Abstract
Background
This study aimed to calculate the treatment costs of acute myocardial infarction (AMI) in the Netherlands for 2012. Also, the degree of association between treatment costs of AMI and some patient and hospital characteristics was examined.
Methods
For this retrospective cost analysis, patients were drawn from the database of the Diagnosis Treatment Combination (Diagnose Behandeling Combinatie, DBC) casemix system, which contains data on the resource use of all hospitalisations in the Netherlands. All costs were based on Euro 2012 cost data.
Results
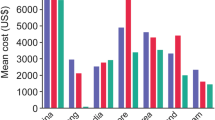
The analysis was based on data of 25,657 patients. Mean treatment costs were estimated at € 5021, with significant cost increases for patients with percutaneous coronary intervention (PCI) treatment. ST-segment elevation myocardial infarction (STEMI) patients receiving thrombolysis incurred the lowest (€ 4286), while non-STEMI patients receiving PCI the highest costs (€ 6060). Length of stay and hospital type were strong predictors of treatment costs.
Conclusions
This study is the most extensive cost assessment of the treatment costs of AMI in the Netherlands thus far. Our results may be used as input for health-economic models and economic evaluations to support the decision making of registration, reimbursement and pricing of interventions in healthcare.

Similar content being viewed by others
References
Keeley EC, Hillis LD. Primary PCI for myocardial infarction with ST-segment elevation. N Engl J Med. 2007;356:47–54.
Poos MJJC. Volksgezondheid Toekomst Verkenning, Nationaal Kompas Volksgezondheid. RIVM: Bilthoven; 14 juni 2012.
Voss GB, Hasman A, Rutten F, et al. Explaining cost variations in DRGs ‘Acute Myocardial Infarction’ by severity of illness. Health Pol. 1994;28:37–50.
Evans E, Imanaka Y, Sekimoto M, et al. Risk adjusted resource utilization for AMI patients treated in Japanese hospitals. Health Econ. 2007;16:347–59.
Hamm CW, Bassand JP, Agewall S, et al. ESC guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation: the task force for the management of acute coronary syndromes (ACS) in patients presenting without persistent ST-segment elevation of the European Society of Cardiology (ESC). Eur Heart J. 2011;32:2999–3054.
Van de Werf F, Bax J, Betriu A, et al. Management of acute myocardial infarction in patients presenting with persistent ST-segment elevation: the task force on the management of ST-segment elevation acute myocardial infarction of the European Society of Cardiology. Eur Heart J. 2008;29:2909–45.
Atary JZ, de Visser M, van den Dijk R, et al. Standardised pre-hospital care of acute myocardial infarction patients: MISSION! guidelines applied in practice. Neth Heart J. 2010;18:408–15.
Tiemann O. Variations in hospitalisation costs for acute myocardial infarction—a comparison across Europe. Health Econ. 2008;17:S33–45.
Kauf TL, Velazquez EJ, Crosslin DR, et al. The cost of acute myocardial infarction in the new millennium: evidence from a multinational registry. Am Heart J. 2006;151:206–12.
Hakkinen U, Chiarello P, Cots F, et al. Patient classification and hospital costs of care for acute myocardial infarction in nine European countries. Health Econ. 2012;21 Suppl 2:19–29.
Aasa M, Henriksson M, Dellborg M, et al. Cost and health outcome of primary percutaneous coronary intervention versus thrombolysis in acute ST-segment elevation myocardial infarction-results of the Swedish Early Decision reperfusion Study (SWEDES) trial. Am Heart J. 2010;160:322–8.
Eagle KA, Goodman SG, Avezum A, et al. Practice variation and missed opportunities for reperfusion in ST-segment-elevation myocardial infarction: findings from the Global Registry of Acute Coronary Events (GRACE). Lancet. 2002;359:373–7.
Dormont B, Milcent C. The sources of hospital cost variability. Health Econ. 2004;13:927–39.
Hvenegaard A, Street A, Sorensen TH, et al. Comparing hospital costs: what is gained by accounting for more than a case-mix index? Soc Sci Med. 2009;69:640–7.
Tan SS, Bouwmans CA, Rutten FF, et al. Update of the Dutch manual for costing in economic evaluations. Int J Tech Assess Health Care. 2012;28:152–8.
Nederlandse Zorgauthoriteit (NZa). http://dbc-tarieven.nza.nl/Nzatarieven/top.do.
Centraal Bureau voor de Statistiek & Ministerie voor Volksgezondheid Welzijn en Sport. http://www.statline.nl.
Oanda. http://www.oanda.com/.
VMS veiligheidsprogramma. http://www.vmszorg.nl/.
Kendall J. The optimum reperfusion pathway for ST elevation acute myocardial infarction: development of a decision framework. Emerg Med J. 2007;24:52–6.
Bertrand ME, Simoons ML, Fox KA, et al. Management of acute coronary syndromes in patients presenting without persistent ST-segment elevation. Eur Heart J. 2002;23:1809–40.
Tan SS, Rutten FF, van Ineveld BM, et al. Comparing methodologies for the cost estimation of hospital services. Eur J Health Econ. 2009;10:39–45.
Dharma S, Juzar DA, Firdaus I, et al. Acute myocardial infarction system of care in the third world. Neth Heart J. 2012;20:254–9.
The Healthcare Inspectorate (IGZ). Basic Set of Hospital Performance Indicators 2004. First edition, The Healthcare Inspectorate: The Hague; 2005.
Friedel H, Delges A, Clouth J, et al. Expenditures of the German statutory health insurance system for patients suffering from acute coronary syndrome and treated with percutaneous coronary intervention. Eur J Health Econ. 2010;11:449–55.
Acknowledgements
The authors are grateful to Rob van Mechelen for his contribution to this study.
Funding
This study was supported by the Dutch Organisation for Health Research and Healthcare Innovation (ZON-MW, grant no. 152002043).
Conflict of interests
None declared.
Author information
Authors and Affiliations
Corresponding author
Additional information
The questions can be answered after the article has been published in print. You have to log in to: www.cvoi.nl.
Rights and permissions
About this article
Cite this article
Soekhlal, R.R., Burgers, L.T., Redekop, W.K. et al. Treatment costs of acute myocardial infarction in the Netherlands. Neth Heart J 21, 230–235 (2013). https://doi.org/10.1007/s12471-013-0386-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12471-013-0386-y