Abstract
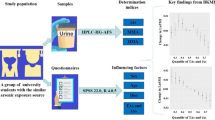
High-level arsenic exposure is widely considered to be associated with hypertension. However, the relationship between arsenic metabolism and hypertension under high-level exposure remains controversial. In addition, the evidence at low-to-moderate levels remains unelucidated. This research aims to evaluate the relationship between arsenic metabolism and the risk of hypertension in a Chinese population under different levels of arsenic exposure. A cross-sectional survey of 1932 participants exposed to different arsenic concentrations through contaminated drinking water was conducted in epidemic areas in southwest and northwest China. Based on the World Health Organization’s drinking-water standards, the study population was stratified into two subgroups: high-exposure (water As concentration (wAs) ≥ 50 μg/L) and low-to-moderate (10 ≤ wAs < 50 μg/L) exposure. Arsenic metabolism capacity was evaluated by the relative fractions of inorganic arsenic (iAs), monomethylarsenate (MMA) and dimethylarsenate (DMA) in urine (denoted by iAs%, MMA%, DMA%, primary methylation index and the secondary methylation index). The relationship between arsenic metabolism and hypertension was evaluated by the leave-one-out approach, which modeled the dynamics of arsenic metabolism. There were significant differences and associations between individual factors and the distribution of urinary arsenic metabolites at different arsenic exposure levels. Increased MMA% was associated with higher risk of hypertension when either iAs% or DMA% decreased at different arsenic exposures. iAs% was associated with lower risk of hypertension only when MMA% decreased in both subgroups. In addition, higher DMA% was both associated with lower hypertension prevalence when either iAs% or MMA% decreased only at low-to-moderate arsenic exposure. In summary, arsenic metabolism, particularly higher MMA%, was associated with increased risk of hypertension in the Chinese arsenic-exposed population with both high and low-to-moderate levels, which provides additional evidence for the assessment of arsenic-induced hypertension incident.




Similar content being viewed by others
Data Availability
The data supporting the results of this study are available from the corresponding authors upon reasonable request.
Abbreviations
- As:
-
Arsenic
- wAs:
-
Water arsenic
- iAs:
-
Inorganic arsenic
- MMA:
-
Monomethylarsonic acid
- DMA:
-
Dimethylarsinic acid
- PMI:
-
Primary methylation index
- SMI:
-
Secondary methylation index
- tAs:
-
Total arsenic in urine
- UCre:
-
Urinary creatinine
- SBP:
-
Systolic blood pressure
- DBP:
-
Diastolic blood pressure
- 95% CIs:
-
95% Confidence intervals
- WHO:
-
World Health Organization
- ISH:
-
International Society of Hypertension
References
Abhyankar LN, Jones MR, Guallar E, Navas-Acien A (2012) Arsenic exposure and hypertension: a systematic review. Environ Health Perspect 120:494–500. https://doi.org/10.1289/ehp.1103988
Abuawad A, Spratlen MJ, Parvez F, Slavkovich V, Ilievski V, Lomax-Luu AM et al (2021) Association between body mass index and arsenic methylation in three studies of Bangladeshi adults and adolescents. Environ Int 149:106401. https://doi.org/10.1016/j.envint.2021.106401
Akerstrom M, Sallsten G, Lundh T, Barregard L (2013) Associations between urinary excretion of cadmium and proteins in a nonsmoking population: renal toxicity or normal physiology? Environ Health Perspect 121:187–191. https://doi.org/10.1289/ehp.1205418
Ameer SS, Engström K, Harari F, Concha G, Vahter M, Broberg K (2015) The effects of arsenic exposure on blood pressure and early risk markers of cardiovascular disease: evidence for population differences. Environ Res 140:32–36. https://doi.org/10.1016/j.envres.2015.03.010
Bae ON, Lim EK, Lim KM, Noh JY, Chung SM, Lee MY et al (2008) Vascular smooth muscle dysfunction induced by monomethylarsonous acid (MMA III): a contributing factor to arsenic-associated cardiovascular diseases. Environ Res 108:300–308. https://doi.org/10.1016/j.envres.2008.06.012
