Abstract
Introduction
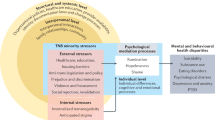
Transgender and non-binary (TNB) individuals are at severe risk of adverse mental health outcomes. Transitioning is associated with marked improvements in mental health. Unfortunately, a significant proportion of TNB individuals experience challenges to fully transitioning. In this paper, we examine the mental health status of TNB individuals who have partially transitioned and have expressed a desire to live fully in a gender different from the one assigned at birth and the barriers deterring them from doing so.
Methods
Using the 2015 US Transgender Survey, we estimated generalized ordered logistic models to predict psychological distress using barriers to transitioning as main predictors and accounting for relevant covariates for a subsample of 9242 TNB adults.
Results
Individuals that list structural barriers to transition such as fearing not receiving needed medical care, becoming homeless, and facing violence were significantly more likely to be in moderate and severe, and severe distress compared to individuals who did not report those barriers.
Conclusions
These findings demonstrate the structural nature of barriers to fully transitioning for transgender adults. Although some interpersonal fears were significant, the majority of concerns associated with psychological distress are structural in nature and speak to the institutional barriers TNB people face during the transition process.
Policy Implications
These structural barriers could be ameliorated through social policy in which transgender individuals could access services and are afforded protections to allow for a transition without the fear of negative consequences.
Similar content being viewed by others
Data Availability
Restricted data access was granted by the Inter-university Consortium for Political and Social Research (ICPSR) at the University of Michigan where the 2015 USTS is archived (James, SE, Herman, J, Keisling, M, Mottet, L, and Anafi, M. U.S. Transgender Survey USTS; Inter-university Consortium for Political and Social Research [distributor], 2019) (https://doi.org/10.3886/ICPSR37229.v1).
Code Availability
Stata 17 do-file is available by request.
References
Ainsworth, T. A., & Spiegel, J. H. (2010). Quality of life of individuals with and without facial feminization surgery or gender reassignment surgery. Quality of Life Research, 19(7), 1019–1024. https://doi.org/10.1007/s11136-010-9668-7
Almazan, A. N., & Keuroghlian, A. S. (2021). Association between gender-affirming surgeries and mental health outcomes. JAMA Surgery, 156(7), 611–618. http://jamanetwork.com/article.aspx?doi=10.1001/jamasurg.2021.0952
Bennett, D. A. (2001). How can I deal with missing data in my study? Australian and New Zealand Journal of Public Health, 25(2), 464–469.
Bethea, M. S., & McCollum, E. E. (2013). The disclosure experiences of male-to-female transgender individuals: a systems theory perspective. Journal of Couple & Relationship Therapy, 12(2), 89–112. https://doi.org/10.1080/15332691.2013.779094
Brumbaugh-Johnson, S. M., & Hull, K. E. (2019). Coming out as transgender: navigating the social implications of a transgender identity. Journal of Homosexuality, 66(8), 1148–1177. https://doi.org/10.1080/00918369.2018.1493253
Budge, S. L., Adelson, J. L., & Howard, K. A. S. (2013). Anxiety and depression in transgender individuals: the roles of transition status, loss, social support, and coping. Journal of Consulting and Clinical Psychology, 81(3), 545–557. https://doi.org/10.1037/a0031774
Cavanaugh, G., & Ladd, L. (2017). “I want to be who I am”: narratives of transgender persons. Journal of LGBT Issues in Counseling, 11(3), 156–173. https://doi.org/10.1080/15538605.2017.1346493
Clements-Nolle, K., Marx, R., & Katz, M. (2006). Attempted suicide among transgender persons: the influence of gender-based discrimination and victimization. Journal of Homosexuality, 51(3), 53–69. https://doi.org/10.1300/j082v51n03_04
Clifford, C., & Orford, J. (2007). The experience of social power in the lives of trans people. In V. Clarke & E. Peel (Eds.), Out in psychology: lesbian, gay, bisexual, trans and queer perspectives (pp. 195–216). John Wiley & Sons.
