Abstract
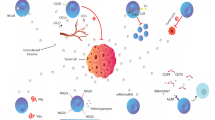
This study was conducted to explore whether acute lymphoblastic leukemia (ALL)-derived exosomes affect natural killer (NK) cells. Exosomes were isolated and identified from Jurkat cells and co-cultured with NK cells. Then, the cytotoxicity, viability, and release of perforin and granzyme B in NK92-MI cells were measured. PCR arrays were used to detect gene expression alterations in the transforming growth factor (TGF)-β pathway of NK92-MI cells treated or not treated with exosomes. The morphology and size of the exosomes isolated from Jurkat cells showed typical characteristics of exosomes, and the expression of cluster of differentiation 63 was detected. Jurkat-derived exosomes were internalized by NK92-MI cells, further inhibiting the proliferation and cytotoxicity of NK92-MI cells. An enzyme-linked immunosorbent assay revealed that the release of perforin and granzyme B from NK92-MI cells decreased after co-culture with exosomes. Similarly, western blot and immunofluorescence staining verified that Jurkat-derived exosomes inhibited the expression of granzyme B and perforin. Furthermore, Jurkat-derived exosomes enhanced the signaling of the TGF-β pathway in NK92-MI cells via the MDS1 and EVI1 complex loci and homeodomain interacting protein kinase 2. In conclusion, we found that ALL-derived exosomes inhibit the biological function of NK cells and provide support for the immunotherapy of ALL.





Similar content being viewed by others
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Change history
27 July 2021
A Correction to this paper has been published: https://doi.org/10.1007/s13205-021-02906-5
References
Barwe SP, Quagliano A, Gopalakrishnapillai A (2017) Eviction from the sanctuary: development of targeted therapy against cell adhesion molecules in acute lymphoblastic leukemia. Semin Oncol 44:101–112. https://doi.org/10.1053/j.seminoncol.2017.06.005
Berchem G et al (2016) Hypoxic tumor-derived microvesicles negatively regulate NK cell function by a mechanism involving TGF-beta and miR23a transfer. Oncoimmunology 5:e1062968. https://doi.org/10.1080/2162402X.2015.1062968
Boyiadzis M, Whiteside TL (2018) Exosomes in acute myeloid leukemia inhibit hematopoiesis. Curr Opin Hematol 25:279–284. https://doi.org/10.1097/MOH.0000000000000439
Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68:394–424. https://doi.org/10.3322/caac.21492
Briand J et al (2020) Radiotherapy-induced overexpression of exosomal miRNA-378a-3p in cancer cells limits natural killer cells cytotoxicity. Epigenomics 12:397–408. https://doi.org/10.2217/epi-2019-0193
Buonamici S et al (2005) EVI1 abrogates interferon-alpha response by selectively blocking PML induction. J Biol Chem 280:428–436. https://doi.org/10.1074/jbc.M410836200
Cao L et al (2019) HIPK2 is necessary for type I interferon-mediated antiviral immunity. Sci Signal. https://doi.org/10.1126/scisignal.aau4604
Chang X et al (2017) The antihelmenthic phosphate niclosamide impedes renal fibrosis by inhibiting homeodomain-interacting protein kinase 2 expression. Kidney Int 92:612–624. https://doi.org/10.1016/j.kint.2017.01.018
Chen W et al (2016) Cancer statistics in China, 2015. CA Cancer J Clin 66:115–132. https://doi.org/10.3322/caac.21338
Dulphy N et al (2016) Underground adaptation to a hostile environment: acute myeloid leukemia vs. natural killer cells. Front Immunol 7:94. https://doi.org/10.3389/fimmu.2016.00094
He L, Wang D, Zou H (2014) Characterization of a novel variant allele, HLA-C*04:03:02, identified in a Chinese Han individual. Tissue Antigens 83:433–434. https://doi.org/10.1111/tan.12333
Huang F, Wan J, Hu W, Hao S (2017) Enhancement of anti-leukemia immunity by leukemia-derived exosomes via downregulation of TGF-beta1 expression. Cell Physiol Biochem 44:240–254. https://doi.org/10.1159/000484677
Inaba H, Greaves M, Mullighan CG (2013) Acute lymphoblastic leukaemia. Nurs Times 381:1943–1955
Katz AJ, Chia VM, Schoonen WM, Kelsh MA (2015) Acute lymphoblastic leukemia: an assessment of international incidence, survival, and disease burden. Cancer Causes Control 26:1627–1642. https://doi.org/10.1007/s10552-015-0657-6
Korzeniewski C, Callewaert DM (1983) An enzyme-release assay for natural cytotoxicity. J Immunol Methods 64:313–320. https://doi.org/10.1016/0022-1759(83)90438-6
Kumar B et al (2018) Acute myeloid leukemia transforms the bone marrow niche into a leukemia-permissive microenvironment through exosome secretion. Leukemia 32:575–587. https://doi.org/10.1038/leu.2017.259