Baris D, Waddell R, Beane Freeman LE, Schwenn M, Colt JS, Ayotte JD et al (2016) Elevated bladder cancer in northern New England: the role of drinking water and arsenic. J Natl Cancer Inst. https://doi.org/10.1093/jnci/djw099
Bommarito PA, Xu X, González-Horta C, Sánchez-Ramirez B, Ballinas-Casarrubias L, Luna RS et al (2019) One-carbon metabolism nutrient intake and the association between body mass index and urinary arsenic metabolites in adults in the Chihuahua cohort. Environ Int 123:292–300. https://doi.org/10.1016/j.envint.2018.12.004
Brammer H, Ravenscroft P (2009) Arsenic in groundwater: a threat to sustainable agriculture in south and south-east Asia. Environ Int 35:647–654. https://doi.org/10.1016/j.envint.2008.10.004
Chen CJ, Wang SL, Chiou JM, Tseng CH, Chiou HY, Hsueh YM et al (2007a) Arsenic and diabetes and hypertension in human populations: a review. Toxicol Appl Pharmacol 222:298–304. https://doi.org/10.1016/j.taap.2006.12.032
Chen Y, Factor-Litvak P, Howe GR, Graziano JH, Brandt-Rauf P, Parvez F et al (2007b) Arsenic exposure from drinking water, dietary intakes of B vitamins and folate, and risk of high blood pressure in Bangladesh: a population-based, cross-sectional study. Am J Epidemiol 165:541–552. https://doi.org/10.1093/aje/kwk037
Chen Y, Wu F, Liu M, Parvez F, Slavkovich V, Eunus M et al (2013) A prospective study of arsenic exposure, arsenic methylation capacity, and risk of cardiovascular disease in Bangladesh. Environ Health Perspect 121:832–838. https://doi.org/10.1289/ehp.1205797
Chen H, Teng Y, Lu S, Wang Y, Wang J (2015) Contamination features and health risk of soil heavy metals in China. Sci Total Environ 512–513:143–153. https://doi.org/10.1016/j.scitotenv.2015.01.025
Das N, Paul S, Chatterjee D, Banerjee N, Majumder NS, Sarma N et al (2012) Arsenic exposure through drinking water increases the risk of liver and cardiovascular diseases in the population of West Bengal, India. BMC Public Health 12:639. https://doi.org/10.1186/1471-2458-12-639
De Loma J, Tirado N, Ascui F, Levi M, Vahter M, Broberg K et al (2019) Elevated arsenic exposure and efficient arsenic metabolism in indigenous women around Lake Poopó, Bolivia. Sci Total Environ 657:179–186. https://doi.org/10.1016/j.scitotenv.2018.11.473
Fano-Sizgorich D, Vásquez-Velásquez C, Yucra S, Vásquez V, Tokeshi P, Aguilar J et al (2021) Total urinary arsenic and inorganic arsenic concentrations and birth outcomes in pregnant women of Tacna, Peru: a cross-sectional study. Expo Health 13:133–140. https://doi.org/10.1007/s12403-020-00377-2
Farzan SF, Howe CG, Zens MS, Palys T, Channon JY, Li Z et al (2017) Urine arsenic and arsenic metabolites in U.S. adults and biomarkers of inflammation, oxidative stress, and endothelial dysfunction: a cross-sectional study. Environ Health Perspect 125:127002. https://doi.org/10.1289/ehp2062
Gao S, Lin PI, Mostofa G, Quamruzzaman Q, Rahman M, Rahman ML et al (2019) Determinants of arsenic methylation efficiency and urinary arsenic level in pregnant women in Bangladesh. Environ Health 18:94. https://doi.org/10.1186/s12940-019-0530-2
Gong G, O’Bryant SE (2012) Low-level arsenic exposure, AS3MT gene polymorphism and cardiovascular diseases in rural Texas counties. Environ Res 113:52–57. https://doi.org/10.1016/j.envres.2012.01.003
Grau-Perez M, Kuo CC, Gribble MO, Balakrishnan P, Jones Spratlen M, Vaidya D et al (2017) Association of low-moderate arsenic exposure and arsenic metabolism with incident diabetes and insulin resistance in the strong heart family study. Environ Health Perspect 125:127004. https://doi.org/10.1289/ehp2566
Gribble MO, Crainiceanu CM, Howard BV, Umans JG, Francesconi KA, Goessler W et al (2013) Body composition and arsenic metabolism: a cross-sectional analysis in the strong heart study. Environ Health 12:107. https://doi.org/10.1186/1476-069x-12-107
