Abstract
Purpose
Chronic pain is a common condition affecting almost one in five Canadians. One of the methods used to treat chronic pain is injection therapies. While they are considered relatively safe procedures, they do carry inherent risk that can result in adverse events. Our goal was to investigate these patient safety events to identify themes that could be used to shape practice guidelines and standards and improve patient safety.
Methods
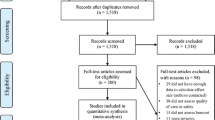
We looked at closed civil legal actions and regulatory college complaints associated with injection therapies for chronic pain in the Canadian Medical Protection Association database from 2015 to 2019. Injury was defined as that arising from, or associated with, plans or actions taken during the provision of health care, rather than an underlying disease or injury.
Results
Of the 91 cases identified, the most common reported complications were neurologic-related symptoms, injury, and infection. Fifty-eight percent (53/91) of patients experienced health care-related harm that had a negative effect on their health or quality of life. Peer experts were critical of the clinical care provided in 74% (67/91) of the cases. Provider-related (60%, 40/67), team-related (75%, 50/67), and system-related factors (21%, 14/67) were identified as contributing factors in these cases. Common examples of provider-related factors were deficiencies in clinical decision-making (48%, 19/40), failure to follow established procedures (43%, 17/40), and situational awareness (38%, 15/40). Common examples of team-related factors were deficiencies in medical record keeping (80%, 40/50) and communication breakdowns (56%, 28/50). All system-related factors were related to inadequate office procedures.
Conclusion
We recommend that clinicians conduct appropriate physical examinations, keep up-to-date with clinical standards, and ensure their documentation reflects their assessment, the patient’s condition, and the treatment rationale.
Résumé
Objectif
La douleur chronique est une affection courante qui touche près d’une personne sur cinq au Canada. Les traitements par injections constituent l’une des méthodes utilisées pour traiter la douleur chronique. Bien que ces thérapies soient considérées comme des interventions relativement sécuritaires, elles comportent des risques inhérents qui peuvent entraîner des événements indésirables. Notre objectif était d’examiner ces événements liés à la sécurité des patient·es afin de cerner les thèmes qui pourraient être utilisés pour façonner les lignes directrices et les normes de pratique et améliorer la sécurité des patient·es.
Méthode
Nous avons examiné les poursuites civiles fermées et les plaintes aux ordres de réglementation associées aux traitements par injection pour la douleur chronique dans la base de données de l’Association canadienne de protection médicale entre 2015 et 2019. Était considérée comme blessure toute lésion découlant de ou associée à des plans mis en place ou des mesures prises pendant la prestation de soins de santé, plutôt que comme une maladie ou une blessure sous-jacente.
Résultats
Sur les 91 cas identifiés, les complications les plus fréquemment signalées étaient des symptômes, des blessures et des infections neurologiques. Cinquante-huit pour cent (53/91) des patient·es ont subi des préjudices liés aux soins de santé qui ont eu un effet négatif sur leur santé ou leur qualité de vie. Les expert·es ont critiqué les soins cliniques fournis dans 74 % (67/91) des cas. Les facteurs liés aux prestataires (60 %, 40/67), à l’équipe (75 %, 50/67) et au système (21 %, 14/67) ont été identifiés comme des facteurs contributifs dans ces cas. Les exemples courants de facteurs liés aux prestataires comportaient les lacunes dans la prise de décision clinique (48 %, 19/40), le non-respect des procédures établies (43 %, 17/40) et la conscience situationnelle (38 %, 15/40). Les lacunes dans la tenue des dossiers médicaux (80 %, 40/50) et les problèmes de communication (56 %, 28/50) comptaient parmi les exemples courants de facteurs liés à l’équipe. Tous les facteurs identifiés comme étant systémiques étaient liés à des procédures administratives inadéquates.
Conclusion
Nous recommandons aux cliniciennes et cliniciens de réaliser des examens physiques appropriés, de se tenir au courant des normes cliniques et de s’assurer que leur documentation reflète leur évaluation, l’état du/de la patient·e et la justification du traitement.


Similar content being viewed by others
References
Campbell F, Hudspith M, Choinière M, et al. An action plan for pain in Canada, 2021. Available from URL: https://www.canada.ca/en/health-canada/corporate/about-health-canada/public-engagement/external-advisory-bodies/canadian-pain-task-force/report-2021.html (accessed February 2023).
