Abstract
Introduction
There has been a changing trend of treating temporomandibular joint subluxation, which range from conservative non-surgical measures to various soft and hard tissue surgical procedures aimed at either augmenting or restricting the condylar path.
Aim
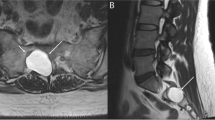
This study was aimed at comparing the efficacy of three major surgical treatment modalities: condylar obstruction creation, obstruction removal and anti-translatory procedures. Also, the location, anatomy and morphology of the TMJs pre- and post-surgery were evaluated and compared using radiographs, sagittal and 3-D Computed Tomographic scans.
Materials and Methods
A 6-year study was carried out on seventy-five patients of various age groups. Twenty-five were operated by the Dautrey’s procedure, 25 by articular eminectomy alone and the remaining 25 by eminectomy followed by meniscal plication and tethering. The distribution of patients in the three groups was random. Effectiveness of the surgical procedure and incidence of complications including recurrence were carefully compiled and compared between the three groups.
Results and Conclusion
Dautrey’s procedure yielded more gratifying and stable results, leading to a successful and permanent correction of chronic recurrent dislocation of the TMJs, with practically nil complications, thus demonstrating it to be an extremely safe, effective and versatile technique, making the joints function normally and securing sufficient volume of mouth opening. There was observed an average increase in articular tubercle height by 3.65 mm and a mean anterior shift of its lowest point by 4.5 mm following the Dautrey’s procedure, which were statistically significant findings. The upper age limit to carry out the Dautrey’s procedure can be safely taken up to 45 years.













Similar content being viewed by others
References
Helman J, Laufer D, Minkov B, Gutman D (1984) Eminectomy as surgical treatment for chronic mandibular dislocations. Int J Oral Surg 47:179–184
Babatunde BO (2011) Evaluation of the mechanism and principles of management of temporomandibular joint dislocation. Systematic review of literature and a proposed new classification of temporomandibular joint dislocation. Head Face Med 7:10–14
Bhandari S, Swain M, Dewoolkar LV (2008) Temporomandibular joint dislocation after laryngeal mask airway insertion. Internet J Anesthesiol 16:1–4
Bauss O, Sadat-Khonsari R, Fenske C, Engelke W, Schwestka-Polly R (2004) Temporomandibular joint dysfunction in Marfan syndrome. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 97:592–598
Undt G, Weichselbraun A, Wagner A, Kermer C, Rasse M (1996) Recurrent mandibular dislocation under neuroleptic drug therapy, treated by bilateral eminectomy. J Craniomaxillofac Surg 24:184–186
Qiu WL, Ha Q, Hu QG (1989) Treatment of habitual dislocation of the temporomandibular joint with subsynovial injection of sclerosant through arthroscope. Proc Chin Acad Med Sci Peking Union Med Coll 4:196–198
Daif ET (2010) Autologous blood injection as a new treatment modality for chronic recurrent temporomandibular joint dislocation. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 109:31–36
Martinez-Perez D, Garcia Ruiz-Espiga P (2004) Recurrent temporomandibular joint dislocation treated with botulinum toxin: report of 3 cases. J Oral Maxillofac Surg 62:244–246
Caminiti MF, Weinberg S (1998) Review Chronic mandibular dislocation: the role of non-surgical and surgical treatment. J Can Dent Assoc 64:484–491
Gadre Kiran Shrikrishna, Kaul Deepak, Ramanojam Shandilya, Shah Shishir (2010) Dautrey’s procedure in treatment of recurrent dislocation of the mandible. J Oral Maxillofac Surg 68:2021–2024
Undt G, Kermer C, Piehslinger E, Rasse M (1997) Treatment of recurrent mandibular dislocation, Part I: Leclerc blocking procedure. Int J Oral Maxillofac Surg 26:92–97
LeClerc G, Girard G (1943) Un nouveau proceed de butee dans le traitment chirurgical de la luvation recidivante de la manchoire inferieure. Mem Acad Chir 69:451–455
