Abstract
Background
We aimed to analyze clinical and inflammatory markers of steroid non-response in patients with moderate/severe ulcerative colitis (UC) at the time of diagnosis.
Methods
This study included patients who were graded as having moderate/severe UC and received corticosteroids as first-line therapy. Demographic, clinical and laboratory findings and pediatric ulcerative colitis activity scores (PUCAS) were recorded. Response to corticosteroids was assessed 30 days after the induction and long-term therapy.
Results
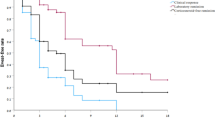
Twenty-eight children were diagnosed as having moderate/severe UC. Their mean age ± SD was 1 2.2 ± 4 years, and 17% were under 5 years of age. PUCAS at their initial admission was 56.9 ± 11.8. UC was observed at the left colon in 9 patients (32.1%), and pancolitis in 19 (67.9%). At the end of the 30th day, UC was completely remitted in 15 patients (53.5%), partially remitted in 2 (7.1%), and no response in 11 (39.2%). Short-term follow-up showed partial remission in 2 patients, and overall remission with steroid in 17 (60.7%). Non-responders were given second-line treatment; steroid dependency was documented in 2 patients (7.1%) and another 2 (7.1%) patients underwent colectomy. Predictors for steroid non-response were analyzed and only PUCAS at the initial admission was found to be associated with non-response to steroids (51.4 ± 11.4 vs. 65.4 ± 6.8, P<0.05).
Conclusions
Approximately half of the pediatric patients had complete response to steroid therapy in a long period. PUCAS could be used as a potential marker of “failed response” to steroid, but should be supported with a number of prospective randomized controlled studies.
Similar content being viewed by others
References
Hyams J, Markowitz J, Lerer T, Griffiths A, Mack D, Bousvaros A, et al. The natural history of corticosteroid therapy for ulcerative colitis in children. Clin Gastroenterol Hepatol 2006;4:1118–1123.
Lopes LH, Sdepanian VL, Szejnfeld VL, de Morais MB, Fagundes-Neto U. Risk factors for low bone mineral density in children and adolescents with inflammatory bowel disease. Dig Dis Sci 2008;53:2746–2753.
Tung J, Loftus EV Jr, Freese DK, El-Youssef M, Zinsmeister AR, Melton LJ 3rd, et al. A population-based study of the frequency of corticosteroid resistance and dependence in pediatric patients with Crohn’s disease and ulcerative colitis. Inflamm Bowel Dis 2006;12:1093–1100.
Oliva-Hemker M, Escher JC, Moore D, Dubinksy M, Hildebrand H, Koda YK, et al. Refractory inflammatory bowel disease in children. J Pediatr Gastroenterol Nutr 2008;47:266–272.
Turner D. Severe acute ulcerative colitis: the pediatric perspective. Dig Dis 2009;27:322–326.
Hyams JS, Davis P, Grancher K, Lerer T, Justinich CJ, Markowitz J. Clinical outcome of ulcerative colitis in children. J Pediatr 1996;129:81–88.
Kugathasan S, Dubinsky MC, Keljo D, Moyer MS, Rufo PA, Wyllie R, et al. Severe colitis in children. J Pediatr Gastroenterol Nutr 2005;41:375–385.
Auvin S, Molinié F, Gower-Rousseau C, Brazier F, Merle V, Grandbastien B, et al. Incidence, clinical presentation and location at diagnosis of pediatric inflammatory bowel disease: a prospective population-based study in northern France (1988–1999). J Pediatr Gastroenterol Nutr 2005;41:49–55.
Turner D, Otley AR, Mack D, Hyams J, de Bruijne J, Uusoue K, et al. Development, validation, and evaluation of a pediatric ulcerative colitis activity index: a prospective multicenter study. Gastroenterology 2007;133:423–432.
Markowitz J. Current treatment of inflammatory bowel disease in children. Dig Liver Dis 2008;40:16–21.
Turner D, Walsh CM, Benchimol EI, Mann EH, Thomas KE, Chow C, et al. Severe paediatric ulcerative colitis: incidence, outcomes and optimal timing for second-line therapy. Gut 2008;57:331–338.
Travis SP, Farrant JM, Ricketts C, Nolan DJ, Mortensen NM, Kettlewell MG, et al. Predicting outcome in severe ulcerative colitis. Gut 1996;38:905–910.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cakir, M., Ozgenc, F., Yusekkaya, H.A. et al. Steroid response in moderate to severe pediatric ulcerative colitis: a single center’s experience. World J Pediatr 7, 50–53 (2011). https://doi.org/10.1007/s12519-011-0245-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12519-011-0245-0