World Health Organization. ICD-11 for mortality and morbidity statistics, 2023. Available from URL: https://icd.who.int/browse11/l-m/en#/http%3a%2f%2fid.who.int%2ficd%2fentity%2f1581976053 (accessed February 2023).
Van Damme S, Becker S, Van der Linden D. Tired of pain? Toward a better understanding of fatigue in chronic pain. Pain 2018; 159: 7–10. https://doi.org/10.1097/j.pain.0000000000001054
Hylands-White N, Duarte R, Raphael J. An overview of treatment approaches for chronic pain management. Rheumatol Int 2017; 37: 29–42. https://doi.org/10.1007/s00296-016-3481-8
American Academy of Family Physicians. AAFP chronic pain toolkit. Available from URL: https://www.aafp.org/dam/AAFP/documents/patient_care/pain_management/cpm-toolkit.pdf (accessed February 2023).
Pain Management Best Practices Inter-Agency Task Force. Pain management best practices inter-agency task force report: updates, gaps, inconsistencies, and recommendations, 2019. Available from URL: https://www.hhs.gov/sites/default/files/pain-mgmt-best-practices-draft-final-report-05062019.pdf (accessed February 2023).
Manchikanti L, Pampati V, Falco FJ, Hirsch JA. Growth of spinal interventional pain management techniques: analysis of utilization trends and Medicare expenditures 2000 to 2008. Spine (Phila Pa 1976) 2013; 38: 157–68. https://doi.org/10.1097/brs.0b013e318267f463
Manchikanti L, Pampati V, Falco FJ, Hirsch JA. Assessment of the growth of epidural injections in the medicare population from 2000 to 2011. Pain Physician 2013; 16: E349–64.
Manchikanti L, Pampati V, Hirsch JA. Utilization of interventional techniques in managing chronic pain in medicare population from 2000 to 2014: an analysis of patterns of utilization. Pain Physician 2016; 19: E531–46.
Shanthanna H, Bhatia A, Radhakrishna M, et al. Interventional pain management for chronic pain: a survey of physicians in Canada. Can J Anesth 2020; 67: 343–52. https://doi.org/10.1007/s12630-019-01547-w
Deng G, Gofeld M, Reid JN, Welk B, Agur AM, Loh E. A retrospective cohort study of healthcare utilization associated with paravertebral blocks for chronic pain management in Ontario. Can J Pain 2021; 5: 130–8. https://doi.org/10.1080/24740527.2021.1929883
Manchikanti L, Hirsch JA, Pampati V, Boswell MV. Utilization of facet joint and sacroiliac joint interventions in Medicare population from 2000 to 2014: explosive growth continues! Curr Pain Headache Rep 2016; 20: 58. https://doi.org/10.1007/s11916-016-0588-2
Manchikanti L, Hirsch JA. Neurological complications associated with epidural steroid injections. Curr Pain Headache Rep 2015; 19: 482. https://doi.org/10.1007/s11916-015-0482-3
McGrath JM, Schaefer MP, Malkamaki DM. Incidence and characteristics of complications from epidural steroid injections. Pain Med 2011; 12: 726–31. https://doi.org/10.1111/j.1526-4637.2011.01077.x
Edlow BL, Wainger BJ, Frosch MP, Copen WA, Rathmell JP, Rost NS. Posterior circulation stroke after C1-C2 intraarticular facet steroid injection: evidence for diffuse microvascular injury. Anesthesiology 2010; 112: 1532–5. https://doi.org/10.1097/aln.0b013e3181d7b15a
Epstein N. The risks of epidural and transforaminal steroid injections in the spine: commentary and a comprehensive review of the literature. Surg Neurol Int 2013; 4: S74–93. https://doi.org/10.4103/2152-7806.109446
Abrecht CR, Saba R, Greenberg P, Rathmell JP, Urman RD. A contemporary medicolegal analysis of outpatient interventional pain procedures: 2009-2016. Anesth Analg 2019; 129: 255–62. https://doi.org/10.1213/ane.0000000000004096
Abrecht CR, Greenberg P, Song E, Urman RD, Rathmell JP. A contemporary medicolegal analysis of implanted devices for chronic pain management. Anesth Analg 2017; 124: 1304–10. https://doi.org/10.1213/ane.0000000000001702
Rathmell JP, Michna E, Fitzgibbon DR, Stephens LS, Posner KL, Domino KB. Injury and liability associated with cervical procedures for chronic pain. Anesthesiology 2011; 114: 918–26. https://doi.org/10.1097/aln.0b013e31820fc7f2
Cranshaw J, Gupta KJ, Cook TM. Litigation related to drug errors in anaesthesia: an analysis of claims against the NHS in England 1995–2007. Anaesthesia 2009; 64: 1317–23. https://doi.org/10.1111/j.1365-2044.2009.06107.x
Canadian Medical Protection Association. Who we are. Available from URL: https://www.cmpa-acpm.ca/en/about/who-we-are (accessed February 2023).
