Abstract
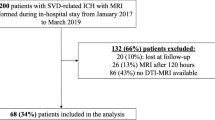
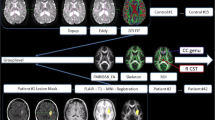
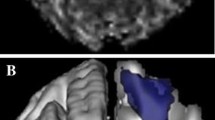
Chronic white matter structural injury is a risk factor for poor long-term outcomes after acute ischemic stroke (AIS). However, it is unclear how white matter structural injury predisposes to poor outcomes after AIS. To explore this question, in 42 AIS patients with moderate to severe white matter hyperintensity (WMH) burden, we characterized WMH and normal-appearing white matter (NAWM) diffusivity anisotropy metrics in the hemisphere contralateral to acute ischemia in relation to ischemic tissue and early functional outcomes. All patients underwent brain MRI with dynamic susceptibility contrast perfusion and diffusion tensor imaging within 12 h and at day 3–5 post stroke. Early neurological outcomes were measured as the change in NIH Stroke Scale score from admission to day 3–5 post stroke. Target mismatch profile, percent mismatch lost, infarct growth, and rates of good perfusion were measured to assess ischemic tissue outcomes. NAWM mean diffusivity was significantly lower in the group with early neurological improvement (ENI, 0.79 vs. 0.82 × 10−3, mm2/s; P = 0.02). In multivariable logistic regression, NAWM mean diffusivity was an independent radiographic predictor of ENI (β = − 17.6, P = 0.037). Median infarct growth was 118% (IQR 26.8–221.9%) despite good reperfusion being observed in 65.6% of the cohort. NAWM and WMH diffusivity metrics were not associated with target mismatch profile, percent mismatch lost, or infarct growth. Our results suggest that, in AIS patients, white matter structural integrity is associated with poor early neurological outcomes independent of ischemic tissue outcomes.
Similar content being viewed by others
References
Wardlaw JM, Smith C, Dichgans M. Mechanisms of sporadic cerebral small vessel disease: insights from neuroimaging. Lancet Neurol. 2013;12(5):483–97. https://doi.org/10.1016/S1474-4422(13)70060-7.
Onteddu SR, Goddeau RP Jr, Minaeian A, Henninger N. Clinical impact of leukoaraiosis burden and chronological age on neurological deficit recovery and 90-day outcome after minor ischemic stroke. J Neurol Sci. 2015;359(1–2):418–23. https://doi.org/10.1016/j.jns.2015.10.005.
Giurgiutiu DV, Yoo AJ, Fitzpatrick K, Chaudhry Z, Leslie-Mazwi T, Schwamm LH, et al. Severity of leukoaraiosis, leptomeningeal collaterals, and clinical outcomes after intra-arterial therapy in patients with acute ischemic stroke. J Neurointerv Surg. 2015;7(5):326–30. https://doi.org/10.1136/neurintsurg-2013-011083.
Arsava EM, Rahman R, Rosand J, Lu J, Smith EE, Rost NS, et al. Severity of leukoaraiosis correlates with clinical outcome after ischemic stroke. Neurology. 2009;72(16):1403–10. https://doi.org/10.1212/WNL.0b013e3181a18823.
Etherton MR, Wu O, Cougo P, Giese AK, Cloonan L, Fitzpatrick KM, et al. Integrity of normal-appearing white matter and functional outcomes after acute ischemic stroke. Neurology. 2017;88(18):1701–8. https://doi.org/10.1212/WNL.0000000000003890.
Rost NS, Cougo P, Lorenzano S, Li H, Cloonan L, Bouts MJ, et al. Diffuse microvascular dysfunction and loss of white matter integrity predict poor outcomes in patients with acute ischemic stroke. J Cereb Blood Flow Metab. 2017. https://doi.org/10.1177/0271678X17706449.
Ay H, Arsava EM, Rosand J, Furie KL, Singhal AB, Schaefer PW, et al. Severity of leukoaraiosis and susceptibility to infarct growth in acute stroke. Stroke. 2008;39(5):1409–13. https://doi.org/10.1161/STROKEAHA.107.501932.
