Abstract
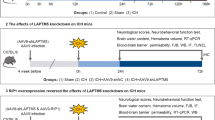
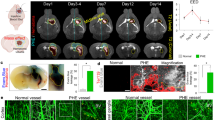
Cell death is a hallmark of secondary brain injury following intracerebral hemorrhage (ICH). The E3 ligase CHIP has been reported to play a key role in mediating necroptosis—an important mechanism of cell death after ICH. However, there is currently no evidence supporting a function of CHIP in ICH. In the present study, we aimed to determine whether CHIP plays an essential role in brain injury after ICH. Our findings indicated that CHIP expression was increased in the peri-hematomal area in rat models of ICH. The AAV/BBB viral platform enables non-invasive, widespread, and long-lasting global neural expression of target genes. Treatment with AAV/BBB-CHIP ameliorated brain injury and inhibited neuronal necroptosis and inflammation in wild type (WT) rats following ICH. Furthermore, rats with CHIP deficiency experienced severe brain injury and increased levels of neuronal necroptosis and inflammation relative to their WT counterparts. However, treatment with AAV/BBB-CHIP attenuated the effects of CHIP deficiency after ICH. Collectively, our results demonstrate that CHIP inhibits necroptosis and pathological inflammation following ICH, and that overexpression of CHIP may represent a therapeutic intervention for ICH. Moreover, the AAV/BBB viral platform may provide a novel avenue for the treatment of brain injury.







Similar content being viewed by others
Abbreviations
- ICH:
-
intracerebral hemorrhage
- CHIP:
-
carboxyl terminus of Hsp70-interacting protein
- WT:
-
wild type
- RIPK1:
-
receptor interacting protein kinase 1
- RIPK3:
-
receptor interacting protein kinase 3
- MLKL:
-
mixed lineage kinase domain-like pseudokinase
- PBS:
-
phosphate-buffered saline
- BBB:
-
blood–brain barrier
- AAV:
-
adeno-associated virus
- PI:
-
propidium iodide
- TUNEL:
-
transferase-mediated deoxyuridine triphosphate-biotin nick-end labeling
- H&E:
-
hematoxylin-eosin staining
- ELISA:
-
enzyme-linked immunosorbent assay
- IL-1β:
-
interleukin-1 beta
- IL-6:
-
interleukin-6
- TNF-α:
-
tumor necrosis factor alpha
- NF-κB:
-
nuclear factor “kappa-light-chain-enhancer” of activated B cells
References
Feigin VL, Lawes CM, Bennett DA, et al. Worldwide stroke incidence and early case fatality reported in 56 population-based studies: a systematic review. Lancet Neurol. 2009;8:355–69.
Sacco S, Marini C, Toni D, Olivieri L, Carolei A. Incidence and 10-year survival of intracerebral hemorrhage in a population-based registry. Stroke. 2009;40:394–9.
Balami JS, Buchan AM. Complications of intracerebral haemorrhage. Lancet Neurol. 2012;11:101–18.
Qureshi AI, Mendelow AD, Hanley DF. Intracerebral haemorrhage. Lancet. 2009;373:1632–44.
Aronowski J, Zhao X. Molecular pathophysiology of cerebral hemorrhage: secondary brain injury. Stroke. 2011;42:1781–6.
Liang X, Chen Y, Zhang L, et al. Necroptosis, a novel form of caspase-independent cell death, contributes to renal epithelial cell damage in an ATP-depleted renal ischemia model. Mol Med Rep. 2014;10:719–24.
Degterev A, Huang Z, Boyce M, Li Y, Jagtap P, Mizushima N, et al. Chemical inhibitor of nonapoptotic cell death with therapeutic potential for ischemic brain injury. Nat Chem Biol. 2005;1:112–9.
Vanden Berghe T, Grootjans S, Goossens V, et al. Determination of apoptotic and necrotic cell death in vitro and in vivo. Methods. 2013;61:117–29.
Galluzzi L, Kepp O, Chan FK, et al. Necroptosis: mechanisms and relevance to disease. Annu Rev Pathol. 2017;12:103–30.
Grootjans S, Vanden Berghe T, Vandenabeele P. Initiation and execution mechanisms of necroptosis: an overview. Cell Death Differ. 2017;24:1184–95.
Su X, Wang H, Kang D, Zhu J, Sun Q, Li T, et al. Necrostatin-1 ameliorates intracerebral hemorrhage-induced brain injury in mice through inhibiting RIP1/RIP3 pathway. Neurochem Res. 2015;40:643–50.
