Abstract
Background
Hepatic encephalopathy, (HE) although commonly associated with cirrhosis, has also been reported in non-cirrhotic portal hypertension (NCPH). The importance of identifying and treating HE in NCPH lies in the fact that many patients may be wrongly diagnosed as having psychiatric or neurologic disorders. Hence, we aimed to systematically review the prevalence of HE in NCPH.
Methods
A comprehensive search of three databases (Medline, Embase and Scopus) was conducted from inception to November 2022 for studies reporting on the prevalence of minimal HE (MHE) and overt HE (OHE) in patients with NCPH. Results were presented as pooled proportions with their 95% confidence intervals (CI).
Results
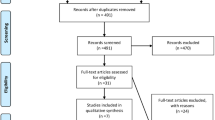
Total 25 studies (n = 1487) were included after screening 551 records. The pooled prevalence of MHE in NPCH was 32.9% (95% CI: 26.7–39.0) without any difference between adult (32.9%, 95% CI: 23.5–42.3) and pediatric patients (32.6%, 95% CI: 26.1–39.1) (p = 0.941). There was no significant difference in the prevalence between patients with NCPH and compensated cirrhosis with odds ratio of 1.06 (95% CI: 0.77–1.44). The pooled event rate for prior history of OHE in NCPH was 1.2% (95% CI: 0.3–2.1).
Conclusion
Around one-third of the patients with NCPH have MHE, irrespective of age group. OHE is extremely rare in NCPH and is usually associated with a precipitating factor.


Similar content being viewed by others
References
Louissaint J, Deutsch-Link S, Tapper EB. Changing epidemiology of cirrhosis and hepatic encephalopathy. Clin Gastroenterol Hepatol. 2022;20:S1-8.
Gioia S, Nardelli S, Ridola L, Riggio O. Causes and management of non-cirrhotic portal hypertension. Curr Gastroenterol Rep. 2020;22:1–8.
Gioia S, Nardelli S, Riggio O, Faccioli J, Ridola L. Cognitive impairement in non-cirrhotic portal hypertension: highlights on physiopathology, diagnosis and management. J Clin Med. 2021;11:101.
Lima LC, Miranda AS, Ferreira RN, Rachid MA, e Silva AC. Hepatic encephalopathy: lessons from preclinical studies. World J Hepatol. 2019;11:173–85.
Yadav SK, Srivastava A, Srivastava A, et al. Encephalopathy assessment in children with extra-hepatic portal vein obstruction with MR, psychometry and critical flicker frequency. J Hepatol. 2010;52:348–54.
Watanabe A. Portal-systemic encephalopathy in non-cirrhotic patients: classification of clinical types, diagnosis and treatment. J Gastroenterol Hepatol. 2000;15:969–79.
Dhiman RK, Chawla Y, Vasishta RK et al. Non-cirrhotic portal fibrosis (idiopathic portal hypertension): experience with 151 patients and a review of the literature. J Gastroenterol Hepatol. 2002;17:6–16.
Peter L, Dadhich SK, Yachha SK. Clinical and laboratory differentiation of cirrhosis and extrahepatic portal venous obstruction in children. J Gastroenterol Hepatol. 2003;18:185–9.
Mínguez B, García-Pagán JC, Bosch J, et al. Noncirrhotic portal vein thrombosis exhibits neuropsychological and MR changes consistent with minimal hepatic encephalopathy. Hepatology. 2006;43:707–14.
Das K, Singh P, Chawla Y, Duseja A, Dhiman RK, Suri S. Magnetic resonance imaging of brain in patients with cirrhotic and non-cirrhotic portal hypertension. Dig Dis Sci. 2008;53:2793–8.
Sharma P, Sharma BC, Puri V, Sarin SK. Minimal hepatic encephalopathy in patients with extrahepatic portal vein obstruction. Am J Gastroenterol. 2008;103:1406–12.
Goel A, Yadav S, Saraswat V, et al. Cerebral oedema in minimal hepatic encephalopathy due to extrahepatic portal venous obstruction. Liver Int. 2010;30:1143–51.
Pasquale C, Ridola L, Pentassuglio I, et al. Type-B (BYPASS) minimal hepatic encephalopathy (MHE) in patients with non-cirrhotic portal hypertension: relationship with the quality of life (QOL). Hepatology. 2010;52:901A-902A.
Srivastava A, Yadav SK, Lal R, et al. Effect of surgical portosystemic shunt on prevalence of minimal hepatic encephalopathy in children with extrahepatic portal venous obstruction: assessment by magnetic resonance imaging and psychometry. J Pediatr Gastroenterol Nutr. 2010;51:766–72.
Yadav SK, Saksena S, Srivastava A, et al. Brain MR imaging and 1H-MR spectroscopy changes in patients with extrahepatic portal vein obstruction from early childhood to adulthood. AJNR Am J Neuroradiol. 2010;31:1337–42.
Srivastava A, Yadav SK, Yachha SK, Thomas MA, Saraswat VA, Gupta RK. Pro-inflammatory cytokines are raised in extrahepatic portal venous obstruction, with minimal hepatic encephalopathy. J Gastroenterol Hepatol. 2011;26:979–86.
Schouten JN, Nevens F, Hansen B, et al. Idiopathic noncirrhotic portal hypertension is associated with poor survival: results of a long-term cohort study. Aliment Pharmacol Ther. 2012;35:1424–33.
Sharma P, Sharma BC. Lactulose for minimal hepatic encephalopathy in patients with extrahepatic portal vein obstruction. Saudi J Gastroenterol. 2012;18:168–72.