Nam KW, Lim JS, Kang DW, Lee YS, Han MK, Kwon HM. Severe white matter hyperintensity is associated with early neurological deterioration in patients with isolated pontine infarction. Eur Neurol. 2016;76(3–4):117–22. https://doi.org/10.1159/000448888.
Feng C, Tan Y, Wu YF, Xu Y, Hua T, Huang J, et al. Leukoaraiosis correlates with the neurologic deterioration after small subcortical infarction. J Stroke Cerebrovasc Dis. 2014;23(6):1513–8. https://doi.org/10.1016/j.jstrokecerebrovasdis.2013.12.032.
Espeland MA, Erickson K, Neiberg RH, Jakicic JM, Wadden TA, Wing RR, et al. Brain and white matter hyperintensity volumes after 10 years of random assignment to lifestyle intervention. Diabetes Care. 2016;39(5):764–71. https://doi.org/10.2337/dc15-2230.
Sajobi TT, Menon BK, Wang M, Lawal O, Shuaib A, Williams D, et al. Early trajectory of stroke severity predicts long-term functional outcomes in ischemic stroke subjects: results from the ESCAPE trial (endovascular treatment for small core and anterior circulation proximal occlusion with emphasis on minimizing CT to recanalization times). Stroke. 2017;48(1):105–10. https://doi.org/10.1161/STROKEAHA.116.014456.
Fazekas F, Barkhof F, Wahlund LO, Pantoni L, Erkinjuntti T, Scheltens P, et al. CT and MRI rating of white matter lesions. Cerebrovasc Dis. 2002;13(Suppl 2):31–6.
Adams HP Jr, Bendixen BH, Kappelle LJ, Biller J, Love BB, Gordon DL, et al. Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke. 1993;24(1):35–41.
Sorensen AG, Wu O, Copen WA, Davis TL, Gonzalez RG, Koroshetz WJ, et al. Human acute cerebral ischemia: detection of changes in water diffusion anisotropy by using MR imaging. Radiology. 1999;212(3):785–92. https://doi.org/10.1148/radiology.212.3.r99se24785.
Wu O, Ostergaard L, Weisskoff RM, Benner T, Rosen BR, Sorensen AG. Tracer arrival timing-insensitive technique for estimating flow in MR perfusion-weighted imaging using singular value decomposition with a block-circulant deconvolution matrix. Magn Reson Med. 2003;50(1):164–74. https://doi.org/10.1002/mrm.10522.
Boxerman JL, Schmainda KM, Weisskoff RM. Relative cerebral blood volume maps corrected for contrast agent extravasation significantly correlate with glioma tumor grade, whereas uncorrected maps do not. AJNR Am J Neuroradiol. 2006;27(4):859–67.
Rost NS, Sadaghiani S, Biffi A, Fitzpatrick KM, Cloonan L, Rosand J, et al. Setting a gold standard for quantification of leukoaraiosis burden in patients with ischemic stroke: the Atherosclerosis Risk in Communities Study. J Neurosci Methods. 2014;221:196–201. https://doi.org/10.1016/j.jneumeth.2013.10.009.
Ferguson KJ, Wardlaw JM, Edmond CL, Deary IJ, Maclullich AM. Intracranial area: a validated method for estimating intracranial volume. J Neuroimaging. 2005;15(1):76–8. https://doi.org/10.1177/1051228404270243.
Lansberg MG, Straka M, Kemp S, Mlynash M, Wechsler LR, Jovin TG, et al. MRI profile and response to endovascular reperfusion after stroke (DEFUSE 2): a prospective cohort study. Lancet Neurol. 2012;11(10):860–7. https://doi.org/10.1016/S1474-4422(12)70203-X.
Collins DL, Neelin P, Peters TM, Evans AC. Automatic 3D intersubject registration of MR volumetric data in standardized Talairach space. J Comput Assist Tomogr. 1994;18(2):192–205.
Mori S, Oishi K, Jiang H, Jiang L, Li X, Akhter K, et al. Stereotaxic white matter atlas based on diffusion tensor imaging in an ICBM template. NeuroImage. 2008;40(2):570–82. https://doi.org/10.1016/j.neuroimage.2007.12.035.