Shen H, Liu C, Zhang D, Yao X, Zhang K, Li H, et al. Role for RIP1 in mediating necroptosis in experimental intracerebral hemorrhage model both in vivo and in vitro. Cell Death Dis. 2017;8:e2641.
Seo J, Lee EW, Sung H. CHIP controls necroptosis through ubiquitylation- and lysosome-dependent degradation of RIPK3. Nat Cell Biol. 2016;18:291–302.
Zhou Y, Wang Y, Wang J, Anne Stetler R, Yang QW. Inflammation in intracerebral hemorrhage: from mechanisms to clinical translation. Prog Neurobiol. 2014;115:25–44.
Pasparakis M, Vandenabeele P. Necroptosis and its role in inflammation. Nature. 2015;517:311–20.
Wei Q, Sha Y, Bhattacharya A, et al. Regulation of IL-4 receptor signaling by STUB1 in lung inflammation. Am J Respir Crit Care Med. 2014;189:16–29.
Chen Z, Barbi J, Bu S, Yang HY, Li Z, Gao Y, et al. The ubiquitin ligase Stub1 negatively modulates regulatory T cell suppressive activity by promoting degradation of the transcription factor Foxp3. Immunity. 2013;39:272–85.
Zhan S, Wang T, Ge W. Multiple functions of the E3 ubiquitin ligase CHIP in immunity. Int Rev Immunol. 2017;36:300–12.
Deverman BE, Pravdo PL, Simpson BP, Kumar SR, Chan KY, Banerjee A, et al. Cre-dependent selection yields AAV variants for widespread gene transfer to the adult brain. Nat Biotechnol. 2016;34:204–9.
Morabito G, Giannelli SG, Ordazzo G, Bido S, Castoldi V, Indrigo M, et al. AAV-PHP.B-mediated global-scale expression in the mouse nervous system enables GBA1 gene therapy for wide protection from synucleinopathy. Mol Ther. 2017;25:2727–42.
Shi CH, Rubel C, Soss SE, Sanchez-Hodge R, Zhang S, Madrigal SC, et al. Disrupted structure and aberrant function of CHIP mediates the loss of motor and cognitive function in preclinical models of SCAR16. PLoS Genet. 2018;14:e1007664.
da Silva-Candal A, Vieites-Prado A, Gutierrez-Fernandez M, et al. Blood glutamate grabbing does not reduce the hematoma in an intracerebral hemorrhage model but it is a safe excitotoxic treatment modality. J Cereb Blood Flow Metab. 2015;35:1206–12.
Del Prete D, Rice RC, Rajadhyaksha AM. Amyloid precursor protein (APP) may act as a substrate and a recognition unit for CRL4CRBN and Stub1 E3 ligases facilitating ubiquitination of proteins involved in presynaptic functions and neurodegeneration. J Biol Chem. 2016;291:17209–27.
Tsvetkov P, Adamovich Y, Elliott E, Shaul Y. E3 ligase STUB1/CHIP regulates NAD(P)H:quinone oxidoreductase 1 (NQO1) accumulation in aged brain, a process impaired in certain Alzheimer disease patients. J Biol Chem. 2011;286:8839–45.
Tang MB, Li YS, Li SH, Cheng Y, Zhang S, Luo HY, et al. Anisomycin prevents OGD-induced necroptosis by regulating the E3 ligase CHIP. Sci Rep. 2018;8:6379.
Stankowski JN, Zeiger SL, Cohen EL, et al. C-terminus of heat shock cognate 70 interacting protein increases following stroke and impairs survival against acute oxidative stress. Antioxid Redox Signal. 2011;14:1787–801.
Dickey CA, Patterson C, Dickson D, Petrucelli L. Brain CHIP: removing the culprits in neurodegenerative disease. Trends Mol Med. 2007;13:32–8.
Saidi LJ, Polydoro M, Kay KR, Sanchez L, Mandelkow EM, Hyman BT, et al. Carboxy terminus heat shock protein 70 interacting protein reduces tau-associated degenerative changes. J Alzheimers Dis. 2015;44:937–47.
Wang Y, Ren F, Wang Y, Feng Y, Wang D, Jia B, et al. CHIP/Stub1 functions as a tumor suppressor and represses NF-kappaB-mediated signaling in colorectal cancer. Carcinogenesis. 2014;35:983–91.
Shang Y, He J, Wang Y, Feng Q, Zhang Y, Guo J, et al. CHIP/Stub1 regulates the Warburg effect by promoting degradation of PKM2 in ovarian carcinoma. Oncogene. 2017;36:4191–200.
