Abstract
Background
In stable coronary artery disease (CAD), the prognostic interaction between clinical variables and treatment appropriateness based on anatomic/functional phenotype needs to be evaluated.
Methods
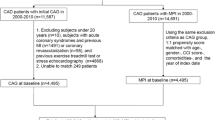
1585 consecutive patients underwent myocardial perfusion scintigraphy and coronary angiography within 90 days. Obstructive CAD (> 70% stenosis) with downstream moderate-to-severe ischemia (> 10%) was considered significant. Coronary revascularization was considered appropriate if all hemodynamically significant lesions were revascularized, while medical therapy only was deemed appropriate in the absence of hemodynamically significant CAD.
Results
Obstructive CAD and moderate-to-severe ischemia were documented in 1184 (75%) and 466 (29%) patients, respectively. Over mean follow-up of 4.7 ± 2.5 years, the primary endpoint (cardiac death and non-fatal myocardial infarction) occurred in 132 (8.2%) patients. Of patients with obstructive CAD, 797 (67%) were managed appropriately. Patients’ management was inappropriate in 389 patients, because either non-hemodynamically significant lesions were revascularized (50%, including 2 patients with non-obstructive lesions being inappropriately revascularized) or ischemia-causing CAD was left untreated (50%). At multivariate analysis, an inappropriate management (P < .001) was correlated with the primary endpoint, together with previous myocardial infarction (P = .009), lower ejection fraction (P < .001) and higher glucose levels (P < .001).
Conclusions
In stable CAD patients, management based on anatomic/functional phenotyping was correlated with a prognostic advantage at long-term follow-up.
Graphical abstract
Correlation between treatment categories and patients’ prognosis. A significantly higher event-rate was observed in patients where hemodynamically significant coronary lesions were left untreated—either because MT was not-adherently chosen or in the case of incomplete revascularization—than in those that were revascularized completely (17.6% vs 5.1%; P < .001). Conversely, the revascularization of non-hemodynamically significant CAD correlated with a higher event-rate than that of similar patients managed medically (13.8% vs 8.3%, P = .04). The event-rate of patients in whom coronary revascularization was performed in the presence of hemodynamically significant CAD (‘appropriate revascularization’) was similar to those with “No CAD/non-obstructive CAD” (5.1% vs 3.5%; P = NS).




Similar content being viewed by others
Abbreviations
- MPS:
-
Myocardial perfusion scintigraphy
- CAD:
-
Coronary artery disease
- CZT:
-
Cadmium-Zinc-Telluride
- ICA:
-
Invasive coronary angiography
- CTCA:
-
Computed tomography coronary angiography
- SDS:
-
Summed difference score
- MI:
-
Myocardial infarction
- LVEF:
-
Left ventricular ejection fraction
References
Neumann FJ, Sousa-Uva M, Ahlsson A, Alfonso F, Banning AP, Benedetto U. 2018 ESC/EACTS Guidelines on myocardial revascularization. Eur Heart J 2019;40:87‐165.
Hachamovitch R, Rozanski A, Shaw LJ, Stone GW, Thomson LE, Friedman JD, et al. Impact of ischaemia and scar on the therapeutic benefit derived from myocardial revascularization vs. medical therapy among patients undergoing stress-rest myocardial perfusion scintigraphy. Eur Heart J 2011;32:1012‐24.
Boden WE, O’Rourke RA, Teo KK, Hartigan PM, Maron DJ, Kostuk WJ, et al. Optimal medical therapy with or without PCI for stable coronary disease. N Engl J Med 2007;356:1503‐16.
Frye RL, August P, Brooks MM, Hardison RM, Kelsey SF, MacGregor JM, et al. A randomized trial of therapies for type 2 diabetes and coronary artery disease. N Engl J Med 2009;360:2503‐15.
Maron DJ, Hochman JS, Reynolds HR, Bangalore S, O’Brien SM, Boden WE, et al. Initial invasive or conservative strategy for stable coronary disease. N Engl J Med 2020;382:1395‐407.
Sud M, Han L, Koh M, Austin PC, Farkouh ME, Ly HQ, et al. Association between adherence to fractional flow reserve treatment thresholds and major adverse cardiac events in patients with coronary artery disease. JAMA 2020;324:2406‐14.
Neglia D, Liga R, Caselli C, Carpeggiani C, Lorenzoni V, Sicari R, et al. Anatomical and functional coronary imaging to predict long-term outcome in patients with suspected coronary artery disease: The EVINCI-outcome study. Eur Heart J Cardiovasc Imaging 2020;21:1273‐82.
De Bruyne B, Fearon WF, Pijls NH, Barbato E, Tonino P, Piroth Z, et al. Fractional flow reserve-guided PCI for stable coronary artery disease. N Engl J Med 2014;371:1208‐17.
Gimelli A, Pugliese NR, Buechel RR, Coceani M, Clemente A, Kaufmann PA, et al. Myocardial perfusion scintigraphy for risk stratification of patients with coronary artery disease: The AMICO registry. Eur Heart J Cardiovasc Imaging 2022;23:372‐80.
