Abstract
Background
Tacrolimus, a calcineurin inhibitor, is recommended by the recent guidelines from the Kidney Disease Improving Global Outcomes Group as the first-line treatment for steroid-resistant nephrotic syndrome (SRNS), but its clinical application in China is still limited. We investigated the efficacy and safety of tacrolimus combined with low-dose corticosteroids in a population of Chinese children with SRNS.
Methods
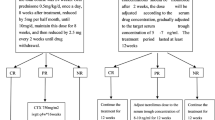
In this prospective non-randomized, non-controlled study, Chinese children with SRNS who failed the previous full-dose prednisone treatment were given tacrolimus (0.1 mg/kg/day) and low-dose prednisone (0.25–0.50 mg/kg/day). We compared the overall remission rate (ORR) and adverse events in the follow-up period with this therapeutic regimen.
Results
A total of 76 children were enrolled into the study with an average follow-up period of 18 ± 6 months (maximum 36 months). ORR achieved by the first, third, and sixth months was 94.7%, 94.7%, and 96.0%, respectively. All patients who attained an initial tacrolimus trough concentration (FK506C0) > 6 ng/mL (60.3%) achieved remission. The relative risk of relapse at FK506C0 < 3 ng/mL compared to 3–6 ng/mL, 6–9 ng/mL, and 9–12 ng/mL was 2.3, 3.2, and 16.9, respectively. During the follow-up period, adverse effects that had been previously reported were rare.
Conclusions
Combination of tacrolimus and low-dose prednisone was safe and effective for the treatment of children with SRNS, with high remission rates observed as early as the first month. Relapses were infrequent, but tended to increase significantly with decreases in FK506C0.
Similar content being viewed by others
References
The primary nephrotic syndrome in children. Identification of patients with minimal change nephrotic syndrome from initial response to prednisone. A report of the International Study of Kidney Disease in Children. J Pediatr. 1981;98:561–4.
Nakanishi K, Iijima K, Ishikura K, Hataya H, Nakazato H, Sasaki S, et al. Two-year outcome of the ISKDC regimen and frequent-relapsing risk in children with idiopathic nephrotic syndrome. Clin J Am Soc Nephrol. 2013;8:756–62.
Wang Y, Dang X, He Q, Zhen Y, He X, Yi Z, et al. Mutation spectrum of genes associated with steroid-resistant nephritic syndrome in Chinese children. Gene. 2017;625:15–20.
Park SJ, Shin JI. Complications of nephrotic syndrome. Korean J Pediatr. 2011;54:322–8.
Mekahli D, Liutkus A, Ranchin B, Yu A, Bessenay L, Girardin E, et al. Long-term outcome of idiopathic steroid-resistant nephrotic syndrome: a multicenter study. Pediatr Nephrol. 2009;24:1525–32.
Kidney Disease Improving Global Outcomes (KDIGO) Glomerulonephritis Work Group. KDIGO Clinical Practice Guideline for Glomerulonephritis. Kidney Inter Suppl. 2012;2:139–274.
Choudhry S, Bagga A, Hari P, Sharma S, Kalaivani M, Dinda A. Efficacy and safety of Tacrolimus versus cyclosporine in children with steroid-resistant nephrotic syndrome: a randomized controlled trial. Am J Kidney Dis. 2009;53:760–9.
Mathieson PW. The podocyte as a target for therapies—new and old. Nat Rev Nephrol. 2011;8:52–6.
Thomson AW, Bonham CA, Zeevi A. Mode of action of Tacrolimus (FK506): molecular and cellular mechanisms. Ther Drug Monit. 1995;17:584–91.
Schönenberger E, Ehrich JH, Haller H, Schiffer M. The podocyte as a direct target of immunosuppressive agents. Nephrol Dial Transplant. 2011;26:18–24.
Faul C, Donnelly M, Merscher-Gomez S, Chang YH, Franz S, Delfgaauw J, et al. The actin cytoskeleton of kidney podocytes is a direct target of the antiproteinuric effect of cyclosporine A. Nat Med. 2008;14:931–8.
Chen W, Liu Q, Liao Y, Yang Z, Chen J, Fu J, et al. Outcomes of tacrolimus therapy in adults with refractory membranous nephrotic syndrome: a prospective, multicenter clinical trial. Am J Med Sci. 2013;345:81–7.
Xu D, Gao X, Bian R, Mei C, Xu C. Tacrolimus improves proteinuria remission in adults with cyclosporine A-resistant or -dependent minimal change disease. Nephrology (Carlton). 2017;22:251–6.
Supavekin S, Surapaitoolkorn W, Kurupong T, Chaiyapak T, Piyaphanee N, Sumboonnanonda A. Tacrolimus in steroid resistant and steroid dependent childhood nephritic syndrome. J Med Assoc Thai. 2013;96:33–40.
Butani L, Rajendra R. Experience with tacrolimus in children with steroid-resistant nephrotic syndrome. Pediatr Nephrol. 2009;24:1517–23.
Morgan C, Sis B, Pinsk M, Yiu V. Renal interstitial fibrosis in children treated with FK506 for nephrotic syndrome. Nephrol Dial Transplant. 2011;26:2860–5.
Flynn JT, Pasko DA. Calcium channel blockers: pharmacology and place in therapy of pediatric hypertension. Pediatr Nephrol. 2000;15:302–16.