Yang K, Zhang TP, Tian C, Jia LX, du J, Li HH. Carboxyl terminus of heat shock protein 70-interacting protein inhibits angiotensin II-induced cardiac remodeling. Am J Hypertens. 2012;25:994–1001.
Xiong W, Liu S, Cai W, Wen J, Fu Y, Peng J, et al. The carboxyl terminus of heat shock protein 70-interacting protein (CHIP) participates in high glucose-induced cardiac injury. Free Radic Biol Med. 2017;106:339–44.
Liu T, Bao YH, Wang Y, Jiang JY. The role of necroptosis in neurosurgical diseases. Braz J Med Biol Res. 2015;48:292–8.
Fakharnia F, Khodagholi F, Dargahi L, Ahmadiani A. Prevention of cyclophilin D-mediated mPTP opening using cyclosporine-a alleviates the elevation of necroptosis, autophagy and apoptosis-related markers following global cerebral ischemia-reperfusion. J Mol Neurosci. 2017;61:52–60.
Linkermann A, Hackl MJ, Kunzendorf U, Walczak H, Krautwald S, Jevnikar AM. Necroptosis in immunity and ischemia-reperfusion injury. Am J Transplant. 2013;13:2797–804.
Zhu X, Tao L, Tejima-Mandeville E, Qiu J, Park J, Garber K, et al. Plasmalemma permeability and necrotic cell death phenotypes after intracerebral hemorrhage in mice. Stroke. 2012;43:524–31.
Qu C, Guo S, Guo H, et al. Increased serum endotoxin and elevated CD14 and IL-1beta expression in a rat model of cerebrogenic multiple organ dysfunction syndrome. Med Chem. 2009;5:462–7.
Dohi K, Jimbo H, Ikeda Y, et al. Pharmacological brain cooling with indomethacin in acute hemorrhagic stroke: antiinflammatory cytokines and antioxidative effects. Acta Neurochir Suppl. 2006;96:57–60.
Wu J, Yang S, Xi G, et al. Microglial activation and brain injury after intracerebral hemorrhage. Acta Neurochir Suppl. 2008;105:59–65.
Zhang Z, Liu Y, Huang Q, Su Y, Zhang Y, Wang G, et al. NF-kappaB activation and cell death after intracerebral hemorrhage in patients. Neurol Sci. 2014;35:1097–102.
Liu DL, Zhao LX, Zhang S, du JR. Peroxiredoxin 1-mediated activation of TLR4/NF-kappaB pathway contributes to neuroinflammatory injury in intracerebral hemorrhage. Int Immunopharmacol. 2016;41:82–9.
Shinohara Y, Konno A, Nitta K, Matsuzaki Y, Yasui H, Suwa J, et al. Effects of neutralizing antibody production on AAV-PHP.B-mediated transduction of the mouse central nervous system. Mol Neurobiol. 2019;56:4203–14.
Weitzman MD, Linden RM. Adeno-associated virus biology. Methods Mol Biol. 2011;807:1–23.
Acknowledgments
The authors thank the Academy of Medical Sciences of Zhengzhou University Translational Medicine platform.
Funding
This work was funded by the National Natural Science Foundation of China to Dr Yu-ming Xu (Key Program grant number 81530037, 2015; General Program grant number 91849115, 2018) and the National Natural Science Foundation of China to Dr Chang-he Shi (General Program grant number 81771290, 2017).
Author information
Authors and Affiliations
Contributions
Yu-ming Xu supervised the whole project; Yu-ming Xu and Chang-he Shi designed and supported the study; Shuo Zhang and Zheng-wei Hu contributed to AAV particle production and immunofluorescence staining; Shuo Zhang, Zheng-wei Hu, Yao-he Wang, and Zhong-xian Zhang performed ICH operations; Shuo Zhang, Hai-yang Luo, Yu-sheng Li, and Bo Song performed behavioral testing, BBB permeability experiments, and H&E staining; Cheng-yuan Mao, Hai-yang Luo, and Mi-bo Tang performed Western blotting; Li-yuan Fan, Yao Zhang, and Wen-kai Yu contributed to ELISA experiments; Shuo Zhang, Zheng-wei Hu, Cheng-yuan Mao, and Hai-yang Luo analyzed the data; and Yu-ming Xu, Chang-he Shi, and Shuo Zhang wrote the manuscript.
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhang, S., Hu, Zw., Luo, Hy. et al. AAV/BBB-Mediated Gene Transfer of CHIP Attenuates Brain Injury Following Experimental Intracerebral Hemorrhage. Transl. Stroke Res. 11, 296–309 (2020). https://doi.org/10.1007/s12975-019-00715-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12975-019-00715-w