Abstract
Background
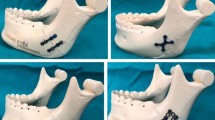
Mandible is the only mobile facial jaw bone and it aides in various functions such as phonation and mastication. Therefore, management of mandible fracture becomes inevitable due to its functional and anatomical importance. Fracture fixation methods and techniques have steadily evolved with various osteosynthesis systems. In this article, we discuss the management of mandible fracture using a newly designed two-dimensional (2D) hybrid V-shaped plate.
Purpose
In this paper, we have evaluated the efficacy of the newly developed 2D V-shaped locking plate in the management of mandibular fractures.
Method
We have assessed 12 cases of different mandibular fractures ranging from symphysis, parasymphysis, angle and subcondylar region. Treatment outcome was assessed both clinically and radiologically at regular intervals with various intraoperative and postoperative parameters.
Result
Results of this study suggest that fixation of mandible fracture with the 2D hybrid V-shaped plate facilitates anatomic reduction and functional stability and carries a low morbidity and infection rate.
Conclusion
The 2D anatomic hybrid V-shaped plate can be a suitable alternative to conventional miniplate and 3D plates as it offers satisfactory anatomic reduction and functional stability. Positioning the plate in relation to the mental nerve and plate adaptation along the angle region are much easier.





Similar content being viewed by others
References
Gruss JS, Phillips JH (1989) Complex facial trauma: the evolving role of rigid fixation and immediate bone graft reconstruction. Clin Plast Surg 16(1):93–104
Hobar PC (1992) Methods of rigid fixation. Clin Plast Surg 19:31–39
Schilli W (1982) Rigid internal fixation by means of compression plates. In: Kruger E, Schilli W (eds) Oral and maxillofacial traumatology. Quintessence, Chicago, pp 308–318
Champy M, Loddé JP, Schmitt R, Jaeger JH, Muster D (1978) Mandibular osteosynthesis by miniature screwed plates via a buccal approach. J Maxillofac Surg 6:14–21
Cawood JI (1985) Small plate osteosynthesis of mandibular fractures. Br J Oral Maxillo-fac Surg 23:77–91
Freihofer HP, Sailer HS (1973) Experiences with intraoral trans-osseous wiring of mandibular fractures. J Max-Fae Surg 1:248
Michelet FX, Deymes J, Dessus B (1973) Osteosynthesis with miniaturised screwed plates in maxillofacial surgery. J Maxilla Fac Surg 1(79):84
Oikarinen K, Altonen M, Kauppi H, Laitakari K (1989) Treatment of mandibular fractures. Need for rigid internal fixation. J Craniomaxillofac Surg 17:24–30
Wald RM, Abemayor E, Zemplenyi J, Mannai C, Lesavoy M (1988) The transoral treatment of mandibular fractures using non-compression miniptates. Ann Plast Surg 20:409–413
Ribeiro-Junior PD, Magro-Filho O, Shastri KA, Papageorge MB (2010) In vitro evaluation of conventional and locking miniplate/screw systems for the treatment of mandibular angle fractures. Int J Oral Maxillofac Surg 39:1109–1114
Nayak SS, Pushpalatha C, Tammanavar PS, Naduwinmani SL, Mohan M (2013) Efficacy of locking plates/screw system in mandibular fracture surgery. J Contemp Dent Pract 14(2):222–226
Ellis E, Graham J (2002) Use of a 2.0 mm locking plate/screw system for mandibular fracture surgery. J Oral Maxillofac Surg 60:642–645
Bhagat JA et al (2019) Development of a new V-shaped implant with locking plates and screws for mandibular fracture fixation: an in vitro study using finite element analysis. Br J Oral Maxillofac Surg 57:805–807
Egol KA, Kubiak EN, Fulkerson E, Kummer FJ, Koval KJ (2004) Biomechanics of locked plates and screws. J Orthop Trauma 18(08):488–493
Misch CE (1990) Density of bone: effect on treatment plans, surgical approach, healing, and progressive bone loading. Int J Oral Implantol 6(2):23–31
Kawai T et al (1997) Radiographic changes during bone healing after mandibular fractures. Br J Oral Maxillofac Surg 35(5):312–318
Braasch DC, Abubaker AO (2013) Management of mandibular angle fracture. Oral Maxillofac Surg Clin N Am 25:591–600
Kaitu H, Tenhulzen D (1985) Compression osteosynthesis of mandibular fractures: a retrospective study. J Oral Maxillofac Surg 43:585
Ardary WC (1989) Prospective clinical evaluation of the use of compression plates and screws in the management of mandible fractures. J Oral Maxillofac Surg 47:1150
Schierle HP, Schmelzeisen R, Rahn B et al (1997) One or two plate fixation of mandibular angle fractures. J Craniomaxillofac Surg 25:162
Ellis EA (2010) Prospective study of 3 treatment methods for isolated fractures of the mandibular angle. J Oral Maxillofac Surg 68:2743–2754. https://doi.org/10.1016/j.joms.2010.05.080
Fox AJ, Kellman RM (2003) Mandibular angle fractures: two-miniplate fixation and complications. Arch Facial Plast Surg 5:464
Valentino J, Levy FE, Marentette LJ (1994) Intraoral mono cortical miniplating of mandible fractures. Arch Otolaryngol Head Neck Surg 120:605
Lindahl L (1977) Condylar fractures of the mandible. I. Classification and relation to age, occlusion, and concomitant injures of teeth and teeth supporting structures, and fractures of the mandibular body. Int J Oral Surg 6:12–21
Hammer B, Schier P, Prein J (1997) Osteosynthesis of condylar neck fractures: a review of 30 patients. Br J Oral Maxillofac Surg 35:288
Parascandolo S, Spinzia A, Parascandolo S, Piombino P, Califano L (2010) Two load sharing plates fixation in mandibular condylar fractures: biomechanical basis. J Cranio-Maxillo-Fac Surg 38:385–390
Meyer C, Kahn J-L, Boutemi P, Wilk A (2002) Photoelastic analysis of bone deformation in the region of the mandibular condyle during mastication. J Cranio-Maxillo-Fac Surg Off Publ Eur Assoc Cranio-Maxillo-Fac Surg 30(3):160–169
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bhagat, M.J.A., Durairaj, D., Naganathan, V. et al. Application of Anatomically Designed 2-Dimensional V Plate in Management of Mandible Fracture: A Pilot Study. J. Maxillofac. Oral Surg. 21, 1363–1368 (2022). https://doi.org/10.1007/s12663-021-01558-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12663-021-01558-5