Gosserez M, Dautrey J (1967) Osteoplastic bearing for treatment of temporomandibular luxation. Transaction of second congress of the international association of oral surgeons Copenhagen, Munksgaard. Int J Oral Surg 4:261–263
Dautrey J (1975) Reflexions sur la chirugie de particulation temporomandibulaire. Stomologica Belg 72:577–579
Pogrel MA (1987) Articular Eminectomy for recurrent dislocation. Br J Oral Maxillofac Surg 25:237–243
Sato J, Suzuki T, Fujimura K (2003) Clinical Evaluation of arthroscopic eminoplasty for habitual dislocation of the temporomandibular joint- comparative study with conventional open eminectomy. J Oral Surg Oral Med Oral Pathol Oral Radiol Endod 95:390–395
Weinberg S (1984) Eminectomy and meniscorrhaphy for internal derangements of the temporomandibular joint. Rationale and operative technique. Oral Surg Oral Med Oral Pathol 57:241–249
Oatis G, Baker D (1984) The bilateral eminectomy as definitive treatment. J Oral Surg 3:294–298
Myrhaug H (1951) A new method of operation for habitual dislocation of the mandible: review of former method of treatment. Acta Odontol Scand 9:247–261
Laskin DM (1973) Myotomy for the management of recurrent and protracted mandibular dislocation. Trans Int Conf Oral Surg 4:264–268
Gould JF (1978) Shortening of the temporalis tendon for hypermobility of the temporomandibular joint. J Oral Surg 36:781–783
Sindet-Pedersen S (1988) Intraoral myotomy of the lateral pterygoid muscle for treatment of recurrent dislocation of the mandibular condyle. J Oral Maxillofac Surg 46:445–448
Varghese Mani (2005) Pterygoid plate disjunction: minimally invasive treatment for internal derangement of the temporomandibular joint. Asian J Oral Maxillofac Surg 17:247–255
Lawler MG (1982) Recurrent dislocation of the mandible : treatment of ten cases by the Dautrey procedure. Br J Oral Surg 20:14–21
To EWH (1991) A complication of the Dautrey’s procedure. Br J Oral Maxillofac Surg 29:100–101
Kobayashi H, Yamazaki T, Okudera H (2000) Correction of recurrent dislocation of the mandible in elderly patients by the Dautrey procedure. Br J Oral Maxillofac Surg 38:54–57
Harsha BC, Turvey TA, Powers SK (1986) Use of autogenous cranial bone graft in maxillofacial surgery: a preliminary report. J Oral Maxillofac Surg 44:11–19
Jackson IT, Helden G, Marx R (1986) Skull bone grafts in maxillofacial and craniofacial surgery. J Oral Maxillofac Surg 44:949–955
Medraa AM, Mahrous AM (2008) Glenotemporal osteotomy and bone grafting in the management of chronic recurrent dislocation and hypermobility of the temporomandibular joint. Br J Oral Maxillofac Surg 46:119–122
Karabouta I (1990) Increasing the articular eminence by the use of blocks of porous coralline hydroxyapatite for treatment of recurrent joint dislocation. J Craniomaxillofac Surg 18:107–109
Revington PJD (1986) The Dautrey procedure—a case for reassessment. Br J Oral Maxillofac Surg 24:217–220
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author of this article has not received any research grant, remuneration, or speaker honorarium from any company or committee whatsoever, and neither owns any stock in any company. The author declares that she does not have any conflict of interest.
Human and Animal Rights
All procedures performed on the patients (human participants) involved were in accordance with the ethical standards of the institution and/or national research committee, as well as with the 1964 Helsinki declaration and its later amendments and comparable ethical standards.
Ethical Approval
This article does not contain any new studies with human participants or animals performed by the author.
Informed Consent
Informed consent was obtained from all the individual participants in this study.
Rights and permissions
About this article
Cite this article
Jeyaraj, P. Chronic Recurrent Temporomandibular Joint Dislocation: A Comparison of Various Surgical Treatment Options, and Demonstration of the Versatility and Efficacy of the Dautrey’s Procedure. J. Maxillofac. Oral Surg. 17, 95–106 (2018). https://doi.org/10.1007/s12663-017-1019-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12663-017-1019-6