Hafeman DM, Ahsan H, Louis ED, Siddique AB, Slavkovich V, Cheng Z et al (2005) Association between arsenic exposure and a measure of subclinical sensory neuropathy in Bangladesh. J Occup Environ Med 47:778–784. https://doi.org/10.1097/01.jom.0000169089.54549.db
Hall EM, Acevedo J, López FG, Cortés S, Ferreccio C, Smith AH et al (2017) Hypertension among adults exposed to drinking water arsenic in northern Chile. Environ Res 153:99–105. https://doi.org/10.1016/j.envres.2016.11.016
He X, Li P, Ji Y, Wang Y, Su Z, Elumalai V (2020) Groundwater arsenic and fluoride and associated arsenicosis and fluorosis in China: occurrence, distribution and management. Expo Health 12:355–368. https://doi.org/10.1007/s12403-020-00347-8
He X, Li P, Wu J, Wei M, Ren X, Wang D (2021) Poor groundwater quality and high potential health risks in the Datong Basin, northern China: research from published data. Environ Geochem Health 43:791–812. https://doi.org/10.1007/s10653-020-00520-7
Hernández A, Marcos R (2008) Genetic variations associated with interindividual sensitivity in the response to arsenic exposure. Pharmacogenomics 9:1113–1132. https://doi.org/10.2217/14622416.9.8.1113
Hernández-Zavala A, Matoušek T, Drobná Z, Paul DS, Walton F, Adair BM et al (2008) Speciation analysis of arsenic in biological matrices by automated hydride generation-cryotrapping-atomic absorption spectrometry with multiple microflame quartz tube atomizer (multiatomizer). J Anal at Spectrom 23:342–351. https://doi.org/10.1039/b706144g
Hsieh CY, Wang SL, Fadrowski JJ, Navas-Acien A, Kuo CC (2019) Urinary concentration correction methods for arsenic, cadmium, and mercury: a systematic review of practice-based evidence. Curr Environ Health Rep 6:188–199. https://doi.org/10.1007/s40572-019-00242-8
Huang YK, Tseng CH, Huang YL, Yang MH, Chen CJ, Hsueh YM (2007) Arsenic methylation capability and hypertension risk in subjects living in arseniasis-hyperendemic areas in southwestern Taiwan. Toxicol Appl Pharmacol 218:135–142. https://doi.org/10.1016/j.taap.2006.10.022
Huang YL, Hsueh YM, Huang YK, Yip PK, Yang MH, Chen CJ (2009) Urinary arsenic methylation capability and carotid atherosclerosis risk in subjects living in arsenicosis-hyperendemic areas in southwestern Taiwan. Sci Total Environ 407:2608–2614. https://doi.org/10.1016/j.scitotenv.2008.12.061
Hudgens EE, Drobna Z, He B, Le XC, Styblo M, Rogers J et al (2016) Biological and behavioral factors modify urinary arsenic metabolic profiles in a U.S. population. Environ Health 15:62. https://doi.org/10.1186/s12940-016-0144-x
Huq ME, Su C, Fahad S, Li J, Sarven MS, Liu R (2018) Distribution and hydrogeochemical behavior of arsenic enriched groundwater in the sedimentary aquifer comparison between Datong Basin (China) and Kushtia district (Bangladesh). Environ Sci Pollut Res Int 25:15830–15843. https://doi.org/10.1007/s11356-018-1756-1
International Society of Hypertension (ISH) (2020) International hypertension practice guidelines of the international society of hypertension in 2020. https://www.chinahc.org.cn/upload/file/20200513/gMjTulL9tL.pdf. Accessed 7 May 2020
Islam MR, Khan I, Attia J, Hassan SM, McEvoy M, D’Este C et al (2012) Association between hypertension and chronic arsenic exposure in drinking water: a cross-sectional study in Bangladesh. Int J Environ Res Public Health 9:4522–4536. https://doi.org/10.3390/ijerph9124522
Jansen RJ, Argos M, Tong L, Li J, Rakibuz-Zaman M, Islam MT et al (2016) Determinants and consequences of arsenic metabolism efficiency among 4,794 individuals: demographics, lifestyle, genetics, and toxicity. Cancer Epidemiol Biomarkers Prev 25:381–390. https://doi.org/10.1158/1055-9965.Epi-15-0718
Jomova K, Jenisova Z, Feszterova M, Baros S, Liska J, Hudecova D et al (2011) Arsenic: toxicity, oxidative stress and human disease. J Appl Toxicol 31:95–107. https://doi.org/10.1002/jat.1649
