Abstract
Background
Polycystic ovarian syndrome (PCOS), a commonly prevalent endocrinopathy among reproductive age group women, is most often associated with obesity. Increased insulin resistance appears to be the central pathophysiologic mechanism responsible for various complications of PCOS. This makes ‘weight loss’ as the first-line treatment approach in PCOS. So various trials have tried to compare metformin (an insulin-sensitizing agent) and orlistat (an anti-obesity drug) aiming to achieve weight loss and hence higher ovulation rate for the group of obese PCOS patients. Keeping an eye on all these background facts, we designed this systematic review and metaanalysis to compare the effects of metformin and orlistat on various aspects of PCOS and to pick the better among the two drugs.
Materials and Methods
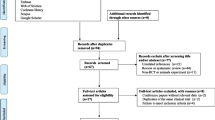
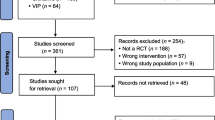
This is a systemic review of randomized control trials that studied the effectiveness of orlistat versus metformin in terms of improvement in ovulation rate, weight loss, lipid profile, etc. Systematic literature search over the period January 2000–December 2016 was performed in the following electronic databases: Medline, embase, google scholar, pubmed and The Cochrane Library and only randomized controlled clinical trials were included in our study. All authors carefully went through all sources of information independently.
Results
According to this study, weight loss, testosterone level after 4 weeks of treatment, total serum cholesterol and triglyceride level showed significant fall in orlistat-treated group.
Conclusion
Our review shows that orlistat is a more effective drug than metformin and should be the preferred drug in obese PCOS in combination with weight loss.

Similar content being viewed by others
References
Fauser BCJM, Tarlatzis BC, Rebar RW, et al. Amsterdam ESHRE/ASRM-Sponsored 3rd PCOS Consensus Workshop Group. Consensus on women’s health aspects of polycystic ovary syndrome (PCOS). Hum Reprod. 2012;27:14–24.
Moran LJ, Pasquali R, Teede HJ, et al. Treatment of obesity in polycystic ovary syndrome: a position statement of the Androgen Excess and Polycystic Ovary Syndrome Society. Fertil Steril. 2009;92:1966–82.
Metwally M, Amer S, Li TC, et al. An RCT of metformin versus orlistat for the management of obese anovulatory women. Hum Reprod. 2009;24:966–75.
Kumar P, Arora S. Orlistat in polycystic ovarian syndrome reduces weight with improvement in lipid profile and pregnancy rates. J Hum Reprod Sci. 2014;7(4):255–61.
Ghandi S, Aflatoonian A, Tabibnejad N, et al. The effects of metformin or orlistat on obese women with polycystic ovary syndrome: a prospective randomized open-label study. J Assist Reprod Genet. 2011;28:591–6.
Jayagopal V, Kilpatrick ES, Holding S, et al. Orlistat is as beneficial as metformin in the treatment of polycystic ovarian syndrome. J Clin Endocrinolmetab. 2005;90:729–33.
Kujawska-Łuczak M, Musialik K, Szulińska M, et al. The effect of orlistat versus metformin on body composition and insulin resistance in obese premenopausal women: 3-month randomized prospective open-label study. Arch Med Sci. 2016. https://doi.org/10.5114/aoms.2016.62014.
Cho LW, Kilpatrick ES, Keevil BG, et al. Effect of metformin, orlistat and pioglitazone treatment on mean insulin resistance and its biological variability in polycystic ovary syndrome. Clin Endocrinol. 2009;70:233–7.
Padwal RS, Majumdar SR. Drug treatments for obesity: orlistat, sibutramine, and rimonabant. Lancet. 2007;369:71–7.
English PJ, Ashcroft A, Patterson M, et al. Metformin prolongs the postprandial fall in plasma ghrelin concentrations in type 2 diabetes. Diabetes Metab Res Rev. 2007;23:299–303.
Agarwal N, Rice SP, Bolusani H, et al. Metformin reduces arterial stiffness and improves endothelial function in young women with polycystic ovary syndrome: a randomized, placebo—controlled, crossover trial. J Clin Endocrinol Metab. 2010;95:722–30.
Orlistat: MedlinePlus Drug Information [Internet]. Medlineplus.gov. 2016 [cited: Sep 15 2016]. https://medlineplus.gov/druginfo/meds/a601244.html.
Filippatos TD, Derdemezis CS, Gazi IF, et al. Orlistat-associated adverse effects and drug interactions. Drug Saf. 2008;31(1):53–65.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Soumya Ranjan Panda is senior Resident, Department of Obstetrics and Gynecology, IMS, BHU, Varanasi, UP. Madhu Jain is a Professor and Head, Department of Obstetrics and Gynecology, IMS, BHU, Varanasi, UP. Shuchi Jain is an Assistant Professor, Department of Obstetrics and Gynecology, IMS, BHU, Varanasi, UP. Riden Saxena is a Phd Scholar, Department of Obstetrics and Gynecology, IMS, BHU, Varanasi, UP. Smrutismita Hota is a Junior Resident, Department of Radiodiagnosis, IMS, BHU, Varanasi, UP.
Rights and permissions
About this article
Cite this article
Panda, S.R., Jain, M., Jain, S. et al. Effect of Orlistat Versus Metformin in Various Aspects of Polycystic Ovarian Syndrome: A Systematic Review of Randomized Control Trials. J Obstet Gynecol India 68, 336–343 (2018). https://doi.org/10.1007/s13224-018-1140-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13224-018-1140-6