Abstract
Purpose of the Study
Intrauterine contraceptive devices (IUCDs) are highly effective form of long-acting reversible contraception having least number of complications. We aimed to find the incidence, risk factors and the management done for incarcerated and transmigrated intrauterine contraceptive devices at a Tertiary Care Teaching Hospital during past 5 years.
Methods
A cross-sectional retrospective analysis of 5 years (January 2013–December 2017) was done, and the case records from Medical Record Department and Family Planning Unit of our institution were analysed.
Results
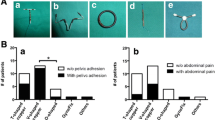
Total number of IUCD insertions done in last 5 years (from January 2013 to December 2017) in our institution was 4557. Misplaced IUCDs requiring surgical interventions were 71 (1.6%) out of which 63 (88.7%) were incomplete perforations or embedded and 8 (11.3%) were complete perforations or transmigrated IUCDs. Transmigration sites were omentum, uterovesical fold, mesentery and bladder. Laparotomy was needed in 4 (5.6%), and 2 (2.8%) needed each laparoscopy and cystoscopy. Main risk factors identified were postpartum previous on or two caesarean sections, low parity, grade of operator and IUCD and uterocervical length discrepancy.
Conclusion
The risk of perforation should not be a reason to defer IUCD insertion and every effort should be made to bring down its failure and complication rates.




Similar content being viewed by others
References
American College of Obstetricians and Gynecologists. ACOG Practice Bulletin No. 121: long-acting reversible contraception: implants and intrauterine devices. Obstet Gynecol. 2011;118(1):184–96.
Goldstuck N. Assessment of uterine cavity size and shape: a systematic review addressing relevance to intrauterine procedures and events. Afr J Reprod Health. 2012;16(3):130–9.
Goldstuck ND, Wildemeersch D. Role of uterine forces in intrauterine device embedment, perforation, and expulsion. Int J Health. 2014;6:735–44.
Heinemann K, Reed S, Moehner S, et al. Risk of uterine perforation with levonorgestrel-releasing and copper intrauterine devices in the European Active Surveillance Study on Intrauterine Devices. Contraception. 2015;91:274–9.
Goldstuck ND, Steyn PS. Intrauterine contraception after cesarean section and during lactation: a systematic review. Int J Womens Health. 2013;5:811–8.
Rowlands S, Oloto E, Horwell HD. Intrauterine devices and risk of uterine perforation: current perspectives. Open Acess J Contracept. 2016;7:19–32.
Varun N, Nigam A, Gupta N. Misplaced IUCD: a case report. Int J Reprod Contracept Obstet Gynecol. 2017;6(11):5155–7.
Kumar H, Sharma P, Aggarwal B. Migrated intrauterine contraceptive device: erosion into sigmoid colon. Int J Res Med Sci. 2018;6(5):1828–30.
Goyal S, Goyal S. Displaced intrauterine device: a retrospective study. J Med Res. 2016;2(2):41–3.
Armo M, Minj IB, Triki AR, et al. Copper T (380 A) and risk of uterine perforation in lactating women: rural scenario. Int J Reprod Contracept Obstet Gynecol. 2017;6(7):3026–9.
Braaten KP, Benson CB, Maurer R, et al. Malpositioned intrauterine contraceptive devices: risk factors, outcomes, and future pregnancies. Obstet Gynecol. 2011;118(5):1014–20.
IUCD Reference Manual for Medical Officers and Nursing Personnel September 2013. Family Planning Division Ministry of Health and Family Welfare Government of India.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
There are no conflicts of interest for any of the authors.
Ethical Statements
Prior ethical clearance was obtained from Institutional Ethical Committee—Human Research of our institution.
Rights and permissions
About this article
Cite this article
Sharma, R., Suneja, A. Incarcerated and Transmigrated Intrauterine Contraceptive Devices Managed at a Tertiary Care Teaching Hospital of East Delhi: A 5-Year Retrospective Analysis. J Obstet Gynecol India 69, 272–278 (2019). https://doi.org/10.1007/s13224-018-1159-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13224-018-1159-8