Gimelli A, Liga R, Giorgetti A, Kusch A, Pasanisi EM, Marzullo P. Relationships between myocardial perfusion abnormalities and poststress left ventricular functional impairment on cadmium-zinc-telluride imaging. Eur J Nucl Med Mol Imaging 2015;42:994‐1003.
Gimelli A, Liga R, Pasanisi EM, Casagranda M, Coceani M, Marzullo P. Influence of cardiac stress protocol on myocardial perfusion imaging accuracy: The role of exercise level on the evaluation of ischemic burden. J Nucl Cardiol 2016;23:1114‐22.
Knuuti J, Wijns W, Saraste A, Capodanno D, Barbato E, Funck-Brentano C, et al. 2019 ESC Guidelines for the diagnosis and management of chronic coronary syndromes. Eur Heart J 2020;41:407‐77.
Neglia D, Aimo A, Lorenzoni V, Caselli C, Gimelli A. Triglyceride-glucose index predicts outcome in patients with chronic coronary syndrome independently of other risk factors and myocardial ischaemia. Eur Heart J Open 2021. https://doi.org/10.1093/ehjopen/oeab004.
Kumar A, Patel DR, Harb SC, Greenberg NL, Bhargava A, Menon V, et al. Implementation of a myocardial perfusion imaging risk algorithm to inform appropriate downstream invasive testing and treatment. Circ Cardiovasc Imaging 2021;14:e011984.
Mancini GBJ, Hartigan PM, Shaw LJ, Berman DS, Hayes SW, Bates ER, et al. Predicting outcome in the COURAGE trial (Clinical Outcomes Utilizing Revascularization and Aggressive Drug Evaluation): Coronary anatomy versus ischemia. JACC Cardiovasc Interv 2014;7:195‐201.
Cheruvu C, Precious B, Naoum C, Blanke P, Ahmadi A, Soon J, et al. Long term prognostic utility of coronary CT angiography in patients with no modifiable coronary artery disease risk factors: Results from the 5 year follow-up of the CONFIRM International Multicenter Registry. J Cardiovasc Comput Tomogr 2016;10:22‐7.
Liga R, Vontobel J, Rovai D, Marinelli M, Caselli C, Pietila M, et al. Multicentre multi-device hybrid imaging study of coronary artery disease: Results from the EValuation of INtegrated Cardiac Imaging for the Detection and Characterization of Ischaemic Heart Disease (EVINCI) hybrid imaging population. Eur Heart J Cardiovasc Imaging 2016;17:951‐60.
Younis A, Goldkorn R, Goldenberg I, Geva D, Tzur B, Mazu A, et al. Impaired fasting glucose is the major determinant of the 20-year mortality risk associated with metabolic syndrome in nondiabetic patients with stable coronary artery disease. J Am Heart Assoc 2017. https://doi.org/10.1161/JAHA.117.006609.
Van Belle E, Cosenza A, Baptista SB, Vincent F, Henderson J, Santos L, et al. Usefulness of routine fractional flow reserve for clinical management of coronary artery disease in patients with diabetes. JAMA Cardiol 2020;5:272‐81.
Chaitman BR, Hardison RM, Adler D, Gebhart S, Grogan M, Ocampo S, et al. The Bypass Angioplasty Revascularization Investigation 2 Diabetes randomized trial of different treatment strategies in type 2 diabetes mellitus with stable ischemic heart disease: Impact of treatment strategy on cardiac mortality and myocardial infarction. Circulation 2009;120:2529‐40.
Lopes RD, Alexander KP, Stevens SR, Reynolds HR, Stone GW, Piña IL, et al. Initial invasive versus conservative management of stable ischemic heart disease in patients with a history of heart failure or left ventricular dysfunction: Insights from the ISCHEMIA Trial. Circulation 2020;142:1725‐35.
Neglia D, Rovai D, Caselli C, Pietila M, Teresinska A, Aguadé-Bruix S, et al. Detection of significant coronary artery disease by noninvasive anatomical and functional imaging. Circ Cardiovasc Imaging 2015. https://doi.org/10.1161/CIRCIMAGING.114.002179.
Kaptoge S, Di Angelantonio E, Lowe G, Pepys MB, Thompson SG, Collins R, et al. C-reactive protein concentration and risk of coronary heart disease, stroke, and mortality: An individual participant meta-analysis. Lancet 2010;375:132‐40.
Disclosure
The authors have indicated that they have no financial conflict of interest.
Ethical approval
The study conformed to the declaration of Helsinki and was approved by the Institution’s human research committee.
Informed consent
All participants gave written informed consent.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The authors of this article have provided a PowerPoint file, available for download at SpringerLink, which summarises the contents of the paper and is free for re-use at meetings and presentations. Search for the article DOI on SpringerLink.com.
The authors have also provided an audio summary of the article, which is available to download as ESM, or to listen to via the JNC/ASNC Podcast.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liga, R., Neglia, D., Cavaleri, S. et al. Prognostic impact of patients’ management based on anatomic/functional phenotype: a study in patients with chronic coronary syndromes. J. Nucl. Cardiol. 30, 736–747 (2023). https://doi.org/10.1007/s12350-022-03070-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12350-022-03070-w