Abstract
Purpose
Hospitalized patients with cancer who experience cardiopulmonary arrest have historically low survival rates. This retrospective cohort study describes outcomes of patients at a large Canadian cancer centre who had a “code medical emergency” activated, and the use of pragmatic criteria to identify patients with poor survival following resuscitation.
Methods
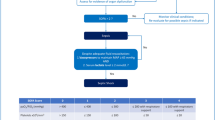
We included hospitalized patients with cancer who had a “code blue” activated between January 2007 and December 2018. Our primary outcome was intensive care unit (ICU) mortality. We developed pragmatic criteria to identify patients with “poor prognosis” for survival from cardiopulmonary resuscitation (CPR) based on disease status and candidacy for further cancer treatment. We used descriptive statistics to analyze the outcomes of poor prognosis patients.
Results
Two hundred and twenty-five patients had a code blue activated. The median age was 61 yr, 52% were male, and 48% had a solid tumour. Overall, 173/225 (77%) patients survived the code blue; 164 were admitted to the ICU, where 49% (81/164) died; 31% survived to hospital discharge; and 16% (n = 27) were alive at one year. One hundred and twenty out of 225 (53%) required chest compressions; spontaneous circulation returned in 61% (73/120), and 12% (14/120) survived to hospital discharge. Patients meeting “poor prognosis” criteria (114, 51%) were more likely to die in the ICU (64% vs 35%; P < 0.001) or in hospital (86% vs 59%; P < 0.001), and more often had goals-of-care discussions prior to the code blue (46% vs 7%; P < 0.001). At one year, only 2% of poor prognosis patients were alive, compared with 24% of patients who did not meet any poor prognosis criteria.
Conclusion
Hospitalized patients with cancer requiring CPR have poor hospital and long-term outcomes. The proposed set of pragmatic criteria may be useful to identify patients unlikely to benefit from CPR and life support, to trigger early goals of care discussions, and to avoid potentially goal-discordant interventions.
Résumé
Objectif
Les patient·es hospitalisé·es atteint·es d’un cancer qui subissent un arrêt cardiorespiratoire ont des taux de survie historiquement bas. Cette étude de cohorte rétrospective décrit les issues des patient·es d’un grand centre canadien de cancérologie pour qui un « code d’urgence médicale » a été activé et l’utilisation de critères pragmatiques pour identifier les patient·es ayant une faible survie après réanimation.
Méthode
Nous avons inclus les personnes hospitalisées atteintes d’un cancer pour qui un « code bleu » avait été activé entre janvier 2007 et décembre 2018. Notre critère d’évaluation principal était la mortalité à l’unité de soins intensifs (USI). Nous avons développé des critères pragmatiques pour identifier les personnes ayant un « mauvais pronostic » de survie à la réanimation cardiorespiratoire (RCR) en fonction de l’état de la maladie et de leur éligibilité à un traitement ultérieur contre le cancer. Nous avons utilisé des statistiques descriptives pour analyser les issues des patient·es ayant un mauvais pronostic.
Résultats
Un code bleu a été activé pour deux cent vingt-cinq patient·es. L’âge médian était de 61 ans, 52 % étaient des hommes et 48 % avaient une tumeur solide. Dans l’ensemble, 173/225 (77 %) patient·es ont survécu au code bleu; 164 ont été admis·es aux soins intensifs, où 49 % (81/164) sont décédé·es; 31 % ont survécu jusqu’à leur congé de l’hôpital; et 16 % (n = 27) étaient en vie après un an. Cent vingt sur 225 (53 %) ont nécessité des compressions thoraciques; la circulation spontanée est revenue chez 61 % (73/120), et 12 % (14/120) ont survécu jusqu’à leur congé de l’hôpital. Les patient·es répondant aux critères de « mauvais pronostic » (114, 51 %) étaient plus susceptibles de mourir à l’USI (64 % vs 35 %; P < 0,001) ou à l’hôpital (86 % vs 59 %; P < 0,001) et avaient plus souvent eu des discussions sur les objectifs de soins avant l’activation du code bleu (46 % vs 7 %; P < 0,001). À un an, seulement 2 % des patient·es ayant un mauvais pronostic étaient en vie, contre 24 % des patient·es qui ne présentaient aucun critère de mauvais pronostic.