Jones MR, Tellez-Plaza M, Sharrett AR, Guallar E, Navas-Acien A (2011) Urine arsenic and hypertension in us adults: the 2003–2008 national health and nutrition examination survey. Epidemiology 22:153–161. https://doi.org/10.1097/EDE.0b013e318207fdf2
Kaufman JA, Mattison C, Fretts AM, Umans JG, Cole SA, Voruganti VS et al (2021) Arsenic, blood pressure, and hypertension in the strong heart family study. Environ Res 195:110864. https://doi.org/10.1016/j.envres.2021.110864
Kuo CC, Howard BV, Umans JG, Gribble MO, Best LG, Francesconi KA et al (2015) Arsenic exposure, arsenic metabolism, and incident diabetes in the strong heart study. Diabetes Care 38:620–627. https://doi.org/10.2337/dc14-1641
Kuo CC, Moon KA, Wang SL, Silbergeld E, Navas-Acien A (2017) The association of arsenic metabolism with cancer, cardiovascular disease, and diabetes: a systematic review of the epidemiological evidence. Environ Health Perspect 125:087001. https://doi.org/10.1289/ehp577
Li B, Sun Y, Sun X, Wang Y, Li X, Kumagai Y et al (2007) Monomethylarsonous acid induced cytotoxicity and endothelial nitric oxide synthase phosphorylation in endothelial cells. Bull Environ Contam Toxicol 78:455–458. https://doi.org/10.1007/s00128-007-9178-7
Li X, Li B, Xi S, Zheng Q, Lv X, Sun G (2013a) Prolonged environmental exposure of arsenic through drinking water on the risk of hypertension and type 2 diabetes. Environ Sci Pollut Res Int 20:8151–8161. https://doi.org/10.1007/s11356-013-1768-9
Li X, Li B, Xi S, Zheng Q, Wang D, Sun G (2013b) Association of urinary monomethylated arsenic concentration and risk of hypertension: a cross-sectional study from arsenic contaminated areas in northwestern China. Environ Health 12:37. https://doi.org/10.1186/1476-069x-12-37
Li Y, Wang D, Li X, Zheng Q, Sun G (2015) A potential synergy between incomplete arsenic methylation capacity and demographic characteristics on the risk of hypertension: findings from a cross-sectional study in an arsenic-endemic area of Inner Mongolia, China. Int J Environ Res Public Health 12:3615–3632. https://doi.org/10.3390/ijerph120403615
Li D, Zhang H, Chang F, Duan L, Zhang Y (2021) Distribution and health-ecological risk assessment of heavy metals: an endemic disease case study in southwestern China. Environ Sci Pollut Res Int. https://doi.org/10.1007/s11356-021-15591-x
Lindberg AL, Sohel N, Rahman M, Persson LA, Vahter M (2010) Impact of smoking and chewing tobacco on arsenic-induced skin lesions. Environ Health Perspect 118:533–538. https://doi.org/10.1289/ehp.0900728
López-Carrillo L, Hernández-Ramírez RU, Gandolfi AJ, Ornelas-Aguirre JM, Torres-Sánchez L, Cebrian ME (2014) Arsenic methylation capacity is associated with breast cancer in northern Mexico. Toxicol Appl Pharmacol 280:53–59. https://doi.org/10.1016/j.taap.2014.07.013
Lucio M, Barbir R, Vučić Lovrenčić M, Canecki Varžić S, Ljubić S, Smirčić Duvnjak L et al (2020) Association between arsenic exposure and biomarkers of type 2 diabetes mellitus in a Croatian population: a comparative observational pilot study. Sci Total Environ 720:137575. https://doi.org/10.1016/j.scitotenv.2020.137575
Luepker RV, Evans A, McKeigue P, Reddy KS (2004) Cardiovascular survey methods. 3rd ed. World Health Organization, Geneva. https://apps.who.int/iris/bitstream/handle/10665/42569/9241545763_eng.pdf;jsessionid=9BDA7C7411BE208697F20F2A7067BD3D?sequence=1
Mendez MA, González-Horta C, Sánchez-Ramírez B, Ballinas-Casarrubias L, Cerón RH, Morales DV et al (2016) Chronic exposure to arsenic and markers of cardiometabolic risk: a cross-sectional study in Chihuahua, Mexico. Environ Health Perspect 124:104–111. https://doi.org/10.1289/ehp.1408742
Moe B, Peng H, Lu X, Chen B, Chen LWL, Gabos S et al (2016) Comparative cytotoxicity of fourteen trivalent and pentavalent arsenic species determined using real-time cell sensing. J Environ Sci (china) 49:113–124. https://doi.org/10.1016/j.jes.2016.10.004
Orosun MM (2021) Assessment of arsenic and its associated health risks due to mining activities in parts of north-central Nigeria: probabilistic approach using Monte Carlo. J Hazard Mater 412:125262. https://doi.org/10.1016/j.jhazmat.2021.125262
