Abstract
Introduction
Pediatric exposures to cannabis edibles have been associated with serious adverse effects, such as respiratory depression. Yet, their incidence and relationship to exposure characteristics are not well defined. We attempt to describe the temporal, demographic, and clinical characteristics of pediatric patients with edible cannabis exposures and examine the relationship between these characteristics and two clinical outcomes: need for respiratory support and hospital admission.
Methods
A retrospective chart review was conducted at a single, tertiary care academic medical center covering a 28-month period. Inclusion criteria were: evaluation in the ED, age <18 years at the time of presentation, and physician documented exposure to edible cannabis. Exclusion criteria were: known or suspected co-ingestion of other substances.
Results
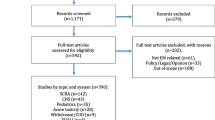
Thirty-two cases of edible cannabis ingestions were identified. Age <10 years was associated with bradypnea, hypertension, hospital admission, and respiratory support. Use of respiratory support was significantly associated with the presence of lethargy, bradypnea, hypercarbia, seizure, and hypertension. There was a five-fold increase in the number of pediatric edible cannabis exposures after recreational cannabis dispensaries opened in Massachusetts. Five patients (16%) required respiratory support and eleven (34%) required hospital admission.
Conclusions
There was a low incidence of need for respiratory support in our population, but hospital admission was more common. Severe symptoms (including lethargy and respiratory depression), need for respiratory support and hospital admission were more frequent in younger children. Exposures occurred with increasing frequency over time. Larger studies are needed to explore the relationship between THC dosage, age, and incidence of adverse outcomes.


Similar content being viewed by others
References
Legislatures NCoS. State Medical Marijuana Laws [Available from: https://www.ncsl.org/research/health/state-medical-marijuana-laws.aspx.
Thomas AA, Dickerson-Young T, Mazor S. Unintentional pediatric marijuana exposures at a Tertiary Care Children’s Hospital in Washington State: a retrospective review. Pediatr Emerg Care. 2018, Publish Ahead of Print.
Whitehill JM, Harrington C, Lang CJ, Chary M, Bhutta WA, Burns MM. Incidence of pediatric cannabis exposure among children and teenagers aged 0 to 19 years before and after medical marijuana legalization in Massachusetts. JAMA Netw Open. 2019;2(8):e199456.
Wang GS, Le Lait MC, Deakyne SJ, Bronstein AC, Bajaj L, Roosevelt G. Unintentional pediatric exposures to marijuana in Colorado, 2009-2015. JAMA Pediatr. 2016;170(9):e160971.
Wang GS, Roosevelt G, Le Lait MC, Martinez EM, Bucher-Bartelson B, Bronstein AC, et al. Association of unintentional pediatric exposures with decriminalization of marijuana in the United States. Ann Emerg Med. 2014;63(6):684–9.
Graham J, Leonard J, Banerji S, Wang GS. Illicit drug exposures in young pediatric patients reported to the National Poison Data System, 2006-2016. J Pediatr. 2020.
Wang GS, Davies SD, Halmo LS, Sass A, Mistry RD. Impact of marijuana legalization in Colorado on adolescent emergency and urgent care visits. J Adolesc Health. 2018;63(2):239–41.
Cao D, Srisuma S, Bronstein AC, Hoyte CO. Characterization of edible marijuana product exposures reported to United States poison centers. Clin Toxicol (Phila). 2016;54(9):840–6.
Wang GS. Pediatric concerns due to expanded cannabis use: unintended consequences of legalization. J Med Toxicol. 2017;13(1):99–105.
Wang GS, Banerji S, Contreras AE, Hall KE. Marijuana exposures in Colorado, reported to regional poison centre, 2000-2018. Inj Prev. 2019.
Wong KU, Baum CR. Acute cannabis toxicity. Pediatr Emerg Care. 2019;35(11):799–804.
Association APH. Cannabis policies in four states [Available from: https://www.apha.org/-/media/Files/PDF/topics/State_Cannabis_Policy.ashx.
