Abstract
Background
In Low- and Middle-Income Countries like India, where the services and surgical care for Congenital Heart Disease (CHD) are available only in selected centres with geographical variations, it is important to detect Heart defects early and give the parents an opportunity to plan ahead for seeking appropriate care at the earliest. Several developments in recent years such as improvement of quality of ultrasound machines, sonographer’s experience, skills and better description of cardiac views have contributed to improve detection rate.
Methods
A retrospective study was done between March 2016 and December 2019, and showed ultrasound evidence of CHD was included.
Results
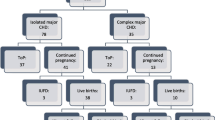
The total number of morphology scans done during study period was 50,435. The number of congenital anomalies detected was 1482, out of which CHD was detected in 334 (22.5%). Outcome of 50 pregnancies were not available while the rest (284) were available for follow up in post-natal period. There were 51 cases of CHD, missed on routine antenatal morphological screening, which were diagnosed in the post-natal period. There were 18 cases of over-diagnosed CHD on antenatal scan, but were found to have normal echo findings after birth.
Conclusion
A systematic approach is crucial for practitioner to determine the patterns of associated defects. Use of step wise strategy helps in determining the correct diagnosis of isolated cardiac defect, associated with other system or a part of syndrome. Systematic audit of morphological scans could play an important role in improving the diagnostic accuracy, which in turn will lead to early detection.


Similar content being viewed by others
References
Bahtiyar MO, Copel JA. Screening for Congenital Heart Disease During Anatomical Survey Ultrasonography. Obstet Gynecol Clin. 2015;42(2):209–23. https://www.obgyn.theclinics.com/article/S0889-8545(15)00015-7/abstract. Accessed 5 Dec 2020.
Saxena A. Congenital heart disease in india: a status report. Indian Pediatr. 2018;55(12):1075–82.
Birth prevalence of congenital heart disease: A cross-sectional observational study from North India Saxena A, Mehta A, Sharma M, Salhan S, Kalaivani M, Ramakrishnan S, Juneja R—Ann Pediatr Card. https://www.annalspc.com/article.asp?issn=0974-2069;year=2016;volume=9;issue=3;spage=205;epage=209;aulast=Saxena. Accessed 5 Dec 2020.
Singh Y, McGeoch L. Fetal anomaly screening for detection of congenital heart defects. J Neonatal Biol. 2016;05(02). https://www.omicsgroup.org/journals/fetal-anomaly-screening-for-detection-of-congenital-heart-defects-2167-0897-100e115.php?aid=73446. Accessed 5 Apr 2020.
Kenkhuis MJA, Bakker M, Bardi F, Fontanella F, Bakker MK, Fleurke-Rozema JH, et al. Effectiveness of 12–13-week scan for early diagnosis of fetal congenital anomalies in the cell-free DNA era. Ultrasound ObstetGynecol Off J IntSoc Ultrasound ObstetGynecol. 2018;51(4):463–9.
Kumar RK. Screening for congenital heart disease in India: Rationale, practical challenges, and pragmatic strategies. Ann Pediatr Cardiol. 2016; 9(2):111–4. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4867793/. Accessed 7 Apr 2020.
Hana J, Pavel V, Michal J, Ilga G, Viktor T, Julia V, et al. Does first-trimester screening modify the natural history of congenital heart disease? Circulation. 2017;135(11):1045–55.
Lavanya S, Seethalakshmi V. A two-year study of patterns and prevalence of congenital malformations. Int J Reprod Contracept Obstet Gynecol [Internet]. 2017; 7(1):114. http://www.ijrcog.org/index.php/ijrcog/article/view/4068. Accessed 25 May 2020.
Bravo-valenzuela NJ, Peixoto AB, Araujo Júnior E. Prenatal diagnosis of congenital heart disease: a review of current knowledge. Indian Heart J. 2018; 70(1):150–64. http://www.sciencedirect.com/science/article/pii/S0019483217305849. Accessed 5 Apr 2020.