Canadian Medical Protection Association. What we do. Available from URL: https://www.cmpa-acpm.ca/en/about/what-we-do (accessed February 2023).
Crosby ET, Duggan LV, Finestone PJ, Liu R, De Gorter R, Calder LA. Anesthesiology airway-related medicolegal cases from the Canadian Medical Protection Association. Can J Anesth 2021; 68: 183–95. https://doi.org/10.1007/s12630-020-01846-7
Calder LA, Whyte EM, Neilson HK, Zhang C, Barry TK, Barry SP. Trends and contributing factors in medico-legal cases involving spine surgery. Spine (Phila Pa 1976) 2022; 47: E469–76. https://doi.org/10.1097/brs.0000000000004332
Zhang Z, Calder L, Finestone PJ, Liu R, Bucevska M, Arneja JS. Medico-legal closed case trends in Canadian plastic surgery: a retrospective descriptive study. Plast Reconstr Surg Glob Open 2021; 9: e3754. https://doi.org/10.1097/gox.0000000000003754
Calder LA, Neilson HK, Whyte EM, Ji J, Bhatia RS. Medico-legal cases involving cardiologists and cardiac test underuse or overuse. CJC Open 2020; 3: 434–41. https://doi.org/10.1016/j.cjco.2020.11.018
McCleery A, Devenny K, Ogilby C, et al. Using medicolegal data to support safe medical care: a contributing factor coding framework. J Healthc Risk Manag 2019; 38: 11–8. https://doi.org/10.1002/jhrm.21348
Hoppes M, Mitchell J. Serious safety events: a focus on harm classification: deviation in care as link, 2014. Available from URL: https://www.ashrm.org/sites/default/files/ashrm/SSE-2_getting_to_zero-9-30-14.pdf (accessed February 2023).
Canadian Medical Protection Association. Documentation and record keeping, 2021. Available from URL: https://www.cmpa-acpm.ca/en/education-events/good-practices/physician-patient/documentation-and-record-keeping (accessed February 2023).
American Society of Anesthesiologists. Statement on documentation of anesthesia care, 2018. Available from URL: https://www.asahq.org/standards-and-guidelines/statement-on-documentation-of-anesthesia-care (accessed February 2023).
