Abstract
Background
Some neonates develop idiopathic hyperbilirubinemia (INHB) requiring phototherapy, yet with no identifiable causes. We searched for an association between abnormal thyroid levels after birth and INHB.
Methods
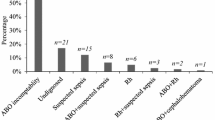
Of 5188 neonates, 1681 (32.4%) were excluded due to one or more risk factors for hyperbilirubinemia. Total thyroxine (TT4) and thyroid stimulating hormone values were sampled routinely at 40–48 hours of age and measured in the National Newborn Screening Program.
Results
Of the 3507 neonates without known causes for hyperbilirubinemia, 61 (1.7%) developed INHB and received phototherapy. Univariate analyses found no significant association between mode of delivery and INHB (vacuum-delivered neonates were a priori excluded). Nonetheless, in cesarean-delivered (CD) neonates, two variables had significant association with INHB: TT4 ≥ 13 µg/dL and birth at 38–38.6 weeks. In vaginally delivered (VD) born neonates, INHB was associated with weight loss > 7.5% up to 48 hours of age. Multivariate logistic regression analysis showed a strong effect of mode of delivery on possible significant association with INHB. In CD neonates, such variables included: TT4 ≥ 13 µg/dL [P = 0.025, odds ratio (OR) 5.49, 95% confidence interval (CI) 1.23–24.4] and birth at 38–38.6 weeks (P = 0.023, OR 3.44, 95% CI 1.19–9.97). In VD neonates, weight loss > 7.5% (P = 0.019, OR 2.1, 95% CI 1.13–3.83) and 1-min Apgar score < 9 (P < 0.001, OR 3.8, 95% CI 1.83–7.9), but not TT4, showed such an association.
Conclusions
INHB was significantly associated with birth on 38–38.6 week and TT4 (≥ 13 µg/dL) in CD neonates, and with a weight loss > 7.5% in VD neonates. We herein highlight some acknowledged risk factors for neonatal hyperbilirubinemia, and thus minimize the rate of INHB.


Similar content being viewed by others
References
American Academy of Pediatrics Subcommittee on Hyperbilirubinemia. Management of hyperbilirubinemia in the newborn infant 35 or more weeks of gestation. Pediatrics. 2004;114:297–316.
Bertini G, Breschi R, Dani C. Physiological weight loss chart helps to identify high-risk infants who need breastfeeding support. Acta Paediatr. 2015;104:1024–7.
Phuapradit W, Chaturachinda K, Auntlamai S. Risk factors for neonatal hyperbilirubinemia. J Med Assoc Thail. 1993;76:424–8.
Gundur NM, Kumar P, Sundaram V, Thapa BR, Narang A. Natural history and predictive risk factors of prolonged unconjugated jaundice in the newborn. Pediatr Int. 2010;52:769–72.
Chang PF, Lin YC, Liu K, Yeh SJ, Ni YH. Identifying term breast-fed infants at risk of significant hyperbilirubinemia. Pediatr Res. 2013;74:408–12.
Keren R, Bhutani VK, Luan X, Nihtianova S, Cnaan A, Schwartz JS. Identifying newborns at risk of significant hyperbilirubinaemia: a comparison of two recommended approaches. Arch Dis Child. 2005;90:415–21.
Kaplan M, Hammerman C. Association between neonatal hyperbilirubinemia and UDP-glucuronosyltransferase 1A1 gene polymorphisms. Pediatr Int. 2013;55:259.
Singh B, Ezhilarasan R, Kumar P, Narang A. Neonatal hyperbilirubinemia and its association with thyroid hormone levels and urinary iodine excretion. Indian J Pediatr. 2003;70:311–5.
Lao TT, Lee CP. Gestational diabetes mellitus and neonatal hyperthyrotropinemia. Gynecol Obstet Investig. 2002;53:135–9.
Leung WC, Chan KK, Lao TT. Neonatal hyperthyrotropinemia in gestational diabetes mellitus and perinatal complications. Neuroendocrinology. 2004;80:124–8.
Bhutani VK, Johnson L, Sivieri EM. Predictive ability of a predischarge hour-specific serum bilirubin for subsequent significant hyperbilirubinemia in healthy term and near-term newborns. Pediatrics. 1999;103:6–14.
Maisels MJ, McDonagh AF. Phototherapy for neonatal jaundice. N Engl J Med. 2008;358:920–8.
Yang WC, Zhao LL, Li YC, Chen CH, Chang YJ, Fu YC, et al. Bodyweight loss in predicting neonatal hyperbilirubinemia 72 hours after birth in term newborn infants. BMC Pediatr. 2013;13:145.
Armanian AM, Hashemipour M, Esnaashari A, Kelishadi R, Farajzadegan Z. Influence of perinatal factors on thyroid stimulating hormone level in cord blood. Adv Biomed Res. 2013;2:48.
Gupta A, Srivastava S, Bhatnagar A. Cord blood thyroid stimulating hormone level—interpretation in light of perinatal factors. Indian Pediatr. 2014;51:32–6.
Miyamoto N, Tsuji M, Imataki T, Nagamachi N, Hirose S, Hamada Y. Influence of mode of delivery on fetal pituitary-thyroid axis. Acta Paediatr Jpn. 1991;33:363–8.
Ryckman KK, Spracklen CN, Dagle JM, Murray JC. Maternal factors and complications of preterm birth associated with neonatal thyroid stimulating hormone. J Pediatr Endocrinol Metab. 2014;27:929–38.
Turan S, Bereket A, Angaji M, Koroglu OA, Bilgen H, Onver T, et al. The effect of the mode of delivery on neonatal thyroid function. J Matern Fetal Neonatal Med. 2007;20:473–6.
Thorpe-Beeston JG, Nicolaides KH, Felton CV, Butler J, McGregor AM. Maturation of the secretion of thyroid hormone and thyroid-stimulating hormone in the fetus. N Engl J Med. 1991;324:532–6.
Gartner LM, Arias IM. Hormonal control of hepatic bilirubin transport and conjugation. Am J Physiol. 1972;222:1091–9.
Van Steenbergen W, Fevery J, De Groote J. Thyroid hormones and the hepatic handling of bilirubin. II. Effects of hypothyroidism and hyperthyroidism on the apparent maximal biliary secretion of bilirubin in the Wistar rat. J Hepatol. 1988;7:229–38.
Van Steenbergen W, Fevery J, De Vos R, Leyten R, Heirwegh KP, De Groote J. Thyroid hormones and the hepatic handling of bilirubin. I. Effects of hypothyroidism and hyperthyroidism on the hepatic transport of bilirubin mono- and diconjugates in the Wistar rat. Hepatology. 1989;9:314–21.
Funding
None.
Author information
Authors and Affiliations
Contributions
IRM proposed the project and wrote the paper. IU and TS contributed equally to this study and are first coauthors. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethical approval
This study was approved by The Helsinki Committee. The informed consents were obtained from newborns’ parents.
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Ulanovsky, I., Smolkin, T., Almashanu, S. et al. Hyperthyroxinemia at birth: a cause of idiopathic neonatal hyperbilirubinemia?. World J Pediatr 14, 247–253 (2018). https://doi.org/10.1007/s12519-017-0113-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12519-017-0113-7