Cramer, R. J., Kaniuka, A. R., Yada, F. N., Diaz-Garelli, F., Hill, R. M., Bowling, J., Macchia, J. M., & Tucker, R. P. (2022). An analysis of suicidal thoughts and behaviors among transgender and gender diverse adults. Social Psychiatry and Psychiatric Epidemiology, 57(1), 195–205. https://doi.org/10.1007/s00127-021-02115-8
Dargie, E., Blair, K. L., Pukall, C. F., & Coyle, S. M. (2014). Somewhere under the rainbow: exploring the identities and experiences of trans persons. The Canadian Journal of Human Sexuality, 23(2), 60–74. https://doi.org/10.3138/cjhs.2378
De Vries, K.M. (2012). Intersectional identities and conceptions of the self: the experience of transgender people. Symbolic Interaction, 35(1), 49–67. https://www.jstor.org/stable/symbinte.35.1.49
Ellis, S. J., McNeil, J., & Bailey, L. (2014). Gender, stage of transition and situational avoidance: a UK study of trans people’s experiences. Sexual and Relationship Therapy, 29(3), 351–364. https://doi.org/10.1080/14681994.2014.902925
Fein, L. A., Salgado, C. J., Alvarez, C. V., & Estes, C. M. (2017). Transitioning transgender: investigating the important aspects of the transition: A brief report. International Journal of Sexual Health, 29(1), 80–88. https://doi.org/10.1080/19317611.2016.1227013
Fontanari, A. M. V., Vilanova, F., Schneider, M. A., Chinazzo, I., Soll, B. M., Schwarz, K., Rodrigues Lobato, M. I., & Brandelli Costa, A. (2020). Gender affirmation is associated with transgender and gender nonbinary youth mental health improvement. LGBT Health, 7(5), 237–247. https://doi.org/10.1089/lgbt.2019.0046
Fredriksen-Goldsen, K. I., Cook-Daniels, L., Kim, H. J., Erosheva, E. A., Emlet, C. A., Hoy-Ellis, C. P., Goldsen, J., & Muraco, A. (2014). Physical and mental health of transgender older adults: an at-risk and underserved population. The Gerontologist, 54(3), 488–500. https://doi.org/10.1093/geront/gnt021
Glick, J. L., Lopez, A., Pollock, M., & Theall, K. P. (2019). “Housing insecurity seems to almost go hand in hand with being trans”: housing stress among transgender and gender non-conforming individuals in New Orleans. Journal of Urban Health, 96(5), 751–759. https://doi.org/10.1007/s11524-019-00384-y
Glick, J. L., Lopez, A., Pollock, M., & Theall, K. P. (2020). Housing insecurity and intersecting social determinants of health among transgender people in the USA: a targeted ethnography. International Journal of Transgender Health, 21(3), 337–349. https://doi.org/10.1080/26895269.2020.1780661
Guittar, N. A., & Rayburn, R. L. (2016). Coming out: the career management of one’s sexuality. Sexuality & Culture, 20(2), 336–357. https://doi.org/10.1007/s12119-015-9325-y
Haas, A. P., Eliason, M., Mays, V. M., Mathy, R. M., Cochran, S. D., D’Augelli, A. R., Silverman, M. M., Fisher, P. W., Hughes, T., Rosario, M., Russell, S. T., Malley, E., Reed, J., Litts, D. A., Haller, E., Sell, R. L., Remafedi, G., Bradford, J., Beautrais, A. L., & …& Clayton, P. J. (2010). Suicide and suicide risk in lesbian, gay, bisexual, and transgender populations: review and recommendations. Journal of Homosexuality, 58(1), 10–51. https://doi.org/10.1080/00918369.2011.534038
Haas, A. P., Rodgers, P. L., & Herman, J.L. (2014). Suicide attempts among transgender and gender non-conforming adults. Williams Institute. https://williamsinstitute.law.ucla.edu/wp-content/uploads/Trans-GNC-Suicide-Attempts-Jan-2014.pdf