Blome A, Yu D, Lu X, Schreyer KE. Pitfalls of extensive documentation in the emergency department. Ochsner J 2020; 20: 299–302. https://doi.org/10.31486/toj.19.0108
Hripcsak G, Vawdrey DK, Fred MR, Bostwick SB. Use of electronic clinical documentation: time spent and team interactions. J Am Med Inform Assoc 2011; 18: 112–7. https://doi.org/10.1136/jamia.2010.008441
Siegler JE, Patel NN, Dine CJ. Prioritizing paperwork over patient care: why can’t we do both? J Grad Med Educ 2015; 7: 16–8. https://doi.org/10.4300/jgme-d-14-00494.1
Cusack CM, Hripcsak G, Bloomrosen M, et al. The future state of clinical data capture and documentation: a report from AMIA’s 2011 policy meeting. J Am Med Inform Assoc 2013; 20: 134–40. https://doi.org/10.1136/amiajnl-2012-001093
Brull R, McCartney CJL, Chan VW, et al. Disclosure of risks associated with regional anesthesia: a survey of academic regional anesthesiologists. Reg Anesth Pain Med 2007; 32: 7–11. https://doi.org/10.1016/j.rapm.2006.07.005
Huang C, Wasserman D. Considering consent to research for patients in chronic pain and with mental illnesses. Am J Bioeth 2017; 17: 51–2. https://doi.org/10.1080/15265161.2017.1388877
Tait RC. Vulnerability in clinical research with patients in pain: a risk analysis. J Law Med Ethics 2009; 37: 59–72. https://doi.org/10.1111/j.1748-720x.2009.00351.x
Hughes J, Greville-Harris M, Graham CA, Lewith G, White P, Bishop FL. What trial participants need to be told about placebo effects to give informed consent: a survey to establish existing knowledge among patients with back pain. J Med Ethics 2017; 43: 867–70. https://doi.org/10.1136/medethics-2016-103964
Kinnersley P, Phillips K, Savage K, et al. Interventions to promote informed consent for patients undergoing surgical and other invasive healthcare procedures. Cochrane Database Syst Rev 2013; 7: CD009445. https://doi.org/10.1002/14651858.cd009445.pub2
Glaser J, Nouri S, Fernandez A, et al. Interventions to improve patient comprehension in informed consent for medical and surgical procedures: an updated systematic review. Med Decis Making 2020; 40: 119–43. https://doi.org/10.1177/0272989x19896348
Lie HC, Juvet LK, Street RL, et al. Effects of physicians’ information giving on patient outcomes: a systematic review. J Gen Intern Med 2022; 37: 651–63. https://doi.org/10.1007/s11606-021-07044-5
Bennett DL, Dharia C v., Ferguson KJ, Okon AE. Patient-physician communication: informed consent for imaging-guided spinal injections. J Am Coll Radiol 2009; 6: 38–44. https://doi.org/10.1016/j.jacr.2008.08.004
Bajada S, Dwamena S, Abdul Z, Williams R, Ennis O. Improving consent form documentation and introduction of procedure-specific labels in a district general hospital. BMJ Qual Improv Rep 2017; 6: u211571.w4730. https://doi.org/10.1136/bmjquality.u211571.w4730
Hurley RW, Adams MC, Barad M, et al. Consensus practice guidelines on interventions for cervical spine (facet) joint pain from a multispecialty international working group. Reg Anesth Pain Med 2022; 47: 3–59. https://doi.org/10.1136/rapm-2021-103031
American Society of Anesthesiologists Task Force on Chronic Pain Management, American Society of Regional Anesthesia and Pain Medicine. Practice guidelines for chronic pain management: an updated report by the American Society of Anesthesiologists Task Force on Chronic Pain Management and the American Society of Regional Anesthesia and Pain Medicine. Anesthesiology 2010; 112: 810–33. https://doi.org/10.1097/aln.0b013e3181c43103
Manchikanti L, Kaye AD, Soin A, et al. Comprehensive evidence-based guidelines for facet joint interventions in the management of chronic spinal pain: American Society of Interventional Pain Physicians (ASIPP) guidelines. Pain Physician 2020; 23: S1–127.
Eloqayli H. Clinical decision-making in chronic spine pain: dilemma of image-based diagnosis of degenerative spine and generation mechanisms for nociceptive, radicular, and referred pain. Biomed Res Int 2018; 2018: 8793843. https://doi.org/10.1155/2018/8793843
Ahiskalioglu EO, Alici HA, Dostbil A, Celik M, Ahiskalioglu A, Aksoy M. Pneumothorax after trigger point injection: a case report and review of literature. J Back Musculoskelet Rehabil 2016; 29: 895–7. https://doi.org/10.3233/BMR-160666
Sato S, Tachibana S, Okazaki K, Namba H, Ichimiya T, Yamakage M. Careful medical interview and ultrasonography enabled detection of acute kidney injury and hematoma after lumbar trigger point injection-a case report. JA Clin Rep 2021; 7: 12. https://doi.org/10.1186/s40981-021-00416-0
Genç S, Eneyli MG, Polat O, Oğuz AB, Enön S. Hemopneumothorax after trigger point injection for fibromyalgia. Altern Ther Health Med 2020; 26: 62–4.