Osorio-Yáñez C, Ayllon-Vergara JC, Arreola-Mendoza L, Aguilar-Madrid G, Hernández-Castellanos E, Sánchez-Peña LC et al (2015) Blood pressure, left ventricular geometry, and systolic function in children exposed to inorganic arsenic. Environ Health Perspect 123:629–635. https://doi.org/10.1289/ehp.1307327
Petrick JS, Ayala-Fierro F, Cullen WR, Carter DE, Vasken Aposhian H (2000) Monomethylarsonous acid (MMA(III)) is more toxic than arsenite in Chang human hepatocytes. Toxicol Appl Pharmacol 163:203–207. https://doi.org/10.1006/taap.1999.8872
Pi K, Wang Y, Xie X, Su C, Ma T, Li J et al (2015) Hydrogeochemistry of co-occurring geogenic arsenic, fluoride and iodine in groundwater at Datong Basin, northern China. J Hazard Mater 300:652–661. https://doi.org/10.1016/j.jhazmat.2015.07.080
Podgorski J, Berg M (2020) Global threat of arsenic in groundwater. Science 368:845–850. https://doi.org/10.1126/science.aba1510
Rahman M, Tondel M, Ahmad SA, Chowdhury IA, Faruquee MH, Axelson O (1999) Hypertension and arsenic exposure in Bangladesh. Hypertension 33:74–78. https://doi.org/10.1161/01.hyp.33.1.74
Reddy RR, Rodriguez GD, Webster TM, Abedin MJ, Karim MR, Raskin L et al (2020) Evaluation of arsenic field test kits for drinking water: recommendations for improvement and implications for arsenic affected regions such as Bangladesh. Water Res 170:115325. https://doi.org/10.1016/j.watres.2019.115325
Scannell Bryan M, Sofer T, Mossavar-Rahmani Y, Thyagarajan B, Zeng D, Daviglus ML et al (2019) Mendelian randomization of inorganic arsenic metabolism as a risk factor for hypertension- and diabetes-related traits among adults in the Hispanic Community Health Study/Study of Latinos (HCHS/SOL) cohort. Int J Epidemiol 48:876–886. https://doi.org/10.1093/ije/dyz046
Shen H, Niu Q, Xu M, Rui D, Xu S, Feng G et al (2016) Factors affecting arsenic methylation in arsenic-exposed humans: a systematic review and meta-analysis. Int J Environ Res Public Health 13:205. https://doi.org/10.3390/ijerph13020205
Spratlen MJ, Grau-Perez M, Best LG, Yracheta J, Lazo M, Vaidya D et al (2018) The association of arsenic exposure and arsenic metabolism with the metabolic syndrome and its individual components: prospective evidence from the strong heart family study. Am J Epidemiol 187:1598–1612. https://doi.org/10.1093/aje/kwy048
States JC, Srivastava S, Chen Y, Barchowsky A (2009) Arsenic and cardiovascular disease. Toxicol Sci 107:312–323. https://doi.org/10.1093/toxsci/kfn236
Steinmaus C, Yuan Y, Kalman D, Atallah R, Smith AH (2005) Intraindividual variability in arsenic methylation in a U.S. population. Cancer Epidemiol Biomarkers Prev 14:919–924. https://doi.org/10.1158/1055-9965.Epi-04-0277
Sun G, Xu Y, Zheng Q, Xi S (2011) Arsenicosis history and research progress in Mainland China. Kaohsiung J Med Sci 27:377–381. https://doi.org/10.1016/j.kjms.2011.05.004
Susko ML, Bloom MS, Neamtiu IA, Appleton AA, Surdu S, Pop C et al (2017) Low-level arsenic exposure via drinking water consumption and female fecundity—a preliminary investigation. Environ Res 154:120–125. https://doi.org/10.1016/j.envres.2016.12.030
Tong S, Li H, Tudi M, Yuan X, Yang L (2021) Comparison of characteristics, water quality and health risk assessment of trace elements in surface water and groundwater in China. Ecotoxicol Environ Saf 219:112283. https://doi.org/10.1016/j.ecoenv.2021.112283
Tseng CH (2009) A review on environmental factors regulating arsenic methylation in humans. Toxicol Appl Pharmacol 235:338–350. https://doi.org/10.1016/j.taap.2008.12.016
Vahter M (2000) Genetic polymorphism in the biotransformation of inorganic arsenic and its role in toxicity. Toxicol Lett 112–113:209–217. https://doi.org/10.1016/s0378-4274(99)00271-4
