Abstract
Objective
Surgeries for cancer of the esophagus are still associated with a high rate of postoperative morbidity. There are few reports of perioperative nutritional support for patients undergoing esophageal cancer surgery, and there is insufficient evidence to recommend routine use of immunonutrition in these patients. The aim of this study was to determine whether preoperative immunonutrition positively influences key clinical outcomes such as postoperative infectious complications, mortality, length of hospital stay, and short-term survival in this population.
Design and Setting
We undertook a retrospective investigation of the effects of preoperative nutritional support on the postoperative course of esophageal cancer surgery at the Department of Gastroenterological Surgery, International University of Health and Welfare Mita Hospital, Tokyo, Japan.
Participants
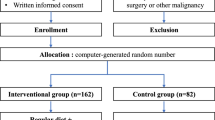
Fifty-five patients who underwent esophagectomy for esophageal cancer were included in this study. Of the 55 patients, 26 patients consumed a liquid dietary supplement (IMPACT group) before surgery and 29 patients did not (STANDARD group).
Intervention
Before surgery, the IMPACT group consumed 750 ml (3 packs)/day of Impact® for 5 consecutive days.
Measurements
The analysis was based on postoperative complications, hospital mortality, length of hospital stay, and short-term survival.
Results
Significantly fewer patients developed postoperative infections in the IMPACT group compared with the STANDARD group (p=.007): 4 of 21 patients in the IMPACT group and 10 of 29 patients in the STANDARD group. Either an infectious complication or another complication developed in 8 patients in the IMPACT group and 13 patients in the STANDARD group, with the result that 6 patients in the STANDARD group died of postoperative complications (p=.001). The duration of hospitalization was 34 days in the IMPACT group and 48 days in the STANDARD group; hence, hospitalization was significantly shorter in patients treated with Impact® (p=.008). The mean 6-month survival rates for the IMPACT group and the STANDARD group were 92% (24/26) and 72% (21/29), respectively (p=.028).
Conclusion
Simple preoperative supplementation significantly improved outcome. Administration of the supplemental diet before esophageal surgery appeared to be an effective strategy in reducing infectious complications, mortality, and hospitalization, and improving short-term survival.
Similar content being viewed by others
References
Daly JM, Lieberman MD, Goldfine J, Shou J, Weitraub F, Rosato EF, Lavin P (1992) Enteral nutrition with supplemental arginine, RNA, and omega 3 fatty acids in patients after operation. Immunologic, metabolic and clinical outcome. Surgery 112:56–67
Gianotti L, Braga M, Vignali A, Balzano G, Zerbi A, Bisagni P, Di Carlo V (1997) Effect of route of delivery and formulation of postoperative nutritional support in patients undergoing major operations for malignant neoplasm. Arch Surg 132:1222–1230
Senkal M, Mumme A, Eickhoff U, Geier B, Spath G, Wulfert D, Joosten U, Frei A, Kemen M (1997) Early postoperative immunonutrition: clinical outcome and costcomparison analysis in surgical patients. Crit Care Med 25:1489–1496
Braga M, Gianotti L, Radaelli G, Vignali A, Mari G, Gentilini O, Di Carlo V (1999) Perioperative immunonutrition in patients undergoing cancer surgery. Results of a rabdomized double-blind phase 3 trial. Arch Surg 134:428–433
Senkal M, Zumtobei V, Bauer KH, Marpe B, Wolfram G, Frei A, Eickhoff U, Kemen M (1999) Outcome and cost-effectiveness of perioperative enteral immunonutrition in patients undergoing elective upper gastrointestinal tract surgery: a prospective randomized study. Arch Surg 134:1309–1316
Gianotti L, Braga M, Nespoli L, Radaelli G, Beneduce A, Di Carlo V (2002) A randomized controlled trial of preoperative oral supplementation with a specialized diet in patients with gastrointestinal cancer. Gastroenterology 122:1763–1770
Braga M, Gianotti L, Nespoli L, Radaelli G, Di Carlo V (2002) Nutritional approach in malnourished surgical patients. A prospective randomized study. Arch Surg 137:174–180