Miao L, Sun J, Yuan H, Jia Y, Xu Z. Combined therapy of low-dose tacrolimus and prednisone in nephrotic syndrome with slight mesangial proliferation. Nephrology (Carlton). 2006;11:449–54.
Noone DG, Iijima K, Parekh R. Idiopathic nephrotic syndrome in children. Lancet. 2018;392:61–74.
Jahan A, Prabha R, Chaturvedi S, Mathew B, Fleming D, Agarwal I. Clinical efficacy and pharmacokinetics of tacrolimus in children with steroid-resistant nephrotic syndrome. Pediatr Nephrol. 2015;30:1961–7.
Prasad N, Manjunath R, Rangaswamy D, Jaiswal A, Agarwal V, Bhadauria D, et al. Efficacy and safety of cyclosporine versus tacrolimus in steroid and cyclophosphamide resistant nephrotic syndrome: a prospective study. Indian J Nephrol. 2018;28:46–52.
Qiu TT, Zhang C, Zhao HW, Zhou JW. Calcineurin inhibitors versus cyclophosphamide for idiopathic membranous nephropathy: a systematic review and meta-analysis of 21 clinical trials. Autoimmun Rev. 2017;16:136–45.
Segarra A, Vila J, Pou L, Majó J, Arbós A, Quiles T, et al. Combined therapy of tacrolimus and corticosteroids in cyclosporin-resistant or -dependent idiopathic focal glomerulosclerosis: a preliminary uncontrolled study with prospective follow-up. Nephrol Dial Transplant. 2002;17:655–62.
Duncan N, Dhaygude A, Owen J, Cairns TD, Griffith M, Mclean AG, et al. Treatment of focal and segmental glomerulosclerosis in adults with tacrolimus monotherapy. Nephrol Dial Transplant. 2004;19:3062–7.
Westhoff TH, van der Giet M. Tacrolimus in the treatment of idiopathic nephrotic syndrome. Expert Opin Investig Drugs. 2007;16:1099–110.
Loeffler K, Manjula G, Verna Y. Tacrolimus therapy in pediatric patients with treatment-resistant nephrotic syndrome. Pediatr Nephrol. 2004;19:281–327.
Gulati S, Prasad N, Sharma RK, Kumar A, Gupta A, Baburaj VP. Tacrolimus: a new therapy for steroid-resistant nephrotic syndrome in children. Nephrol Dial Transplant. 2008;23:910–3.
Bhimma R, Adhikari M, Asharam K, Connolly C. Management of steroid-resistant focal segmental glomerulosclerosis in children using tacrolimus. Am J Nephrol. 2006;26:544–51.
Wu B, Mao J, Shen H, Fu H, Wang J, Liu A, et al. Triple immunosuppressive therapy in steroid-resistant nephrotic syndrome children with tacrolimus resistance or tacrolimus sensitivity but frequently relapsing. Nephrology (Carlton). 2015;20:18–24.
Caro J, Gutiérrez-Solís E, Rojas-Rivera J, Aqraz I, Ramos N, Rabasco C, et al. Predictors of response and relapse in patients with idiopathic membranous nephropathy treated with tacrolimus. Nephrol Dial Transplant. 2015;30:467–74.
Brown EA, Upadhyaya K, Hayslett JP, Kashgarian M, Siegel NJ. The clinical course of mesangial proliferative glomerulonephritis. Medicine (Baltimore). 1979;58:295–303.
Shakeel S, Mubarak M, Kazi JI, Lanewala A. The prevalence and clinicopathological profile of IgM nephropathy in children with steroid-resistant nephrotic syndrome at a single centre in Pakistan. J Clin Pathol. 2012;65:1072–6.
Wang W, Xia Y, Mao J, Chen Y, Wang D, Shen H, et al. Treatment of tacrolimus or cyclosporine A in children with idiopathic nephrotic syndrome. Pediatr Nephrol. 2012;27:2073–9.
Troyanov S, Wall CA, Miller JA, Scholey JW, Cattran DC, Toronto Glomerulonephritis Registry Group. Focal and segmental glomerulosclerosis: definition and relevance of a partial remission. J Am Soc Nephrol. 2005;16:1061–8.
Kallash M, Diego A. Efficacy of Tacrolimus in the treatment of children with focal segmental glomerulosclerosis. World J Pediatr. 2014;10:151–4.
Moorani KN, Khan KM, Ramzan A. Infections in children with nephrotic syndrome. J Coll Physicians Surg Pak. 2003;13:337–9.
Gulati S, Kher V, Gupta A, Arora P, Rai PK, Sharma RK. Spectrum of infections in Indian children with nephrotic syndrome. Pediatr Nephrol. 1995;9:431–4.
Funding
No funding was secured for this study.
Author information
Authors and Affiliations
Contributions
HXC designed the study, analyzed the data, and wrote the paper. QC analyzed the data. FL collected the cases. XCW guided writing of the paper. All authors contributed to the critical revision and final approval of the manuscript.
Corresponding author
Ethics declarations
Ethical approval
The study protocol was approved by Local Ethics Committee of The Second Xiangya Hospital.
Conflict of interest
No financial benefits have been received from any party related directly or indirectly to the subject of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chen, HX., Cheng, Q., Li, F. et al. Efficacy and safety of tacrolimus and low-dose prednisone in Chinese children with steroid-resistant nephrotic syndrome. World J Pediatr 16, 159–167 (2020). https://doi.org/10.1007/s12519-019-00257-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12519-019-00257-z