Mazziotta J, Toga A, Evans A, Fox P, Lancaster J, Zilles K, et al. A probabilistic atlas and reference system for the human brain: International Consortium for Brain Mapping (ICBM). Philos Trans R Soc Lond Ser B Biol Sci. 2001;356(1412):1293–322. https://doi.org/10.1098/rstb.2001.0915.
McConnell Brain Imaging Centre. BIC - The McConnell Brain Imaging Centre: home page. 2015. 2006.
Basser PJ, Jones DK. Diffusion-tensor MRI: theory, experimental design and data analysis - a technical review. NMR Biomed. 2002;15(7–8):456–67. https://doi.org/10.1002/nbm.783.
Wardlaw JM, Valdes Hernandez MC, Munoz-Maniega S. What are white matter hyperintensities made of? Relevance to vascular cognitive impairment. J Am Heart Assoc. 2015;4(6):001140. https://doi.org/10.1161/JAHA.114.001140.
O'Sullivan M, Lythgoe DJ, Pereira AC, Summers PE, Jarosz JM, Williams SC, et al. Patterns of cerebral blood flow reduction in patients with ischemic leukoaraiosis. Neurology. 2002;59(3):321–6.
Sam K, Crawley AP, Conklin J, Poublanc J, Sobczyk O, Mandell DM, et al. Development of white matter hyperintensity is preceded by reduced cerebrovascular reactivity. Ann Neurol. 2016;80(2):277–85. https://doi.org/10.1002/ana.24712.
Henninger N, Lin E, Baker SP, Wakhloo AK, Takhtani D, Moonis M. Leukoaraiosis predicts poor 90-day outcome after acute large cerebral artery occlusion. Cerebrovasc Dis. 2012;33(6):525–31. https://doi.org/10.1159/000337335.
Vos SB, Jones DK, Viergever MA, Leemans A. Partial volume effect as a hidden covariate in DTI analyses. NeuroImage. 2011;55(4):1566–76. https://doi.org/10.1016/j.neuroimage.2011.01.048.
Acknowledgements
This study is supported by the Statins Augment smalL Vessel function and improve stroke Outcomes (SALVO) study (NIH-NINDS 5R01NS082285).
Funding
The study was funded in part by the NIH-National Institute of Neurological Disorders and Stroke R01NS082285-01A1 (N.S.R.); National Institute of Biomedical Imaging and Bioengineering (P41EB015896); and American Heart Association 17CPOST33680102.
Author information
Authors and Affiliations
Contributions
Mark Etherton: study concept and design, acquisition of data, analysis and interpretation of data, drafting, and critical revision of the manuscript.
Ona Wu: study concept and design, analysis and interpretation of data, critical revision of the manuscript for intellectual content.
Anne-Katrin Giese: analysis and interpretation of data, critical revision of the manuscript for intellectual content.
Arne Lauer; acquisition of data, critical revision of the manuscript for intellectual content.
Gregoire Boulouis: acquisition of data, critical revision of the manuscript for intellectual content.
Brittany Mills: acquisition of data.
Lisa Cloonan: acquisition of data.
Kathleen L. Donahue: acquisition of data.
William Copen: study concept and design, critical revision of the manuscript for intellectual content.
Pamela Schaefer: study concept and design, critical revision of the manuscript for intellectual content.
Natalia S. Rost: study concept and design, analysis and interpretation of data, critical revision of the manuscript for intellectual content.
Corresponding author
Ethics declarations
Conflict of Interest
Mark R. Etherton is in part supported by the American Heart Association (17CPOST33680102). Ona Wu is in part supported by NIH Health (P50NS051343, R01NS082285, R01NS086905) and NIBIB (P41EB015896). Anne-Katrin Giese reports no disclosures. Arne Lauer reports no disclosures. Gregoire Boulouis reports no disclosures. Brittany Mills reports no disclosures. Lisa Cloonan reports no disclosures. Kathleen L. Donahue reports no disclosures. William Copen reports no disclosures. Pamela Schaefer reports no disclosures. Natalia S. Rost is in part supported by the NIH-NINDS R01NS082285 and R01NS086905.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Etherton, M.R., Wu, O., Giese, AK. et al. White Matter Integrity and Early Outcomes After Acute Ischemic Stroke. Transl. Stroke Res. 10, 630–638 (2019). https://doi.org/10.1007/s12975-019-0689-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12975-019-0689-4