Mudge L, Isenring E, Jamieson GG (2011) Immunonutrition in patients undergoing esophageal cancer resection. Dis Esophagus 24:160–165
Nakamura M, Iwahashi M, Takifuji K, nakamori M, Naka T, Ishida K, Ojima T, Iida T, Katsuda M, hayata K, Yamaue H (2009) Optimal dose of preoperative enteral immunonutrition for patients with esophageal cancer. Surg Today 39:855–860
Takeuchi H, Ikeuchi S, Kawaguchi Y, Kitagawa Y, Isobe Y, Kubochi K, Kitajima M, Matsumoto S (2007) Clinical significance of perioperative immunonutrition for patients with esophageal cancer. World J Surg 31:2160–2167
Sakurai Y, Masui T, Yoshida I, Tonomura S, Shoji M, Nakamura Y, Isogaki J, Uyama I, Komori Y, Ochiai M (2007) Randomized clinical trial of the effects of perioperative use of immune-enhancing enteral formula on metabolic and immunological status in patients undergoing esophagectomy. World J Surg 31:2150–2157
The Japan Esophageal Society (2009) Japanese Classification of Esophageal Cancer, tenth edition: part I. Esophagus 6:1–25
Ando N, Kato H, Igaki H, Shinoda M, Ozawa S, Shimizu H, Nakamura T, Yabusaki H, Aoyama N, Kurita A, Ikeda K, Kanda T, Tsujinaka T, Nakamura K, Fukuda H (2012) A randomized trial comparing postoperative adjuvant chemotherapy with cisplatin and 5- fluorouracil versus preoperative chemotherapy for localized advanced squamous cell carcinoma of the thoracic esophagus (JCOG9907). Ann Surg Oncol 19:68–74
ASPEN Board of Directors and the Clinical Guidelines Task Force (2002) Guidelines for the use parenteral and enteral nutrition in adult and pediatric patients. J Parenter Enteral Nutr 26:144
American Gastroenterological Association Medical Position Statement (1995) Guidelines for the use of enteral nutrition. Gastroenterology 108:1280–1281
Klein S, Kinney J, Jeejeebhoy K, Alpers D, Hellerstein M, Murray M, Twomey B (1997) Nutritional support in clitical practice: review of the published data and recommendation for future directions. J Parenter Enteral Nutr 21:133–156
Beale RJ, Bryg DJ, Bihari DJ (1999) Immunonutrition in the critically ill: a systematic review of clinical outcome. Crit Care Med 27:2799–2805
Heys S, Walker LG, Smith I, Eremin O (1999) Enteral nutrition supplementation with key nutrients in patients with critical illness and cancer: a meta-analysis of randomized controlled clinical trials. Ann Surg 229:467–477
Braga M, Gianotti L (2005) Preoperative immunonutrition: cost-benefit analysis. J Parenter Enteral Nutr 29:57–61
Miyata H, Yano M, Yasuda T, Hamano R, Yamasaki M, Hou E, Motoori M, Shiraishi O, Tanaka K, Mori M, Doki Y (2012) Randomized study of clinical effect of enteral nutritional support during neoadjuvant chemotherapy on chemotherapy-related toxicity in patients with esophageal cancer. Clin Nutr 31:330–336
Gadsby R (2013) Percutaneous endoscopic gastrostomy (PEG) feeding in elderly people with diabetes resident in nursing homes. J Nutr Health Aging 1:16–18
Kimyagarov S, Turgeman D, Fleissig Y, Klid R, Kopel B, Adunsky A (2013) Percutaneous endoscopic gastrostomy (PEG) tube feeding of nursing home residents is not associated with improved body composition parameters. J Nutr Health Aging 2:162–165
Chang CC (2012) Prevalence and factors associated with feeding difficulty in institutionalized elderly with dementia in Taiwan. J Nutr Health Aging 3:258–261
Zaherah Mohamed Shah F, Suraiya HS, Poi PJH, Tan KS, Lai PSM, Ramakrishnan K, Mahadeva S (2012) Long-term nasogastric tube feeding in elderly stroke patients — an assessment of nutritional adequacy and attitudes to gastrostomy feeding in Asians. J Nutr Health Aging 8:701–706
Waitzberg DL, Saito H, Plank LD, Jamieson GG, Jagannath P, Hwang TL, Mijares JM, Bihari D (2006) Postsurgical infections are reduced with specializd nutrition support. World J Surg 30:1592–1604
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kubota, K., Kuroda, J., Yoshida, M. et al. Preoperative oral supplementation support in patients with esophageal cancer. J Nutr Health Aging 18, 437–440 (2014). https://doi.org/10.1007/s12603-014-0018-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-014-0018-2