Schultz DM, Hagedorn JM, Abd-Elsayed A, Stayner S. Safety of interlaminar cervical epidural injections: experience with 12,168 procedures in a single pain clinic. Pain Physician 2022; 25: 49–58.
Bicket MC, Chakravarthy K, Chang D, Cohen SP. Epidural steroid injections: An updated review on recent trends in safety and complications. Pain Manag 2015; 5: 129–46. https://doi.org/10.2217/pmt.14.53
Manchikanti L, Malla Y, Wargo BW, Cash KA, Pampati V, Fellows B. A prospective evaluation of complications of 10,000 fluoroscopically directed epidural injections. Pain Physician 2012; 15: 131–40.
Shanthanna H, Park J. Acute epidural haematoma following epidural steroid injection in a patient with spinal stenosis. Anaesthesia 2011; 66: 837–9. https://doi.org/10.1111/J.1365-2044.2011.06770.X
Manchikanti L, Malla Y, Warge BW, Cash KA, Pampati V, Fellows B. Complications of fluoroscopically directed facet joint nerve blocks: a prospective evaluation of 7,500 episodes with 43,000 nerve blocks. Pain Physician 2012; 15: E143–50.
Weingarten TN, Hooten WM, Huntoon MA. Septic facet joint arthritis after a corticosteroid facet injection. Pain Med 2006; 7: 52–6. https://doi.org/10.1111/j.1526-4637.2006.00089.x
Fayeye O, Silva AH, Chavda S, Furtado NR. Subdural empyema following lumbar facet joint injection: an exceeding rare complication. Neurol Neurochir Pol 2016; 50: 203–6. https://doi.org/10.1016/J.PJNNS.2016.01.013
Kim SY, Han SH, Jung MW, Hong JH. Generalized infection following facet joint injection: a case report. Korean J Anesthesiol 2010; 58: 401–4. https://doi.org/10.4097/kjae.2010.58.4.401
Kim BR, Lee JW, Lee E, Kang Y, Ahn JM, Kang HS. Intra-articular facet joint steroid injection–related adverse events encountered during 11,980 procedures. Eur Radiol 2020; 30: 1507–16. https://doi.org/10.1007/s00330-019-06483-3
Goel V, Patwardhan AM, Ibrahim M, Howe CL, Schultz DM, Shankar H. Complications associated with stellate ganglion nerve block: a systematic review. Reg Anesth Pain Med 2019; 44: 669–78. https://doi.org/10.1136/rapm-2018-100127
Shankar H, Simhan S. Transient neuronal injury followed by intravascular injection during an ultrasound guided stellate ganglion block. Anesth Pain 2013; 2: 134–41. https://doi.org/10.5812/aapm.7823
Pennekamp W, Krumova EK, Feigl GP, et al. Permanent lesion of the lateral femoral cutaneous nerve after low-volume ethanol 96% application on the lumbar sympathetic chain. Pain Physician 2013; 16: 391–7.
Nagpal A, Eckmann M, Small S, Stevens S. Onset of spontaneous lower extremity pain after lumbar sympathetic block. Pain Physician 2015; 18: E89–91.
Author contributions
Emma MacLean contributed to analysis and drafting of the article. Gary Garber contributed to data acquisition and analysis, interpretation of data, and drafting the article. Kate Barbosa contributed to data acquisition and analysis, interpretation of data, and drafting the article. Richard Liu contributed to data acquisition and analysis, interpretation of data, and drafting the article. Allison Verge contributed to conception of the article and review of the manuscript. Karim Mukhida contributed to conception of the article, review of the data, and drafting the article.
Acknowledgements
Emma MacLean’s work on this project was supported by a Research in Medicine studentship provided by the Faculty of Medicine at Dalhousie University, Halifax, NS, Canada.
Disclosures
None of the authors have any conflicts of interest to declare.
Funding statement
This study was not funded.
Editorial responsibility
This submission was handled by Dr. Philippe Richebé, Associate Editor, Canadian Journal of Anesthesia/Journal canadien d’anesthésie.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
MacLean, E., Garber, G., Barbosa, K. et al. Lessons learned from examination of Canadian medico-legal cases related to interventional therapies for chronic pain management. Can J Anesth/J Can Anesth 70, 1504–1515 (2023). https://doi.org/10.1007/s12630-023-02531-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12630-023-02531-1