Abstract
Aim
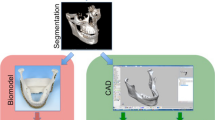
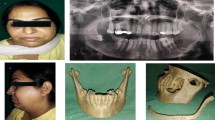
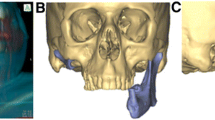
To assess the usefulness of 3D models for the surgical management of mandibular pathology requiring resection with continuity defects reconstructed using reconstruction plates.
Patients and Method
A bidirectional study was conducted in 40 patients, 20 each in group 1 and 2. Group 1 included those patients taken up for resection with continuity defects and reconstruction using reconstruction plates without using 3D models and Group 2 included those patients managed similarly with 3D models. Pre-operative pathological model and mirrored model was fabricated for accurate placement and pre-bending of plates and determining the position and length of the screws. The level of understanding of the patients with regards to the diagnosis and extent of the disease (VAS 0–10), treatment planning (VAS 0–10), accuracy of fixation by a blinded surgeon (VAS 0–5), operative time, change in the mouth Opening, occlusal disturbance, implant-related complications was assessed as outcome measures and tested statistically.
Results
The level of understanding of the patients with regards to the diagnosis and extent of the disease, treatment planning, operative time and accuracy of fixation was found to be statistically significant with superior performance in Group 2. No statistical significance was elicited in the change in mouth opening. No limitation in the mandibular range of movements and occlusal disturbance was found in any patient. No implant-related complications were found during the follow-up.
Conclusion
3D model fabrication can serve as a valuable adjunct in improving clinical outcomes with minimal operating time, increased patient compliance and radiological accuracy of fixation.
















Similar content being viewed by others
References
Mankovich NJ, Cheeseman AM, Stoker NG (1990) The display of three-dimensional anatomy with stereolithographic models. J Digit Imaging 3:200–203. https://doi.org/10.1007/BF03167610
Mehra P, Miner J, D’Innocenzo R et al (2011) Use of 3-D stereolithographic models in oral and maxillofacial surgery. J Maxillofac Oral Surg 10:6–13. https://doi.org/10.1007/s12663-011-0183-3
Santler C, Karcher H, Ruda C (1998) Indications and limitations of three-dimensional models in cranio-maxillofacial surgery. J Cranio-Maxillo-Fac Surg 26:11–16. https://doi.org/10.1016/S1010-5182(98)80029-2
Cunningham LL, Madsen MJ, Peterson G (2005) Stereolithographic modeling technology applied to tumor resection. J Oral Maxillofac Surg 63:873–878. https://doi.org/10.1016/j.joms.2005.02.027
Chow LK, Cheung LK (2007) The usefulness of stereomodels in maxillofacial surgical management. J Oral Maxillofac Surg 65:2260–2268. https://doi.org/10.1016/j.joms.2006.11.041
Lantada AD, Morgado PL (2012) Rapid prototyping for biomedical engineering: current capabilities and challenges. Annu Rev Biomed Eng 14:73–96. https://doi.org/10.1146/annurev-bioeng-071811-150112
Thomas DJ, Azmi MABM, Tehrani Z (2014) 3D additive manufacture of oral and maxillofacial surgical models for preoperative planning. Int J Adv Manuf Technol 71:1643–1651
Shaheen E, Alhelwani A, Van De Casteele E et al (2018) Evaluation of dimensional changes of 3D printed models after sterilization: a pilot study. Open Dent J 12:72–79. https://doi.org/10.2174/1874210601812010072
Asaumi J, Kawai N, Honda Y et al (2001) Comparison of three-dimensional computed tomography with rapid prototype models in the management of coronoid hyperplasia. Dentomaxillofac Radiol 30:330–335. https://doi.org/10.1038/sj/dmfr/4600646
Hwang WJ, Lee DH, Choi W et al (2017) Analysis of orbital volume measurements following reduction and internal fixation using absorbable mesh plates and screws for patients with orbital floor blowout fractures. J Craniofac Surg 28:1664–1669. https://doi.org/10.1097/SCS.0000000000003730
https://all3dp.com/1/types-of-3d-printers-3d-printing-technology/
Seol G-J, Jeon E-G, Lee J-S et al (2014) Reconstruction plates used in the surgery for mandibular discontinuity defect. J Korean Assoc Oral Maxillofac Surg 40:266. https://doi.org/10.5125/jkaoms.2014.40.6.266
Suomalainen A, Stoor P, Mesimäki K et al (2015) Rapid prototyping modelling in oral and maxillofacial surgery: a two year retrospective study. J Clin Exp Dent 7:e605–e612. https://doi.org/10.4317/jced.52556
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All Authors declare that they have no conflict of interest in this original study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Roy Chowdhury, S.K., Shadamarshan Rengasayee, A. & Krishnaprabhu, R. The Application of Pre-operative Three-Dimensional Models in the Management of Mandibular Pathology: Is it Really Useful? An Institutional Study. J. Maxillofac. Oral Surg. 20, 121–131 (2021). https://doi.org/10.1007/s12663-020-01419-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12663-020-01419-7