Abstract
Background
Combined supine-prone myocardial perfusion imaging (CSP MPI) has been shown to reduce attenuation artifact in comparison to supine-only (SU) MPI in mixed-gender populations with varying risk for coronary artery disease (CAD), often where patients served as their own controls. However, there is limited direct comparison of these imaging strategies in men.
Methods
934 male patients underwent CSP or SU MPI. Diagnostic certainty of interpretation was compared. Within the cohort, 116 were referred for left heart catheterization (LHC) to assess for CAD. Sensitivity, specificity, and area under the curve (AUC) were compared with additional analysis based on body mass index (BMI).
Results
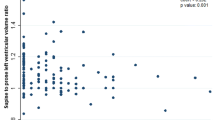
597 patients completed the SU protocol and 337 patients completed the CSP protocol. Equivocal studies were seen more frequently in the SU group (13%) than in the CSP group (4%, P < .001). At catheterization, the specificity for CSP MPI of 70% was higher than 40% for SU MPI (P = .032). The CSP AUC (0.80 ± 0.06) was significantly larger than SU AUC (0.57 ± 0.05, P = .004). CSP specificity was significantly higher in obese patients.
Conclusions
CSP MPI increases diagnostic certainty and improves test accuracy for CAD detection in men with CAD risk factors, especially obese patients, compared to SU MPI.

Similar content being viewed by others
Abbreviations
- AC:
-
Attenuation correction
- BMI:
-
Body mass index
- CABG:
-
Coronary artery bypass grafting
- CAD:
-
Coronary artery disease
- CSP:
-
Combined supine-prone
- EKG:
-
Electrocardiogram
- FFR:
-
Fractional flow reserve
- LHC:
-
Left heart catheterization
- MPI:
-
Myocardial perfusion imaging
- PCI:
-
Percutaneous coronary intervention
- SPECT:
-
Single photon emission computed tomography
- SU:
-
Supine
References
Hendel RC. Attenuation correction: Eternal dilemma or real improvement? J Nucl Med Mol Imaging 2005;49:30-42.
Esquerre J-P, Coca FJ, Martinez SJ, Guiraud RF. Prone decubitus: A solution to inferior wall attenuation in thallium-201 myocardial tomography. J Nucl Med 1989;30:398-401.
Segall GM, Davis M. Prone versus supine thallium myocardial SPECT: A method to decrease artifactual inferior defects. J Nucl Med 1989;30:548-55.
Kiat H, Van Train KF, Friedman JD, Germano G, Silagan G, Wang FP, et al. Quantitative stress-redistribution thallium-201 SPECT using prone imaging: Methodologic development and validation. J Nucl Med 1992;33:1509-15.
Slomka PJ, Nishina H, Abidov A, Hayes SW, Friedman JD, Berman DS, et al. Combined quantitative supine-prone myocardial perfusion SPECT improves detection of coronary artery disease and normalcy rates in women. J Nucl Cardiol 2007;14:44-52.
Berman DS, Kang XP, Nishina H, Slomka PJ, Shaw LJ, Hayes SW, et al. Diagnostic accuracy of gated Tc-99m sestamibi stress myocardial perfusion SPECT with combined supine and prone acquisitions to detect coronary artery disease in obese and non-obese patients. J Nucl Cardiol 2006;13:191-201.
Hayes SW, DeLorenzo A, Hachamovich R, Dhar SC, Hsu P, Cohen I, et al. Prognostic implications of combined prone and supine acquisitions in patients with equivocal or abnormal supine myocardial perfusion SPECT. J Nucl Med 2003;44:1633-40.
Malkemeker D, Brenner R, Martin WH, Sampson UK, Feurer ID, Kronenberg MW, et al. CT-based attenuation correction versus prone imaging to decrease equivocal interpretation of rest/stress TC-99m tetrofosmin SPECT MPI. J Nucl Cardiol 2007;14:314-23.
Hendel RC, Berman DS, Di Carli MF, Heidenreich PA, Henkin RE, Pellikka PA, et al. CCF/ASNC/ACR/AHA/ASE/SCCT/SCMR/SNM 2009 appropriate use criteria for cardiac radionuclide imaging: A report of the American College of Cardiology Foundation Appropriate Use Criteria Task Force, the American Society of Nuclear Cardiology, the American College of Radiology, the American Heart Association, the American Society of Echocardiography, the Society of Cardiovascular Computed Tomography, the Society for Cardiovascular Magnetic Resonance, and the Society of Nuclear Medicine. Circulation 2009;119:e561-87.