Herman, J. L., Brown, T. N., Haas, A.P. (2019). Suicide thoughts and attempts among transgender adults: findings from the 2015 US Transgender Survey. Williams Institute. https://williamsinstitute.law.ucla.edu/wp-content/uploads/Suicidality-Transgender-Sep-2019.pdf
James, S. E., Herman, J. L., Rankin, S., Keisling, M., Mottet, L., & Anafi, M. (2016). The report of the 2015 U.S. Transgender Survey executive summary. National Center for Transgender Equality. https://transequality.org/sites/default/files/docs/usts/USTS-Executive-Summary-Dec17.pdf
James, SE, Herman, J, Keisling, M, Mottet, L, and Anafi, M. (2019). 2015 U.S. Transgender Survey (USTS). Inter-university Consortium for Political and Social Research [distributor]. https://doi.org/10.3886/ICPSR37229.v1
Keo-Meier, C., Fitzgerald, K. M., Pardo, S. T., & Babcock, J. (2011). The effects of hormonal gender affirmation treatment on mental health in female-to-male transsexuals. Journal of Gay & Lesbian Mental Health, 15(3), 281–299. https://doi.org/10.1080/19359705.2011.581195
Kessler, R. C., Andrews, G., Colpe, L. J., Hiripi, E., Mroczek, D. K., Normand, S. L., Walters, E. E., & Zaslavsky, A. M. (2002). Short screening scales to monitor population prevalences and trends in non-specific psychological distress. Psychological Medicine, 32(6), 959–976. https://doi.org/10.1017/s0033291702006074
Kessler, R. C., Barker, P. R., Colpe, L. J., Epstein, J. F., Gfroerer, J. C., Hiripi, E., Howes, M. J., Normand, S. L. T., Manderscheid, R. W., Walters, E. E., & Zaslavsky, A. M. (2003). Screening for serious mental illness in the general population. Archives of General Psychiatry, 60(2), 184–189
Kim, G., DeCoster, J., Bryant, A. N., & Ford, K. L. (2016). Measurement equivalence of the K6 scale: the effects of race/ethnicity and language. Assessment, 23(6), 758–768. https://doi.org/10.1177/1073191115599639
Klein, A., & Golub, S. A. (2016). Family rejection as a predictor of suicide attempts and substance misuse among transgender and gender nonconforming adults. LGBT Health, 3(3), 193–199. https://doi.org/10.1089/lgbt.2015.0111
Koch, J. M., McLachlan, C. T., Victor, C. J., Westcott, J., & Yager, C. (2020). The cost of being transgender: where socio-economic status, global health care systems, and gender identity intersect. Psychology & Sexuality, 11(1–2), 103–119. https://doi.org/10.1080/19419899.2019.1660705
Kuper, L. E., Wright, L., & Mustanski, B. (2018). Gender identity development among transgender and gender nonconforming emerging adults: an intersectional approach. International Journal of Transgenderism, 19(4), 436–455. https://doi.org/10.1080/15532739.2018.1443869
Lev, A. I. (2006). Transgender Emergence within Families. In D. F. Morrow & L. Messinger (Eds.), Sexual orientation & gender expression in social work practice: working with gay, lesbian, bisexual, & transgender people (pp. 263–283). Columbia University Press.
Maguen, S., Shipherd, J. C., Harris, H. N., & Welch, L. P. (2007). Prevalence and predictors of disclosure of transgender identity. International Journal of Sexual Health, 19(1), 3–13. https://doi.org/10.1300/J514v19n01_02
Marquez-Velarde, G., Miller, G. H., Shircliff, J. E., & Suárez, M. I. (2022). The impact of family support and rejection on suicide ideation and attempt among transgender adults in the U.S. Unpublished manuscript.
