Abstract
Background
Antenatal variant of Bartter syndrome is characterized by a history of polyhydramnios, premature birth, metabolic alkalosis, hypokalemia, polyuria and renal salt wasting. In this report we present a premature female baby with antenatal Barter syndrome who had three episodes of urinary tract infection (UTI), without evidence for congenital anomaly of the kidneys or urinary tract.
Methods
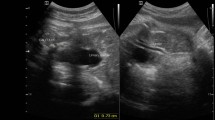
Antenatal Bartter syndrome was diagnosed according to the standard criteria. Ultrasound scan and voiding cystourethrography were performed to exclude congenital anomaly of the kidneys and urinary tract.
Results
The baby presented with early hyperkalemia and acidosis. The typical biochemical features of the Bartter syndrome were observed in the second month. Despite appropriate treatment she had persistent hypercalciuria. The clinical course was complicated with recurrent episodes of febrile UTIs. Urinary tract system imaging did not demonstrate congenital anomalies. She finally died of severe dehydration, acidosis and renal failure.
Conclusion
Since no congenital anomaly of the kidneys or urinary tract was demonstrated in our patient, we believe that severe, persistent hypercalciuria is the most important risk factor for development of recurrent UTIs.
Similar content being viewed by others
References
Peters M, Konrad M, Seyberth HW. Hereditary hypokalemic salt-losing tubular disorders. Saudi J Kidney Dis Transpl 2003;14:386–397.
Rodriguez-Soriano J. Bartter and related syndromes: the puzzle is almost solved. Pediatr Nephrol 1998;12:315–327.
Finer G, Shalev H, Birk OS, Galron D, Jeck N, Sinai-Treiman L, et al. Transient neonatal hyperkalemia in the antenatal (ROMK defective) Bartter syndrome. J Pediatr 2003;142:318–323.
Peters M, Jeck N, Reinalter S, Leonhardt A, Tönshoff B, Klaus G, et al. Clinical presentation of genetically defined patients with hypokalemic salt-losing tubulopathies. Am J Med 2002;112:183–190.
Nozu K, Fu XJ, Kaito H, Kanda K, Yokoyama N, Przybyslaw Krol R, et al. A novel mutation in KCNJ1 in a Bartter syndrome case diagnosed as pseudohypoaldosteronism. Pediatr Nephrol 2007;22:1219–1223.
Cho JT, Guay-Woodford LM. Heterozygous mutations of the gene for Kir 1.1 (ROMK) in antenatal Bartter syndrome presenting with transient hyperkalemia, evolving to a benign course. J Korean Med Sci 2003;18:65–68.
Haas NA, Nossal R, Schneider CH, Lewin MA, Ocker V, Holder M, et al. Successful management of an extreme example of neonatal hyperprostaglandin-E syndrome (Bartter’s syndrome) with the new cyclooxygenase-2 inhibitor rofecoxib. Pediatr Crit Care Med 2003;4:249–251.
Shalev H, Ohali M, Kachko L, Landau D. The neonatal variant of Bartter syndrome and deafness: preservation of renal function. Pediatrics 2003;112:628–633.
Vachvanichsanong P, Malagon M, Moore ES. Urinary tract infection in children associated with idiopathic hypercalciuria. Scan J Urol Nephrol 2001;35:112–116.
López MM, Castillo LA, Chávez JB, Ramones C. Hypercalciuria and recurrent urinary tract infection in Venezuelan children. Pediatr Nephrol 1999;13:433–437.
StojanoviĆ VD, MiloseviĆ BO, DjapiĆ MB, Bubalo JD. Idiopathic hypercalciuria associated with urinary tract infection in children. Pediatr Nephrol 2007;22:1291–1295.
Weber S, Schneider L, Peters M, Misselwitz J, Rönnefarth G, Böswald M, et al. Novel paracellin-1 mutations in 25 families with familial hypomagnesemia with hypercalciuria and nephrocalcinosis. J Am Soc Nephrol 2001;12:1872–1881.
Lieske JC, Swift H, Martin T, Patterson B, Toback FG. Renal epithelial cells rapidly bind and internalize calcium monohydrate crystals. Proc Natl Acad Sci USA 1994;91:6987–6991.
Lieske JC, Leonard R, Toback FG. Adhesion of calcium oxalate monohydrate crystals to renal epithelial cells is inhibited by specific anions. Am J Physiol 1995;268(4 Pt 2):F604–612
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tasic, V., Pota, L. & Gucev, Z. Recurrent urinary tract infections in an infant with antenatal Bartter syndrome. World J Pediatr 7, 86–88 (2011). https://doi.org/10.1007/s12519-010-0021-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12519-010-0021-6