Richards JR, Smith NE, Moulin AK. Unintentional cannabis ingestion in children: a systematic review. J Pediatr. 2017;190:142–52.
Thomas AA, Mazor S. Unintentional marijuana exposure presenting as altered mental status in the pediatric emergency department: a case series. J Emerg Med. 2017;53(6):e119–e23.
Wang GS, Roosevelt G, Heard K. Pediatric marijuana exposures in a medical marijuana state. JAMA Pediatr. 2013;167(7):630–3.
Lapoint J. Cannabinoids. In: Hoffman R, Howland, M, Lwein, N, Nelson, L, Goldfrank, L, editor. Goldfrank’s Toxicologic Emergencies. 10 ed: McGraw Hill Professional 2014.
Claudet I, Le Breton M, Brehin C, Franchitto N. A 10-year review of cannabis exposure in children under 3-years of age: do we need a more global approach? Eur J Pediatr. 2017;176(4):553–6.
Le Garrec S, Dauger S, Sachs P. Cannabis poisoning in children. Intensive Care Med. 2014;40(9):1394–5.
Heizer JW, Borgelt LM, Bashqoy F, Wang GS, Reiter PD. Marijuana misadventures in children: exploration of a dose-response relationship and summary of clinical effects and outcomes. Pediatr Emerg Care. 2018;34(7):457–62.
Marx GE, Chen Y, Askenazi M, Albanese BA. Syndromic surveillance of emergency department visits for acute adverse effects of marijuana, Tri-County Health Department, Colorado, 2016-2017. Public Health Rep. 2019;134(2):132–40.
Kliegman RM. Nelson textbook of pediatrics. 21st edition. ed. Philadelphia, MO: Elsevier; 2019. pages cm p.
Goodwin RD, Cheslack-Postava K, Santoscoy S, Bakoyiannis N, Hasin DS, Collins BN, et al. Trends in cannabis and cigarette use among parents with children at home: 2002 to 2015. Pediatrics. 2018;141(6).
Dharmapuri S, Miller K, Klein JD. Marijuana and the pediatric population. Pediatrics. 2020;146(2).
Ashton CH. Pharmacology and effects of cannabis: a brief review. Br J Psychiatry. 2001;178:101–6.
Commonwealth of Massachusetts Cannabis Control Commission 935 CMR 500.150: Adult Use of Marijuana, Edibles, (2021).
Acknowledgements
The authors would like to acknowledge Catherine W. Carr, MLIS, AHIP, for her contribution as education clinical services librarian.
Funding
Dr. Carreiro is funded by NIH/NIDA (K23DA045242).
Author information
Authors and Affiliations
Contributions
Dr. Kaczor conceptualized and designed the study, designed the data collection instruments, collected and organized the data, interpreted the results, and reviewed and revised the manuscript.
Dr. Mathews participated in study design, drafted the initial manuscript, interpreted the results, and reviewed and revised the manuscript.
Dr. LaBarge participated in study design, performed data extraction, interpreted the results, and reviewed and revised the manuscript.
Ms. Chapman participated in study design, designed the data collection instruments, interpreted the results, and reviewed and revised the manuscript.
Dr. Carreiro participated in study conceptualization and design, carried out statistical analysis of the data, interpreted the results, and reviewed and revised the manuscript.
All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflict of Interest
None.
Additional information
Supervising Editor: Trevonne M. Thompson, MD
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Previous Presentations: Abstract accepted to the 2021 American College of Medical Toxicology Annual Scientific Meeting
Supplementary Information
ESM 1
(DOCX 33.6 kb)
Rights and permissions
About this article
Cite this article
Kaczor, E.E., Mathews, B., LaBarge, K. et al. Cannabis Product Ingestions in Pediatric Patients: Ranges of Exposure, Effects, and Outcomes. J. Med. Toxicol. 17, 386–396 (2021). https://doi.org/10.1007/s13181-021-00849-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13181-021-00849-0