D’Antiga L, Dacchille P, Boniver C, et al. Clues for minimal hepatic encephalopathy in children with noncirrhotic portal hypertension. J Pediatr Gastroenterol Nutr. 2014;59:689–94.
Siramolpiwat S, Seijo S, Miquel R, et al. Idiopathic portal hypertension: natural history and long-term outcome. Hepatology. 2014;59:2276–85.
Yogesh KR, Ali M, Pugazhendi T, et al. Minimal hepatic encephalopathy in children withextrahepatic portal vein obstruction. Indian J Gastroenterol. 2014;33:A54.
Babar G, Thomas V. Occurrence of minimal hepatic encephalopathy in patients of extrahepatic portal hypertensionversus cirrhosis of the liver (Child A) – a comparative study. Indian J Gastroenterol. 2015;34:A32.
Nicoletti V, Gioia S, Lucatelli P, et al. Hepatic encephalopathy in patients with non-cirrhotic portal hypertension: description, prevalence and risk factors. Dig Liver Dis. 2016;48:1072–7.
Yadav SK, Goel A, Saraswat VA, et al. Evaluation of cognitivity, proinflammatory cytokines, and brain magnetic resonance imaging in minimal hepatic encephalopathy induced by cirrhosis and extrahepatic portal vein obstruction. J Gastroenterol Hepatol. 2016;31:1986–94.
El-Karaksy HM, Afifi O, Bakry A, Kader AA, Saber N. A pilot study using lactulose in management of minimal hepatic encephalopathy in children with extrahepatic portal vein obstruction. World J Pediatr. 2017;13:70–5.
Suresh MV, Jagadisan B, Kandasamy P, Senthilkumar GP. Stroop test validation to screen for minimal hepatic encephalopathy in pediatric extrahepatic portal venous obstruction. J Pediatr Gastroenterol Nutr. 2018;66:802–7.
Liu M, He WT, Chen DS, Hu DH. Analysis of influencing factors on hepatic encephalopathy in patients with non-cirrhotic portal hypertension. Zhonghua Gan Zang Bing Za Zhi. 2019;27:673–6.
Lv Y, Li K, He C, et al. TIPSS for variceal bleeding in patients with idiopathic non-cirrhotic portal hypertension: comparison with patients who have cirrhosis. Aliment Pharmacol Ther. 2019;49:926–39.
Elkrief L, Lazareth M, Chevret S, et al. Liver stiffness by transient elastography to detect porto-sinusoidal vascular liver disease with portal hypertension. Hepatology. 2021;74:364–78.
Wöran K, Semmler G, Jachs M, et al. Clinical course of porto-sinusoidal vascular disease is distinct from idiopathic noncirrhotic portal hypertension. Clin Gastroenterol Hepatol. 2022;20:e251–66.
Ferenci P, Lockwood A, Mullen K, Tarter R, Weissenborn K, Blei AT. Hepatic encephalopathy–definition, nomenclature, diagnosis, and quantification: final report of the working party at the 11th World Congresses of Gastroenterology, Vienna, 1998. Hepatology. 2002;35:716–21.
Sharma P, Sharma BC, Puri V, Sarin SK. Natural history of minimal hepatic encephalopathy in patients with extrahepatic portal vein obstruction. Am J Gastroenterol. 2009;104:885–90.
Groeneweg M, Quero JC, De Bruijn I, et al. Subclinical hepatic encephalopathy impairs daily functioning. Hepatology. 1998;28:45–9.
Bao ZJ, Qiu DK, Ma X, et al. Assessment of health-related quality of life in Chinese patients with minimal hepatic encephalopathy. World J Gastroenterol. 2007;13:3003–8.
Krishna YR, Yachha SK, Srivastava A, Negi D, Lal R, Poddar U. Quality of life in children managed for extrahepatic portal venous obstruction. J Pediatr Gastroenterol Nutr. 2010;50:531–6.
D’Antiga L, Casotti V, Caffi LG, et al. The conundrum of cognitive dysfunction in children with portal hypertension: the experience of Bergamo. Italy J Clin Exp Hepatol. 2022;12:723–4.
Bajaj JS, Saeian K, Christensen KM, et al. Probiotic yogurt for the treatment of minimal hepatic encephalopathy. Am J Gastroenterol. 2008;103:1707–15.
Author information
Authors and Affiliations
Contributions
Conceptualization: SG, AS; data curation: SG, SG, SA; formal analysis: SG, AS, SA; funding acquisition: N/A; investigation: SG, AS, SA, KK; methodology: SG, SA; project administration: SG, AR; resources: SG, AS, SA; software: SG; supervision: SG, KK; validation: SG, AR; visualization: SG; roles/writing — original draft: SG, AS, SA; writing — review and editing: SG, AS, SA, KK, AR.
Corresponding author
Ethics declarations
Ethical approval
Not required.
Conflict of interest
SG, AS, SA, KK and AR declare no competing interests.
Disclaimer
The authors are solely responsible for the data and the contents of the paper. In no way, the Honorary Editor-in-Chief, Editorial Board Members, the Indian Society of Gastroenterology or the printer/publishers are responsible for the results/findings and content of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Giri, S., Singh, A., Angadi, S. et al. Prevalence of hepatic encephalopathy in patients with non-cirrhotic portal hypertension: A systematic review and meta-analysis. Indian J Gastroenterol 42, 642–650 (2023). https://doi.org/10.1007/s12664-023-01412-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12664-023-01412-1