Abstract
Background
This study aimed to evaluate the clinical features of posterior reversible encephalopathy syndrome (PRES) in children.
Methods
The medical records of 31 patients from five medical centers who were diagnosed with PRES from 2001 to 2013 were retrospectively analyzed. In the 31 patients, 16 were males, and 15 females, with a median age of 7 years (3–12 years). Patients younger than 10 years accounted for 74.2% of the 31 patients.
Results
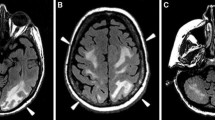
Seizure, the most common clinical sign, occurred in 29 of the 31 patients. Visual disturbances were also observed in 20 patients. Cerebral imaging abnormalities were bilateral and predominant in the parietal and occipital white matter. In this series, three patients died in the acute phase of PRES. One patient had resolution of neurologic presentation within one week, but no apparent improvement in radiological abnormalities was observed at eight months. One patient showed gradual recovery of both neurologic presentation and radiological abnormalities during follow-up at eight months. One patient developed long-term cortical blindness. All of the PRES patients with hematologic tumor had a worse prognosis than those without hematologic tumor.
Conclusions
Seizure is a prevalent characteristic of children with PRES. Poor prognosis can be seen in PRES patients with hematologic tumor.
Similar content being viewed by others
References
Hinchey J, Chaves C, Appignani B, Breen J, Pao L, Wang A, et al. A reversible posterior leukoencephalopathy syndrome. N Engl J Med 1996;334:494–500.
Dillon WP, Rowley H. The reversible posterior cerebral edema syndrome. AJNR Am J Neuroradiol 1998;19: 591.
Trullemans F, Grignard F, Van Camp B, Schots R. Clinical findings and magnetic resonance imaging in severe cyclosporine-related neurotoxicity after allogeneic bone marrow transplantation. Eur J Haematol 2001;67:94–99.
Siebert E, Spors B, Bohner G, Endres M, Liman TG. Posterior reversible encephalopathy syndrome in children: radiological and clinical findings-a retrospective analysis of a German tertiary care center. Eur J Paediatr Neurol 2013;17:169–175.
Lee VH, Wijdicks EF, Manno EM, Rabinstein AA. Clinical spectrum of reversible posterior leukoencephalopathy syndrome. Arch Neurol 2008;65:205–210.
Liman TG, Bohner G, Heuschmann PU, Endres M, Siebert E. The clinical and radiological spectrum of posterior reversible encephalopathy syndrome: the retrospective Berlin PRES study. J Neurol 2012;259:155–164.
Young GB. Encephalopathy of infection and systemic inflammation. J Clin Neurophysiol 2013;30:454–461.
Kim SJ, Im SA, Lee JW, Chung NG, Cho B, Kim HK, et al. Predisposing factors of posterior reversible encephalopathy syndrome in acute childhood leukemia. Pediatr Neurol 2012;47:436–442.
Bartynski WS. Posterior reversible encephalopathy syndrome, part 2: controversies surrounding pathophysiology of vasogenic edema. AJNR Am J Neuroradiol 2008;29:1043–1049.
Panis B, Vlaar AM, van Well GT, Granzen B, Weber JW, Postma AA, et al. Posterior reversible encephalopathy syndrome in paediatric leukaemia. Eur J Paediatr Neurol 2010;14:539–545.
Won SC, Kwon SY, Han JW, Choi SY, Lyu CJ. Posterior reversible encephalopathy syndrome in childhood with hematologic/oncologic diseases. J Pediatr Hematol Oncol 2009;31:505–508.
Lucchini G, Grioni D, Colombini A, Contri M, De Grandi C, Rovelli A, et al. Encephalopathy syndrome in children with hemato-oncological disorders is not always posterior and reversible. Pediatr Blood Cancer 2008;51:629–633.
Ishikura K, Ikeda M, Hamasaki Y, Hataya H, Nishimura G, Hiramoto R, et al. Nephrotic state as a risk factor for developing posterior reversible encephalopathy syndrome in paediatric patients with nephrotic syndrome. Nephrol Dial Transplant 2008;23:2531–2536.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Li, H., Liu, Y., Chen, J. et al. Posterior reversible encephalopathy syndrome in patients with hematologic tumor confers worse outcome. World J Pediatr 11, 245–249 (2015). https://doi.org/10.1007/s12519-015-0027-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12519-015-0027-1