Winchester DE, Kitchen A, Brandt JC, Dusaj RS, Virani SS, Bradley SM, et al. Metrics of quality care in veterans: Correlation between primary-care performance measures and inappropriate myocardial perfusion imaging. Clin Cardiol 2015;38:195-9.
Tilkemeier PL, Cooke CD, Grossman GB, Mcallister BD, Ward BD, Clinical Guidelines and Quality Standards, American Society of Nuclear Cardiology. ASNC Imaging Guidelines for Nuclear Cardiology Procedures: Standardized reporting of radionuclide myocardial perfusion and function. Am Soc Nucl Cardiol 2009. doi:10.1007/s12350-009-9095-8.11.
Hendel RC, Wackers FJ, Berman D, Ficaro E, DePuey E, Klein EG, et al. American Society of Nuclear Cardiology Consensus Statement: Reporting of radionuclide myocardial perfusion imaging studies. J Nucl Cardiol 2003;10:705-8.
DeLong ER, DeLong DM, Clarke-Pearson DL. Comparing the areas under two or more correlated receiver operating characteristic curves: A non-parametric approach. Biometrics 1998;44:837-45.
Nishina H, Slomka PJ, Abidov A, Yoda S, Akincioglu C, Kang X, et al. Combined supine and prone quantitative myocardial perfusion SPECT: Method development and clinical validation in patients with no known coronary artery disease. J Nucl Med 2006;47:51-8.
Arsanjani R, Hayes SW, Fish M, Shalev A, Nakanishi R, Thomson L, et al. Two-position supine/prone myocardial perfusion SPECT(MPS) imaging improves visual inter-observer correlation and agreement. J Nucl Cardiol 2014;21:703-11.
Perault C, Loboguerro A, Lien J-C, Wampach H, Gibold C, Ouzan J, et al. Quantitative comparison of prone and supine myocardial SPECT images. Clin Nucl Med 1994;20:678-84.
Katayama T, Ogata N, Tsuruya Y. Diagnostic accuracy of supine and prone thallium-201 stress myocardial perfusion single-photon emission computed tomography to detect coronary artery disease in inferior wall of the left ventricle. Ann Nucl Med 2008;24:317-21.
Rozanski A, Diamond GA, Berman D, Forrester JS, Morris D, Swan HJC. The declining specificity of exercise radionuclide ventriculography. N Engl J Med 1983;309:518-22.
Rozanski A, Berman D. The efficacy of cardiovascular nuclear medicine studies. Semin Nucl Med 1987;2:104-20.
Li J, Elrashidi MY, Flammer AJ, Lennon RJ, Bell MR, Holmes D, et al. Long-term outcomes of fractional flow reserve-guided vs. angiography-guided percutaneous coronary intervention in contemporary practice. Eur Heart J 2013;34:1375-83.
Takamura T, Horiguchi Y, Kanna M, Matsushita H, Sudo Y, Kikuchi S, et al. Validation of prone myocardial perfusion SEPCT with a variable focus collimator versus supine myocardial perfusion SPECT with or without computed tomography-derived attenuation correction. Ann Nucl Med 2015. doi:10.1007/s12149-015-1019-x.
Malkerneker D, Brenner R, Martin WH, Sampson UK, Feurer ID, Kronenberg MW, et al. CT-based attenuation correction versus prone imaging to decrease equivocal interpretations of rest/stress Tc-99m tetrofosmin SPECT MPI. J Nucl Cardiol 2007;14:314-23.
Reyes E, Wiener S, Underwood SR, European Council of Nuclear Cardiology. Myocardial perfusion scintigraphy in Europe 2007: A survey of the European Council of Nuclear. Cardiology 2012;39:160-4.
Shin J, Pokhara H, Williams K, Mehta R, Ward RP. SPECT myocardial perfusion imaging with prone only acquisitions: Correlation with coronary angiography. J Nucl Cardiol 2009;16:590-6.
Disclosure
The authors report no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
See related editorial, doi:10.1007/s12350-015-0389-8.
Rights and permissions
About this article
Cite this article
Taasan, V., Wokhlu, A., Taasan, M.V. et al. Comparative accuracy of supine-only and combined supine-prone myocardial perfusion imaging in men. J. Nucl. Cardiol. 23, 1470–1476 (2016). https://doi.org/10.1007/s12350-015-0358-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12350-015-0358-2