Beavin C, et al. Country-specific estimates of unintended pregnancy and abortion incidence: a global comparative analysis of levels in 2015–2019. BMJ Glob Health. 2022;7(3):e007151. https://doi.org/10.1136/bmjgh-2021-007151. (PMID: 35332057; PMCID: PMC8943721).
State of World Population 2022 [Internet]. United Nations Population Fund (UNFPA); Available from: https://www.unfpa.org/sites/default/files/pub-pdf/EN_SWP22%20report_0.pdf
Sarder A, Islam SMS, Maniruzzaman TA, et al. Prevalence of unintended pregnancy and its associated factors: evidence from six south Asian countries. PLoS ONE. 2021;16(2):e0245923.
Sen S, Cetinkaya A, Cavuslar A. Perceptıon scale of barrıers to contraceptıve use: a methodologıcal study. Fertil Res Pract. 2017;3(1):11.
Raj A, Ghule M, Ritter J, et al. Cluster Randomized Controlled Trial Evaluation of a Gender Equity and Family Planning Intervention for Married Men and Couples in Rural India. PLoS ONE. 2016;11(5):e0153190. https://doi.org/10.1371/journal.pone.0153190. (PMID: 27167981; PMCID: PMC4864357).
Ezeanolue EE, Iwelunmor J, Asaolu I, et al. Impact of male partner’s awareness and support for contraceptives on female intent to use contraceptives in southeast Nigeria. BMC Public Health. 2015;15(1):879.
Agyekum MW, Henry EG, Kushitor MK, et al. Partner support and women’s contraceptive use: insight from urban poor communities in Accra, Ghana. BMC Womens Health. 2022;22(1):256.
Caetano C, Bliekendaal S, Engler Y, et al. From awareness to usage of long-acting reversible contraceptives: results of a large European survey. Int J Gynecol Obstet. 2020;151(3):366–76.
Khatri B, Khadka A, Amatya A, et al. Perception And Use Of Intrauterine Contraceptive Devices (IUCD) Among Married Women Of Reproductive Age In Bhaktapur Nepal. Open Access J Contracept. 2019;28(10):69–77.
Thummalachetty N, Mathur S, Mullinax M, et al. Contraceptive knowledge, perceptions, and concerns among men in Uganda. BMC Public Health. 2017;17(1):792.
Paul P, Mondal D. Association between intimate partner violence and contraceptive use in India: exploring the moderating role of husband’s controlling behaviors. J Interpers Violence. 2022;37(17–18):NP15405–33. https://doi.org/10.1177/08862605211015212. (Epub 2021 May 17. PMID: 34000903).
Prusty RK, Begum S. Missing men in family planning: understanding the socio-spatial differentials in male sterilization and male spacing methods of contraception in India. J Biosoc Sci. 2023;55(1):116–30. https://doi.org/10.1017/S0021932021000717. (Epub 2021 Dec 20. PMID: 34927580).
Choudhary A, Nakade M, Shrivastava D. Family planning knowledge, attitude and practice among women of reproductive age from rural area of central India. Int J Curr Res Rev. 2020;12(14):02–7. https://doi.org/10.31782/IJCRR.2020.0207.
Nayak R, Panda M, Padhy S, et al. Awareness regarding emergency contraception among married women attending urban health centre, Berhampur, Odisha, India. Int J Res Med Sci. 2020;8(2):524. https://doi.org/10.18203/2320-6012.ijrms20200229.
Singh S, Hussain R, Shekhar C, et al. Incidence of treatment for postabortion complications in India, 2015. BMJ Glob Health. 2020;5:e002372. https://doi.org/10.1136/bmjgh-2020-002372.
Woldeyohannes D, Arega A, Mwanri L. Reasons for low utilization of intrauterine device utilisation amongst short term contraceptive users in Hossana town, Southern Ethiopia: a qualitative study. BMC Womens Health. 2022;22(1):30.
Patient-centered contraceptive counseling | ACOG [Internet]. Available from: https://www.acog.org/clinical/clinical-guidance/committee-statement/articles/2022/02/patient-centered-contraceptive-counseling. Accessed 24 Jul 2022.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Our study had no conflict of interest.
Ethical Approval
Institutional ethical committee clearance was obtained for study. The study has been performed in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards. The authors hereby declare that the article is original; neither the article nor a part of it is under consideration for publication anywhere else and has not been previously published anywhere. We have declared all vested interests. We have meticulously followed the instructions. The article if published shall be the property of the journal.
Informed Consent
Informed consent was obtained from all patients included in study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Sneha Mittal is a Visiting Student; Vineeta Gupta is Professor and Head of Department; Namrata Saxena is Professor; Kirti Lata is a Junior Resident.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mittal, S., Gupta, V., Saxena, N. et al. Patient Perspectives on Contraceptive use in North India: A Case for Increased Contraceptive Counseling by Providers. J Obstet Gynecol India 73, 512–521 (2023). https://doi.org/10.1007/s13224-023-01781-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13224-023-01781-9