Abstract
Background
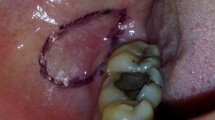
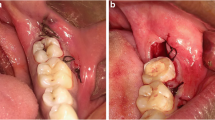
Surgical removal of the mandibular third molar requires reflection of the mucoperiosteal flap. Several studies have suggested different varieties and innovative designs for flap reflection. We have designed a randomized controlled trial (RCT) to check the feasibility of two flap designs: lingual-based triangular flap (LBTF) and buccal-based triangular flap (BBTF) by calculating the duration of surgery and evaluating postoperative complications such as pain, swelling, and trismus.
Materials and Method
It was a non-inferiority parallel-group RCT. The trial was registered in the Control Trial Register of India (CTRI/2021/10/037182) and was performed according to Consolidated Standards of Registered Trial (CONSORT) guidelines. Intraoperative surgery time and postoperative pain, swelling, and trismus were measured and analyzed by a two-sample t test. The Chi-square test was used to measure gender distribution in the study.
Result
Of the total of 88 required subjects, gender distribution and performed surgical time were statistically insignificant with a p-value of 0.76 and 0.48, respectively. The pain was significantly higher in the LBTF group in the 5th and 7th postoperative days with a p-value of 0.02 and 0.028. The swelling was statistically higher during all the follow-ups except for the 28th day in the LBTF group with values of 0.006, 0.002 and 0.003, respectively. There was no significant difference in inter-incisional distance (IID) between the groups during postoperative check-ups.
Conclusion
LBTF shows no edge over BBTF during mandibular third molar disimpaction.




Similar content being viewed by others
References
Hashemipour MA, Tahmasbi-Arashlow M, Fahimi-Hanzaei F (2013) Incidence of impacted mandibular and maxillary third molars: a radiographic study in a Southeast Iran population. Med Oral Patologia Oral y Cirugia Bucal 18(1):e140
Hyam DM (2018) The contemporary management of third molars. Aust Dent J 63:S19-26
Medina-Solís CE, Mendoza-Rodríguez M, Márquez-Rodríguez S, De la Rosa-Santillana R, Islas-Zarazua R, Navarrete-Hernández J, Maupomé G (2014) Reasons why erupted third molars are extracted in a public university in Mexico. West Indian Med J 63(4):354
Asif JA, Noorani TY, Alam MK (2017) Tooth auto-transplantation: an alternative treatment. Bull Tokyo Dent Coll 58(1):41–48
Blanco G, Lora D, Marzola C (2016) The different types of flaps in the surgical relations of the third impacted molars–literature review. Dentistry 7(425):2161–1122
Yolcu ÜM, Acar AH (2015) Comparison of a new flap design with the routinely used triangular flap design in third molar surgery. Int J Oral Maxillofac Surg 44(11):1390–1397
Troiano G, Laino L, Cicciù M, Cervino G, Fiorillo L, D’amico C, Zhurakivska K, Muzio LL (2018) Comparison of two routes of administration of dexamethasone to reduce the postoperative sequelae after third molar surgery: a systematic review and meta-analysis. Open Dent J 12:181
Moher D, Hopewell S, Schulz KF, Montori V, Gøtzsche PC, Devereaux PJ, Elbourne D, Egger M, Altman DG (2012) CONSORT 2010 explanation and elaboration: updated guidelines for reporting parallel /group randomised trials. Int J Surg 10(1):28–55
World Medical Association. Ethical principles for medical research involving human subjects. Eur J Emerg Med. 2001;8(3):221–3.
Yuasa H, Kawai T, Sugiura M (2002) Classification of surgical difficulty in extracting impacted third molars. Br J Oral Maxillofac Surg 40(1):26–31
Delgado DA, Lambert BS, Boutris N, McCulloch PC, Robbins AB, Moreno MR, Harris JD. Validation of digital visual analog scale pain scoring with a traditional paper-based visual analog scale in adults. J Am Acad Orthopaedic Surg Glob Res Rev 2018;2(3).
Vishal KT, Ranjan R, Sharma N. Primary closure after surgical extraction of mandibular third molar with or without tube drain: a prospective study. J Fam Med Primary Care. 2020;9(2):637.
Goldsmith SM, De Silva RK, Tong DC, Love RM (2012) Influence of a pedicle flap design on acute postoperative sequelae after lower third molar removal. Int J Oral Maxillofac Surg 41(3):371–375
Ogundipe OK, Ugboko VI, Owotade FJ (2011) Can autologous platelet-rich plasma gel enhance healing after surgical extraction of mandibular third molars? J Oral Maxillofac Surg 69(9):2305–2310
Sanchís Bielsa JM, Hernández Bazán S, Peñarrocha Diago M. Flap repositioning versus conventional suturing in third molar surgery.
Osunde OD, Adebola RA, Saheeb BD (2012) A comparative study of the effect of suture-less and multiple suture techniques on inflammatory complications following third molar surgery. Int J Oral Maxillofac Surg 41(10):1275–1279
Menziletoglu D, Guler AY, Basturk F, Isik BK, Erdur EA (2020) Comparison of two different flap designs for bilateral impacted mandibular third molar surgery. J Stomatol Oral Maxillof Surg 121(4):368–372
Balakrishnan G, Narendar R, Kavin T, Venkataraman S, Gokulanathan S (2017) Incidence of trismus in transalveolar extraction of lower third molar. J Pharm Bioallied Sci 9(Suppl 1):S222
Choudhury R, Rastogi S, Rohatgi RG, Abdulrahman BI, Dutta S, Giri KY (2022) Does pedicle flap design influence the postoperative sequel of lower third molar surgery and quality of life? J Oral Biol Craniofac Res 12(5):694–701
Ahmad M, Khan ZA, Khan TU, Alqutub MN, Mokeem SA, AlMubarak AM, Haider M, Al-Askar M, Ahmed N, Aldahiyan N, Vohra F (2021) Influence of surgical flap design (Envelope and Szmyd) for removal of impacted mandibular third molars on clinical periodontal parameters: a clinical trial. Int J Environ Res Public Health 18(9):4465
Xie Q, Wei S, Zhou N, Huang X (2021) Modified envelope flap, a novel incision design, can relieve complications after extraction of fully horizontal impacted mandibular third molar. J Dental Sci 16(2):718–722
Bello SA, Adeyemo WL, Bamgbose BO, Obi EV, Adeyinka AA (2011) Effect of age, impaction types and operative time on inflammatory tissue reactions following lower third molar surgery. Head Face Med 7(1):1–8
Mobilio N, Vecchiatini R, Vasquez M, Calura G, Catapano S (2017) Effect of flap design and duration of surgery on acute postoperative symptoms and signs after extraction of lower third molars: a randomized prospective study. J Dental Res Dental Clinics Dental Prospects 11(3):156
Acknowledgements
None.
Funding
This research did not receive any grant from any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest.
Ethical Approval
The study was initiated after taking Institutional ethical clearances from RIMS, Ranchi, Memo No. 312 dated 09/07/2021.
Research Involving Human Participants and/or Animals
The research involves human participants. The research protocol had been approved by the institutional ethical committee.
Informed Consent
Written informed consent had been taken from all the study subjects.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shahi, A.K., Vishal, Sharma, S. et al. Comparison of Buccal and Lingual-Based Triangular Flap During Mandibular Third Molar Extraction for Reducing Postoperative Complications: A Randomized Controlled Trial. J. Maxillofac. Oral Surg. (2024). https://doi.org/10.1007/s12663-023-02092-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12663-023-02092-2