Abstract
Introduction
The reconstitution of form and function after maxillofacial tumor resection or traumatic bony defects is a challenge when considering reconstructive options. The reconstructive options will depend upon whether the tissues to be replaced included bone alone or both bone and soft tissue (composite resection).
Methodology
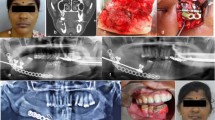
This study was carried out on nine patients who with benign tumors or cysts of the mandible that required segmental resection. Mandibular reconstruction using mandibular transport distraction osteogenesis was performed for all the cases. Depending on whether the condyle was spared or sacrificed, the type of mandibular transport distractor either fixed on the remnant condyle-ramus unit or had a condylar component replacing the resected condyles. Depending on the location of the defect, transport distraction was carried our anterior to posterior or posterior to anterior.
Results
A total of nine cases of benign mandibular pathologies were operated. Segmental resection with condylar preservation was carried out in seven cases, segmental resection with condylar resection was carried out in two cases. In cases with condylar resection, the reconstruction plate of the distractor device had a condylar component. Anterior to posterior transport distraction was carried out in seven cases, and posterior to anterior transport distraction carried out in two cases. The amount of distracted bone ranged from 38 to 46 mm.
Conclusion
Mandibular transport distraction osteogenesis offers a modality of reconstruction where the patient’s native host bone is osteotomized and gradually distracted to induce the formation of regenerated osseous structure and soft tissue. Being cost-effective, not requiring a steep learning curve/long operative time, and not technically demanding as vascularized bone grafts/flaps, it is feasible in the Indian setup as a practical reconstructive option for benign jaw tumors.






Similar content being viewed by others
References
Likhterov I, Roche AM, Urken ML (2019) Contemporary osseous reconstruction of the mandible and the maxilla. Oral Maxillofac Surg Clin North Am 31(1):101–116
Fernandes RP, Yetzer JG (2013) Reconstruction of acquired oromandibular defects. Oral Maxillofac Surg Clin North Am 25(2):241–249
Neelakandan RS, Bhargava D (2012) Transport distraction osteogenesis for maxillomandibular reconstruction: current concepts and applications. J Maxillofac Oral Surg 11(3):291–299
Kademani D, Keller E (2006) Iliac crest grafting for mandibular reconstruction. Atlas Oral Maxillofac Surg Clin North Am 14(2):161–170
Pogrel MA, Podlesh S, Anthony JP, Alexander J (1997) A comparison of vascularized and nonvascularized bone grafts for reconstruction of mandibular continuity defects. J Oral Maxillofac Surg 55(11):1200–1206
Foster RD, Anthony JP, Sharma A, Pogrel MA (1999) Vascularized bone flaps versus nonvascularized bone grafts for mandibular reconstruction: an outcome analysis of primary bony union and endosseous implant success. Head Neck 21(1):66–71
Okoturo E (2016) Non-vascularised iliac crest bone graft for immediate reconstruction of lateral mandibular defect. Oral Maxillofac Surg 20(4):425–429
Camarini C, Spagnol G, Pinotti MM, Canto AM, Maciel FA, Freitas RR (2020) Mandibular reconstruction with block iliac crest an institutional experience. Craniomaxillofac Trauma Reconstr 13(4):285–289
Reconstruction M (2012) Potter JK. In: Bagheri SC, Bell RB, Khan HA (eds) Current therapy in oral and maxillofacial surgery, 1st edn. Elsevier Saunders, St Louis (MO), pp 483–496
Marx RE (1991) Current advances in reconstruction of the mandible in head and neck cancer surgery. Semin Surg Oncol 7(1):47–57
Farhadieh RD, Dickinson R, Yu Y, Gianoutsos MP, Walsh WR (1999) The role of transforming growth factor-beta, insulin-like growth factor I, and basic fibroblast growth factor in distraction osteogenesis of the mandible. J Craniofac Surg 10(1):80–86
Latalski M, Elbatrawy YA, Thabet AM, Gregosiewicz A, Raganowicz T, Fatyga M (2001) Enhancing bone healing during distraction osteogenesis with platelet-rich plasma. Injury 42(8):821–824
Swennen GR, Schutyser F, Mueller MC, Kramer FJ, Eulzer C, Schliephake H (2005) Effect of platelet-rich-plasma on cranial distraction osteogenesis in sheep: preliminary clinical and radiographic results. Int J Oral Maxillofac Surg 34(3):294–304
Gentile RD (2020) Easy platelet-rich fibrin (injectable/topical) for post-resurfacing and microneedle therapy. Facial Plast Surg Clin North Am 28(1):127–134
Masuki H, Okudera T, Watanebe T, Suzuki M, Nishiyama K, Okudera H, Nakata K, Uematsu K, Su CY, Kawase T (2016) Growth factor and pro-inflammatory cytokine contents in platelet-rich plasma (PRP), plasma rich in growth factors (PRGF), advanced platelet-rich fibrin (A-PRF), and concentrated growth factors (CGF). Int J Implant Dent 2(1):19
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, analysis and interpretation of data was performed by TZ. PKK, PD and DPS helped in the acquisition of data. RSN revised it critically for important intellectual content and made substantial contributions to the conception and design of the work. All authors commented on previous versions of the manuscript and read and approved the final.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
“All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.”
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Neelakandan, R.S., Zachariah, T., Kuchimanchi, P.K. et al. Versatility of Transport Distraction Osteogenesis for Reconstruction of Lateral Mandibular Ablative Defects. J. Maxillofac. Oral Surg. 23, 630–638 (2024). https://doi.org/10.1007/s12663-023-01923-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12663-023-01923-6