Wang SL, Li WF, Chen CJ, Huang YL, Chen JW, Chang KH et al (2011) Hypertension incidence after tap-water implementation: a 13-year follow-up study in the arseniasis-endemic area of southwestern Taiwan. Sci Total Environ 409:4528–4535. https://doi.org/10.1016/j.scitotenv.2011.07.058
Wei B, Yu J, Wang J, Yang L, Li H, Kong C et al (2017) The relationships between arsenic methylation and both skin lesions and hypertension caused by chronic exposure to arsenic in drinking water. Environ Toxicol Pharmacol 53:89–94. https://doi.org/10.1016/j.etap.2017.05.009
Wei M, Wu J, Li W, Zhang Q, Su F, Wang Y (2021) Groundwater geochemistry and its impacts on groundwater arsenic enrichment, variation, and health risks in Yongning county, Yinchuan plain of northwest China. Expo Health. https://doi.org/10.1007/s12403-021-00391-y
World Health Organization (2011) Arsenic in drinking-water background document for development of who guidelines for drinking-water quality. https://www.who.int/water_sanitation_health/dwq/chemicals/arsenic.pdf. Accessed 25 Nov 2021
World Health Organization (2020) The world health statistics 2020. https://www.who.int/data/gho/publications/world-health-statistics. Accessed 25 May 2020
Wu B, Wang G, Wu J, Fu Q, Liu C (2014) Sources of heavy metals in surface sediments and an ecological risk assessment from two adjacent plateau reservoirs. PLoS ONE 9:e102101. https://doi.org/10.1371/journal.pone.0102101
Xiao C, Ma T, Du Y, Liu Y, Liu R, Zhang D et al (2021) Impact process of the aquitard to regional arsenic accumulation of the underlying aquifer in Central Yangtze River Basin. Environ Geochem Health 43:1091–1107. https://doi.org/10.1007/s10653-020-00541-2
Yu Y, Guo Y, Zhang J, Xie J, Zhu Y, Yan J et al (2017) A perspective of chronic low exposure of arsenic on non-working women: risk of hypertension. Sci Total Environ 580:69–73. https://doi.org/10.1016/j.scitotenv.2016.11.204
Zeng Q, Zhang A (2020) Assessing potential mechanisms of arsenic-induced skin lesions and cancers: human and in vitro evidence. Environ Pollut 260:113919. https://doi.org/10.1016/j.envpol.2020.113919
Zhang C, Mao G, He S, Yang Z, Yang W, Zhang X et al (2013) Relationship between long-term exposure to low-level arsenic in drinking water and the prevalence of abnormal blood pressure. J Hazard Mater 262:1154–1158. https://doi.org/10.1016/j.jhazmat.2012.09.045
Zhang Q, Hou Y, Wang D, Xu Y, Wang H, Liu J et al (2020) Interactions of arsenic metabolism with arsenic exposure and individual factors on diabetes occurrence: baseline findings from arsenic and non-communicable disease cohort (ASNCD) in China. Environ Pollut 265:114968. https://doi.org/10.1016/j.envpol.2020.114968
Acknowledgements
This work was supported by grants from National Nature Science Foundation of China (Grant Number 81372933). We gratefully acknowledged the assistance and cooperation of the faculty and staff of the Centers for Endemic Disease Control and Prevention in Shanxi, Inner Mongolia, and Dali, Yunnan, and thank all those who participated in our study. We would like to thank Darren Jen-Sung Lu and Juehan (Hanna) Ye from the University of Pennsylvania for editing this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author declare they have no actual or potential competing financial interests.
Ethical Approval
The present study was approved by Ethics Committee of China Medical University (No.13059).
Informed Consent
All study participants provided written informed consent.
Research Involving Human and Animal Rights
This study followed the institutional guidelines of the “Declaration of Helsinki Ethical Principles” for all procedures involving human participants and was approved by Ethics Committee of China Medical University.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Dong, Y., Zhou, M., Zhang, M. et al. The Association Between Arsenic Metabolism and Hypertension Among Population with Varying Arsenic Exposure Levels in China. Expo Health 14, 411–430 (2022). https://doi.org/10.1007/s12403-022-00462-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12403-022-00462-8