Conclusion
Les personnes hospitalisées atteintes d’un cancer nécessitant une RCR ont de mauvaises issues intra-hospitalières et à plus long terme. L’ensemble de critères pragmatiques proposé peut être utile pour identifier la patientèle peu susceptible de bénéficier de la RCR et du maintien des fonctions vitales, pour amorcer rapidement des discussions sur les objectifs de soins et pour éviter les interventions potentiellement discordantes par rapport à ces objectifs.

Similar content being viewed by others
References
Zhu A, Zhang J. Meta-analysis of outcomes of the 2005 and 2010 cardiopulmonary resuscitation guidelines for adults with in-hospital cardiac arrest. Am J Emerg Med 2016; 34: 1133–9. https://doi.org/10.1016/j.ajem.2016.03.008
Ebell MH, Afonso AM. Pre-arrest predictors of failure to survive after in-hospital cardiopulmonary resuscitation: a meta-analysis. Fam Pract 2011; 28: 505–15. https://doi.org/10.1093/fampra/cmr023
Reisfield GM, Wallace SK, Munsell MF, Webb FJ, Alvarez ER, Wilson GR. Survival in cancer patients undergoing in-hospital cardiopulmonary resuscitation: a meta-analysis. Resuscitation 2006; 71: 152–60. https://doi.org/10.1016/j.resuscitation.2006.02.022
Ewer MS, Kish SK, Martin CG, Price KJ, Feeley TW. Characteristics of cardiac arrest in cancer patients as a predictor of survival after cardiopulmonary resuscitation. Cancer 2001; 92: 1905–12. https://doi.org/10.1002/1097-0142(20011001)92:7%3C1905::aid-cncr1708%3E3.0.co;2-6
Vitelli CE, Cooper K, Rogatko A, Brennan MF. Cardiopulmonary resuscitation and the patient with cancer. J Clin Oncol 1991; 9: 111–5. https://doi.org/10.1200/jco.1991.9.1.111
Miller AH, Sandoval M, Wattana M, Page VD, Todd KH. Cardiopulmonary resuscitation outcomes in a cancer center emergency department. Springerplus 2015; 4: 106. https://doi.org/10.1186/s40064-015-0884-z
Becker G, Sarhatlic R, Olschewski M, Xander C, Momm F, Blum HE. End-of-life care in hospital: current practice and potentials for improvement. J Pain Symptom Manage 2007; 33: 711–9. https://doi.org/10.1016/j.jpainsymman.2006.09.030
Finan M, Stoudt K, Canecchia L, et al. Suitability and outcomes of cardiopulmonary resuscitation in cancer patients at a tertiary oncology center. Am J Respir Crit Care Med 2017; 195: A5035.