Malard F, Mohty M (2020) Acute lymphoblastic leukaemia. Lancet 395:1146–1162. https://doi.org/10.1016/S0140-6736(19)33018-1
Mitani K (2004) Molecular mechanisms of leukemogenesis by AML1/EVI-1. Oncogene 23:4263–4269. https://doi.org/10.1038/sj.onc.1207777
Mizia-Malarz A, Sobol-Milejska G (2019) NK Cells as Possible Prognostic Factor in Childhood Acute Lymphoblastic Leukemia. Dis Mark 2019:3596983. https://doi.org/10.1155/2019/3596983
Oelsner S et al (2019) Genetically engineered CAR NK cells display selective cytotoxicity against FLT3-positive B-ALL and inhibit in vivo leukemia growth. Int J Cancer 145:1935–1945. https://doi.org/10.1002/ijc.32269
Peng D et al (2018) miR-34c-5p promotes eradication of acute myeloid leukemia stem cells by inducing senescence through selective RAB27B targeting to inhibit exosome shedding. Leukemia 32:1180–1188. https://doi.org/10.1038/s41375-018-0015-2
Prieto D et al (2017) S100–A9 protein in exosomes from chronic lymphocytic leukemia cells promotes NF-kappaB activity during disease progression. Blood 130:777–788. https://doi.org/10.1182/blood-2017-02-769851
Raimondo S et al (2015) Chronic myeloid leukemia-derived exosomes promote tumor growth through an autocrine mechanism. Cell Commun Signal 13:8. https://doi.org/10.1186/s12964-015-0086-x
Roma-Rodrigues C, Fernandes AR, Baptista PV (2019) Counteracting the effect of leukemia exosomes by antiangiogenic gold nanoparticles. Int J Nanomed 14:6843–6854. https://doi.org/10.2147/IJN.S215711
Rouce RH et al (2016) The TGF-beta/SMAD pathway is an important mechanism for NK cell immune evasion in childhood B-acute lymphoblastic leukemia. Leukemia 30:800–811. https://doi.org/10.1038/leu.2015.327
Sharma P, Diergaarde B, Ferrone S, Kirkwood JM, Whiteside TL (2020) Melanoma cell-derived exosomes in plasma of melanoma patients suppress functions of immune effector cells. Sci Rep 10:92. https://doi.org/10.1038/s41598-019-56542-4
Shilling HG, McQueen KL, Cheng NW, Shizuru JA, Negrin RS, Parham P (2003) Reconstitution of NK cell receptor repertoire following HLA-matched hematopoietic cell transplantation. Blood 101:3730–3740. https://doi.org/10.1182/blood-2002-08-2568
Steinbichler TB, Dudas J, Riechelmann H, Skvortsova II (2017) The role of exosomes in cancer metastasis. Semin Cancer Biol 44:170–181. https://doi.org/10.1016/j.semcancer.2017.02.006
Tran HC et al (2017) TGFbetaR1 blockade with galunisertib (LY2157299) enhances anti-neuroblastoma activity of the anti-GD2 antibody dinutuximab (ch14.18) with natural killer cells. Clin Cancer Res 23:804–813. https://doi.org/10.1158/1078-0432.CCR-16-1743
Wu CH et al (2019) Extracellular vesicles derived from natural killer cells use multiple cytotoxic proteins and killing mechanisms to target cancer cells. J Extracell Vesicles 8:1588538. https://doi.org/10.1080/20013078.2019.1588538
Xie C, Du LY, Guo F, Li X, Cheng B (2019) Exosomes derived from microRNA-101-3p-overexpressing human bone marrow mesenchymal stem cells suppress oral cancer cell proliferation, invasion, and migration. Mol Cell Biochem 458:11–26. https://doi.org/10.1007/s11010-019-03526-7
Yang C, Yang H, Liu J, Zhu L, Yu S, Zhang X, Gao L (2019) Focus on exosomes: novel pathogenic components of leukemia. Am J Cancer Res 9:1815–1829
Zhao C, Du F, Zhao Y, Wang S, Qi L (2019) Acute myeloid leukemia cells secrete microRNA-4532-containing exosomes to mediate normal hematopoiesis in hematopoietic stem cells by activating the LDOC1-dependent STAT3 signaling pathway. Stem Cell Res Ther 10:384. https://doi.org/10.1186/s13287-019-1475-7
Funding
This work was supported by Science, Technology and Innovation Bureau of Bao’an District, Basic Research Project of Healthcare in Bao'an District (no. 2019JD450).
Author information
Authors and Affiliations
Contributions
Conceptualization and funding acquisition: JX. Data curation: HY, TH, DW, LC, and XL. Formal analysis: XL, KC, HH, SL, and YZ. Experimental studies: HY, TH, KC, HH, SL, and YZ. Software: DW, LC, XL, and XL. Writing—original draft and review and editing: all authors. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict on interests.
Rights and permissions
About this article
Cite this article
Yu, H., Huang, T., Wang, D. et al. Acute lymphoblastic leukemia-derived exosome inhibits cytotoxicity of natural killer cells by TGF-β signaling pathway. 3 Biotech 11, 313 (2021). https://doi.org/10.1007/s13205-021-02817-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s13205-021-02817-5