Meyer, I. H. (1995). Minority stress and mental health in gay men. Journal of Health and Social Behavior, 36(1), 38–56. https://pubmed.ncbi.nlm.nih.gov/7738327/
Meyer, I. H. (2003). Prejudice, social stress, and mental health in lesbian, gay, and bisexual populations: conceptual issues and research evidence. Psychological Bulletin, 129(5), 674–697. https://doi.org/10.1037/0033-2909.129.5.674
Meyer, I. H., Schwartz, S., & Frost, D. M. (2008). Social patterning of stress and coping: does disadvantaged social statuses confer more stress and fewer coping resources? Social Science & Medicine, 67(3), 368–379. https://doi.org/10.1016/j.socscimed.2008.03.012
Miller, G. H., Marquez-Velarde, G., Suárez, M. I., & Glass, C. (2022). Support saves lives: Exploring the relationship between stage of transition, social support, and retrospective K-12 educational experiences in transgender suicidality. Unpublished manuscript.
Moody, C., & Smith, N. G. (2013). Suicide protective factors among trans adults. Archives of Sexual Behavior, 42(5), 739–752. https://doi.org/10.1007/s10508-013-0099-8
Mustanski, B., Andrews, R., & Puckett, J. A. (2016). The effects of cumulative victimization on mental health among lesbian, gay, bisexual, and transgender adolescents and young adults. American Journal of Public Health, 106(3), 527–533. https://doi.org/10.2105/AJPH.2015.302976
Olson, K. R., Durwood, L., DeMeules, M., & McLaughlin, K. A. (2016). Mental health of transgender children who are supported in their identities. Pediatrics, 137(3), e20153223. https://doi.org/10.1542/peds.2015-3223
Olson-Kennedy, J., Chan, Y. M., Garofalo, R., Spack, N., Chen, D., Clark, L., Ehrensaft, D., Hidalgo, M., Tishelman, A., & Rosenthal, S. (2019). Impact of early medical treatment for transgender youth: protocol for the longitudinal, observational trans youth care study. JMIR Research Protocols, 8(7), e14434. https://doi.org/10.2196/14434
Orne, J. (2011). You will always have to ‘out’ yourself: reconsidering coming out through strategic outness. Sexualities, 14(6), 681–703. https://doi.org/10.1177/1363460711420462
Pitts, M.K., Couch, M., Mulcare, H., Croy, S., & Mitchell, A. (2009). Transgender people in Australia and New Zealand: Health, well-being and access to health services. Feminism & Psychology, 19, 475–495. https://doi.org/10.1177/0959353509342771
Prochaska, J. J., Sung, H. Y., Max, W., Shi, Y., & Ong, M. (2012). Validity study of the K6 scale as a measure of moderate mental distress based on mental health treatment need and utilization. International Journal of Methods in Psychiatric Research, 21(2), 88–97. https://doi.org/10.1002/mpr.1349
Pusch, R. S. (2005). Objects of curiosity: Transgender college students’ perceptions of the reactions of others. Journal of Gay & Lesbian Issues in Education, 3(1), 45–61. https://doi.org/10.1300/J367v03n01_06
Rudin, J., Ruane, S., Ross, L., Farro, A., & Billing, T. (2014). Hostile territory: Employers’ unwillingness to accommodate transgender employees. Equality, Diversity and Inclusion: An International Journal. https://doi.org/10.1108/EDI-12-2013-0116
Russomanno, J., Patterson, J. G., & Jabson, J. M. (2019). Food insecurity among transgender and gender nonconforming individuals in the Southeast United States: a qualitative study. Transgender Health, 4(1), 89–99. https://doi.org/10.1089/trgh.2018.0024
Russomanno, J., & Tree, J. M. J. (2020). Food insecurity and food pantry use among transgender and gender non-conforming people in the Southeast United States. BMC Public Health, 20(1), 1–11. https://doi.org/10.1186/s12889-020-08684-8
Shelton, J., & Bond, L. (2017). “It just never worked out”: how transgender and gender expansive youth understand their pathways into homelessness. Families in Society, 98(4), 284–291. https://doi.org/10.1606/1044-3894.2017.98.33
Simons, L., Schrager, S. M., Clark, L. F., Belzer, M., & Olson, J. (2013). Parental support and mental health among transgender adolescents. Journal of Adolescent Health, 53(6), 791–793.