Choi Y, Kim JW, Suh KJ, et al. Identification of a potentially avoidable cardiopulmonary resuscitation in hematology and oncology wards. BMC Palliat Care 2019; 18: 93. https://doi.org/10.1186/s12904-019-0477-7
Bestvina CM, Polite BN. Implementation of advance care planning in oncology: a review of the literature. J Oncol Pract 2017; 13: 657–62. https://doi.org/10.1200/jop.2017.021246
Varon J, Marik PE. Cardiopulmonary resuscitation in patients with cancer. Am J Hosp Palliat Med 2007; 24: 224–9. https://doi.org/10.1177/1049909107301485
Wright AA, Zhang B, Ray A, et al. Associations between end-of-life discussions, patient mental health, medical care near death, and caregiver bereavement adjustment. JAMA 2008; 300: 1665–73. https://doi.org/10.1001/jama.300.14.1665
Caissie A, Kevork N, Hannon B, Le LW, Zimmermann C. Timing of code status documentation and end-of-life outcomes in patients admitted to an oncology ward. Support Care Cancer 2014; 22: 375–81. https://doi.org/10.1007/s00520-013-1983-4
Spring J, McKinlay J, Puxty K, et al. Perspectives on advance care planning for patients with hematologic malignancies: an international clinician questionnaire. Ann Am Thorac Soc 2021; 18: 1533–9. https://doi.org/10.1513/annalsats.202006-678oc
Bernacki RE, Block SD. Communication about serious illness care goals: a review and synthesis of best practices. JAMA Intern Med 2014; 174: 1994–2003. https://doi.org/10.1001/jamainternmed.2014.5271
Epstein AS, Volandes AE, Chen LY, et al. A randomized controlled trial of a cardiopulmonary resuscitation video in advance care planning for progressive pancreas and hepatobiliary cancer patients. J Palliat Med 2013; 16: 623–31. https://doi.org/10.1089/jpm.2012.0524
Volandes AE, Paasche-Orlow MK, Mitchell SL, et al. Randomized controlled trial of a video decision support tool for cardiopulmonary resuscitation decision making in advanced cancer. J Clin Oncol 2013; 31: 380–6. https://doi.org/10.1200/jco.2012.43.9570
Stein RA, Sharpe L, Bell ML, Boyle FM, Dunn SM, Clarke SJ. Randomized controlled trial of a structured intervention to facilitate end-of-life decision making in patients with advanced cancer. J Clin Oncol 2013; 31: 3403–10. https://doi.org/10.1200/jco.2011.40.8872
Clayton JM, Butow PN, Tattersall MH, et al. Randomized controlled trial of a prompt list to help advanced cancer patients and their caregivers to ask questions about prognosis and end-of-life care. J Clin Oncol 2007; 25: 715–23. https://doi.org/10.1200/jco.2006.06.7827
Bruckel JT, Wong SL, Chan PS, Bradley SM, Nallamothu BK. Patterns of Resuscitation care and survival after in-hospital cardiac arrest in patients with advanced cancer. J Oncol Pract 2017; 13: 821–30. https://doi.org/10.1200/jop.2016.020404
Khasawneh FA, Kamel MT, Abu-Zaid MI. Predictors of cardiopulmonary arrest outcome in a comprehensive cancer center intensive care unit. Scand J Trauma Resusc Emerg Med 2013; 21: 18. https://doi.org/10.1186/1757-7241-21-18
Zafar W, Ghafoor I, Jamshed A, Gul S, Hafeez H. Outcomes of in-hospital cardiopulmonary resuscitation among patients with cancer: experience from Pakistan. Am J Hosp Palliat Med 2017; 34: 212–6. https://doi.org/10.1177/1049909115617934
Author contributions
Sangeeta Mehta, Laveena Munshi, and Santhosh Thyagu contributed to the study conception and design. Material was prepared by Sumesh Shah. Data were collected and analyzed by Sabrina H. M. Yeung and Ramy Boles. Data were collected by Sarah Seedon and Mobolaji Moore. The first draft of the manuscript was written by Sabrina H. M. Yeung and Ramy Boles and all authors commented on previous versions of the manuscript.
Disclosures
None.
Funding statement
No funding received.
Prior conference presentations
Critical Care Canada Forum 2019 (Toronto, ON, Canada; 10–13 November 2019); Can J Anesth 2020; 67: S135–6; https://doi.org/10.1007/s12630-019-01552-z
Editorial responsibility
This submission was handled by Dr. Patricia S. Fontela, Associate Editor, Canadian Journal of Anesthesia/Journal canadien d’anesthésie.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yeung, S.H.M., Boles, R., Munshi, L. et al. Resuscitation outcomes in patients with cancer: experience in a large urban cancer centre. Can J Anesth/J Can Anesth 70, 1234–1243 (2023). https://doi.org/10.1007/s12630-023-02505-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12630-023-02505-3