Qiu X, Weng Z, Liu M, Chen X, Wu Q, Ling W, et al. Prenatal diagnosis and pregnancy outcomes of 1492 fetuses with congenital heart disease: role of multidisciplinary-joint consultation in prenatal diagnosis. Sci Rep. 2020;10(1):7564. https://www.nature.com/articles/s41598-020-64591-3. Accessed 5 May 2020.
Yadav. Spectrum of antenatally diagnosed cardiac anomalies in a tertiary referral center of North India. http://www.heartindia.net/article.asp?issn=2321-449x;year=2019;volume=7;issue=3;spage=123;epage=128;aulast=Yadav. Accessed 14 Apr 2020.
Meshram. Prevalence, profile, and pattern of congenital heart disease in Central India: a prospective, observational study. http://www.nigjcardiol.org/article.asp?issn=0189-7969;year=2018;volume=15;issue=1;spage=45;epage=49;aulast=Meshram. Accessed 3 Jul 2020.
Miceli F. A review of the diagnostic accuracy of fetal cardiac anomalies. Australas J Ultrasound Med. 2015;18(1):3.
Goetzinger K, Shanks A, Odibo A, Macones G, Cahill A. Advanced maternal age and the risk of major congenital anomalies. Am J Perinatol. 2016;34(03):217–22.
Best KE, Rankin J. Is advanced maternal age a risk factor for congenital heart disease? Birt Defects Res A ClinMolTeratol. 2016;106(6):461–7.
Sinkovskaya ES, Chaoui R, Karl K, Andreeva E, Zhuchenko L, Abuhamad AZ. Fetal cardiac axis and congenital heart defects in early gestation. ObstetGynecol. 2015;125(2):453–60.
CDC. Data and Statistics on Congenital Heart Defects |CDC. centers for disease control and prevention. 2019. https://www.cdc.gov/ncbddd/heartdefects/data.html. Accessed 5 Apr 2020.
Changlani TD, Jose A, Sudhakar A, Rojal R, Kunjikutty R, Vaidyanathan B. Outcomes of infants with prenatally diagnosed congenital heart disease delivered in a tertiary-care pediatric cardiac facility. Indian Pediatr 2015;52(10):852–6. http://link.springer.com/10.1007/s13312-015-0731-x. Accessed 26 May 2020.
Zühlke L, Lawrenson J, Comitis G, De Decker R, Brooks A, Fourie B, et al. Congenital heart disease in low- and lower-middle-income countries: current status and new opportunities. CurrCardiol Rep. 2019;21(12):163.
Abqari S, Gupta A, Shahab T, Rabbani M, Ali SM, Firdaus U. Profile and risk factors for congenital heart defects: A study in a tertiary care hospital. Ann Pediatr Cardiol. 2016;9(3):216–21. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5007929/. Accessed 6 Dec 2020.
Raju KP, Prasad SG. Telemedicine and Tele-echocardiography in India. Cardiovasc Imaging. 2017;1(2):10.
Britton N, Miller MA, Safadi S, Siegel A, Levine AR, McCurdy MT. Tele-Ultrasound in resource-limited settings: a systematic review. Front Public Health. 2019; 7. https://www.frontiersin.org/articles/10.3389/fpubh.2019.00244/full. Accessed 6 Dec 2020.
Funding
Did not require funding as it is a retrospective study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Nil, Varunashree ND (VND), Ravi Shankar (RS), Manish Kumar (MK), Preethi Navaneethan, (PN), Santosh Benjamin (SB), Smitha Elizabeth Jacob (SMJ), Bijesh Yadav (BY) and Swati Rathore (SR) declare that they have no conflict of interest.
Ethical approval
A retrospective study was done from a prospectively maintained database of the antenatal morphology scans done in the Department of Obstetrics and Gynaecology, after obtaining approval from the institutional review board and ethics committee (IRB Min No. 10495 retro dated 18/01/2017).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Varunashree, N.D., Shankar, R., Navaneethan, P. et al. Efficacy of Antenatal Ultrasound Examination in Diagnosis of Congenital Cardiac Anomalies in an Unselected Population: Retrospective Study from a Tertiary Centre. J Obstet Gynecol India 71, 277–284 (2021). https://doi.org/10.1007/s13224-020-01424-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13224-020-01424-3