Speer, S. A., & Green, R. (2007). On passing: the interactional organization of appearance attributions in the psychiatric assessment of transsexual patients. In V. Clarke & E. Peel (Eds.), Out in psychology: lesbian, gay, bisexual, trans and queer perspectives (pp. 335–368). John Wiley & Sons. https://doi.org/10.1002/9780470713099.ch16
StataCorp. (2021). Stata Statistical Software (Release 17). StataCorp LLC
Stotzer, R. (2009). Violence against transgender people: a review of United States data. Aggression and Violent Behavior, 14(3), 170–179. https://doi.org/10.1016/j.avb.2009.01.006
Suárez, M. I., Marquez-Velarde, G., Glass, C., & Miller, G. H. (2022). Cis-normativity at work: Exploring discrimination against US trans workers. Gender in Management, 37(6), 16–731. https://doi.org/10.1108/GM-06-2020-0201
Swan, J., Phillips, T. M., Sanders, T., Mullens, A. B., Debattista, J., & Brömdal, A. (2021). Mental health and quality of life outcomes of gender-affirming surgery: a systematic literature review. Journal of Gay & Lesbian Mental Health. https://doi.org/10.1080/19359705.2021.2016537
Tomita, K. K., Testa, R. J., & Balsam, K. F. (2019). Gender-affirming medical interventions and mental health in transgender adults. Psychology of Sexual Orientation and Gender Diversity, 6(2), 182–193. https://doi.org/10.1037/sgd0000316
White Hughto, J. M., Gunn, H. A., Rood, B. A., & Pantalone, D. W. (2020). Social and medical gender affirmation experiences are inversely associated with mental health problems in a U.S. non-probability sample of transgender adults. Archives of Sexual Behavior, 49(7), 2635–2647.
White Hughto, J. M., Rose, A. J., Pachankis, J. E., & Reisner, S. L. (2017). Barriers to gender transition-related healthcare: Identifying underserved transgender adults in Massachusetts. Transgender Health, 2(1), 107–118. https://doi.org/10.1089/trgh.2017.0014
Williams, R. (2006). Generalized ordered logit/partial proportional odds models for ordinal dependent variables. The Stata Journal, 6(1), 58–82. https://doi.org/10.1177/1536867X0600600104
Williams, R. (2016). Understanding and interpreting generalized ordered logit models. The Journal of Mathematical Sociology, 40(1), 7–20. https://doi.org/10.1080/0022250X.2015.1112384
Acknowledgements
We acknowledge Dr. Mario I. Suárez for his assistance during the data acquisition process.
Funding
This manuscript was completed during GMV’s Career Enhancement Fellowship year with the Institute for Citizens and Scholars (formerly Woodrow Wilson National Fellowship Foundation). GHM is a scholar in the Health Equity Scholars for Action program, supported by the Robert Wood Johnson Foundation. The program exists to challenge biases and conventions in research and academia to be more equitable by funding and supporting early-career researchers from historically underrepresented backgrounds.
Biosocial Research Training, T32 HD091058, Stephanie M. Hernandez, Population Research Infrastructure Program, P2C HD050924, Stephanie M. Hernandez
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Data analyses were performed by GMV. The first draft of the manuscript was written by GMV, GHM, SMH, and MM. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Marquez-Velarde, G., Miller, G.H., Hernandez, S.M. et al. Partial Transition and Mental Health: Barriers to a Full Transition. Sex Res Soc Policy 21, 436–445 (2024). https://doi.org/10.1007/s13178-023-00837-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13178-023-00837-9