Abstract
Background
Since exchange blood transfusion (EBT) is associated with serious complications, phototherapy has been made more powerful to reduce the need for EBT in the developed world. This study was undertaken to determine the indications for EBT in neonatal jaundice (NNJ) at our unit and what proportion of EBTs was possibly avoidable.
Methods
All the babies who had EBT for hyperbilirubinemia over a three-year period were included. Age, sex, weight, place of delivery, blood group of baby and mother, other investigations, management, and the outcome of the babies were recorded.
Results
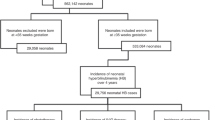
Of the 1686 babies admitted to the neonatal unit, 90 (5.3%) had EBT. Fourteen (15.6%) were inborn while 76 (84.4%) were out-born babies. Fifty-six (62.2%) babies were admitted primarily for NNJ while 34 (37.8%) developed NNJ during admission. Thirty-six (40.0%) of the babies had phototherapy for more than 24 hours prior to EBT either because they were of very low birthweight or NNJ was detected very early and therapy was so commenced. Sixty-eight (75.6%) babies had single EBT while the remaining 22 (24.4%) had two sessions of EBT. Factors associated with severe NNJ in babies requiring EBT included low birthweight (<2500 g, 44.4%), ABO incompatibility (30.0%), glucose-6-phosphate dehydrogenase deficiency (34.4%) and septicemia (26.1%). Twenty-seven (30.0%) of the neonates developed features of kernicterus: 26 before admission while 1 during admission; all except one were delivered outside the hospital.
Conclusions
The EBT rate in our center was high. With more effective phototherapy, EBT could be avoided in most of the babies who initially had phototherapy for more than 24 hours before EBT and repeated EBT sessions. Health education of the population at risk, especially pregnant women, and early referral at the primary health care level will reduce the burden of severe NNJ.
Similar content being viewed by others
References
Maisels MJ. Neonatal Hyperbilirubinaemia. In: Klaus MH, Fanaroff AA, eds. Care of the High Risk Neonate, 5th ed. Philadelphia: WB Saunders Company, 1986: 324–362.
Ibe BC. Neonatal Jaundice. In: Azubuike JC, Nkanginieme KEO, eds. Paediatrics and Child Health in a Tropical Region, 1st ed. Owerri: African Educational Services, 1999: 44–51.
Owa JA, Taiwo O, Adebiyi JAO, Dogunro SA. Neonatal Jaundice at Wesley Guild Hospital, Ilesa and Ife State Hospital, Ile-Ife. Nig J Paediatr 1989;16:23–30.
Owa JA, Osinaike AI. Neonatal morbidity and mortality in Nigeria. Indian J Pediatr 1998;65:441–449.
Palmer DC, Drew JH. Jaundice: a 10 year review of 41,000 live born infants. Aust Paediatr J 1983;19:86–89.
Newman TB, Maisels MJ. Less aggressive treatment of neonatal jaundice and reports of kernicterus: lessons about practice guidelines. Pediatrics 2000;105:242–245.
Hansen TW. Kernicterus in term and near term infants—the specter walks again. Acta Paediatr 2000;89:1155–1157.
Suvanand S, Kapoor SK, Reddaiah VP, Singh U, Sundaram KR. Risk factors for cerebral palsy. Indian J Pediatr 1997;64:677–685.
Maisels MJ, McDonagh AF. Phototherapy for neonatal jaundice. N Engl J Med 2008;358:920–928.
Hansen TW. Acute management of extreme neonatal jaundice—the potential benefits of intensified phototherapy and interruption of enterohepatic bilirubin circulation. Acta Paediatr 1997;86:843–846.
Steiner LA, Bizzarro MJ, Ehrenkranz RA, Gallagher PG. A decline in the frequency of neonatal exchange transfusions and its effect on exchange-related morbidity and mortality. Pediatrics 2007;120:27–32.
Maisels MJ. Why use homeopathic doses of phototherapy? Pediatrics 1996;98;283–287.
Mills JF, Tudehope D. Fibreoptic phototherapy for neonatal jaundice. Cochrane Database Syst Rev 2001;(1):CD002060.
Lock M, Ray JG. Higher neonatal morbidity after routine early hospital discharge: are we sending newborns home too early? CMAJ 1999;161:249–253.
Gourley GR, Kreamer BL, Cohnen M. Inhibition of beta-glucuronidase by casein hydrolysate formula. J Pediatr Gastroenterol Nutrit 1997;25:267–272.
Gourley GR, Kreamer B, Cohnen M, Kosorok MR. Neonatal Jaundice and Diet. Arch Paediatr Adolesc Med 1999;153:184–188.
Alpay F, Sarici SU, Tosuncuk HD, Serdar MA, Inanç N, Gökçay E. The value of first-day bilirubin measurement in predicting the development of significant hyperbilirubinemia in healthy term newborns. Pediatr 2000;106:E16.
Hansen TW. Extreme neonatal jaundice: How frequent is it? Acta Paediatr 2008;97:1002–1003.
Udoma EJ, Udo JJ, Etuk SJ, Duke ES. Morbidity and mortality among infants with normal birth weight in a Newborn Baby Unit. Nig J Paediatr 2001;28:13–17.
Etuk SJ, Etuk IS, Ekott MI, Udoma EJ. Perinatal outcome in pregnancies booked for antenatal care but delivered outside health facilities in Calabar, Nigeria. Acta Tropica 2000;75:29–33.
Ogunniyi SO, Faleyimu BL, Makinde ON, Adejuyigbe EA, Ogunniyi FA, Owolabi AT. Delivery care services utilization in an urban Nigerian population. Nig J Med 2000;9:81–85.
Watchko JF. Vigintiphobia revisited. Pediatrics 2005;115:1747–1753.
American Academy of Pediatrics, Subcommittee on Hyperbilirubinemia. Management of hyperbilirubinemia in the newborn infant 35 weeks or more of gestation. Pediatrics 2004;114:297–316.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Owa, J.A., Ogunlesi, T.A. Why we are still doing so many exchange blood transfusion for neonatal jaundice in Nigeria. World J Pediatr 5, 51–55 (2009). https://doi.org/10.1007/s12519-009-0009-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12519-009-0009-2